This week, our In Focus section reviews two Medicaid managed care requests for proposals (RFPs) released on January 10, 2020. The District of Columbia Department of Health Care Finance (DHCF) issued an RFP for the DC Healthy Families Program (DCHFP); the District of Columbia Healthcare Alliance Program (Alliance); and the Immigrant Children’s Program (ICP) as part of a broader effort to fully transition Medicaid to managed care over the next five years. The new contracts will cover approximately 224,000 lives. Meanwhile, the Kentucky Cabinet for Health and Family Services (CHFS), Department for Medicaid Services (DMS) released a statewide Medicaid managed care RFP to serve approximately 1.2 million lives. In December 2019, Kentucky announced that it will cancel and rebid the current Medicaid managed care contracts.
DC Medicaid Managed Care RFP
In April 2019, the District of Columbia awarded contracts for the Medicaid program, DCHFP; the Alliance program, covering low-income adults not eligible for Medicaid; and the ICP, covering low-income immigrant children not eligible for Medicaid to incumbents AmeriHealth Caritas, Trusted Health Plan, and Anthem/Amerigroup. The three plans will continue to serve members through fiscal 2020, however, in September 2019, DC, announced that it would rebid the Medicaid contracts. The new contracts will cover approximately 224,000 lives, including 22,000 additional adults with Special Health Care Needs, formerly enrolled in Medicaid fee-for-service, effective October 1, 2020. DC intends to award contracts to up to three managed care organizations (MCOs).
The previous RFP, released in August 2018, came after an administrative law judge ruled in December 2017, that the District failed to treat all bidder’s equally and “undermined the integrity of the procurement process,” ordering DC to reevaluate the bids of the previous procurement.
Evaluation
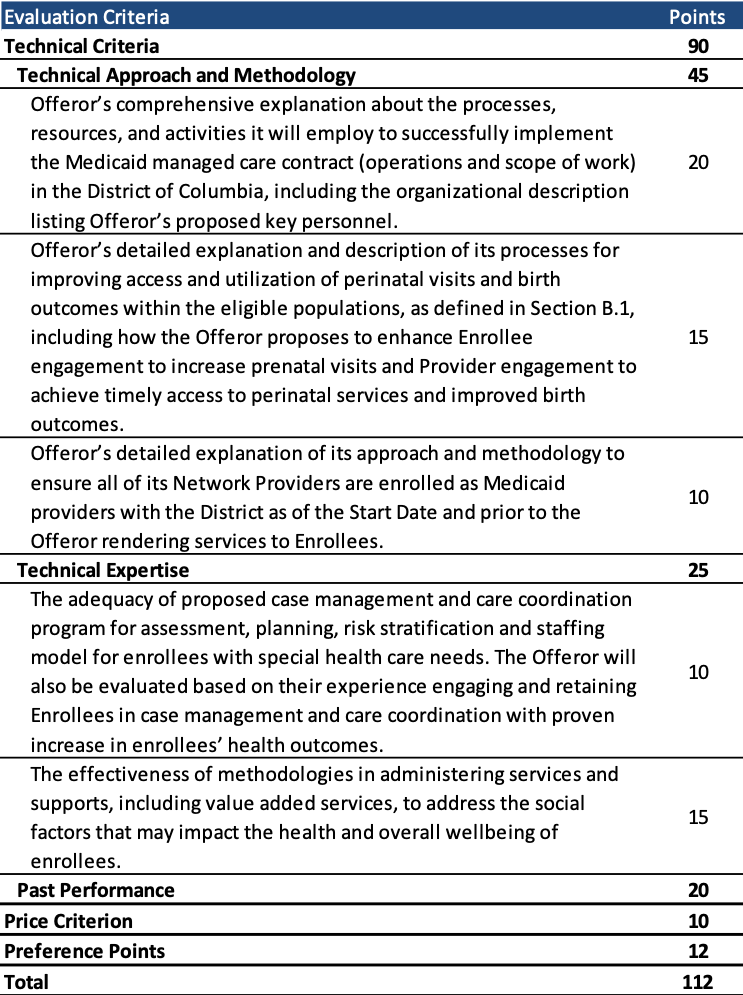
Proposals will be scored out of a total of 112 points, consisting of technical criteria, price, and preference points. The price evaluation is objective, with the lowest price receiving the maximum score.
Timeline
Proposals are due January 31, 2020. Contracts will run from October 1, 2020, through September 30, 2021, with four one-year renewal options.
Current Market
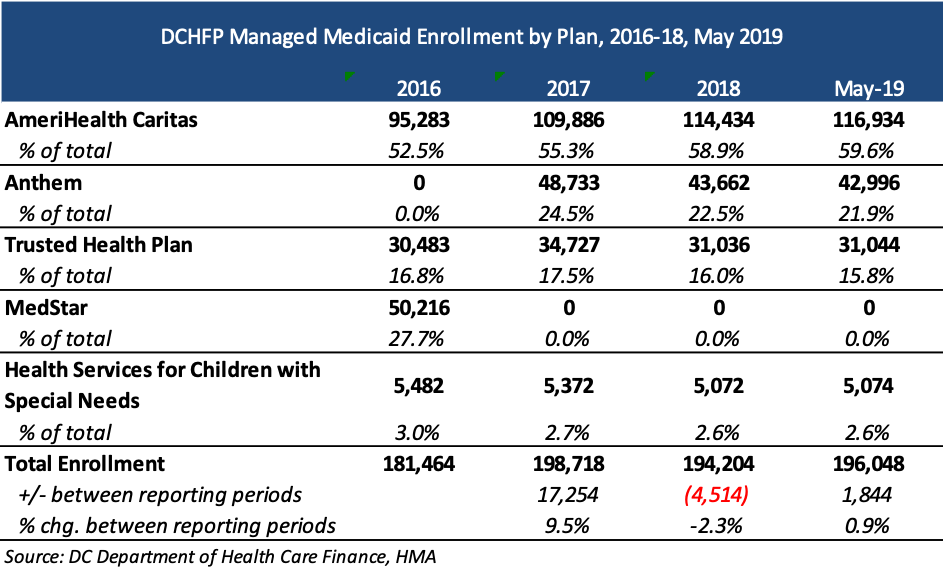
Current incumbents are AmeriHealth Caritas, Anthem, and Trusted Health Plan, serving 196,000 individuals as of May 2019. During this same period, there were also nearly 15,600 Alliance members, for which a breakout is unavailable.
Kentucky Medicaid Managed Care RFP
In November 2019, Kentucky awarded Medicaid managed care contracts to Aetna, Humana, Molina, UnitedHealthcare, and WellCare. The following month, the state announced it will cancel and rebid those contracts. Governor Beshear stated that the original RFP included a now cancelled section 1115 waiver, Kentucky HEALTH, that mandated Medicaid work requirements for certain individuals. The $8 billion contracts were awarded in the last 11 days of the former administration, with members of the General Assembly’s Government Contract Review Committee unanimously voting to reject the contracts in the last day. In a filed protest, one MCO called the award process “irretrievably defective.”
Under the new procurement, the state plans to contract with up to five Medicaid MCOs, effective January 2021. One of the selected MCOs will also contract to provide services for enrollees in foster care, Adoption Assistance, and Juvenile Justice under the Kentucky SKY (Supporting Kentucky Youth) program.
The state’s Medicaid managed care program has been enacted since November 2011 and has been statewide since January 2013. Newly selected MCOs will provide statewide Medicaid and Kentucky Children’s Health Insurance Program (KCHIP) coverage for:
- Families and Children
- SSI Adults without Medicare
- SSI Children
- Foster Care Children
- Dual Eligibles (Medicaid and Medicare eligible)
- ACA MAGI Adults
- ACA Former Foster Care Children
Aged, Blind, or Disabled (ABD) individuals will remain in Medicaid fee-for-service. They primarily reside in long term care facilities or are served by a home and community-based waiver program.
Two different rates will be developed for MCOs – one for plans in Region 3 and one for plans in Regions 1, 2, 4-8. Region 3 includes Bullitt, Carroll, Hardin, Henry, Jefferson, Larue, Marion, Meade, Nelson, Oldham, Shelby, Spencer, Trimble, and Washington counties.
Kentucky SKY (Supporting Kentucky Youth) Program
One of the winning MCOs will also be contracted to provide covered services, population health management, and care management services to foster care, adoption assistance, and juvenile justice enrollees under the Kentucky SKY (Supporting Kentucky Youth) program. The MCO will oversee and coordinate both physical and behavioral health, dental care, social services, and wraparound services in order to meet the intensive health care needs of the children.
Evaluation
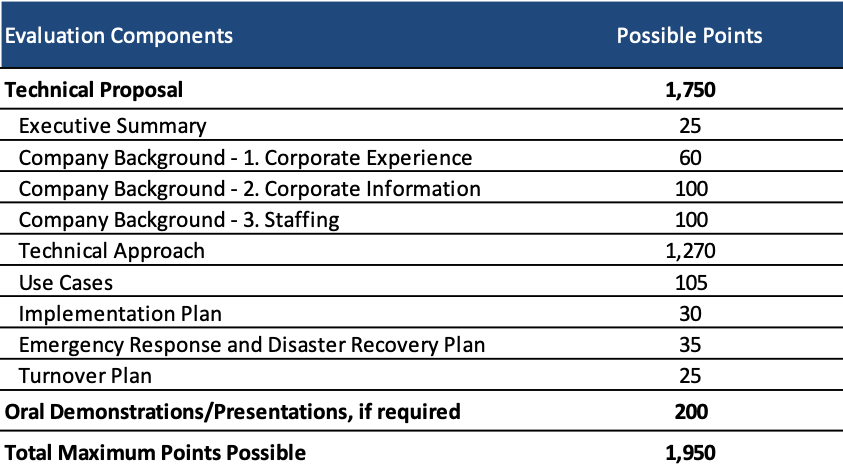
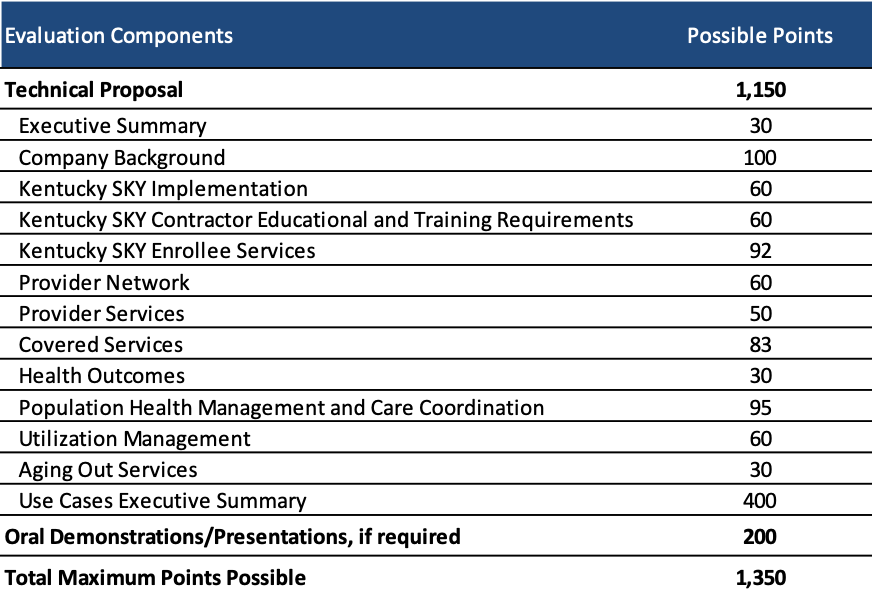
Medicaid managed care proposals will be scored out of a total 1,950 possible points. The technical proposal consists of 1,750 points and a possible oral demonstrations/presentation, worth 200 points, may be required.
MCOs may also submit a proposal for Kentucky SKY. The proposal will only be scored if the MCO is selected for a managed care contract.
Timeline
Proposals are due February 7, 2020. Contracts will run from January 1, 2021, through December 31, 2024, with six additional two-year renewal options.
Current Market
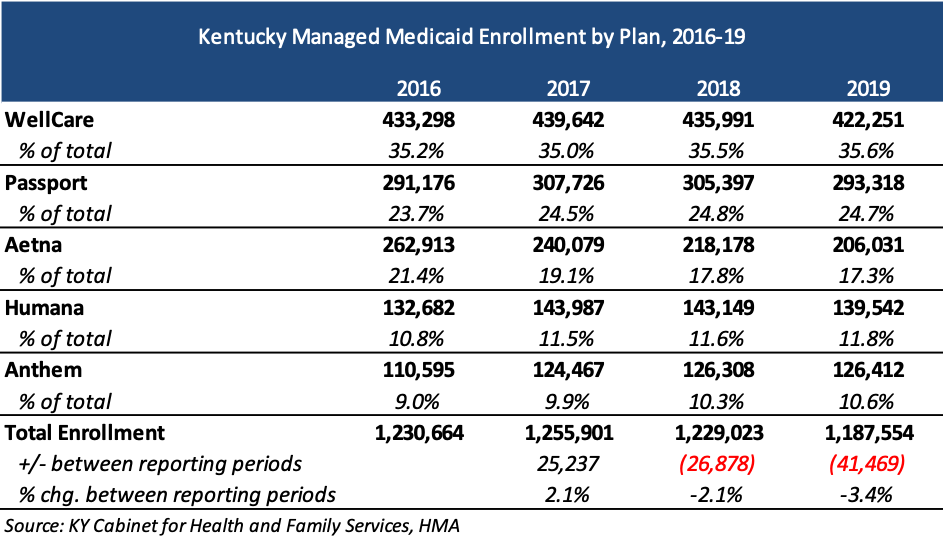
Current Medicaid incumbents are Aetna, Anthem, Humana, Passport, and WellCare, with a total of 1.2 million lives as of December 2019. WellCare has the largest market share, with 35.6 percent of enrollment.