This week's roundup:
- In Focus: CMS Invites States to Apply for Transforming Maternal Health Model
- California SBHIP Participants See Positive Outcomes
- Florida Final Actions Against Medicaid Managed Care Plans Total $33.2 Million
- Kansas Denies Aetna, CareSource Protests Over KanCare Awards
- North Dakota Awards Medicaid Enterprise Systems Integrator Contract to Leidos
- Oregon Releases State-Based Insurance Marketplace Solution RFP
- South Carolina Governor Vetoes Study Committee to Examine Medicaid Expansion
- Utah Submits Section 1115 Medicaid Demonstration Amendment Request
- CMS Proposes CY 2025 Medicare Hospital OPPS/ASC Rule Addressing Health Disparities, Maternal Health
- CMS Launches Making Care Primary Model Across Eight States
- CMS Launches Medicare Dementia Care Model
- U.S. Paid $50 Billion for Medicare Advantage Upcoding
- FTC to Sue PBMs after Report Finds Affiliate Pharmacies Received 200 Times More for Common Cancer Drugs
- More News Here
In Focus
CMS Invites States to Apply for Transforming Maternal Health Model
This week, our In Focus section reviews the notice of funding opportunity (NOFO) for the Transforming Maternal Health (TMaH) Model, which the Centers for Medicare & Medicaid Services (CMS) Center for Medicaid and Medicare Innovation (the Innovation Center) announced on December 15, 2023. States interested in participating in this model must submit an application to CMS during the competitive application process.
As described in a December 2023 In Focus, pregnancy-related deaths have more than doubled since 1987 to 17.6 deaths per 100,000 live births, with health disparities only worsening outcomes for different racial and ethnic groups. For example, the pregnancy-related mortality rates for Black and Native American and Alaska Native people are approximately two to three times higher than the rate for White people. In recent years, 38 states have extended postpartum coverage, and 11 states now offer doula coverage for Medicaid enrollees. This initiative accelerates the focus on maternal outcomes and, with Medicaid paying for nearly 43 percent of births, has the potential to affect health across generations.
This model is designed exclusively to improve maternal healthcare for people enrolled in Medicaid and the Children’s Health Insurance Program (CHIP). The TMaH model takes a whole-person approach to pregnancy, childbirth, and postpartum care, addressing the physical, mental health, and social needs people experience during pregnancy.
Model Overview
Up to 15 participating state Medicaid agencies (SMAs) will receive as much as $17 million over the 10-year period to develop a value-based alternative payment model for maternity care services, with the intention of improving quality and health outcomes and promoting the long-term sustainability of services. TMaH will focus on three pillars:
- Access to care, infrastructure, and workforce capacity
- Quality improvement and safety
- Whole-person care delivery
The TMaH model is designed to support birthing persons along their care journey, expanding continuity, and improving outcomes.
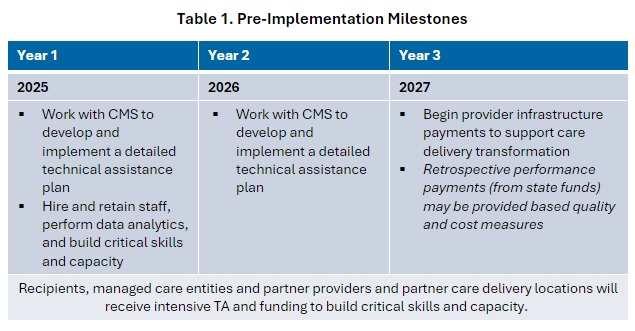
During the model’s first three years, states will receive targeted technical assistance to achieve pre-implementation milestones. The table below highlights the key activities in the pre-implementation phase.
Following pre-implementation, participants will enter a seven-year implementation period during which the SMAs will implement the program with partners, such as managed care organizations (MCOs), perinatal quality collaboratives, hospitals, birth centers, health centers and rural health clinics, maternity care providers, and community-based organizations.
In year four, states will offer partnering providers and care delivery sites upside-only performance payments from state funds (no cooperative funds may be used). In year five, states will transition partner provider and partner care delivery locations to a new value-based payment model. CMS will lead the development of the value-based model, and it will be finalized during the pre-implementation period.
The model also requires a health equity plan, which has been a consistent requirement across models from the Innovation Center. Awardees must develop a plan that addresses disparities among underserved populations, such as racial and ethnic groups and people living in rural areas, who are at higher risk for poor maternal outcomes.
State Medicaid Agency Requirements
For states considering TMaH, the NOFO outlines the requirements for participating SMAs, which include:
- States must include CHIP if pregnant people receive services through CHIP
- States that have managed care plans must contract with at least MCO for implementation
- Collaborate with partner providers (e.g., OBs, midwives, doulas), care delivery location (e.g., hospitals, birth centers, federally qualified health centers), and partner organizations
- Collaborate in the process to create cost and quality benchmarks with CMS
- Be actively involved in technical assistance activities, including attending regularly scheduled calls, providing input and working on portions of documents as appropriate
- Execute the data-sharing agreements necessary to support the exchange of data and information related to the TA activities and completion of milestones
- Provide CMS and contractors the necessary information and data to support the development of documents to help reach milestones
- States must demonstrate their ability to meet these requirements as part of the NOFO process, and CMS will evaluate their responses as part of the selection process
TMaH Opportunities and Considerations
The model offers states resources and technical assistance to develop value-based alternative payment models to support whole-person pregnancy, birth, and postpartum care and improved outcomes. Many SMAs already are working on programs to innovate care and payment, and the TMaH is an opportunity to expand and accelerate those programs.
The model offers an opportunity for states that have yet to expand postpartum coverage or added doula benefits to adopt these policies with the funding and technical assistance they may need to support their efforts.
SMAs interested in this opportunity should evaluate their application readiness and pre-plan for the application.
What’s Next?
States interested in TMaH should submit a letter of intent by August 8, 2024. Applications are due by September 20, 2024, and the model is expected to start January 2025.
The Health Management Associates team will continue to evaluate the TMaH model as more information becomes available. For more information, contact Amy Bassano ([email protected]), Melissa Mannon ([email protected]), and Andrea Maresca ([email protected]).
HMA Roundup
California
California SBHIP Participants See Positive Outcomes. Fierce Healthcare reported on July 3, 2024, that the California Student Behavioral Health Incentive Program (SBHIP), which offers incentive payments for Medicaid plans to build capacity for behavioral health services in K-12 schools, has shown decreased student absences, improved student grades, and increased teacher’s accommodation for behavioral health needs, since it began in 2022. SBHIP currently has 22 Medi-Cal managed care plans and approximately 300 local educational agencies participating. SBHIP is expected to impact 1.4 million school-aged children. Read More
Florida
Florida to Appeal Judge’s Decision to Dismiss CHIP Premiums Lawsuit. Florida Health News reported on July 9, 2024, that Florida will appeal a recent U.S. District Court Judge ruling, which dismissed Florida’s lawsuit over federal rules prohibiting states from dropping beneficiaries from the Children’s Health Insurance Plan (CHIP) if their parents did not pay premiums on time. The state will appeal the court decision in the 11th U.S. Circuit Court of Appeals in Atlanta. Read More
Florida Final Actions Against Medicaid Managed Care Plans Total $33.2 Million. Florida Politics reported on July 4, 2024, that Florida took 288 final actions totaling $33.2 million against Medicaid managed care plans, with all but one that resulted in liquidated damages during the fiscal year beginning July 1, 2023. Every contracted health plan had liquidated damages levied against them as a result of desk reviews. Read More
Kansas
Kansas Denies Aetna, CareSource Protests Over KanCare Awards. The Kansas Reflector reported on July 8, 2024, that Kansas has denied separate protests filed by CVS/Aetna and CareSource over the KanCare Medicaid capitated managed care procurement. The state provided a written response to Aetna and CareSource listing shortcomings of their proposals, including issues with the descriptions to improve services for Kansas Medicaid enrollees. Contracts with incumbents Centene/Sunflower Health Plan and UnitedHealthcare, and non-incumbent Elevance/Healthy Blue are slated to begin January 1, 2025. Read More
Maine
Maine Medicaid Expansion Reduced Uncompensated Care Costs. The Bangor Daily News reported on July 9, 2024, that Maine’s Medicaid expansion reduced uncompensated care costs by 26 percent per year, totaling a $126 million reduction, during the first two years of the COVID-19 pandemic from 2019 to 2021. Significant cost reductions occurred across larger, general acute care hospitals and was driven by a large decline in charity care costs. Read More
Minnesota
Minnesota Issues Corrective Action Plan to Blue Plus Over Alleged Medicaid Contract Breach. The Star Tribune reported on July 9, 2024, that Minnesota has sent a corrective action plan to Blue Cross and Blue Shield of Minnesota subsidiary, Blue Plus, over failure to suspend payments to certain health care providers as requested by the state. The state alleges that the health maintenance organization breached the Prepaid Medical Assistance and MinnesotaCare contract provisions relating to financial recovery for fraud and abuse between 2019 to 2022. Read More
North Carolina
CareSource Names David Herndon North Carolina Market President. CareSource announced on July 9, 2024, that David Herndon has been named North Carolina market president. Herndon previously served as the executive vice president and chief business operations officer for the Hawaii Medical Service Association and was also the former president of Hawaii operations for UnitedHealthcare. Read More
North Carolina Audit Finds LME-MCO Made Improper Payments to Executives Prior to Consolidation. North Carolina Health News reported on July 8, 2024, that Eastpointe Health Services, a North Carolina local management entity-managed care organization (LME-MCO), made improper payments totaling $1.1 million to two executives after Eastpointe was ordered to merge with Trillium, according to an internal audit conducted by the state Department of Health and Human Services. The audit recommends that Trillium seek to recoup the $1.1 million paid out before the consolidation date. LME-MCOs provide specialized behavioral services for individuals with severe mental health conditions or intellectual and developmental disabilities. Read More
North Dakota
North Dakota Awards Medicaid Enterprise Systems Integrator Contract to Leidos. Leidos Holdings, Inc. announced on July 9, 2024, that it has been awarded a contract to provide Medicaid Enterprise Systems Integrator services in North Dakota. Leidos will assist the state in modernizing existing integration platforms, implementing modern integration, and identifying management capabilities. The contract was implemented in April 2024. Read More
Oregon
Oregon Releases State-Based Insurance Marketplace Solution RFP. The Oregon Department of Human Services (ODHS) released on July 3, 2024, a request for proposals (RFP) seeking a State-Based Insurance Marketplace Solution vendor to transition the state health insurance exchange from the federal marketplace to a state-based marketplace. The state plans to contract with one or more vendors to provide an information technology platform and a consumer assistance center. The platforms must be ready in time for November 1, 2026 open enrollment. The initial term of the contract is negotiable, although it is anticipated to be seven years with options to renew. Proposals are due August 12. Read More
Pennsylvania
Pennsylvania Governor Passes Telehealth Parity Bill, Sets Medicaid Accessibility Standards. HealthLeaders reported on July 10, 2024, that Pennsylvania Governor Josh Shapiro signed legislation mandating telehealth payment parity, which requires payers to reimburse telehealth services at the same rate as in-person services. The legislation, which aims to reduce barriers to health care access in rural regions, also includes setting accessibility standards for state Medicaid and Children’s Health Insurance Program coverage. Read More
South Carolina
South Carolina Governor Vetoes Study Committee to Examine Medicaid Expansion. South Carolina Public Radio reported on July 3, 2024, that South Carolina Governor Henry McMaster vetoed a bill which would have created a legislative committee to examine options for improving healthcare access, specifically through Medicaid expansion. Governor McMaster is opposed to spending state funds to study Medicaid expansion. Read More
Utah
Utah Submits Section 1115 Medicaid Demonstration Amendment Request. The Centers for Medicare & Medicaid Services announced on July 8, 2024, that Utah submitted a request to amend its section 1115 Medicaid Reform Demonstration to expand health related social services (HRSS) to individuals who were inmates of a correctional facility and received justice-involved reentry services through Utah’s demonstration program. The amendment would also increase the eligibility age limit for fertility preservation treatment for individuals diagnosed with cancer to 50 years of age or younger. The federal comment period will be open through August 7. Read More
Virginia
Virginia Medicaid Enrollees Struggle to Receive Prenatal Care, Secret Shopper Survey Finds. VPM reported on July 9, 2024, that more than 95 percent of calls from individuals posing as new Virginia Medicaid enrollees seeking prenatal care did not result in an available appointment, according to a secret shopper survey commissioned by the Virginia Department of Medical Assistance Services and conducted by Health Services Advisory Group in 2023. Out of 1,844 calls seeking prenatal care, 13 resulted in an appointment being scheduled within state standards for acceptable wait times. Stakeholders and providers cited inaccurate and out-of-date health care provider directories as a significant driver of the problem. Read More
National
CMS Proposes CY 2025 Medicare Hospital OPPS/ASC Rule Addressing Health Disparities, Maternal Health. The Centers for Medicare & Medicaid Services (CMS) announced on July 10, 2024, the Calendar Year (CY) 2025 Hospital Outpatient Prospective Payment System (OPPS) and Ambulatory Surgical Center (ASC) Payment System proposed rule. This year’s rule includes proposed policies to address health disparities, reduce maternal mortality and morbidity, expand access to behavioral health, and improve transparency. Specifically, the proposed rule seeks to make exceptions to the Medicaid clinic services “four walls” requirement; codify the requirement of 12 months of continuous eligibility for children enrolled in Medicaid and CHIP; propose an add-on payment to the All-Inclusive Rate for certain Indian Health Services and tribal facilities to increase access to certain high-cost drugs; expand the hospital outpatient, ASC, and rural emergency hospital quality program measure sets to include equity measures; and eliminate barriers for incarcerated individuals to enroll in and maintain their Medicare coverage. Read More
CMS Launches Making Care Primary Model Across Eight States. The Centers for Medicare & Medicaid Services (CMS) announced on July 10, 2024, that it has launched the Making Care Primary (MCP) Model with 133 participants across Colorado, Massachusetts, Minnesota, New Jersey, New Mexico, New York, North Carolina, and Washington. The ten-year model aims to improve the delivery of advanced primary care services for Medicare enrollees. Participants are comprised of both federally qualified health centers and small primary care organizations. MCP’s three progressive tracks include building infrastructure, implementing advanced primary care, and optimizing care and partnerships. Read More
CMS Launches Medicare Dementia Care Model. The Centers for Medicare & Medicaid Services (CMS) announced on July 8, 2024, that it has launched the Guiding an Improved Dementia Experience (GUIDE) Model for 96 participating organizations that have been providing GUIDE care delivery services for over a year to Medicare part B beneficiaries with dementia. Another 294 participants who have not yet established Dementia Care Programs will begin offering GUIDE services on July 1, 2025. The model, which tests a comprehensive package of care coordination and management, caregiver education, and certain respite services, will run for eight years. Read More
U.S. District Court Judge Blocks Medicare Advantage Broker Compensation Limits. Modern Healthcare reported on July 10, 2024, that a U.S. District Court judge granted a stay on a Centers for Medicare & Medicaid Services final rule capping the total compensation Medicare Advantage plans can pay brokers, which includes administrative expenses that were previously excluded from limits. The U.S. District Judge Reed O’Connor has not issued a final decision in the case. Read More
U.S. Paid $50 Billion for Medicare Advantage Upcoding. The Wall Street Journal reported on July 8, 2024, that the U.S. paid out approximately $50 billion to Medicare Advantage (MA) insurers for additional diagnoses not treated by doctors that were added by MA insurers from 2018 through 2021, according to a WSJ analysis. The analysis found many diagnoses made by insurers for which patients received no treatment or that contradicted their doctors’ views. For example, MA insurers were paid $700 million for more than 66,000 diagnoses of diabetic cataracts for MA beneficiaries who had already received cataract surgery. Additionally, around 18,000 MA recipients had insurer-driven diagnoses of HIV but were not receiving treatment from doctors. Read More
Public Health Emergency Policies Significantly Improved Health Coverage, Cost Barriers. Fierce Healthcare reported on July 8, 2024, that the number of non-elderly Americans who delayed or went without necessary medical care due to costs dropped by 4.75 million from 2019 to 2022, according to a study from the Urban Institute. The share of uninsured adults fell from 14.5 to 12.4 percent over the same time period, with the largest decline in states that expanded Medicaid. Researchers anticipate that the end of Medicaid continuous coverage requirement and the potential expiration of enhanced Marketplace tax subsidies could make health coverage improvements difficult to sustain. Read More
Medicare Advantage Has Highest Gross Margins Per Enrollee in 2023, Medicaid Lowest, KFF Study Finds. KFF reported on July 2, 2024, that health payer profits per member are highest in Medicare Advantage plans with gross margins at $1,982 per enrollee, and lowest in Medicaid plans, according to an analysis of financial performance in 2023. Gross margins in Medicaid managed care plans decreased to $753 per member in 2023, compared to $804 in 2022. The report also found that simple medical loss ratios have remained relatively stable across Medicaid managed care and Medicare Advantage plans, ranging from 83 to 89 percent from 2018 to 2023. Read More
Industry News
FTC to Sue PBMs after Report Finds Affiliate Pharmacies Received 200 Times More for Common Cancer Drugs. Health Payer Specialist reported on July 10, 2024, that the Federal Trade Commission (FTC) plans to sue the three largest pharmacy benefit managers (PBMs) following a study which found they paid their own mail-order pharmacies as much as 200 times more than the price at independent pharmacies for common cancer drugs, generating at least $1 billion in excess revenue. The FTC estimated that increased reimbursement rates for two specialty generic drugs (Zytiga and Gleevec) led to $1.6 billion in excess revenue for pharmacies affiliated with the three largest PBMs between 2020 and 2022. Read More
RFP Calendar
HMA News & Events
NEW THIS WEEK ON HMA INFORMATION SERVICES
(Exclusive Access for HMAIS Subscribers):
HMAIS Reports
- Updated Florida State Overview
- Updated Indiana State Overview
Medicaid Data
Medicaid Enrollment:
- Florida SNP Membership at 809,315, Mar-24 Data
- Florida Medicaid Fee for Service vs. Managed Care Penetration, 2014-23
- Kentucky Medicaid Managed Care Enrollment is Down 8%, Jul-24 Data
- Michigan Medicaid Managed Care Enrollment is Down 6.1%, Mar-24 Data
- Nevada Medicaid Fee for Service vs. Managed Care Penetration, 2014-23
- New Hampshire Medicaid Fee for Service vs. Managed Care Penetration, 2014-23
- New Mexico Medicaid Fee for Service vs. Managed Care Penetration, 2014-23
- Pennsylvania Medicaid Managed Care Enrollment is Down 6.7%, Apr-24 Data
- Pennsylvania Medicaid LTSS Enrollment is Down 3.7%, Apr-24 Data
- Wisconsin SNP Membership at 100,103, Mar-24 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Alabama Medicaid Agency Accounting, Auditing, and Consulting Services RFP, Jul-24
- Mississippi D-SNP Model Contract, 2021-25
- North Dakota Medicaid Enterprise Systems Integrator RFP Documents, 2023-24
- Oregon State Based Insurance Marketplace Solution RFP, Jul-24
Medicaid Program Reports, Data, and Updates:
- Arizona Quarterly Progress Reports for CMS, 2019-24
- Pennsylvania Physical HealthChoices Databooks, CY 2018-25
- Pennsylvania Medical Assistance Advisory Committee (MAAC) Meeting Materials, Jun-24
- Pennsylvania MLTSS Subcommittee Meeting Materials, 2021-24
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Andrea Maresca at [email protected].