This week, we reviewed the request for proposals (RFP) issued by the Arizona Health Care Cost Containment System (AHCCCS) on November 1, 2016, to reprocure Medicaid managed care contracts for the Arizona Long Term Care System (ALTCS) program. ALTCS is one of the oldest Medicaid managed long term services and supports (MLTSS) programs in the country, providing integrated acute care, LTSS, and behavioral health services to individuals who are elderly, individuals with physical disabilities, and individuals with intellectual or developmental disabilities (I/DD). However, this RFP only covers the roughly 26,500 individuals who are elderly or individuals with a physical disability (E/PD); this RFP does not include individuals with I/DD, who are covered through a state-run model.
Covered Populations, Estimated Annual Spending
The ALTCS E/PD RFP covers nearly all Medicaid and Medicaid-Medicare dual eligible members statewide who are elderly or have a physical disability. As of October 1, 2016, there were 26,532 ALTCS E/PD members covered by one of three existing MCOs. The ALTCS program is currently broken out into seven geographic services areas (GSAs), which will be consolidated down to three GSAs under this RFP. As detailed in the table below, based on the 2017 actuarial certification for ALTCS E/PD rates, the average statewide per-member-per-month (PMPM) rate is around $3,300. Based on this PMPM membership of roughly 26,500, annual payments to MCOs under ALTCS E/PD contracts exceed $1 billion.
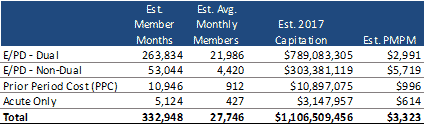
Source: ALTCS Actuarial Certification, 2017
D-SNP Requirements
ALTCS E/PD health plans awarded under this RFP must operate a Medicare Dual Eligible Special Needs Plan (D-SNP) by January 1, 2018. Bidders must submit a non-binding notice of intent to apply as a D-SNP no later than November 10, 2016, with the final application due by February 1, 2017. The RFP states that AHCCCS will not contract with any D-SNP to serve the ALTCS E/PD Medicaid population outside of awarded ALTCS E/PD contracts. Going forward, the state intends to continue to take steps to improve alignment for dual eligible members.
RFP Timeline
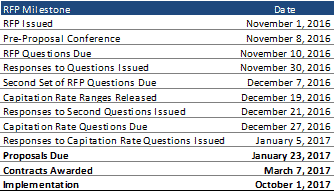
AHCCCS will conduct three rounds of questions and answers over the next two months, with proposals due to the state on January 23, 2017. AHCCCS intends to award contracts and begin transition activities in March, 2017, with operational implementation set for October 1, 2017.
Proposal Evaluation
ALTCS E/PD proposals will be evaluated across the following four categories, and will be weighted in order from high to low, although weighting is not specified in the RFP documents, with program and capitation sections weighted higher than access/network and administrative.
- Program (including oral presentations)
- Capitation
- Access to Care/Network
- Administrative
The Capitation section will be scored separately for each GSA, while the other three categories will be scored statewide.
Contract Awards, Terms
AHCCCS intends to award a maximum of three contracts in the Central GSA, and a maximum of one contract in each of the North and South GSAs, with the exception of potentially awarding two contracts for Pima County in the South GSA.
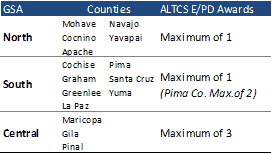
To be eligible for an ALTCS E/PD contract award in the Central GSA, bidders must also submit a bid for the North GSA. AHCCCS does not intend to award any bidders a statewide contract to cover all three GSAs. Contracts will begin October 1, 2017, with an initial three year term. There are three contract renewal terms available – one two-year renewal term, followed by two one-year renewal terms.
Current ALCTS Market
There are three MCOs currently serving the ALTCS E/PD market. Mercy Care Plan, which has an ASO arrangement with Aetna, is the largest, with more than 41 percent of the market, followed by United at more than 38 percent. Centene’s Bridgeway Health Solutions is the third plan, with just under 20 percent market share. UnitedHealthcare is the only ALTCS MCO currently operating in all three of the redesigned GSAs.
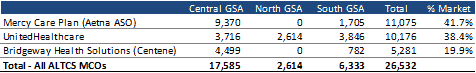
Note: GSAs in table above based on RFP, not current GSA design.
Source: AHCCCS Enrollment Data, October 2016.
RFP Documents, Bidders Library
The ALTCS E/PD RFP, bidders library, and other documents are available at: https://www.azahcccs.gov/PlansProviders/HealthPlans/YH18-0001.html