This week's roundup:
- In Focus: CMS Introduces Significant Proposed Changes to Medicare Advantage and Medicare Prescription Drug Benefit Programs for 2024
- California to Transition Dual Eligibles in 31 Counties to Medi-Cal Managed Care Plans in January 2023
- Georgia Receives Approval for 2 State-Directed Payment Programs
- Hawaii Governor Proposes Medicaid Provider Reimbursement Rate Increases
- Iowa Releases Medicaid Enterprise Systems RFI
- Idaho Looks to Expand Access to Crisis Services for Individuals with Developmental Disabilities
- Indiana Releases Medicaid NEMT RFP
- New Mexico Proposes 16 New Programs in Section 1115 Medicaid Waiver Renewal Application
- New York Medicaid Pharmacy Carve-Out Could Cost $400 Million More Annually, Wakely Report Finds
- Oregon Governor-Elect to Appoint James Schroeder as Interim Director of OHA
- Puerto Rico to Receive $17.6 Billion in Medicaid Funding Over 5 Years Under Omnibus Spending Bill
- Vermont Considers Punitive Cuts to 2023 All-Payer ACO Budget
- Washington Receives Federal Approval to Offer Exchange Plans to Non-Citizens
- Medicaid Eligibility Redeterminations to Begin April 2023 Under Omnibus Spending Bill
- Rise Health Secures Investments from Lorient Capital, Martis Capital
The next HMA Weekly Roundup will be January 11, 2023.
In Focus
CMS Introduces Significant Proposed Changes to Medicare Advantage and Medicare Prescription Drug Benefit Programs for 2024
This week, our In Focus section reviews a rule proposed by the Centers for Medicare & Medicaid Services (CMS) on December 14, 2022, that would revise regulations governing Medicare Advantage (MA or Part C), the Medicare Prescription Drug Benefit (Part D), Medicare cost plans and Programs of All-Inclusive Care for the Elderly (PACE).
Background
The proposed rule reflects the agency’s focus on increasing transparency, improving health equity, reducing the cost of care, and improving access to behavioral health services. Collectively, these are among the most impactful policy changes CMS has proposed to the MA and Part D programs in recent years. CMS also writes that many of the policy proposals are informed by public comments to the agency’s earlier requests for input.
MA and Part D stakeholders will want to consider providing feedback and analysis to CMS regarding the impact of these changes. The changes would begin to take effect for contract year 2024, but stakeholders can begin gap assessments and strategic planning now. Comments on the proposed rule are due by February 13, 2023.
Increased Transparency in Utilization Management and Marketing Policies
The rule proposes to increase the transparency of MA plans’ utilization management and prior authorization policies, with the goal of ensuring that MA enrollees receive the same access to medically necessary care they would receive in Traditional Medicare.
- CMS proposes that MA organizations must include current evidence in widely used treatment guidelines or clinical literature made publicly available to CMS, enrollees, and providers when creating internal clinical coverage criteria, in situations when no applicable Medicare statute, regulation, National Coverage Determinations (NCD), or Local Coverage Determinations (LCD) establishes when an item or service must be covered.
- The proposed rule also would streamline prior authorization requirements, including adding continuity of care requirements in ongoing care for beneficiaries by requiring that when an enrollee is granted prior authorization approval it will remain valid for the full course of treatment.
- The rule would require all MA plans to establish a Utilization Management Committee to review policies annually and ensure consistency with Traditional Medicare’s national and local coverage decisions and guidelines.
The proposed rule also takes steps to address potentially misleading marketing while also ensuring that Medicare beneficiaries have accurate information to make coverage choices.
Increased Focus on Health Equity and Culturally Competent Care
The prosed rule includes several policies designed to increase health equity across the program.
- In addition to a number of other changes in the Star Ratings program, which measures the quality of care across MA and Part D plans, the proposed rule introduces a health equity index (HEI) reward, beginning with the 2027 plan year. This reward will use data from 2024 and 2025 and is intended to further encourage MA and Part D plans to improve care for enrollees with certain social risk factors (dual eligibility, low-income subsidies, and disability).
- CMS also proposes clarification of a current requirement for MA organizations to expand the list of populations that they must provide services to in a culturally competent manner.
- CMS proposes requiring MA organizations to develop and maintain procedures to offer digital health education to enrollees to improve access to medically necessary covered telehealth benefits.
- In addition, CMS proposes requiring MA organizations to include providers’ cultural and linguistic capabilities in provider directories.
- CMS proposes that MA organizations must address health disparities as part of existing requirements to develop and maintain quality improvement programs.
- CMS also proposes to specify in Medicare regulations that MA organizations, cost plans, and Part D sponsors must provide materials to enrollees on a standing basis in any non-English language that is the primary language of at least 5 percent of the individuals in a plan benefit package service area or accessible format using auxiliary aids and services upon receiving a request for the materials or otherwise learning of the enrollee’s preferred language and/or need for an accessible format using auxiliary aids and services. The agency also proposes to extend this requirement to individualized plans of care for special needs plans.
Improving Access to Behavioral Health
CMS proposes policies to strengthen network adequacy requirements and reaffirms the responsibility of MA organizations to provide behavioral health services.
- Specifically, CMS proposes to specify certain types of mental health professionals as specialty types for which there are specific minimum standards and on which MA networks are evaluated by CMS; amend general access to services standards to explicitly include behavioral health services; codify standards for appointment wait times for both primary care and behavioral health services; clarify that the emergency medical services that must not be subject to prior authorization include behavioral health services to evaluate and stabilize an emergency medical condition; require that MA organizations notify enrollees when the enrollee’s behavioral health or primary care provider(s) are dropped midyear from networks; and require MA organizations to establish care coordination programs, including coordination of community, social, and behavioral health services.
- CMS also proposes to require organizations to identify certain providers waived to treat patients with medications for opioid use disorder (MOUD) in their provider directories.
Improving Drug Affordability and Access in Part D
CMS proposes greater formulary flexibility for MA and Part D plans for certain biological products and authorized generics. CMS proposes to permit Part D sponsors to immediately substitute: (1) a new interchangeable biological product for its corresponding reference product; (2) a new unbranded biological product for its corresponding brand name biological product; and (3) a new authorized generic for its corresponding brand name equivalent.
In addition, CMS proposes several new requirements for Part D sponsors related to Medication Therapy Management (MTM) programs.
- Part D sponsors are required to provide an MTM program that ensures Part D drugs are appropriately used to optimize health outcomes through improved medication use and to reduce the risk of adverse events.
- CMS is proposing several changes to MTM eligibility criteria with the goal of promoting more consistent, equitable, and expanded access to MTM services.
Making Permanent the Limited Income Newly Eligible Transition (LI NET) Program
The LI NET program currently operates as a demonstration program that provides immediate and retroactive Part D coverage for eligible low-income beneficiaries who do not yet have prescription drug coverage. In this proposed rule, CMS proposes making the LI NET program a permanent part of Medicare Part D, as required by statute.
Expanding Low-Income Subsidies Under Part D
CMS proposes to implement a section of the Inflation Reduction Act (IRA), enacted in August 2022, which expands eligibility under the Part D low-income subsidy (LIS) program. Under the provision, individuals with incomes up to 150 percent of the federal poverty level (FPL) and who meet statutory resource requirements will qualify for the full low-income subsidy beginning on or after January 1, 2024. This change will provide the full subsidy to those who currently qualify for only a partial subsidy.
Strengthening Current Policies for MA Plans Serving Populations with Special Needs
The proposed rule includes several proposals to codify existing policies that govern special needs
plans (SNP), which are MA plans specifically designed to provide targeted care and limit enrollment to special needs individuals. Specifically, CMS proposes to codify recent statutory requirements concerning the definition of severe or disabling chronic condition and several other provisions relating to the definition of a Chronic Condition SNP. The rule also proposes several updates to policies governing Programs of All-Inclusive Care for the Elderly (PACE), including technical changes to PACE contracting and application evaluation processes, requirements for medical clearance of PACE personnel, requirements for contracting for specialty services, and codification of certain care planning and care coordination requirements.
The HMA Medicare team will continue to analyze these proposed changes. We have the depth and breadth of expertise to assist with tailored analysis, to model policy impacts, and to support the drafting of comment letters to this rule.
If you have questions about the contents of CMS’s Medicare Advantage proposed rule and how it will impact MA plans, providers, and patients, please contact John Richardson ([email protected]), Julie Faulhaber ([email protected]), Amy Bassano ([email protected]), or Andrea Maresca ([email protected]).
HMA Roundup
California
California Releases Residency Program for SUD Treatment RFA. The California Department of Health Care Services released on December 20, 2022, a request for applications (RFA) for nearly $3.4 million in grant funding to implement the California Residency Program Collaborative, which aims to expand physician capacity to treat substance use disorder (SUD) and opioid use disorder. Each applying organization can receive up to $70,000 in funds, which will be distributed between January 1, 2023, and June 30, 2024. Read More
California to Distribute $12 Million in Grants for Youth OUD. The California Department of Health Care Services announced on December 14, 2022, that it will distribute $12 million in grants to organizations to tackle youth opioid use disorder (OUD). Grants, ranging from $50,000 to $500,000, will support prevention, treatment, and recovery services for youth with, or at risk of, OUD. The grants are part of the California Medication-Assisted Treatment Expansion Project. Read More
California to Transition Dual Eligibles in 31 Counties to Medi-Cal Managed Care Plans in January 2023. The California Medical Association announced on December 13, 2022, that the California Department of Health Care Services will transition Medicare-Medicaid dual eligibles in 31 counties to Medi-Cal managed care, effective January 1, 2023, as part of the CalAIM initiative. Approximately 325,000 beneficiaries will be impacted. The transition, intended to improve care coordination, will not impact Medicare coverage, benefits, or providers. Currently, more than 70 percent of dual eligibles in the state are enrolled in Medi-Cal managed care plans. Read More
Georgia
Georgia Receives Approval for 2 State-Directed Payment Programs. The Georgia Department of Community Health announced on December 16, 2022, that it had received federal approval for two state-directed payment programs. The Strengthening the Reinvestment Of a Necessary-workforce in Georgia and the Private Hospital Directed Payment Program will direct approximately $900 million toward supporting eligible teaching hospitals and private acute-care hospitals. Read More
Hawaii
Hawaii Governor Proposes Medicaid Provider Reimbursement Rate Increases. Kaua’i Now News reported on December 19, 2022, that Hawaii Governor Josh Green is proposing Medicaid provider reimbursement rate increases in the state’s fiscal 2023-25 biennium budget. Additional funds would also be available for homeless services and outreach programs, expansion of the intensive care and medical surgical units at Hilo Medical Center, and nursing and medical-related programs at University of Hawaii campuses and community colleges. Read More
Iowa
Iowa Reaches $44.4 Million Settlement with Former Pharmacy Benefit Manager. Iowa Attorney General Tom Miller announced on December 15, 2022, a $44.4 million settlement with Centene/Envolve over allegations that it overbilled the state’s Medicaid program for pharmacy benefits and services. The settlement will be split between Iowa and the Federal Medicaid program. Centene operates Iowa Total Care, a managed care organization for the state Medicaid program.
Iowa Releases Medicaid Enterprise Systems RFI. The Iowa Department of Health and Human Services released on December 14, 2022, a request for information (RFI) seeking responses regarding integration services and solutions that can be used to support Medicaid Enterprise Systems delivery transformation. Responses are due on February 3, 2023. Read More
Idaho
Idaho Looks to Expand Access to Crisis Services for Individuals with Developmental Disabilities. The Idaho Department of Health and Welfare announced on December 16, 2022, that it will seek federal approval to use Medicaid funds to support increased access to crisis services for individuals with developmental disabilities. New components would include residential treatment (including a stabilization unit for individuals in crisis requiring care and a step-down housing setting for individuals transitioning back into the community); specialized clinical teams; and increased community capacity building. Read More
Indiana
Indiana Releases Medicaid NEMT RFP. The Indiana Family and Social Services Administration released on December 13, 2022, a request for proposals (RFP) for Non-Emergency Medical Transportation (NEMT) services for the state’s Medicaid fee-for-service (FFS) populations. The state will award a four-year contract with two, one-year renewal options. The current FFS NEMT provider is Southeastrans, and Indiana had 348,000 FFS enrollees in November 2022. Part one of the proposals are due by February 14, 2023, and part two is due February 17. Read More
Minnesota
Minnesota Is Accepting Grant Applications for HCBS Providers in Rural Communities. The Minnesota Department of Human Services announced on December 19, 2022, that grants of $100,000 to $250,000 are available for providers of home and community-based services (HCBS) in rural and under-served communities. Applications will be accepted from December 12 through January 17. The state will also distribute $4 million in grants to 12 organizations to support technology that will help beneficiaries keep medical appointments, connect with HCBS, and combat social isolation. Read More
Montana
Montana Governor Proposes Increase to Medicaid Reimbursement Rates for Nursing Facilities. The Daily Montanan reported on December 16, 2022, that Montana Governor Greg Gianforte is proposing an increase in Medicaid per diem rates for nursing facilities. However, the proposed increase would be less than the amount recommended by a state-sponsored rate survey prepared by Guidehouse. Read More
New Mexico
New Mexico Community-Based Organizations Receive $1.1 Million from UnitedHealthcare to Address Social Determinants of Health. UnitedHealthcare announced on December 16, 2022, an investment of more than $1.1 million to community-based organizations in New Mexico to address social determinants of health, including funding for food and housing security, education and training, maternity care, rural care, and behavioral health. Read More
New Mexico Proposes 16 New Programs in Section 1115 Medicaid Waiver Renewal Application. The Santa Fe New Mexican reported on December 16, 2022, that the New Mexico Human Services Department asked federal regulators to renew its Section 1115 Medicaid waiver for five more years, including 16 new covered initiatives. The renewal request, submitted to the Centers for Medicare & Medicaid Services (CMS), proposes continuous Medicaid coverage for children up to age six, home visiting programs for new parents, housing supports following inpatient or emergency care, and home-delivered meals. The waiver would also cover medication-assisted treatment for incarcerated individuals for 30 days before release and provide a 30-day supply of medication after release. The state’s current 1115 waiver is set to expire on December 31, 2023. In September 2022, New Mexico released a request for proposals for the state’s Medicaid managed care program called Turquoise Care, previously Centennial Care. Read More
New Mexico Requests $1.6 Billion for Fiscal 2024 to Improve Medicaid Program, Behavioral Health Initiatives. The New Mexico Human Services Department (HSD) announced on December 14, 2022, it is requesting a budget of $1.6 billion for fiscal 2024, a 14.4 percent increase over fiscal 2023. The request includes funding for continuous enrollment for children up to age six, a medical respite housing program for people experiencing homelessness, and home-delivered meals for individuals in the community benefit program. The budget will also fund behavioral health initiatives, like implementing Certified Community Behavioral Health Clinics and raising non-Medicaid behavioral health reimbursement rates from 85 percent of Medicaid to 100 percent. Read More
New York
New York Medicaid Pharmacy Carve-Out Could Cost $400 Million More Annually, Wakely Report Finds. Health Payer Specialist reported on December 16, 2022, that the New York Department of Health’s plan to carve-out pharmacy services from managed care could cost $400 million more annually than the current system, according to a report from Wakely, an HMA Company. The initiative, NYRx, would create a single state-run fee-for-service pharmacy plan for Medicaid members and is scheduled to begin on April 1, 2023. Currently, Medicaid plans use their own pharmacy benefit managers. Read More
Oklahoma
Oklahoma to Allocate $52 Million in Supplemental Medicaid Hospital Payments. The Journal Record reported on December 15, 2022, that $52 million will be allocated across participating Oklahoma hospitals through the Medicaid Supplemental Hospital Offset Payment Program by the end of 2022. The program provides supplemental payments to compensate hospitals for the difference between Medicaid reimbursements and the actual cost of services. Read More
Oregon
Oregon Governor-Elect to Appoint James Schroeder as Interim Director of OHA. The Oregon Capital Chronicle reported on December 14, 2022, that Oregon Governor-elect Tina Kotek plans on appointing James Schroeder, chief executive of Health Share of Oregon, as interim director of the Oregon Health Authority (OHA) on January 10, 2023. Patrick Allen is the current director. Read More
Puerto Rico
Puerto Rico to Receive $17.6 Billion in Medicaid Funding Over 5 Years Under Omnibus Spending Bill. NBC News reported on December 20, 2022, that the fiscal 2023 Omnibus Appropriations bill released by Congress provides more than $17.6 billion in Medicaid funding for Puerto Rico over the next five years. The bill would increase the federal government’s share of Medicaid costs in Puerto Rico to 76 percent. Read More
Vermont
Vermont Considers Punitive Cuts to 2023 All-Payer ACO Budget. VTDigger reported on December 19, 2022, that Vermont’s Green Mountain Care Board will vote on a proposed 1.5 percent punitive cut to the $15.2 million organizational budget of OneCare Vermont, a not-for-profit, all-payer accountable care organization (ACO) that is part of the University of Vermont Health Network. Board chair Owen Foster proposed the 2023 budget cut, citing a lack of health-related performance measures. Blue Cross Blue Shield of Vermont also announced it would end its relationship with the ACO, citing a lack of tangible quality outcomes and inability to bend the cost curve. Read More
Washington
Washington Receives Federal Approval to Offer Exchange Plans to Non-Citizens. Becker’s Payer Issues reported on December 16, 2022, that Washington received federal approval of a Section 1332 waiver application, allowing the state to offer health and dental Exchange plans to anyone regardless of immigration status, effective 2024. More than 105,000 individuals, representing 23 percent of the state’s uninsured population, will be able to access Exchange coverage. Read More
Wisconsin
Wisconsin Awards $17.3 Million in HCBS Grants. WSAW reported on December 15, 2022, that the Wisconsin Department of Health Services announced the final 26 awardees for the Medicaid home and community-based services (HCBS) grant opportunity. There are 69 awardees receiving a total of $17.3 million. The funding is available through the American Rescue Plan Act. Read More
National
Medicaid Eligibility Redeterminations to Begin April 2023 Under Omnibus Spending Bill. Congress released on December 20, 2022, a fiscal 2023 Omnibus Appropriations bill, which would require states to begin Medicaid eligibility redeterminations on April 1, 2023 and end enhanced FMAP on December 31, 2023. The bill also includes a two percent cut to Medicare reimbursement rates; an extension of postpartum Medicaid eligibility through 2029; and funding of $1 billion for Mental Health Block Grants, $383 million for Certified Community Behavioral Health Clinics, and $4.9 billion to address opioid misuse. Under the bill, Medicaid and Children’s Health Insurance Programs (CHIP) would be required to provide a year of continuous coverage for children under age 19 and develop coverage plans for justice-involved populations. Medicaid managed care entities would be required to maintain an online network of providers, effective July 2025. Additionally, the bill provides five years of funding for Medicaid in Puerto Rico and permanent funding for coverage in other U.S. territories. A continuing resolution extended the deadline for passing the bill to December 23, 2022. Read More
CMS Calls For Increase Oversight of Medicaid EPSDT Program, OIG Report Finds. Bloomberg Law reported on December 20, 2022, that the U.S. Office of the Inspector General (OIG) is calling for improved oversight of the Medicaid Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) program by the Centers for Medicare & Medicaid Services (CMS), after a report found discrepancies between Medicaid claims data and medical documentation for lead toxicity among children in five states. OIG also requested CMS remind state Medicaid programs of the requirements of the EPSDT program. Read More
Congress Proposes Extending Medicare Telehealth Flexibilities Through 2024 in Omnibus Spending Bill. The Associated Press reported on December 20, 2022, that the fiscal 2023 Omnibus Appropriations bill released by Congress would extend Medicare telehealth flexibilities that were implemented during the COVID-19 pandemic through 2024. Congress also plans to study telehealth and telehealth fraud. Read More
HHS Releases Ownership Information on All Medicare-Certified Hospitals. The U.S. Department of Health and Human Services (HHS) released on December 20, 2022, ownership information on all Medicare-certified hospitals for the first time. There are more than 7,000 hospitals that are certified to participate in Medicare. Read More
CMS Releases Public Comments for Access to Coverage, Care in Medicaid, CHIP RFI. The Centers for Medicare & Medicaid Services (CMS) released on December 20, 2022, a report summarizing public comments received in response to the 2022 request for information (RFI): Access to Coverage and Care in Medicaid & the Children’s Health Insurance Program (CHIP). Common themes included equity and cultural competence, provider reimbursements, payment compliance, and improved communications with beneficiaries seeking coverage. Read More
CMS Releases 2023 Basic Health Program Federal Funding Methodology Final Rule. The Centers for Medicare & Medicaid Services (CMS) released on December 16, 2022, the 2023 Basic Health Program Federal Funding Methodology Final Rule, which provides the information necessary to determine federal payment amounts for states that elect to establish a Basic Health Program. The Basic Health Program allows states to offer healthcare coverage for low-income individuals who churn in and out of Medicaid and the Children’s Health Insurance Program. States with a Basic Health Program are eligible to receive federal funds equal to 95 percent of the premium tax credits and cost sharing reductions otherwise available to enrollees through the Exchange. The rule will remain in effect until CMS proposes and finalizes a new Basic Health Program payment methodology. Read More
CMS Proposes Rule to Streamline MA Prior Authorization, Prevent Deceptive Marketing. Fierce Healthcare reported on December 15, 2022, that the Centers for Medicare & Medicaid Services (CMS) proposed a rule that requires Medicare Advantage (MA) plans to streamline prior authorization requirements and would ban MA plan ads from using confusing language or imagery that make it appear as though they are produced by the government. The rule also proposes adding health equity measures to the Star ratings and a requirement that MA plans review utilization management policies annually. Read More
Medicaid, CHIP Enrollment Nears 90 Million in July 2022, MACPAC Says. The Medicaid and CHIP Payment and Access Commission (MACPAC) announced on December 15, 2022, that almost 90 million individuals were enrolled in Medicaid and Children’s Health Insurance Program (CHIP) as of July 2022, a 7.2 percent increase from 2021, according to the 2022 Medicaid and CHIP Data Book. Medicaid spending in fiscal 2021 neared $753 billion, an increase of 9.6 percent from 2021, and CHIP spending was just above $21 billion, a 6.7 percent increase from 2021. Read More
Industry News
SavaSeniorCare to Cease Operations in January 2023. Skilled Nursing News reported on December 20, 2022, that SavaSeniorCare will transition its five remaining nursing homes to local operators and cease operations in January 2023. Sava operated 92 facilities as of September 2022. Read More
Rise Health Secures Investments from Lorient Capital, Martis Capital. Rise Health announced on December 19, 2022, investments by Lorient Capital and Martis Capital to expand in the southwestern United States. Rise Health, which was founded in 2021, uses technology to operate and support value-based primary care clinics. Read More
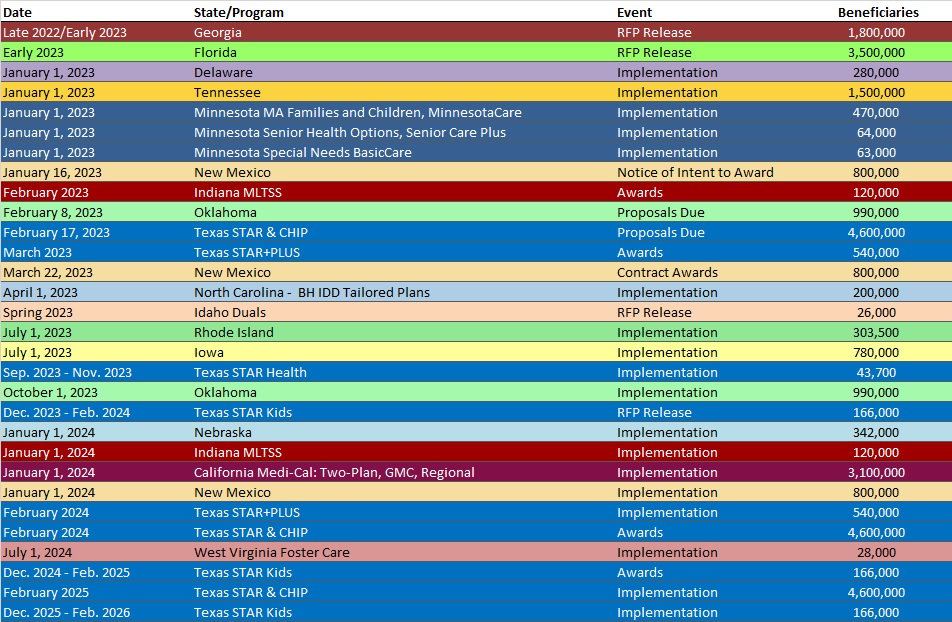
RFP Calendar
HMA News & Events
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Colorado RAE Enrollment is Up 6.4%, Oct-22 Data
- New Jersey Medicaid Managed Care Enrollment is Up 5.6%, Oct-22 Data
- Oklahoma Medicaid Enrollment is Up 11.8%, Oct-22 Data
- Pennsylvania Medicaid Managed Care Enrollment is Up 5.5%, Oct-22 Data
- Puerto Rico Medicaid Managed Care Enrollment is Up 2.4%, Oct-22 Data
- West Virginia Medicaid Managed Care Enrollment is Up 4.5%, Oct-22 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- California Residency Program for SUD Treatment RFA, Dec-22
- Indiana Medicaid Fee-For-Service Non-Emergency Medical Transportation RFP, Dec-22
- Iowa Medicaid Enterprise Modernization Effort Integration Services RFI, Dec-22
- New York Care Coordination Organization/Health Home Program Evaluation RFP
- Oklahoma SoonerSelect Children’s Specialty Plan RFP, Dec-22
- Texas STAR Health Foster Care RFP and Scoring, Oct-22
Medicaid Program Reports, Data, and Updates:
- Arizona AHCCCS Annual Audited Financial Reports, FY 2008-21
- California Medi-Cal Health Plan Financial Reports, 2021
- Georgia Medicaid Managed Care Rate Certifications, FY 2019-22
- Idaho Medicaid Facts, Figures, and Trends Reports, 2013-23
- Louisiana Medicaid Financial Forecast Reports, SFY 2018-22
- Ohio OBM Monthly Financial Reports, 2022
- Pennsylvania MLTSS Subcommittee Meeting Materials, 2021-22
- Texas Financial Statistical Reports by Health Plan and Program, 2020-22
- Texas OIG UnitedHealthcare Administrative and Medical Expenses Audit, Aug-22
- Virginia Medallion 4.0 and CCC Plus Medicaid Operations Analysis, 2017-22
- Washington Apple Health Plan Report Cards, 2020-22
- Washington Medicaid Managed Care Capitation Rate Development, CY 2015-22
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.