On May 16, 2022, no announcements were made concerning the impending end of the COVID-19 Public Health Emergency (PHE) declaration. What does this mean for state Medicaid programs and stakeholders, including consumers? When will the PHE declaration expire?
Today’s In Focus is the latest in our series discussing Medicaid’s preparations for the end of the PHE. HMA experts address these and other questions intertwined in the unprecedent “unwinding” work ahead for the Medicaid program.
The silence from the U.S. Department of Health and Human Services on May 16th means the Biden Administration is highly likely to sign another extension of the COVID-19 PHE declaration by July 15th. It is most likely that the PHE will then be renewed, for the maximum 3-month extension, to October 13th. While the Secretary could make an announcement to end the PHE before the full three months, the current experience with COVID-19 variants and fraught political climate make this scenario unlikely.
Beyond July, the Administration could continue to sign additional extensions of the PHE for the maximum three months permitted by statute. Regardless of the end date, the Administration committed to notify states and stakeholders 60 days before the scheduled end date.[i] Figure 1 describes key dates associated with potential future extensions of the COVID-19 PHE.
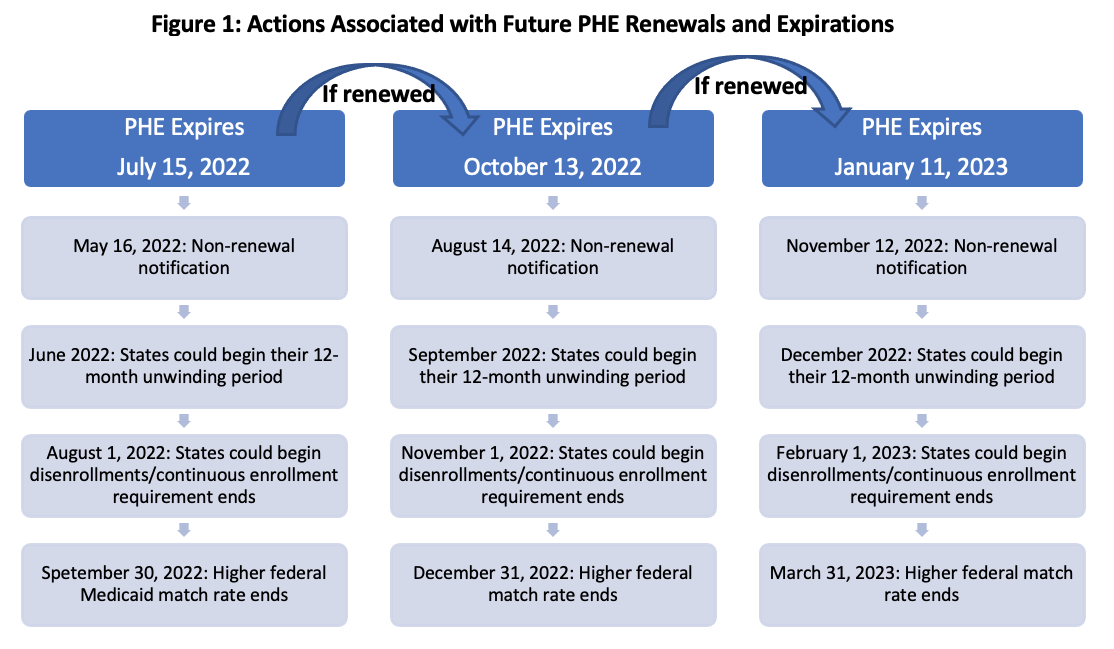
An extension of the COVID-19 PHE in July would provide more time to plan for its imminent end. HMA’s experts are working with stakeholders to use this additional time to develop and implement plans and improve processes to manage the PHE unwinding activities.
What Should States and Medicaid Stakeholders Do Now?
Although an extension cannot address the myriad of challenges for states and stakeholders, the following are some of the top-of-mind issues we are continuing to work with states, health plans, providers, community workers, and other stakeholders to address.
Operational and systems readiness. States and stakeholders now have more time to analyze, develop, and implement changes that will support more efficient eligibility and enrollment operations during and after the PHE unwinding period. Examples of high impact activities to support this function include:
- Stakeholders can continue to strengthen partnerships and processes to provide assistance to Medicaid enrollees and minimize unnecessary loss of coverage by eligible individuals.
- States, health plans, and other stakeholders can further solidify the operational plans for sharing member contact information files to prepare for renewals and redeterminations.
- States and stakeholders can also make on-line functionality mobile friendly and update workflow management systems.
Workforce. Training and retaining the eligibility workforce are among the most significant challenges for state and local governments. Stakeholders engaging with consumers may face similar challenges with their outreach and assistors. Strategies to alleviate some of these constraints include:
- State agencies could automate certain processes such as hand-offs to the Marketplace program.
- All stakeholders can update staffing models to support the anticipated volume of workload.
- Stakeholders should also be planning new staff training and refresher trainings, for eligibility workers and other staff who engage with Medicaid members.
Communications and outreach strategies. Working with individuals managing through complex life circumstances requires new or refreshed strategies. The months ahead will be an important time to:
- Assess relationships with trusted community partners.
- Test messaging and develop effective campaigns to engage members and trusted partners.
- Where permissible, pilot texting programs, implement opt-in for texting reminders, and improve texting capabilities to ensure two-way functionality to make the process more consumer friendly.
Marketplace collaboration and smoothing consumer transitions. Guidance from the Centers for Medicare and Medicaid Services (CMS) describes the variety of ways states can partner and engage their Medicaid health plans.[ii] One critical area that needs additional attention is the education and process for “handing off” Medicaid enrollees to the Marketplace. Some state marketing and insurance rules present barriers to smooth transitions. Potential strategies to address these challenges include:
- Stakeholders as well as state and local agencies can update and strengthen training on Marketplace requirements and processes for workers who will be engaging with consumers.
- State leaders can identify and pilot more consumer-friendly systems and processes. For example, state agencies could pilot changes to streamline health plan marketing rules designed to ease consumer transitions between coverage programs.
- State leaders and health plans can collaborate on materials and consistent messaging to support Medicaid and CHIP members transitioning to the Marketplace.
- State based marketplaces can offer special enrollment periods to help ease consumer transitions and smooth out the workload for assistors and program administrators.
Looking Ahead: Expect the Unexpected
Several recent developments make extensions of the PHE past July increasingly likely.
Notably, Administration officials and public health experts have begun discussing a potentially significant wave of COVID-19 infections and deaths this fall and winter, driven by new omicron subvariants.
Further, ending the PHE will inevitably lead to some otherwise eligible individuals losing Medicaid coverage and others to experience challenges in reconnecting with coverage. These are not favorable headlines for elected officials approaching November’s mid-term elections.
Another variable is the potential for Congress to make changes to law which links certain Medicaid policies to the PHE declaration. We cannot yet rule out the possibility that Congress could uncouple the PHE declaration from the higher federal Medicaid match rate and continuous coverage requirement (similar to a proposal incorporated in the House-passed Build Back Better Act).
Looking longer term, we are working with states and stakeholders to consider how they will assess the impact of their outreach and assistance and temporary policies. Collecting and analyzing this information as the work is underway can provide important information about effective strategies, unexpected challenges, and help with real time problem solving.
The near-term planning efforts and the operational and system transformations are applicable to the special circumstances surrounding the PHE unwinding. However, the vast majority are applicable as policymakers, state agencies, and stakeholders consider the future for consumer experiences and efficiencies for program administrators.
Please contact our HMA experts below for more information about our work with clients to address these issues.
Related posts:
HMA Experts Lay Out Scenarios for Transitioning from COVID-19 Public Health Emergency
[i] Note to the Communications Control Center (CCC)
[ii] Overview of Strategic Approach to Engaging Managed Care Plans to Maximize Continuity of Coverage as States Resume Normal Eligibility and Enrollment Operations MARCH 2022 UPDATE


