This week's roundup:
- In Focus: How Can Medicare and Medicaid Providers Utilize CMS’ COVID-19 Roadmap?
- Arkansas Seeks Federal Approval to Offer Full Medicaid Coverage to Pregnant Women
- California Awards $340 Million Population Health Management Contract to Gainwell Technologies
- California Medi-Cal Contract Awards Face Appeals
- Iowa Awards NEMT Contract to MTM
- Maryland Releases Dental Benefits Administrator RFP
- Maryland Releases Medicaid NEMT Broker RFP
- New Mexico Delays Medicaid Managed Care RFP Release to Third Quarter of 2022
- Oklahoma Releases Medicaid Dental Managed Care RFP
- Tennessee Proposes PMPM Medicaid Spending Cap to Replace Proposed Aggregate Cap
- Texas Delays Releases of STAR/CHIP, STAR Kids RFPs
- MedPAC Eyes Potential Standardized Benefit Options for Medicare Advantage
- CMS Proposes Rule to Standardize Medicaid, CHIP Eligibility and Enrollment
- CVS to Acquire Signify Health
- Maximus Retains Contract to Support CMS Contact Center Operations
In Focus
How Can Medicare and Medicaid Providers Utilize CMS’ COVID-19 Roadmap?
This week, our In Focus section identifies steps that Medicare and Medicaid plans and providers can undertake to effectively return to normal operations after the end of the COVID-19 public health emergency (PHE) declaration. On August 18, 2022, the Centers for Medicare & Medicaid Services (CMS) released a roadmap to support healthcare providers with preparing for the eventual end of the PHE. CMS also published a series of fact sheets summarizing the status of Medicare Blanket waivers and flexibilities by provider type as well as flexibilities applicable to the Medicaid providers and stakeholders.
In its announcement, CMS expressed concern that the continued PHE flexibilities could contribute to further decline in patient, resident, and client safety beyond what has already been observed. As a result, the agency is cautiously working to balance ongoing PHE needs while conveying more urgency for providers to prepare for the eventual end of the PHE flexibilities and waivers.
CMS has already ended certain flexibilities and waivers. The agency could phase out other flexibilities as it prepares to let the PHE declaration lapse. This means that providers and health plans should act now to assess flexibilities and waivers in use and develop a plan to transition to post-PHE environment.
Phase-out of COVID-19 Flexibilities
During the COVID-19 PHE, CMS has utilized Medicare and Medicaid waivers and flexibilities extensively. For example, Medicare has not enforced certain federal requirements during this time to allow hospitals to utilize off-site locations to screen and treat patients when needed as well as to minimize certain reporting requirements. The agency’s flexibilities also have accelerated adoption of telehealth and audio only services, particularly for behavioral health services.
Medicare and Medicaid providers across the states utilized PHE flexibilities to varying degrees, in part depending on experiences in individual communities, capacity, and other provider specific factors. Additionally, over the course of the PHE health plan and provider staffing and workflows have changed dramatically. This means health plans and providers will need a tailored plan to support the transition to the post PHE environment.
HMA’s experts are working with hospitals, health systems, clinics, and other providers as well as health plans on the steps they need to take now to prepare for multiple transitions. Our experts identified six immediate steps that Medicare and Medicaid plans and providers can be undertaking now to ensure they can effectively return to normal operations, including:
- Review performance on the patient and clinician safety metrics cited in the new CMS resources. In instances where providers have gaps and suboptimal safety and quality outcomes, they will need assistance developing and implementing mitigation and quality improvement plans.
- Utilize CMS’ tailored fact sheets to identify specific flexibilities and waivers in use now and the “normal” federal regulations that will be in effect once the PHE lapses. This assessment should include the blanket waivers and provider specific flexibilities, including:
- Flexibilities around the requirements and timing for practitioner training
- Expansion of allowable sites of service that permitted more expansive use of telehealth and virtual services as well as screening and treatment provided at alternative sites
- Relaxation of federal requirements pertaining to surge capacity protocols
- Flexibilities for staffing requirements, including medical records departments, nursing facilities, among others
- Waiver of requirement for hospitals to submit occupational mix surveys and to have a utilization review plan with a UR committee focused on services furnished to Medicare and Medicaid enrollees
- Applicable of the Extreme and Uncontrollable Circumstances Policy in Medicare’s Shared Savings Program and use of other flexibilities for MSSP Accountable Care Organizations (ACOs)
- Non enforcement of certain physician self-referral laws
- Waiver of numerous reporting requirements including those pertaining to verbal orders, discharge planning, HEDIS and STARs measure reporting, among others
- Project impact of ending Medicaid’s continuous coverage policy and support individuals with actions they may need to take at the end of the PHE. Once the PHE ends, Medicaid’s enhanced federal funding for states and continuous coverage policy will end. HMA is working with health plans, providers and other stakeholders to project how this change will impact the enrollment and payer mix on state and local levels. Additionally, patients and their caregivers will need support from plans, providers, and consumer groups to ensure they renew their coverage or transition to other coverage programs when needed. HMA’s experts have written extensively about our work to support the Medicaid unwinding activities here and here.
- Develop a plan to transition from “PHE” to “post-PHE” expectations that is informed by the assessment of flexibilities in use. Key components of the plan include:
- Anticipated resource needs to reflect changes in staffing and workflows during the PHE
- Articulation of specific compliance procedures and regular reporting requirements that will resume and the process for this transition
- Develop training and education opportunities for staff that may be new or need refresher on normal policies and procedures as well as timeframes for making these changes
- Update budgets projections to account for changes in reimbursement rates for certain services post-PHE. Certain reimbursement amounts and payment methodologies will change post-PHE, such as payment for administering the COVID-19 vaccine in a Medicare patient’s home among other changes. Providers will need to project the financial impact of these payment changes and update coding and billing manuals and procedures where applicable.
- Build strategies to sustain changes to care models implemented during the COVID-19 PHE while also addressing health disparities. Some providers and facilities adopted care models and modified existing ones during the PHE that may have improved patient outcomes and experiences, maximized expertise of practitioners, and improved value-based care. For example, some providers have embraced the Medicare Hospital Without Walls Initiative and will need to assess their options as some of those flexibilities are phased out. Other federal opportunities have newly emerged during the pandemic, such as the Rural Emergency Hospital designation and pending changes to the Medicare Shared Savings Program (MSSP).
What’s Next
The COVID-19 PHE declaration next expires on October 12, 2022. While a renewal of the PHE declaration is possible into early 2023, providers should be using this time to prepare for resumption of normal policies and procedures.
The expiration of PHE flexibilities and waivers are not, however, happening in a vacuum. Providers need to make this transition amidst a dynamic healthcare sector with high expectations for continuous improvement in quality, patient experiences, and value. During this transitional period HMA’s experts are working with health plans and providers to develop or revisit strategic plans and investments to refocus attention on improving models of care and value-based payment approaches, including strategies that will help mitigate health disparities.
For questions, please contact Melinda Estep, Mary Walter, and Andrea Maresca.
HMA Roundup
Arkansas
Arkansas Seeks Federal Approval to Offer Full Medicaid Coverage to Pregnant Women. KTLO reported on August 31, 2022, that Arkansas is seeking federal approval to offer full Medicaid coverage to pregnant women, not just services directly related to the pregnancy, that would include coverage of services like behavioral health care. The state is also making women with high-risk pregnancies eligible for home visits by a nurse during their pregnancy for up to 60 days after the baby is born. Read More
California
California Awards $340 Million Population Health Management Contract to Gainwell Technologies. The California Department of Health Care Services announced on September 6, 2022, its intent to award a $340 million contract for population health management (PHM) services to Gainwell Technologies as part of the state’s California Advancing and Innovating Medi-Cal (CalAIM) initiative. The PHM service will integrate data from multiple sources, perform core population health management functions, and give various types of users access to comprehensive, whole-person information about the Medi-Cal members they serve. The contract will begin on January 1, 2024, and run for three years, with one three-year option. Read More
CA Medicaid Plan Invests $14 Million to Address Rural Healthcare Needs in Kern County. 23ABC reported on September 6, 2022, that Kern Health Systems has invested $14 million to help address the healthcare needs of rural Medicaid enrollees in Kern County. Funding from Kern Health Systems, which is the Local Initiative for Medi-Cal Managed Care in the county, is being used to create partnerships with community providers, expand recuperative and respite care options, strengthen healthcare infrastructure, and address social needs like transportation, daycare, and translation services. Read More
Medi-Cal Contract Awards Face Appeals from Aetna, Blue Shield of CA, Community Health Group, Centene. The California Department of Health Care Services announced on September 2, 2022, that CVS Health/Aetna Better Health of California, Blue Shield of California Promise Health Plan, Community Health Group, and Centene/Health Net Community Solutions have submitted appeals of the recent California Medi-Cal Medicaid managed care awards. Aetna, Blue Shield of California, and Community Health all failed to win contracts. Centene was awarded contracts in nine counties but not in Los Angeles, Sacramento, and Kern counties. Read More
Iowa
Iowa Awards NEMT Contract to MTM. The Iowa Department of Human Services announced on September 1, 2022, its intent to award Medical Transportation Management (MTM) with a risk-based contract to provide non-emergency medical transportation (NEMT) services to the state’s fee-for-service (FFS) Medicaid population. The FFS population is estimated at between 10,000 and 12,000. The contract will begin on January 1, 2023, and run for three years with three one-year extension options. Read More
Maine
Governor Announces $1.9 Million Initiative to Expand SUD Treatment in Rural Areas. Maine Governor Janet Mills announced on August 31, 2022, a $1.9 million federally funded initiative to expand treatment of substance use disorder (SUD) in rural Maine. Funds would help behavioral health providers expand staff training and development and increase the number of patients they serve. The initiative will complement state grants for renovation and capital costs, which will be issued in late September, to increase the number of available beds for residential SUD treatment and medically supervised withdrawal. Read More
Maryland
Maryland Releases Dental Benefits Administrator RFP. The Maryland Department of Health released on September 6, 2022, a request for proposals (RFP) for a dental benefits administrator (DBA) to serve the state’s 1.6 million Medicaid enrollees. Previously, only certain populations received dental services through the Maryland Healthy Smiles Dental Program. However, Maryland enacted legislation to provide dental services, including diagnostic, preventive, restorative, and periodontal services, to all Medicaid enrollees effective January 1, 2023. The contract will run for two years following the implementation period, with three one-year renewal options. Proposals are due by November 22, 2022. Read More
Maryland Releases Medicaid NEMT Broker RFP. The Maryland Department of Health released on September 2, 2022, a request for proposals (RFP) for a statewide, Medicaid Non-Emergency Medical Transportation broker. Beginning February 2023, the broker will engage in design, development, and implementation with the state. Implementation will be in three phases. In phase one, the broker will serve at least nine of Maryland’s 24 jurisdictions, followed by expansion into the other jurisdictions in phase two. In phase three, the broker will serve all jurisdictions for three years, with two optional years, not to exceed seven years. Currently, NEMT services are managed separately by each local jurisdiction. Proposals are due November 1, 2022. Read More
Minnesota
Minnesota Reports 90,000 Basic Health Plan Members Will Benefit from Continued Enhanced Premium Subsidies. The Minnesota Department of Human Services reported on September 6, 2022, that 90,000 MinnesotaCare members will benefit from continued enhanced subsidies through the Inflation Reduction Act. MinnesotaCare is a Basic Health Plan, which covers individuals up to 200 percent of the federal poverty level (FPL). Individuals with incomes under 160 percent of poverty will not have to pay premiums, and individuals with incomes between 160 and 200 percent of poverty will pay reduced premiums through 2025. Read More
New Mexico
New Mexico Delays Medicaid Managed Care RFP Release to Third Quarter of 2022. The New Mexico Department of Health and Human Services announced In August that it would delay the release of a request for proposals (RFP) for the state’s Centennial Care Medicaid managed care program to the third quarter of 2022. The RFP was first scheduled to be released on September 2. Current incumbents are Blue Cross Blue Shield of New Mexico, Presbyterian Health Plan, and Centene/Western Sky Community Care. Read more.
New York
ACOs Save Medicare Program $450 Million in 2021, Crain’s Reports. Crain’s New York Business reported on September 7, 2022, that New York accountable care organizations (ACOs) saved the Medicare program about $450 million in 2021, according to a Crain’s analysis of federal data. Of the 51 Medicare ACOs in the state, 28 earned payments from the Centers for Medicare & Medicaid Services for their performance in the program. Read More
Oklahoma
Oklahoma Releases Medicaid Dental Managed Care RFP. The Oklahoma Health Care Authority (OHCA) released on September 1, 2022, a request for proposals (RFP) seeking at least two Medicaid dental managed care plans to serve 919,000 members. Contracts will run from the award date, which is expected to be between January 6, 2023, and June 30, 2023, with six one-year renewal options. Enrollment will begin on October 1, 2023. Proposals are due by October 31, 2022. Current dental benefit plans are DentaQuest, Liberty Dental Plan of Oklahoma, and MCNA Dental. Read More
Pennsylvania
Pennsylvania Medicaid Managed Care Contracts Are Implemented September 1. Philadelphia Business Journal reported on August 30, 2022, that the Pennsylvania Physical HealthChoices managed care contracts were implemented statewide on September 1, 2022. Read More
Tennessee
Tennessee Proposes PMPM Medicaid Spending Cap to Replace Proposed Aggregate Spending Cap. The Centers for Medicare & Medicaid Services (CMS) announced on September 6, 2022, that Tennessee has proposed a per member per month cap on Medicaid spending to address federal objections to a previously proposed aggregate spending cap or block grant. The new proposal is in the form of an amendment to the state’s pending TennCare III 1115 Medicaid waiver application. The amendment also proposes removing pharmacy expenditure authority and associated flexibilities and revising reinvestment frameworks for demonstration savings. Public comments will be accepted through October 6, 2022. Read More
Texas
Texas Delays Releases of STAR/CHIP, STAR Kids RFPs. The Texas Department of Health and Human Services announced on August 31, 2022, it has delayed posting the STAR and Children’s Health Insurance Program (CHIP) request for proposals (RFP) from the first quarter of fiscal 2023 to the second quarter of fiscal 2023 (between December 2022 and February 2023). The new contracts will be implemented in the second quarter of fiscal 2025, at least three months later than initially scheduled. Additionally, the release of the state’s STAR Kids RFP was delayed from the third quarter fiscal 2023 to the second quarter of fiscal 2024 (between December 2023 and February 2024). The STAR Kids contracts, which serve individuals with disabilities age 20 and younger, will be implemented in the second quarter of fiscal 2026, one year later than originally anticipated. Read More
Utah
Governor Appoints Executive Director, Chairman for One Utah Health Collaborative. Utah Governor Spencer Cox announced on September 6, 2022, that Jaime Wissler has been named executive director and Ryan Morley has been named chairman of the board of One Utah Health Collaborative, a community-owned not-for-profit launched in fall 2021. The One Utah Health Collaborative will work to reduce the growth of total Medicaid spending in the state as well as expand access to behavioral health care and wellness initiatives for Medicaid beneficiaries. Read More
National
CMS Seeks Public Input to Improve Programs, Policies. The Centers for Medicare & Medicaid Services (CMS) released on September 6, 2022, a request for information (RFI) on accessing healthcare and related challenges, understanding provider experiences, and advancing health equity. The RFI also seeks to assess the impact of COVID-19 waivers and flexibilities. CMS intends to use the comments to reduce disparities and promote efficiency and innovation across its programs and policies. Responses are due November 4, 2022. Read More
Skilled Nursing Facility Occupancy Was Flat at 77.3 Percent in June 2022, Report Finds. McKnight’s Senior Living reported on September 7, 2022, that occupancy in skilled nursing facilities decreased by nine basis points to 77.3 percent in June 2022, according to the Skilled Nursing Monthly Report from the National Investment Center for Seniors Housing & Care. Previously, occupancy had increased four months in a row. Read More
23 States, DC Extend Postpartum Medicaid Coverage to 12 Months. The Associated Press reported on September 5, 2022, that 23 states and the District of Columbia have extended postpartum Medicaid coverage to 12 months, with several more states planning to do so. Medicaid covers about 42 percent of births nationally. Read More
MedPAC Eyes Potential Standardized Benefit Options for Medicare Advantage. Fierce Healthcare reported on September 2, 2022, that the Medicare Payment Advisory Commission (MedPAC) is researching potential standardized benefit options for Medicare Advantage plans in an effort to simplify plan choice for seniors. The findings will be included in MedPAC’s annual report to Congress next year. Read More
52 Percent of MAGI Determinations Were Completed in Under 24 Hours, CMS Report Finds. The Centers for Medicare & Medicaid Services (CMS) released on September 1, 2022, its first quarterly Medicaid and Children’s Health Insurance Program (CHIP) Modified Adjusted Gross Income (MAGI) application processing time report, which found that 52 percent of MAGI determinations were completed in under 24 hours. The report also showed that about two thirds of determinations were completed within seven days. Missouri had the highest portion of Medicaid applications processed in over 45 days at 83 percent in March 2022. The report covered 47 states for the period from January to March 2022. Read More
CMS Proposes Rule to Standardize Medicaid, CHIP Eligibility and Enrollment. The Centers for Medicare & Medicaid Services (CMS) announced on August 31, 2022, a proposed rule that would standardize Medicaid and Children’s Health Insurance Program (CHIP) eligibility and enrollment procedures by limiting renewals to once every 12 months, allowing applicants 30 days to respond to information requests, and requiring prepopulated renewal forms. The proposed rule would also end lifetime benefit limits in CHIP, eliminate pre-enrollment waiting periods, and allow states to transfer children’s eligibility directly from Medicaid to CHIP. Finally, the rule proposes automatic consideration of older adults for Medicare Shared Savings Programs and standardization of state recordkeeping requirements. Public comments will be accepted through November 7. Read More
Medicare Advantage Plans With Higher Premiums Do Not Necessarily Provide Better Quality Care, Study Finds. Healthcare Finance News reported on August 31, 2022, that Medicare Advantage (MA) plans with higher premiums do not necessarily mean members will receive higher quality care, according to a RAND study published in the Journal of the American Medical Association. Rather than looking at MA premium prices alone, the study says, seniors should consider Star Ratings and other factors when selecting a plan. Read More
Major Gaps Exist in Behavioral Health Workforce, Study Finds. Health Affairs reported on August 30, 2022, that major gaps existed in the nation’s behavioral health workforce in 2020, with 50 percent of U.S. counties having no psychiatrists or addiction medicine specialists. The data comes from the Health Affairs Behavioral Health Workforce Tracker. Read More
Most State Medicaid Website Offer Information in Multiple Languages, Kaiser Reports. Kaiser Family Foundation (KFF) reported on August 26, 2022, that most state Medicaid websites offer information in multiple languages. However, KFF also reported that gaps exists. Translations may be available only in a limited number of languages, and translated information may be less reliable than information in English. In addition, most states do not make information and applications available in multiple formats to improve accessibility for individuals with disabilities. Read More
Industry News
CVS to Acquire Signify Health. CNBC reported on September 5, 2022, that CVS Health has agreed to acquire home health company Signify Health for approximately $8 billion in cash, or $30.50 per share. Private equity firm New Mountain Capital owns roughly 60 percent of Signify’s common stock. Read More
Maximus Retains Contract to Support CMS Contact Center Operations. The Washington Business Journal reported on September 2, 2022, that Maximus won a contract to continue supporting the contact center operations of the Centers for Medicare & Medicaid Services (CMS), which fields questions from enrollees about Medicare benefits and Exchange plans. The contract is for one year, with nine one-year options, and has a value $6.6 billion over the entire 10 years. Maximus is the current contract holder. Read More
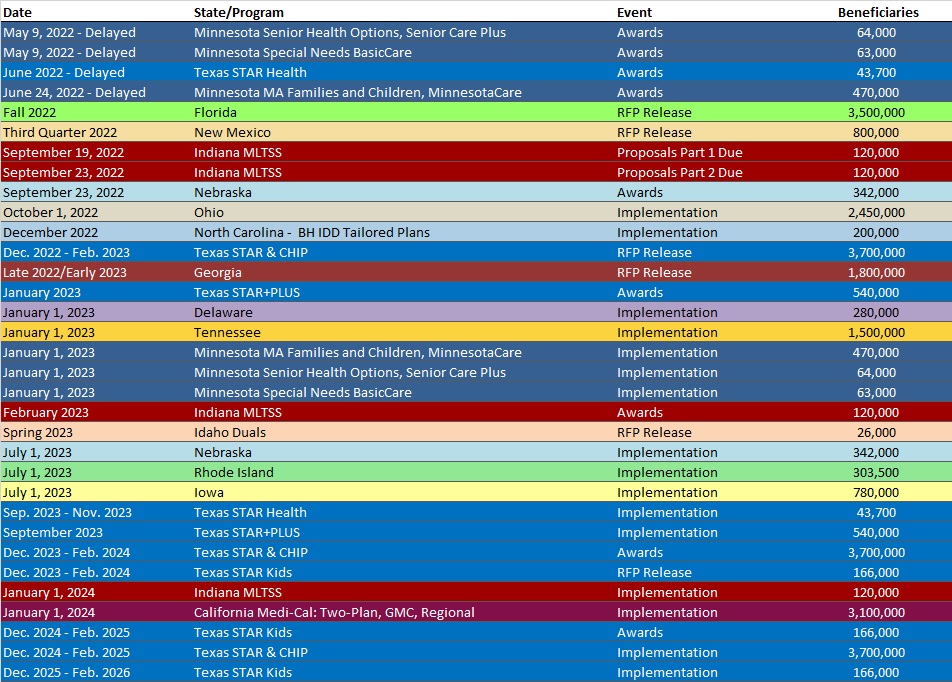
RFP Calendar
HMA News & Events
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- California Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Illinois Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Nevada Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- New Hampshire Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
Medicaid Financials and Utilization Data:
- MLRs Average 84.3% at Texas Medicaid MCOs, 2021 Data
- MLRs Average 84.4% at Utah Medicaid MCOs, 2021 Data
- MLRs Average 85.5% at Virginia Medicaid MCOs, 2021 Data
- MLRs Average 82.1% at Wisconsin Medicaid MCOs, 2021 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- California Medi-Cal Managed Care Two-Plan, GMC, and Regional Models RFP, Proposals, Evaluation, Awards, and Appeals, Sep-22
- California Population Health Management Service IFP and Award, Sep-22
- CMS Make Your Voice Heard RFI, Sep-22
- Iowa Health Link RFP, Proposals, Scoring, Awards, and Related Documents, 2022
- Iowa Medicaid NEMT RFP, Award, and Related Documents, 2022
- Maryland Medicaid Dental Benefits Administrator RFP, Sep-22
- Maryland Medicaid NEMT Administrator RFP, Sep-22
- New Hampshire Medicaid Care Management Dental Benefit RFI and Responses, Aug-22
- Oklahoma SoonerSelect Dental Program RFP, Sep-22
Medicaid Program Reports, Data, and Updates:
- New Mexico Medicaid Advisory Committee and Subcommittee Meeting Materials, Aug-22
- Oklahoma Medical Advisory Meeting Materials, 2017-22
- Texas Medicaid CHIP Data Analytics Unit Quarterly Reports, 2018-22
- Wyoming Medicaid Annual Reports, SFY 2013-21
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.