This week, our In Focus section reviews the Mountain Health Promise request for proposals (RFP) released by the West Virginia Department of Health and Human Resources on September 30, 2022, for specialized Medicaid managed care for children and youth in foster care.
Mountain Health Promise RFP
The selected managed care organization (MCO) will provide physical and behavioral health services to children and youth in the foster care system, individuals receiving adoption assistance, youth formerly in foster care up to age 26 who aged out of foster care while on Medicaid in the state of West Virginia, and children eligible under the children with serious emotional disorders (CSED) waiver. Potential expansions could include, but are not limited to, children at risk for foster care placement and the family of youth in crisis. Additionally, the MCO will act as an administrative services organization (ASO) and provide statewide administrative services for all individuals accessing socially necessary services (SNS).
Some of the goals of the program include:
- Enhance coordination and access to services
- Enhance quality of care and minimize barriers for youth and families/improve access to treatment
- Reduce fragmentation and offer seamless continuity of care
- Improve health and social outcomes for youth and impacts on families
- Help reduce the number of children removed from the home and reduce lengths of stay per episode of care through increased family-centered care that provides necessary and coordinated services to all members of the family
- Decrease children involved with the juvenile justice and corrections systems
- Reduce out-of-home and out-of-state placements
- Develop new or enhance existing services, such as children’s mobile crisis response (CMCR), inState Psychiatric Residential Treatment Facilities (PRTF) to reduce the need for out-of-state placements, and intensive home-based treatment
Physical and behavioral health services will be reimbursed through a Medicaid per member per month (PMPM) capitation payment. For SNS administration, the Bureau for Social Services (BSS) will provide a fixed monthly rate. The PMPM capitation rate will not include carved out SNS costs.
It is encouraged, but not required, that the MCO subcontract with regional child welfare organizations, residential mental health treatment facilities (RMHTFs), and organizations that provide home and community-based services for children with serious emotional disorders to assist in the care coordination of services for this population.
Market
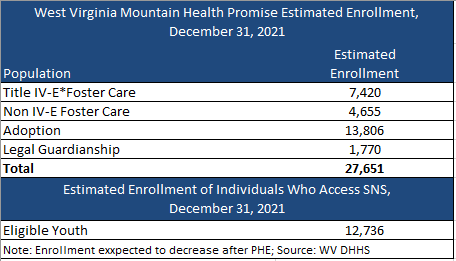
There are nearly 28,000 individuals currently enrolled in Mountain Health Promise, with about 13,000 eligible for SNS. Enrollment, however, is expected to decrease following the end of the Public Health Emergency (PHE). CVS Health/Aetna is the incumbent plan. Aetna had contracted with Kepro to serve as the ASO for SNS.
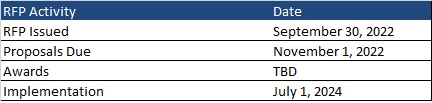
Timeline
Proposals are due November 1, 2022. The contract is anticipated to run from July 1, 2024, through June 30, 2025, with three one-year options.
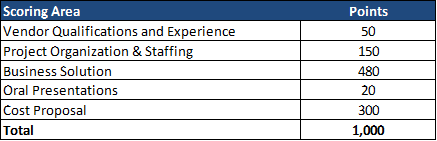
Evaluation
The winning MCO will be chosen based on the highest score of a possible total 1,000 points. The technical evaluation will be a total of 700 of 1,000 points. Cost represents 300 of 1,000 total points.