As Medicare, state Medicaid agencies, Medicare Advantage plans, Medicaid managed care organizations, and commercial insurers increasingly adopt alternative payment models (APMs), Health Management Associates (HMA) provides a range of innovative and successful approaches to value-based care (VBC).
Our subject matter experts can help you succeed with
value-based payments (VBP).
WHAT WE DO
Offer insights for transforming the care delivery model to efficiently deliver optimal patient and population-level health outcomes while successfully managing total cost of care
Ensure quality is the primary goal of VBP program design and implementation
Develop payment models that align the incentives of payers and providers
Integrate physical and behavioral healthcare, and close gaps related to social determinants of health and health equity
Help clients successfully transition from fee-for-service to value-based payments by providing expertise in change management, analytics, network engagement, and IT infrastructure
Improve the patient and provider experience
Qualify, manage, and monitor health insurance risk
Prepare for and succeed in accreditation for VBP capabilities
ORGANIZATIONS WE SUPPORT
Those engaged in VBP or interested in engaging in VBP
Payers
Providers
Purchasers
Those interested in advancing the broader movement to value
Federal, State & Local Governments
Associations
Foundations
Investment Firms
HMA Can Support You Through All Phases of Value-Based Care
From contract to care plan, we have the experience and guidance tools to support your organization’s move to value-based care and risk-based contracting.
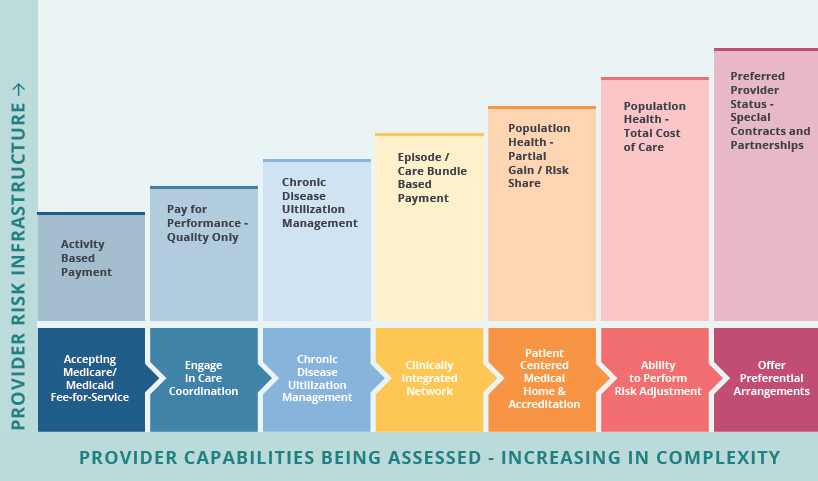
This graphic showcases the capabilities needed to address the complexities of risk-based contracting and deliver value-based care. As your organization moves from left-to-right along the glidepath to risk, additional strategies and capabilities must be developed. For example, utilizing Institute for Healthcare Improvement frameworks for quality improvement, regulatory and credentialing needs, and specialty access within a clinically integrated network. NEJM Catalyst. (2017). What is value-based healthcare?
Our philosophy involves applying a health equity model to close social determinant gaps and health disparities. Value-based healthcare is all about the care delivery model. Under value-based care agreements, providers are rewarded for helping patients improve their health, reduce the effects of emerging/rising risks and incidence of chronic disease, and live healthier lives in an evidence-based way.
Our Comprehensive Approach
Our collaborative approach will be tailored and customized to your needs to help you successfully implement VBP.
Our integrated process is based on the following model:
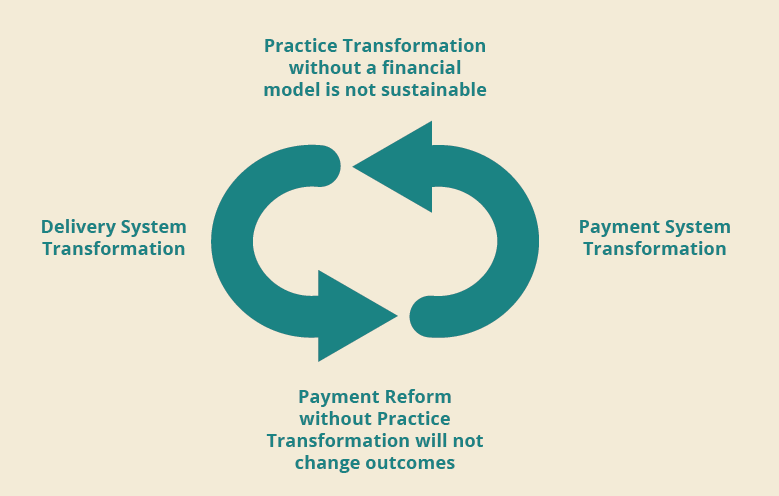
WHAT HMA PROVIDES
Determine readiness across key building blocks for moving to value-based payments and achieving continuous improvement across healthcare organizations.
Implementation that includes benchmarks and measurements of success. We facilitate stakeholder input to capture and analyze data from these interactions through surveys, focus groups, and interviews.
Aligning incentives with providers is key to successful value-based care strategies. Understanding methods for identifying and closing gaps in care pathways for common chronic conditions or addressing rising/emergent risks as well as how to create buy-in among providers and other members of the care team.
Including actuarial expertise required for contracting in key areas such as financial projections, reserves, total cost of care analysis, and benchmarking. We provide an assessment of third-party software to support APMs.
Including methods for incorporating whole-person care into clinical algorithms that apply to every interaction with the patient and their families. Integrating behavioral health with physical health and addressing social determinants of health/health-related social needs into VBC programs.
Assist with identifying key performance indicators (KPIs) and quality measurement incentives
for pay-for-performance or pay-for- value to support population health outcomes and support total cost of care in various VBP arrangements.
Provide support and consultation on scope of requirements to ensure VBC contract meets delegation requirements for operational, state, CMS regulatory and accreditation requirements.
OUR EXPERTS INCLUDE
Former CEOs, COOs, CFOs, and chief medical officers and other physician executives as well as executive quality leaders of the following organizations:
Providers including hospitals, academic medical centers, physician practices, community health centers, rural health centers, and federally qualified health centers
Medicaid, Medicare, Marketplace and Commercial MCOs
State and federal agencies
In addition, HMA offers expert actuaries, coders, analytic staff, and clinicians to support your transformation.
Contact our experts: