Previously, HMA developed a comprehensive series of webinars reviewing the potential for using 1115 waivers to expand and improve health care services for the justice-involved population. With California becoming the first state earlier in 2023 to receive approval for the authority to provide a specific set of Medicaid services for up to 90 days in advance of release to youth and adults in state prisons, county jails, and youth correctional facilities, and many other states with pending waivers of a similar type, this blog post considers the implications of this emerging policy trend for local and regional managed care organizations (MCOs) in 2024.
The Opportunity
Delivering Medicaid services through MCOs has become the dominant strategy employed by states with 41 states (including the District of Columbia) using managed care for at least certain Medicaid populations. Local and regional MCOs represent a key component in this landscape across the country and often are deeply rooted in the states and communities they serve because of their specific focus on a single or limited number of markets.
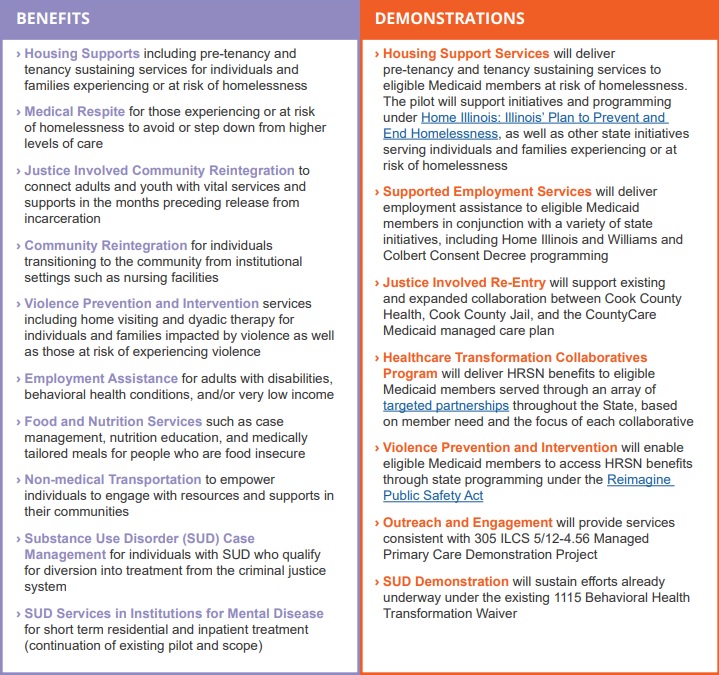
With the precedent now in place for federal authority (and federal financial participation) to provide services such as reentry case management, behavioral health and physical health consultation services (in-person or via telehealth), laboratory and radiology services, medications as well as medication administration, medication assisted therapy inclusive of counseling, and community health worker services, states have a clear pathway toward pursuing the ability to provide services for the justice-involved population prior to release. Among the many important implementation questions states will need to consider as they continue to pursue the authority to provide these services is how the specific services will be delivered and financed. Given the dominance of Medicaid managed care, states will have to grapple with how MCOs can be leveraged to support a successful implementation of the delivery of services to the justice-involved population. The strong community presence of local and regional MCOs within the Medicaid managed care ecosystem makes these MCOs important entities for states to consider. Local and regional MCOs should consider what role they believe they can play as partners to states in these initiatives to serve justice-involved populations as successfully as they have served other Medicaid populations.
While the opportunities for local and regional MCOs will evolve over time, initial opportunities to contemplate are as follows:
- Serving as a Thought Partner: There is already significant interest across states in pursuing the ability to deliver services in advance of release but local and regional MCOs can support state officials looking to develop in greater detail the most viable path forward to do so. Local and regional MCOs can be well positioned serve as thought partners to states by educating themselves about California’s 1115 waiver approval and engaging state officials in their markets as partners to think through how the approach taken by California can be adapted to a given state’s goals and environment.
- Serving as the Lead Case Manager: Providing reentry case management to coordinate the reentry process for the justice-involved population is likely to be a key service in any service array from this population. To ensure the complex coordination related to this process occurs successfully across multiple organizations, local and regional MCOs can explore working with states to serve as the lead entity for case management as individuals are enrolled (or reenrolled) in managed care.
- Facilitating Enrollment Continuity and Continuity of Care: The process for transitioning to Medicaid coverage and care after these have been interrupted as a result of incarceration can be daunting for both the justice-involved population and well as state administrators and providers. Local and regional MCOs can play an intervening role here to provide support to all parties involved to produce a result where the enrollment process is as seamless as possible and critical care delivery is maintained specific to an individual’s health and social needs.
- Providing Infrastructure Funding: In partnership with states, local and regional MCOs can infrastructure funding to build capacity to support many of these entities who will be involved with the reentry process. Such entities can include, for example, behavioral health providers, community-based organizations, primary care providers, and social service providers. The type of capacity needed will likely include data sharing, technology changes, and workforce development.
- Providing Technical Assistance: In addition to supporting capacity-building, local and regional MCOs can provide technical assistance to entities involved with the reentry process. Complex operational, policy, and technology issues will arise during the reentry process that are specific to a given entity. Local and regional MCOs, because of their focused knowledge and experience in specific markets, are well positioned to provide expertise and guidance on issues ranging from care management to claims submission.
What’s Next?
As more states with pending 1115 waivers for reentry services for the justice-involved population gain approval, local and regional MCOs should anticipate engagement from states on planning and implementation in in 2024. Given this, taking action early to engage state partners and prepare your organization to serve this population is a prudent step to consider now.
For More Information
If you have questions about how HMA can support your efforts related to the Medicaid services for justice-involved populations and local and regional MCOs, please contact Michael Engelhard, managing director, Linda Follenweider, managing director, or Patrick Tigue, managing director.