This week, we reviewed the Medicaid long-term services and supports (LTSS) redesign draft paper published on March 7, 2017, by the Nebraska Department of Health and Human Services (DHHS). The paper is the follow-up to a January 2016 DHHS concept paper, which identified increasing pressure on the state’s Medicaid LTSS system. The LTSS redesign paper addresses identified high-priority systemic issues in the current LTSS system, recommends longer-term system changes, and outlines a transition to managed LTSS (MLTSS). Nebraska has long been in discussion around a transition to MLTSS, and this draft redesign paper potentially puts the state on a timeline to begin providing mandatory MLTSS statewide to older adults and individuals with disabilities (Phase 1) as of January 1, 2019, with MLTSS to follow for individuals with intellectual or developmental disabilities (Phase 2) on July 1, 2019. We estimate the potential MLTSS population at more than 50,000 beneficiaries with annual LTSS spending between $800 million and $850 million.
MLTSS Approach
Rather than recommending a standalone MLTSS program or a separate contracting approach, as many states have, the Nebraska recommendations would expand the scope of the existing statewide Heritage Health program MCOs to cover the target MLTSS population. Heritage Health is Nebraska’s new statewide Medicaid managed care program, which launched on January 1, 2017, with three MCOs under contract. These three plans – Centene’s Nebraska Total Care, UnitedHealthcare, and WellCare – are already administering physical, behavioral, and pharmacy benefits for individuals enrolled in Nebraska’s home and community-based services (HCBS) waivers, while their waiver services and other LTSS benefits are reimbursed fee-for-service. These waivers include:
- Aged and Disabled Waiver;
- TBI Waiver;
- Children’s Developmental Disabilities Waiver (consolidated with the DD adult waiver effective April 1, 2017);
- Adult Day HCBS Waiver; and
- Developmental Disabilities Adult Comprehensive Waiver (consolidated with the DD child waiver effective April 1, 2017).
The report also recommends that individuals in nursing facilities and assisted living homes be included from the outset, rather than delayed as some states have, to encourage meeting the state’s long-term care rebalancing goals and reduce incentives to avoid community-based settings.
Finally, the report recommends preserving Nebraska’s Program of All-Inclusive Care for the Elderly (PACE), which is available only in the Omaha area, as an option for individuals over 55.
Based on information provided by the state’s MLTSS Advisory Council in 2014, as well as historical data on I/DD waiver populations, we estimate the fully-implemented MLTSS population at more than 50,000 beneficiaries statewide. Federal fiscal year 2016 spending for LTSS services was more than $840 million, with a fairly even split between HCBS and institutional services.
Additional Models Considered
The LTSS redesign report considered two alternative models to the MLTSS approach: expanding Medicare ACO models or provider-led networks. The report concludes that expanded ACOs would not provide statewide coverage, nor do the existing ACOs in Nebraska have experience in providing LTSS to Medicaid beneficiaries. In fact, the report concluded that there is no active model anywhere in the country in which a standalone ACO is successfully providing Medicaid LTSS.
On the provider-led network approach, the report again notes that there is no existing program in which provider-led organizations are providing integrated MLTSS, although the report acknowledges that Alabama, Arkansas, and North Carolina are pursuing this model. Ultimately, the report concludes that DHHS could pursue this model if there were adequate interest and capacity among providers, but that provider-led networks would require significant assistance to get to a point where they could accept full-risk for the MLTSS population.
Timing, Next Steps
Nebraska DHHS will be holding a series nine listening sessions across the state over the next two weeks, between March 20 and March 30, with two public webinars scheduled for March 28 and 29. Public comments will be accepted through April 14, with a finalized LTSS redesign plan expected to be made public in May 2017. Based on this timeline, and assuming the state moves forward with the recommended MLTSS approach, the state’s three Heritage Health MCOs would begin providing mandatory MLTSS statewide to older adults and individuals with disabilities (Phase 1) as of January 1, 2019, with MLTSS to follow for individuals with I/DD (Phase 2) on July 1, 2019.
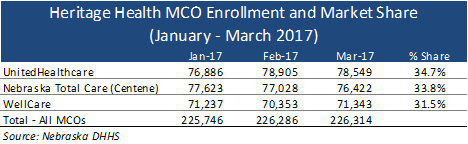
Current Heritage Health MCOs
Across the three Heritage Health MCOs, there are more than 226,000 Medicaid beneficiaries enrolled, with enrollment distributed fairly evenly across UnitedHealthcare, Centene’s Nebraska Total Care, and WellCare. Each plan has between 71,000 and 79,000 members, or between 31 percent and 35 percent of the total market.