This week, our In Focus section reviews the Kentucky Medicaid managed care organizations (MCOs) request for proposals (RFP), issued by the Kentucky Finance and Administration Cabinet on May 16, 2019. The Kentucky Cabinet for Health and Family Services (CHFS), Department for Medicaid Services (DMS) will select up to five Medicaid MCOs to manage health care services for more than 1.2 million people, starting July 2020. Contracts are estimated at more than $7 billion.
The state’s Medicaid managed care program has been enacted since November 2011 and has been statewide since January 2013. Newly selected MCOs will provide statewide Medicaid and Kentucky Children’s Health Insurance Program (KCHIP) coverage for:
- Families and Children
- SSI Adults without Medicare
- SSI Children
- Foster Care Children
- Dual Eligibles (Medicaid and Medicare eligible)
- ACA MAGI Adults
- ACA Former Foster Care Children
Two different rates will be developed for MCOs – one for plans in Region 3 and one for plans in Regions 1, 2, 4-8. Region 3 includes Bullitt, Carroll, Hardin, Henry, Jefferson, Larue, Marion, Meade, Nelson, Oldham, Shelby, Spencer, Trimble, and Washington counties.
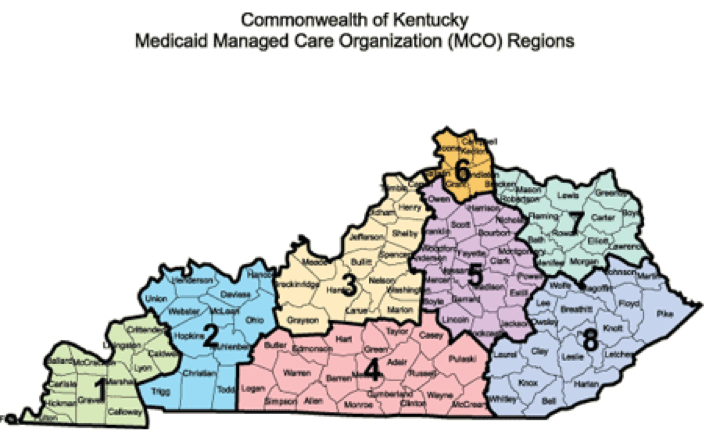
Source: The Kentucky Finance and Administration Cabinet
Kentucky SKY (Supporting Kentucky Youth) Program
One of the winning MCOs will also be contracted to provide covered services, population health management, and care management services to foster care, adoption assistance, and juvenile justice enrollees under the Kentucky SKY (Supporting Kentucky Youth) program. The MCO will oversee and coordinate both physical and behavioral health, dental care, social services, and wraparound services in order to meet the intensive health care needs of the children.
Evaluation
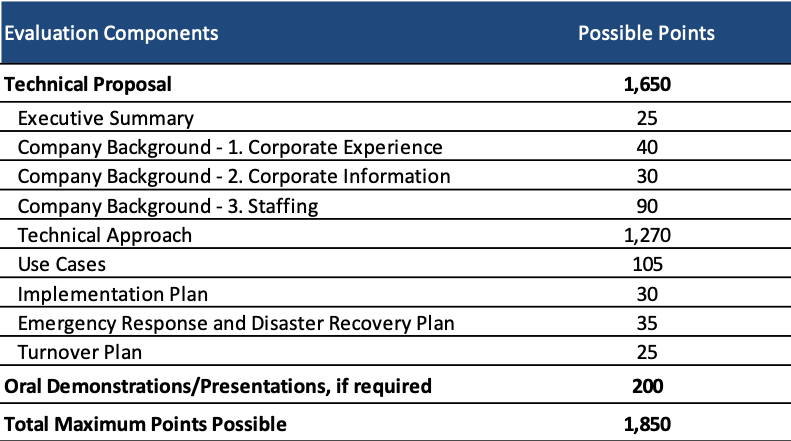
Medicaid managed care proposals will be scored out of a total 1,850 possible points. The technical proposal consists of 1,650 points and a possible oral demonstrations/presentation, worth 200 points, may be required. Kentucky may also request a Best and Final Offer (BAFO).
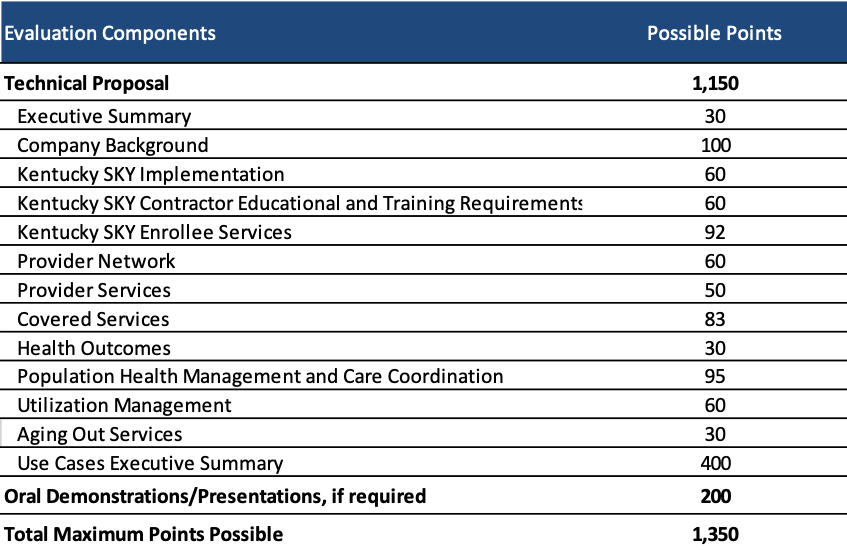
MCOs may also submit a proposal for Kentucky SKY. The proposal will only be scored if the MCO is selected for a managed care contract.
Timeline
Proposals are due July 5, 2019. Contracts will be effective July 1, 2020, through December 31, 2025, and may be renewed for five additional two-year periods through December 31, 2035.

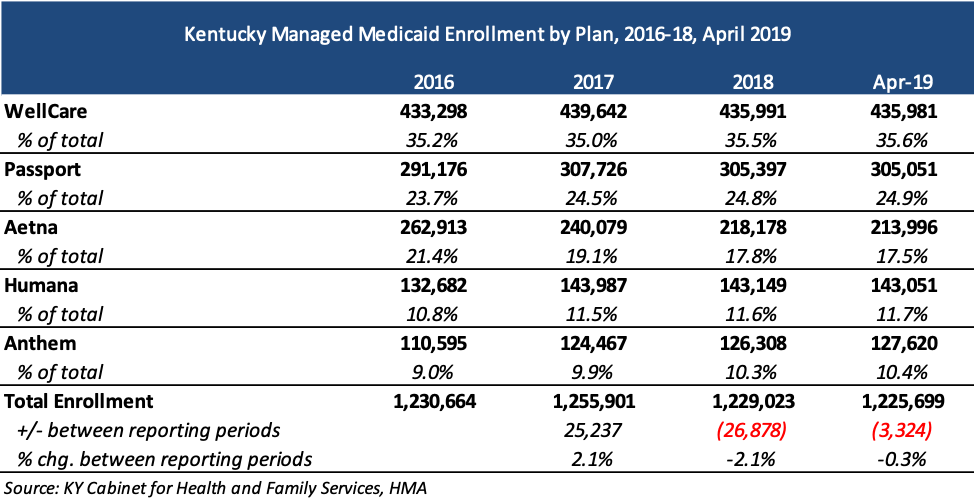
Current Market
Current Medicaid incumbents are Aetna, Anthem, Humana, Passport, and WellCare, with a total of 1.2 million lives as of April 2019. WellCare has the largest market share, with 35.6 percent of enrollment.