This week our In Focus reviews the Missouri MO HealthNet (MHD) Medicaid Managed Care Program request for proposals (RFP), released on November 19, 2021, by the Department of Social Services (DSS). The MHD managed care program serves about 850,000 Medicaid and Children’s Health Insurance Program (CHIP) members including the state’s newly implemented Medicaid expansion population, across all regions of Missouri. Missouri’s General Plan managed care program covers TANF, CHIP, expansion and similar eligibility groups but does not include individuals with disabilities or those over age 65. The RFP also contains a separate section for a single, statewide Specialty Plan for foster children and children receiving adoption subsidy assistance. Managed care organizations must bid on and win a General Plan contract in order to be eligible for the Specialty Plan contract.
Program Goals
DSS noted nine guiding principles for the MHD Managed Care program:
- All members must be linked with a primary care provider
- Wellness/prevention of disease
- Chronic care management/care management
- Utilization of the appropriate setting at the right cost
- Emphasis on the individual person
- Evidence-based guidelines for improved quality of care and use of resources
- Encouragement of responsibility and investment on the part of the member to ensure wellness
Participation in the Medicaid Reform and Transformation Program, which includes personal responsibility (member incentives), the Local Community Care Coordination Program (LCCCP) initiative, state provider incentive program, Value-Based Purchasing Strategies, and requirements for increased accountability and transparency (see section below for additional information)
Ensuring that the needs of vulnerable Missourians are addressed in a financially sustainable manner
Medicaid Reform and Transformation Program
The Medicaid Reform and Transformation Program is designed to engage members, providers, and health plans in transforming the service delivery system and increasing accountability and transparency.
Health plans will offer member incentives to promote responsible behavior and encourage efficient use of health care services. Plans will be required to ensure 15 percent of eligible members participate in the incentive program. Additionally, plans will use the state provider incentive program to improve health outcomes, promote delivery of trauma informed care, decrease inappropriate utilization of services, and decrease health risk factors.
Health plans will need to develop a Local Community Care Coordination Program (LCCCP) to be implemented no later than July 1, 2022, using any delivery model that focuses on providing care management, care coordination, and disease management through local healthcare providers. This can include accountable care organizations (ACOs), patient-centered medical homes (PCMHs), primary care management (PCCM), or other models approved by the state agency.
Plans will also implement value-based models and purchasing strategies. These provider payment or delivery system design strategies will incorporate performance and quality initiatives.
Additionally, health plans will participate in the Show Me ECHO (Extension for Community Healthcare Outcomes) project, a telehealth program connecting interdisciplinary teams of experts with primary care providers and other professionals to improve patient care access, quality and efficiency.
Specialty Health Plan
The Specialty Health Plan for Children and Youth in the Care and Custody of the State combines select behavioral health services into a single, specialized health plan for children in the custody of DSS and children receiving adoption subsidy assistance. The plan establishes a trauma-informed, comprehensive, and integrated behavioral health and physical health delivery system. Approximately 40,000 children and youth will be enrolled in this Specialty Plan.
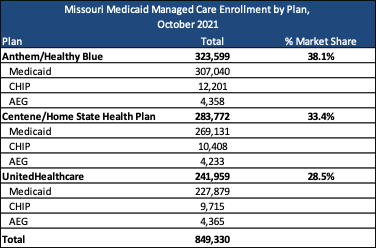
Current Market
Current incumbents are Anthem/Healthy Blue, Centene/Home State Health Plan, and UnitedHealthcare, serving 849,330 members as of October 2021. Anthem has the highest market share by enrollment at 38.1 percent.
Timeline
The RFP was released on November 19, 2021, with proposals due by December 29. The contract will be effective for one year with four one-year renewal options. Current contracts expire June 30, 2022. Fiscal year 2023 managed care payments are estimated to be $2 billion.
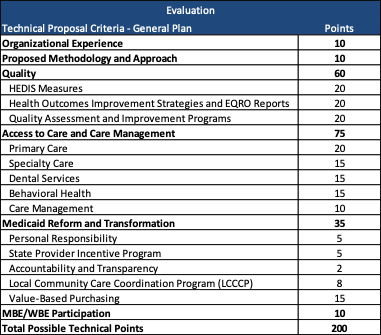
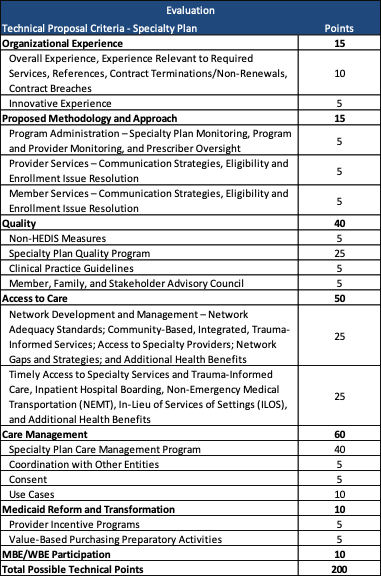
Evaluation
Technical proposals for the general and the specialty plans will each be scored out of 200 points, as shown below. DSS will award no more than three plans for the General Plan Managed Care Program and will award one plan for the Specialty Plan Managed Care Program.