This week, we reviewed the request for proposals (RFP) issued on February 27, 2017, by the Illinois Department of Healthcare and Family Services (HFS) to rebid the majority of the state’s existing Medicaid managed care program contracts, consolidate multiple programs into a single streamlined program, and expand managed care statewide. The RFP will consolidate the current Family Health Plans/ACA Adults (FHP/ACA) program, the Integrated Care Program (ICP), and the Managed Long Term Services and Supports (MLTSS) program into a single contracting approach, while reducing the number of contracted managed care organizations (MCOs) from 11 to between four and seven. The RFP does not impact the Medicare-Medicaid Alignment Initiative (MMAI) duals demonstration at this time. When fully implemented by the end of 2018, the new managed care program will cover roughly 2.7 million Medicaid beneficiaries in all 102 counties in Illinois.
RFP Covered Populations
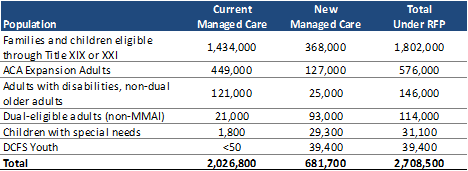
The RFP covers all non-MMAI (duals demonstration) beneficiaries currently covered under the FHP/ACA, ICP, and MLTSS programs, a little over 2 million members. In addition, the RFP geographically expands managed care to more than 680,000 new members, of which about 500,000 are families, children, and ACA adults. The expansion also includes around 93,000 dual eligibles who are not covered under the MMAI demonstration, as well as 25,000 non-dual seniors and adults with disabilities. The RFP also significantly expands managed care for children with special health care needs, defined as enrollees under the age of 21 who are eligible for Medicaid through Supplemental Security Income (SSI), Division of Specialized Care for Children (DSCC), or a disability category of eligibility.
Finally, a separate contract will be awarded to one successful statewide bidder for the Department of Children and Family Services (DCFS) Youth population, for children who are or have previously been under the care of DCFS. DCFS Youth will be mandatorily enrolled in managed care, except for those children who have been adopted or entered a guardianship, who will have the opportunity to opt-out of managed care.
The RFP does not carve-in home and community-based services (HCBS) waiver or intermediate care facility services for individuals with intellectual or developmental disabilities (I/DD), but bidders must be capable of assuming responsibility for these services with 180 days’ notice if the state decides to include them in the managed care service package at a future date.
Behavioral Health 1115 Waiver, Integrated Health Homes
On October 5, 2016, HFS submitted a Section 1115 demonstration waiver proposal (link) to the Centers for Medicare & Medicaid Services (CMS) with the goals of strengthening the state’s behavioral health care system and promoting greater integration of physical and behavioral health. The waiver specifically proposes the inclusion of a package of new benefits (link) for individuals with severe mental illness (SMI) and substance use disorders (SUD), as well individuals nearing release from the Illinois Department of Corrections (IDOC) and Cook County Jail systems. Additionally, the waiver proposes four initiatives aimed at increasing behavioral health integration and the use of value-based payment structures in Medicaid. This includes providing MCOs and providers with resources to pursue development of integrated health homes (IHHs) (link). Illinois intends to design and implement IHHs, and is requesting support around workforce integration, provider readiness assessment, encouraging partnerships and integration between physical and behavioral providers, the launching of disease-specific pilot projects, and data collection and reporting.
Evaluation Process, Financial Proposals
Bidders will be evaluated on meeting pass/fail proposal requirements, a technical proposal section (worth 500 out of 900 total points), a financial proposal (300 out of 900), and an oral presentation (100 out of 100). The technical proposal includes topics around integration of physical and behavioral health, IT solutions, specific sections on children with special needs and LTSS, and alternative and value-based payments. Under the financial proposal, bidders will submit bid rates that must fall within the rate cell ranges to be provided by HFS in the forthcoming data book.
Contract Awards
Under the RFP, interested bidders may submit a Proposal Option A, under which a MCO bids to serve all populations in all 102 counties statewide (new regions are designated in the RFP for the purposes of rate-setting alone). Alternatively, government-owned or minority-owned MCOs may submit a Proposal Option B, under which they bid only to serve Cook County. HFS intends to award between three and five MCO contracts under the statewide option (including Cook County), and between one and two additional MCO contracts under Option B for Cook County only. Contracts will be for an initial term of four years, with two optional two-year extensions, taking the potential full life of the contracts to eight years.
RFP Calendar, Implementation Timing
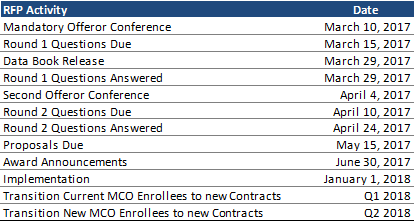
A mandatory bidders/offerors conference will be held on March 10, 2017. There will be two rounds of questions and answers, a data book release, and a second, encouraged but optional, conference before proposals are due to HFS on May 15, 2017. Award announcements are tentatively planned for the end of June, with contracts in effect on January 1, 2018. The RFP indicates that HFS will plan to transition all current MCO enrollees covered under the RFP to new contracts within the first 90 days of implementation, or during the first quarter (Q1) of 2018. This will be followed by the transition of all new MCO enrollees under the RFP in the following 90 days, or during Q2 2018.
Current Medicaid Managed Care Market
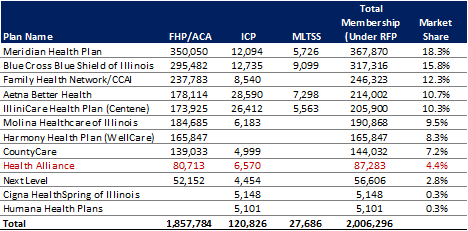
As of December 2016, there were 12 MCOs in contract with HFS across the three managed care programs under this RFP, as well as the MMAI duals demonstration. As of January 1, 2017, however, Health Alliance has ended its contracts in both the FHP/ACA and ICP programs. While Meridian Health Plan and Blue Cross Blue Shield of Illinois are the largest plans in terms of current market share, no plan has greater than 20 percent of the market.
Additionally, MCO participation across the five current mandatory managed care regions, and sometimes across the counties within a region, varies from program to program. A map of MCO participation by region is available here, current as of July 1, 2016.
Link to RFP, Appendices, Related Documents
https://www.illinois.gov/hfs/info/MedicaidManagedCareRFP/Pages/default.aspx