This week, our In Focus Focus reviews the Mississippi Children’s Health Insurance Program (CHIP) request for qualifications (RFQ) issued by the state’s Division of Medicaid on June 8, 2018. The Mississippi CHIP program provides statewide health coverage in all 82 counties to children in families with incomes up to 209 percent of the federal poverty level (FPL). As of March 2018, 46,958 children were enrolled in CHIP.
Services Covered
Managed care organizations (MCOs) will provide all Medically Necessary covered services allowed under CHIP. Services include inpatient hospital, outpatient hospital, physician, behavioral/substance use disorder, and prescription drug services.
CHIP Eligible Populations
Populations who are eligible for CHIP are shown below:
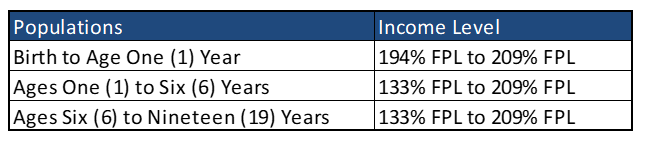
Depending on income level, some CHIP members will be responsible for cost sharing for certain services.
Network Requirements
MCOs will need to meet network adequacy requirements showing full range of medical specialties necessary to provide the covered benefits and establish Geographic Access Standards for urban and rural areas for all provider types. They will be required to contract with Federally Qualified Health Centers (FQHCs) and Rural Health Clinics (RHCs). The MCO networks must also include contracts with out-of-state providers for Medically Necessary Services and Indian Health Care Providers.
Population Health Management
Plans will also need to develop and execute a Population Health Management program to address the needs of both rural and urban beneficiaries as well as address race, ethnicity, income level, age, gender, language barriers and physical disabilities. The program will look to reduce the cost of care for members, improve health, help members manage their health needs and risks, support providers in delivery of care, and help modernize and execute data analytics strategies. Plans will be required to develop protocols for providing population health management services in alternative and community-based settings, including homeless shelters, public community organization facilities, homes, and schools.
Evaluation Criteria
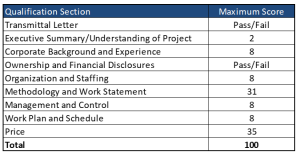
MCOs will receive scores of up to 100 points. The Evaluation Committee will evaluate the Management and Technical qualifications independent and separate of each. Price will not be an evaluation factor; however, it will be part of the total score make-up. Each MCO will receive 35 points for price despite there not being pricing information included within the Offeror’s qualification.
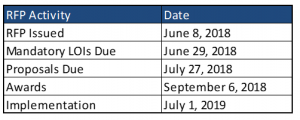
RFP Timeline
MCOs were required to submit a mandatory letter of intent by June 29. Proposals are due on July 27, with awards announced on September 6. Contracts will run from July 1, 2019 through June 30, 2022, with the option for two one-year extensions.
Contract Awards
The Mississippi Division of Medicaid will contract with at least two MCOs. MCOs can submit protests within seven days of the award.
Current CHIP Market
UnitedHealthcare of Mississippi and Magnolia Health Plan currently serve the 46,968 children as of March 2018.