Alabama
Alabama Organizations Urge Governor to Adopt Medicaid Expansion. The Alabama Daily News reported on May 19, 2024, that advocacy group Cover Alabama, along with more than 80 businesses and organizations, signed a letter requesting that Governor Kay Ivey expand the state’s Medicaid program to cover nearly 300,000 uninsured individuals in the state. The letter addresses the potential financial gains associated with Medicaid expansion, including access to $619.4 million in federal funds and the federal government paying $397 million in annual expenses currently covered by the state. Ivey’s office has indicated that she remains opposed to expansion, although some Republican lawmakers have engaged in expansion-related discussions in the past year. Read More
Arizona
Arizona Awards FFS PBM Contract to OptumRX. The Arizona Health Care Cost Containment System announced on May 20, 2024, that it has awarded a pharmacy benefit manager (PBM) contract to incumbent United/OptumRX to provide services for the state’s fee-for-service Medicaid populations. The contract is anticipated to start on October 1, 2024, and will run for three years with two one-year renewal options. Read More
California
California Bill to Create Universal Healthcare System Dies in Assembly Appropriations Committee. The San Joaquin Valley Sun reported on May 16, 2024, that a California bill to create CalCare, a state-run, single-payer, universal healthcare plan, has died in the Assembly Appropriations Committee. Since 2007, the state has unsuccessfully tried to enact a single-payer healthcare bill. Read More
Delaware
Delaware Receives Federal Approval for Medicaid 1115 Waiver Extension. The Centers for Medicare & Medicaid Services approved on May 17, 2024, Delaware’s five-year extension of its Section 1115 Diamond State Health Plan demonstration, effective through December 31, 2028. The extension will include clinically appropriate substance use disorder treatment services for short-term residents in residential and inpatient treatment settings that qualify as an institution for mental diseases; adult dental services; coverage for former foster care youth under age 26 who currently reside in Delaware; and contingency management services for certain adults with stimulant use disorder or opioid use disorder. Read More
Florida
Florida Centene Subsidiary, CityBlock Partner to Provide Primary Care, Care Coordination Services. Fierce Healthcare reported on May 21, 2024, that Medicaid value-based care provider Cityblock has entered a partnership with Centene subsidiary Sunshine Health to provide primary care and care coordination services to Medicaid beneficiaries in 11 counties in central Florida. The partnership, which began May 1, will provide services at home or in local clinics. Cityblock has previously partnered with Centene subsidiaries in New York and Ohio. Read More
Florida Lawsuit Over CHIP Guidelines Challenged by Biden Administration. Health News Florida reported on May 16, 2024, that the Biden administration filed a motion to dismiss Florida’s lawsuit challenging guidelines from the Centers for Medicare & Medicaid Services prohibiting the state from removing children from the Children’s Health Insurance Program (CHIP), KidCare, if parents stopped paying required premiums. The Biden administration contends that the guidelines adhere to the Consolidated Appropriations Act of 2023 while Florida has argued that the guidelines violate the Administrative Procedure Act. Florida initially filed the lawsuit in February and additionally requested a preliminary injunction, which has not yet been ruled upon. Read More
Illinois
Illinois House Committee Passes Bill to Strengthen Children’s Behavioral Health Transformation Initiative. Health News Illinois reported on May 21, 2024, that the Illinois House Mental Health & Addiction Committee approved a bill, sponsored by Representative Lindsey LaPointe (D-Chicago), that would further strengthen childhood mental health services as a part of the Illinois Children’s Behavioral Health Transformation Initiative. Specifically, the bill would establish a workgroup with the Department of Healthcare and Family Services, Medicaid managed care organizations, and other stakeholders to identify leading indicators for behavioral health crisis risk and make recommendations by September. The bill would also require the State Board of Education to work with agencies and stakeholders to develop a universal mental health screening of students, with a phased in plan slated to begin next April. The bill now heads to the full House for final review. Read More
Illinois Senate Committee Approves Bills Comprising Governor’s Insurance Reform Package. Health News Illinois reported on May 22, 2024, that the Illinois Senate Insurance Committee approved two bills comprising Governor JB Pritzker’s insurance reform package. HB 5395, sponsored by Senator Robert Peters (D-Chicago), would ban insurers from using step therapy, the practice of asking patients to try cheaper treatments prior to authorizing more expensive options; increase transparency standards; and streamline availability of providers’ information. It would also require insurers to cover the first 72 hours of inpatient mental treatment at a hospital if notified of the admission and treatment plan within 48 hours. HB 2499, sponsored by Senator Laura Fine (D-Glenview), would ban short-term, limited-duration plans that do not cover all essential benefits beginning in 2025. Both bills next head to the full Senate for further review. Read More
Illinois to Grant $200 Million in Additional Healthcare Transformation Grants. Health News Illinois reported on May 20, 2024, that Illinois will award $200 million to six to 10 projects in the next round of healthcare transformation grants. Safety-net hospitals will be prioritized. The Department of Healthcare and Family Services and Capital Development Board will accept applications through the end of June, and awards are expected to be announced later this year. Read More
Indiana
Indiana Faces Lawsuit Over Cuts that Remove Compensation for Family Caregivers. ABC News reported on May 17, 2024, that the American Civil Liberties Union of Indiana and Indiana Disability Rights groups, on behalf of parents of two children with disabilities, are suing the Indiana Family and Social Services Administration (FSSA) in response to the state’s decision to stop reimbursing family members and guardians for home care beginning July 1. The lawsuit alleges that the decision is a violation of the Americans with Disabilities Act and federal Medicaid laws and could result in the unnecessary institutionalization of children with complex medical needs. Affected families have spoken out against the decision, which was proposed to save costs in light of a nearly $1 billion Medicaid shortfall. The lawsuit states that the FSSA’s efforts to work with families, including new reimbursement rates, have not been sufficient. Read More
Kansas
Kansas Governor Signs Bill to Invest in Mental Health Pilot Program, New Psychiatric Hospital. KSNT reported on May 16, 2024, that Kansas Governor Laura Kelly signed the omnibus reconciliation spending limit bill, which will provide $4.5 million to the Mental Health Intervention Pilot and invest $26.5 million into building a new psychiatric hospital in Wichita. The pilot program authorizes school districts to enter into agreements with local community mental health centers to support students and families with mental health needs. Read More
Louisiana
Louisiana Senator Proposes Bill for Medicaid Doula Services. 7 KPLC reported on May 21, 2024, that Louisiana Senator Regina Ashford Barrow (D-Baton Rouge) proposed a bill that would require Medicaid to cover doula services before, during, and after childbirth. The bill currently awaits review in the Senate Finance Committee. Read More
Nevada
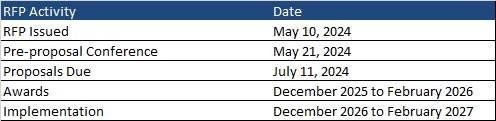
Nevada Solicits Public Input for Upcoming Coordination-only D-SNP RFP. The Nevada Division of Health Care Financing and Policy released on May 17, 2024, a solicitation of public input regarding an upcoming request for proposals (RFP) for the Coordination-Only Dual Special Needs Plan (CO D-SNP) Program. CO D-SNP State Medicaid Agency Contracts will be effective from January 1, 2026, through December 31, 2029, with awards to be announced in early January 2025. The solicitation will accept input from plans and stakeholders on items such as inclusion of health risk assessments, covered populations, expansion of service area, supplemental benefits, and quality measures through June 17. Read More
Nevada Extends Postpartum Medicaid Coverage to 12 Months. The Centers for Medicare & Medicaid Services announced on May 17, 2024, approval for Nevada’s Medicaid state plan amendment to extend Medicaid postpartum coverage to 12 months. Read More
New Mexico
New Mexico Sets Expectations for MCOs to Invest in Behavioral Health Accessibility Under New Contracts. The Santa Fe New Mexican reported on May 20, 2024, that New Mexico expects its four managed care organizations (MCOs) under the revamped Medicaid managed care program, called Turquoise Care, to make financial investments to address gaps in access to care, specifically for behavioral health accessibility. The new contracts include requirements regarding behavioral health appointment wait times and providing mobile crisis services. The state will impose sanctions on MCOs that fail to meet required standards. Read More
New York
New York Appeals Court Blocks State from Transitioning Municipal Retirees to Medicare Advantage Plans. Crain’s New York Business reported on May 22, 2024, that a New York State appeals court upheld a previous ruling barring New York City from transferring 250,000 municipal retirees from traditional Medicare to private Medicare Advantage plans. The state first announced the transition in 2018 in an effort to save money, though the decision was met with opposition from retirees, who noted that the transition may be more expensive and reduce their access to providers. In 2023, a class-action lawsuit was filed against the city to block the transition and a trial court granted the request. Read More
New York Comptroller Raises Concerns Over Managed Care Tax Revenue in Enacted Budget. Crain’s New York reported on May 20, 2024, that New York Comptroller Thomas DiNapoli has criticized the state’s enacted budget and its financial reliance on implementing a Medicaid managed care tax. The managed care tax has not yet received federal approval, although the state still included $350 million in expected revenue from it. The Division of Budget is expected to release an update to the state’s financial plan by the end of this month. Read More
New York Senator Introduces Bill to Increase Transparency in Medicaid Managed Long Term Care Plans. Spectrum Local News reported on May 16, 2024, that New York State Senator Rachel May (D-Syracuse) introduced a bill that would require the state to make Medicaid Managed Long Term Care (MLTC) data public, including the number of enrollees, types of services received, and amount of home care hours provided. The bill is intended to enhance accountability of MLTC plans and ensure allocated funding goes to home care services. The bill is currently being reviewed by the Senate Health Committee. Lawmakers previously proposed legislation to eliminate MLTC plans and revert to a fee-for-service model; however, it is unlikely to pass during the current legislative sessions. Read More
Tennessee
Tennessee Receives Federal Approval for Section 1115 TennCare III Waiver Amendment. The Centers for Medicare & Medicaid Services (CMS) approved on May 17, 2024, Tennessee’s request to amend its Medicaid section 1115 demonstration entitled, “TennCare III,” effective through December 30, 2030. The amendment allows for modifications including the expansion of eligibility for parents and caretaker relatives of dependent children, a new benefit to cover a supply of diapers for infants and young children, and enhanced home and community-based services for beneficiaries with disabilities. Read More
Washington
Washington Reentry Demonstration Initiative to Provide Pre-release Medicaid Services. The Washington State Health Care Authority announced on May 21, 2024, that it has invited the state’s carceral facilities to participate in the Reentry Demonstration Initiative, which provides pre-release Medicaid services for those leaving incarceration. The services include care management, substance use disorder treatment, and targeting of infectious diseases. The voluntary initiative functions under the Medicaid Transformation Project, the state’s Section 1115 demonstration, and the first cohort of participating carceral facilities will launch on July 1, 2025. Read More
Wisconsin
Wisconsin Medicaid LTC Contract Award Slated to Go to Molina. Molina Healthcare announced on May 22, 2024, that the Wisconsin Department of Health Services (DHS) plans to award the company the Medicaid long-term care (LTC) Family Care and Family Care Partnership program contract to provide services in Geographic Service Region 5. The contract is expected to begin on January 1, 2025, and last for two years with the option for three two-year renewals. Molina Healthcare of Wisconsin will offer the program benefits under the brand name, My Choice Wisconsin. Molina currently serves approximately 5,600 members in both the Family Care and Family Care Partnership program. The state has approximately 55,000 total members enrolled in the two programs. Read More
National
Biden Administration Releases National Maternal Mental Health Strategy. RollCall reported on May 15, 2024, that the Biden Administration’s Advisory Committee for Women’s Services’ (ACWS) Task Force on Maternal Mental Health has launched the first national maternal mental health strategy which recommends a whole of government approach to reducing untreated mental health and substance use conditions during and after pregnancy. The strategy includes initiatives and recommendations for states to support data and research; prevention, screening and diagnosis; intervention and treatment; community practices; and community engagement. The Administration also sent The Task Force on Maternal Mental Health’s Report to Congress, which catalogues best practices, existing federal programs and coordination, and feedback from stakeholders. Read More
CMS Launches Websource for EMTALA Complaints. The Centers for Medicare & Medicaid Services (CMS) announced on May 21, 2024, that it has launched a new websource to allow individuals to more easily file an Emergency Medical Treatment and Labor Act (EMTALA) complaint. Medicare-participating hospitals are required under EMTALA to provide medical screening exams for individuals arriving at hospital emergency departments to determine if the person has an emergency medical condition. Read More
Senate Finance Committee Chair Plans to Introduce Legislation Targeting Rogue Exchange Marketers. Modern Healthcare reported on May 21, 2024, that Senate Finance Committee Chair Ron Wyden (D-Oregon) informed the Centers for Medicare & Medicaid Services (CMS) of plans to introduce legislation that would allow federal regulators to fine rogue brokers and agents who sign individuals up for Exchange plans without their consent. CMS indicated this month that it is considering issuing monetary penalties for these faulty agents and brokers. The agency received approximately 40,000 complaints from people who had unknowingly been switched to Exchange plans in the first three months of 2024, and 50,000 complaints of unauthorized enrollments during the annual sign-up period for 2024. Read More
Senate Finance Committee Releases White Paper on Increasing Medicare Physician Reimbursement. Modern Healthcare reported on May 20, 2024, that the Senate Finance Committee released a white paper proposing adjusting Medicare doctor reimbursement to account for inflation. The white paper considers payment reform policies including incentives to increase provider participation in alternative payment models, potential changes to Medicare’s budget neutrality requirements, and ensuring clinicians can own and operate their practices. The paper also aims to identify solutions for better treatment and management of chronic conditions. Read More
U.S. House Energy, Commerce Health Subcommittee Passes Legislation to Extend Telehealth Flexibilities by Two Years. Stat News reported on May 16, 2024, that the U.S. House Energy and Commerce health subcommittee passed legislation to extend Medicare telehealth flexibilities by two years. Flexibilities include allowing visits to be conducted from any location and permitting additional providers to bill for telehealth. The legislation also would address payment disparities for rural providers and reimburse Rural Health Clinic and Federally Qualified Health Centers at parity with in-person visits. The bill will next be reviewed by the full committee. Read More
Senators Introduce Bill to Improve Pay for PCPs, Reduce Cost-Sharing For Medicare Beneficiaries. Fierce Healthcare reported on May 15, 2024, that United States Senators Sheldon Whitehouse (D-Rhode Island) and Bill Cassidy (R-Louisiana) introduced a bill, titled the Pay Primary Care Providers (PCPs) Act aimed at supporting and improving pay for PCPs. The bill would reward PCPs providing high-quality care and provide Medicare beneficiaries with reduced cost-sharing for some primary care services. The senators released a request for information for feedback on policy questions. The deadline to respond is July 15. Read More
Senators to Introduce Bill that Would Extend Acute Hospital Care at Home Bill for Five Years. The Hill reported on May 15, 2024, that U.S. Senators Tom Carper (D-Delaware) and Tim Scott (R-South Carolina) plan to introduce a bill that would extend the expiration date of the Acute Hospital Care at Home (AHCAH) waiver program for another five years. The program, currently set to expire December 31, 2024, permits inpatient-level hospital services to be conducted in patients’ homes. Read More
CMS Discards Stacking Provision Under Medicaid Drug Rebate Proposed Rule. The Centers for Medicare & Medicaid Services (CMS) announced on May 15, 2024, that it will not be finalizing the “stacking” provision under the proposed Medicaid Drug Rebate Program rule, which would have required companies to stack discounts and rebates throughout a transaction when reporting best prices. CMS will continue to gather information from manufacturers on best price stacking methodologies to better inform new rules. Read More