This week, our In Focus section shares HMA’s takeaways from the Centers for Medicare & Medicaid Services (CMS) white paper on the CMS Innovation Center Strategy Refresh: Driving Health System Transformation – A Strategy for the CMS Innovation Center’s Second Decade.
The Strategy Refresh, released October 20, 2021, provides a comprehensive overview of lessons from the Innovation Center’s first decade, goals, and next steps in five identified strategic areas. It also shares new models or concepts that the Innovation Center is exploring. Several of the Innovation Center’s articulated approaches are reflective of recommendations in the Issue Brief, Center for Medicare and Medicaid Innovation: Recommendations for Future Direction, written by Health Management Associates (HMA) experts Jennifer Podulka, Yamini Narayan, and Lynea Holmes. The Strategic Refresh also highlights the imperative to include payers beyond Medicare, importantly Medicaid and commercial insurers, in models to achieve person-centered accountable and equitable care.
The five strategic objectives include:
- Driving accountable care that results in all Medicare enrollees and most Medicaid enrollees in a care relationship with accountability for quality and total cost of care by 2030.
- Embedding health equity in all models through mandatory reporting of demographic and, as appropriate, social determinants of health data, and including underserved populations and safety net providers in new models.
- Supporting innovation by strengthening patient engagement and person-centered measures across all models.
- Facilitating approaches and specific targets that address price and affordability for high-value care, including new approaches to cost-sharing and drug prices.
- Pursuing more collaborative and ongoing partnerships with a broader group of stakeholders to improve quality, achieve equitable outcomes and reduce healthcare costs, and allow for multi-payer alignment in new models by 2030.
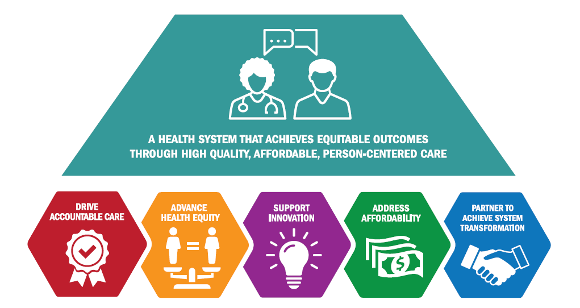
Source: The Centers for Medicare & Medicaid Services
As laid out in the strategy document, all stakeholders will be engaged and included in the Innovation Center’s work in the decade ahead. For some partners, this will happen directly through participation in a model. For others, the Innovation Center is expecting transformation as expectations are reshaped with input from all stakeholders, broader dissemination of actionable tools and information occurs, and patient engagement becomes more common throughout the healthcare system. The Innovation Center intends to use the new objectives to streamline and reduce the number of ongoing models in a way that drives toward health equity, simplicity in design and participation, and affordability in and outside of the model.
Our top takeaways from the strategy document include:
- Health equity will be embedded in all of CMS and the Innovation Center’s work – from rethinking and developing models to its pursuit of tools and opportunities that are more inclusive of underserved populations and providers. CMS will apply a health equity lens to streamline and reduce competing models, address misaligned incentives, and include populations that could benefit from accountable and value-based healthcare delivery.
- Future models will focus on integrating whole-person care, and several are likely to include a total cost of care approach. The Innovation Center points to behavioral health, palliative care, and care for people with complex needs and serious illness as areas that can be explored for greater integration with primary care and provide significant opportunity to improve care and outcomes while reducing overall costs. It plans to test payment and regulatory flexibilities for model participants that can support the provision of home or community-based care. The strategy also signals that the Innovation Center is further along in its thinking about models that test affordability and cost structures for prescription drugs in Medicare.
- A variety of new engagement opportunities and tools, such as dashboards, could be available to assist a broader group of stakeholders in becoming accountable care entities. In particular, the Innovation Center intends to be more purposeful in its engagement strategy to gather ongoing input from safety net providers and others who have not previously participated in the Innovation Center’s models. This approach could enable the Innovation Center – and partners – to be more supportive of accountable care and innovation for specific populations, for example the Medicare and Medicaid dually eligible population and individuals who can benefit from home and community-based services.
- A tailored approach to facilitate provider participation in new – and possibly existing — models will be employed, where possible. In particular, the Innovation Center shared its intent to support and work with providers regardless of their starting point, current capacity to obtain and use actionable data, and financial constraints that may impede them from assuming risk and advancing higher quality care for the individuals they serve. Beyond participation, stakeholders must also be prepared to demonstrate their success which will become clearer as CMS updates quality and outcomes measures for reporting.
- Medicare alone cannot drive healthcare transformation. While the Innovation Center’s strategy commits to strengthening Medicare-specific alternative payment models (APMs), it also calls for collaboration with states, particularly state Medicaid programs, and commercial payers. Multi-payer alignment has proved challenging for CMS over the past ten years, but the lessons learned and articulated openness for renewed communication with states and payers could provide a new pathway for making progress on system transformation. The Innovation Center is also positioning itself to drive greater collaboration within CMS as well as other partners within the Department of Health and Human Services administering public healthcare programs, including the Food and Drug Administration (FDA), the Indian Health Service (IHS), and the Administration for Community Living (ACL).
The Innovation Center will soon hold listening sessions with stakeholders and reinvigorate its work with and input from the Learning Action Network (LAN). If the Innovation Center is successful in changing the focus of conversations and opportunities for collaboration, this could lead to higher expectations for Medicaid and Medicare fee-for-service providers and plans, as well as commercial payers.
HMA staff have extensive experience in assessing the implications of Innovation Center opportunities. If your organization is interested in assessing its opportunities, contact our subject matter experts to learn how our team can assist with a data-based consultation.
