This week, our In Focus section reviews the Texas STAR+PLUS managed care services request for proposals (RFP) released on March 31, 2022, by the Texas Health and Human Services Commission (HHSC). The STAR+PLUS program, including the STAR+PLUS Home and Community-based Services (HCBS) program, provides acute care services and Long-Term Services and Supports (LTSS) to the aged and disabled.
Background
The STAR+PLUS program’s 540,000 beneficiaries are served by Anthem, Centene, Molina, and UnitedHealthcare. Cigna’s Texas STAR+PLUS Medicaid members (as well as the Medicare-Medicaid plan (MMP) members) were reassigned to Molina, effective January 1, 2022.
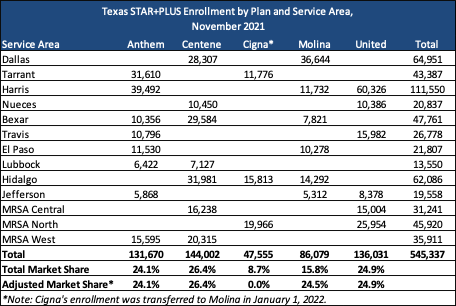
The STAR+PLUS program operates under a Section 1115 waiver and a Section 1915 waiver to expand the Medicaid managed care delivery system statewide and provide HCBS under a Medicaid managed care model.
The state threw out the previous awards for STAR+PLUS contracts in 2020 because of discrepancies in the evaluation and scoring of the bids. The STAR+PLUS contracts had been awarded to Aetna, Anthem/Amerigroup, Centene/Superior, El Paso Health, Molina, and UnitedHealthcare. Implementation was set to begin September 1, 2020. This marked the second time that year in which the procurement faced major setbacks because of problems with the procurement process.
Integration of acute care services and LTSS is an essential feature of STAR+PLUS. MCOs will also provide access to behavioral health services, such as mental health and substance use disorder counseling and treatment.
RFP
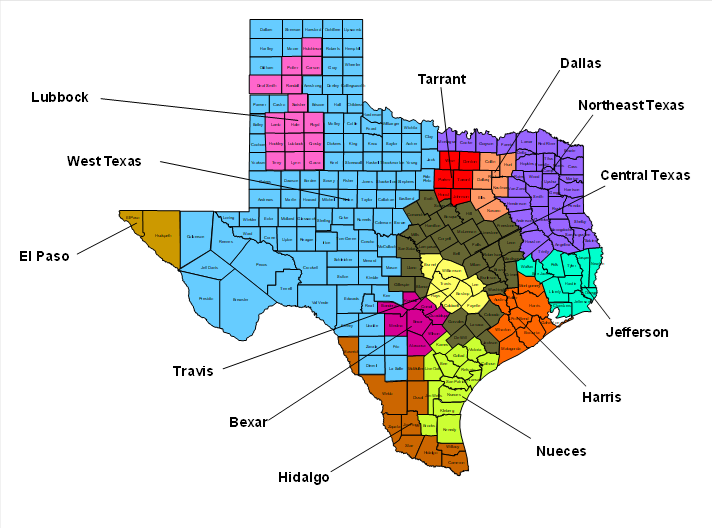
HHSC plans to award contracts to at least two managed care organizations (MCOs) in each of the state’s Service Areas (SAs). MCOs may bid on multiple SAs, and if chosen for an SA, must serve all counties within the SA. Contracts, worth a total of $10.3 billion per year, will run for six-years with three possible two-year renewal options.
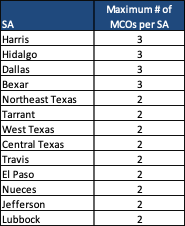
There will be a maximum number of MCOs selected per SA as follows:
MCOs must also submit a notice of intent to apply for a Dual-Eligible Special Needs Plan contract to the Centers for Medicare & Medicaid Services by November 2022 or, if the Texas Medicare-Medicaid Dual Demonstration is continued beyond 2023, a notice of intent to apply for a Dual Eligibles Medicare-Medicaid Plan (MMP) contract.
HHSC will implement a voluntary pilot program in STAR+PLUS to test person-centered strategies and improvements for covering intellectual and developmental disabilities (IDD) waiver services under a capitated model. The new pilot program, STAR+PLUS Pilot Program (SP3) will carve LTSS into the STAR+PLUS program for people with IDD, traumatic brain injuries (TBI), acquired brain injuries (ABI) and similar functional needs in one of the service areas (either Bexar, Medicaid Rural Service Area Northeast or Tarrant). It will operate for two years beginning September 1, 2023, and will then be evaluated. Pilot Program participation will be limited to one or two STAR+PLUS MCOs.
Timeline
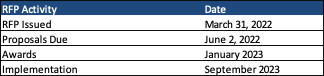
Proposals are due by June 2, 2022, and awards are expected in January 2023. Contract start date is September 2023.
Evaluation
Technical proposals will be scored based on the following criteria:
- Delivers person-centered service coordination that connects member needs to effective care.
- Demonstrates an understanding of the unique elements of service coordination and the needs of the STAR+PLUS population, inclusive of individuals with physical, behavioral health, and intellectual or developmental needs.
- Demonstrates an effective, person-centered process and infrastructure to identify, assess, and respond to individual member’s needs and strengths.
- Demonstrates engagement of providers, member’s family, and community supports serving the member in the service coordination process.
- Supports successful transitions of care for members between programs, services, and settings.
- Demonstrates how data will be used to inform service coordination approaches and to measure success.
- Ensure members have timely access to the services they need.
- Demonstrates the ability to deliver person-centered services timely in the least restrictive and most appropriate integrated setting for individuals covered in the STAR+PLUS Program.
- Demonstrates use of innovative and proven strategies to promote access to providers and services, including addressing provider shortages and barriers to care in specific areas of the state.
- Demonstrates the ability to coordinate and ensure the delivery of the full array of services across programs and payers to support members’ needs and preferences in a holistic way.
- Demonstrates provision of member services and supports that are culturally and linguistically appropriate, accessible, and responsive to the needs of members in the STAR+PLUS Program.
- Demonstrates a proactive approach to outreach and education to support members in successfully managing their health and directing their Services.
- Encourage providers to participate in the Medicaid program.
- Demonstrates effective collaboration and communication with the provider community as evidenced by network participation and provider satisfaction.
- Demonstrates proactive strategies to streamline processes and reduce administrative burden for providers.
- Demonstrates transparent, efficient policies and processes for key business operations, such as credentialing, contracting, claims payment, and utilization management (UM).
- Demonstrates support to providers in complex clinical decision-making through decision-support tools, best practice guidelines, and UM approaches.
- Utilizes network development strategies and incentives that ensure appropriate access for members.
- Demonstrates supports to providers serving the member using technology, data, and processes and tools to better inform and improve care across programs.
- Ensure a sustainable Medicaid program by incentivizing value in the service delivery model and optimizing resources.
- Demonstrates proven strategies to monitor and manage healthcare quality and improve key quality metrics that align with the goals of the state.
- Demonstrates a system of care that identifies, invests in, and rewards desired outcomes with regards to access, high-value care, and community integration.
- Demonstrates advances in value-based care and delivery system reform and supports Providers through these transitions with necessary data and information.
- Demonstrates achievable cost efficiencies and program integrity through effective monitoring and control of spending and UM trends.
- Use data, technology, and reporting to facilitate and demonstrate strong performance and oversight.
- Demonstrates capability to meet all requirements related to access to services, service delivery, quality of care, operations, and financial performance.
- Demonstrates consistent, timely, and accurate delivery of data, analysis, and reporting.
- Demonstrates process improvements and cost efficiencies using automation and data solutions.
- Utilizes integrated systems and processes with the state and other vendors to facilitate appropriate member transitions.