Individuals with behavioral health needs often find themselves involved with law enforcement or in hospital emergency rooms during times of crisis. Health Management Associates (HMA) has released a model framework examining a third option for care – Crisis Diversion Facilities.
114 Results found.

HMA experts author LA city and county studies
HMA Community Strategies (HMACS) experts have released a pair of evaluation reports commissioned by the City of Los Angeles and the County of Los Angeles.
HMACS worked with the Los Angeles Housing + Community Investment Department (HCIDLA) to facilitate the inaugural, interactive Los Angeles Poverty Prevention Summit and produced a report and policy recommendations.
The report, Breaking the Cycle of Poverty, Defining Innovative and Equitable Strategies, summarized ideas and input from the summit and provides analysis and recommendations to move forward by harnessing existing resources and leveraging them with other efforts to alleviate poverty in the county.
A second report, prepared for the Los Angeles County Chief Executive Office, evaluated strategies to combat homelessness put forth by the Office of Homeless Initiatives (HI). The evaluation of HI’s strategies is summarized in the report, Evaluating the Effectiveness of Los Angeles County’s Strategies to Expand and Enhance Interim Housing and Emergency Shelter Services. The report focuses on analyzing existing strategies and how they are preforming and goes on to identify best practices and areas of needed improvement.
HMACS is involved in continued work to address homelessness, poverty and other social determinants of health in Los Angeles County and beyond with the goal of improving health and wellbeing, particularly for at-risk patients and families.
The HMACS teams, led by Principal Charles Robbins, also included Catherine Guerrero, Nayely Chavez, and Rathi Ramasamy as well as Michael Stiffler and Kara Riehman.

HMA explores potential issues for individuals with end-stage renal disease enrolling in Medicare Advantage
Starting in 2021, Medicare beneficiaries with End-Stage Renal Disease (ESRD) will be able to enroll in any Medicare Advantage (MA) plan. The Anthem Public Policy Institute asked HMA to explore some of the potential issues associated with how MA plans are currently paid by the Centers for Medicare & Medicaid Services (CMS) for individuals with ESRD, and identify any possible modifications that CMS or Congress could make to more closely align payment with costs.
This white paper was prepared for Anthem Public Policy Institute by HMA Managing Principal Jon Blum, Principal Eric Hammelman, and Senior Consultant Narda Ipakchi.

HMA prepares report detailing economic implications of a Medicaid expansion in Missouri
On January 30, 2020, the Missouri Hospital Association issued a press release outlining a report prepared by Health Management Associates. Read the official press release.
The report, Medicaid Expansion in Missouri – Economic Implications for Missouri and Interviews Reflecting Arkansas, Indiana, and Ohio Experiences, was prepared by HMA MMS Managing Director Matt Powers and Managing Principal Sharon Silow-Carroll, and Jack Meyer. They conducted interviews with leaders directly involved with expansion in Arkansas, Indiana, and Ohio to evaluate the policy and operational adjustments they undertook to design a budget-conscious program while maximizing state value. Those interviews allowed clarification of many of the questions raised about state-level costs and budget savings of a potential Missouri expansion.
The report was commissioned by the Missouri Hospital Association and Missouri Primary Care Association and released in partnership with stakeholders from the healthcare community.

Hospital Charges and Reimbursement for Medicines: Analysis of Cost-to-Charge Ratios
This report is an update to a previous report examining hospital markups for separately paid drugs. Our prior analysis examined hospital charges and reimbursement for 20 drugs and found that hospitals marked up charges for those drugs, on average, 487 percent of their acquisition cost. We also found that hospitals receive 252 percent of estimated hospital acquisition cost from commercial payers. Hospital reimbursement data was obtained from the Magellan Rx Management Medical Pharmacy Trend Report™: 2016 Seventh Edition (the Magellan report) and charges were calculated from Medicare claims data. For more information, please refer to our prior analysis.

Michigan Medicaid Managed Care Results Announced
In previous editions of The Michigan Update (most recently in August) we have reported on the Michigan Department of Health and Human Services’ (MDHHS) release of a Request for Proposals (RFP) to re-procure its Medicaid managed care contracts. The RFP was released in early May with bidder responses due in early August. This procurement is for at least five years, with the possibility of up to three one-year extensions. The total cost of the procurement for five years is estimated to be $35 billion. On October 13, 2015 the State of Michigan announced the much anticipated results of the re-procurement.
Since the prices paid to the contracted HMOs are set by the state, the health plan selection was based solely on technical scores. The HMOs were required to bid on entire regions, which were configured differently than in the past. The reconfiguration required a number of the HMOs to expand their service areas to meet the “entire region” requirement. The new regional configuration appears in the map below:
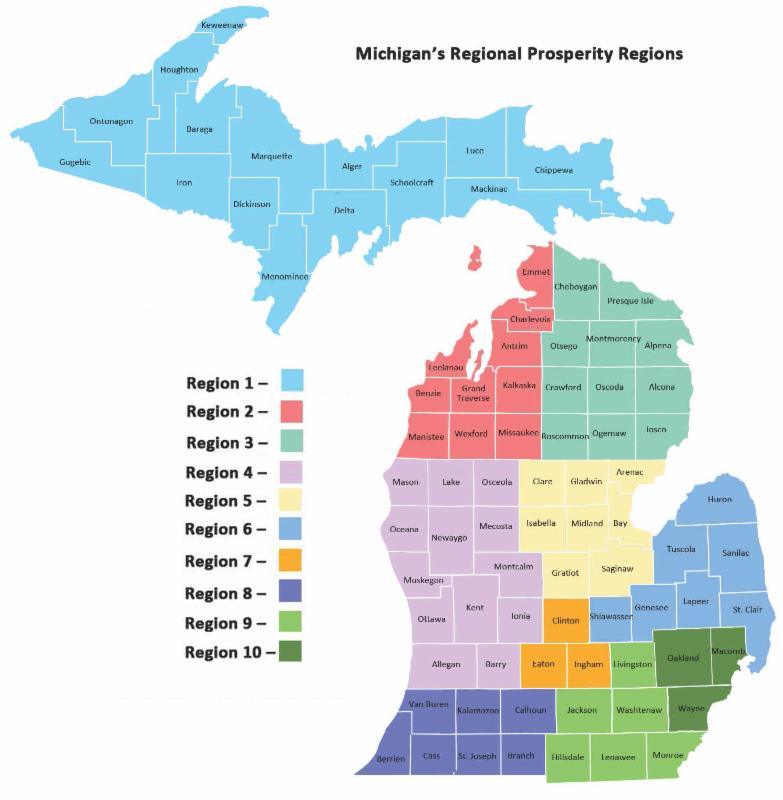
Note: Region 2 and Region 3 were required to be bid together.
The RFP included a proposed number of HMOs that would be awarded contracts for each of these regions. To minimize disruptions for Medicaid enrollees, in each region (other than the Upper Peninsula) the number of plans selected was one more than the proposed maximum number of awards for that region. Proposals from the HMOs were evaluated based on demonstrated competencies and also statements of their proposed approaches to many new initiatives related to population health, care management, behavioral health integration, patient-centered medical homes, health information technology and payment reform.
Not every HMO was successful in each region for which it submitted a bid. Two plans were not successful in any region. One is Sparrow PHP, which is an incumbent plan in Region 7. The other is MI Complete Health (Centene/Fidelis SecureCare) which is not currently a Medicaid plan in any part of the state but does have an Integrated Care Organization contract to serve dual Medicare/Medicaid enrollees in Macomb and Wayne counties as part of Michigan’s dual eligible demonstration.
The following table indicates the regions for which each bidding HMO was and was not successful. In addition, the numerical values show the rank of that plan based on their evaluation scores among the successful bidders for each region. If an HMO is a current contractor for all counties in a region, their result is shaded green. If the HMO is a current contractor for some but not all counties in a region, their result is shaded yellow. The number of Medicaid enrollees currently served in each of the regions, eligible through both “traditional” Medicaid and the Healthy Michigan Plan, appear in the bottom row on the table; across all regions, this is more than 1.6 million Medicaid enrollees.
Technical Evaluation Results
|
|
Region 1
|
Region 2
|
Region 3
|
Region 4
|
Region 5
|
Region 6
| Region 6 |
Region 8
|
Region 9
|
Region 10
|
|
Aetna Better Health
(CoventryCares)
|
|
|
|
|
No
|
|
|
Yes – 4
|
Yes – 4
|
Yes – 7
|
|
Blue Cross Complete
|
|
|
|
Yes – 3
|
|
Yes – 5
|
Yes – 3
|
|
Yes – 3
|
Yes – 5
|
|
HAP Midwest Health Plan
|
|
|
|
|
|
Yes – 6
|
|
|
No
|
No
|
|
Harbor Health
Plan
|
|
|
|
|
|
|
|
|
|
Yes – 8
|
|
McLaren Health
Plan
|
|
Yes – 3
|
Yes – 3
|
Yes – 4
|
Yes – 3
|
Yes – 3
|
Yes – 2
|
Yes – 3
|
Yes – 6
|
Yes – 4
|
|
Meridian Health Plan of MI
|
|
Yes – 1
|
Yes – 4
|
Yes – 5
|
Yes – 2
|
Yes – 4
|
No
|
Yes – 5
|
Yes – 5
|
Yes – 3
|
|
MI Complete Health
(Centene/Fidelis)
|
|
|
|
|
|
|
|
|
No
|
No
|
|
Molina Healthcare
of MI
|
|
Yes – 4
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
Yes – 1
|
Yes – 1
|
Yes – 1
|
Yes – 2
|
|
Priority Health Choice
|
|
No
|
No
|