This week's roundup:
- In Focus: Biden Approves Major Health Care Proposals but the Work Is Just Beginning for CMS and Stakeholders
- Gain Knowledge and Networking Opportunities at HMA’s Annual Conference; More Than 300 Already Confirmed to Attend
- Arizona Works on New Health Plan Contracts for ALTCS-EPD Program
- Delaware Judge Denies Motion to Quash Audit of Medicaid Program
- District of Columbia Accepts Bids from 2 Medicaid Managed Care Plans
- Florida Medicaid Plan Capitated Rates to Fall, Driven by Lower Utilization
- Illinois Announces PACE Program Awardees
- Massachusetts Seeks Input on Improving Medicaid MCO/ACO Risk Adjustment Model
- Minnesota Releases RFP for School-Linked SUD Services for Students
- Missouri Medicaid Software Vendor Wins $23 Million in Lawsuit Against State
- Nebraska Delays Medicaid Managed Care Awards to August 31
- North Carolina Legislators Fail to Reach an Agreement on Medicaid Expansion
- CMS Proposes Rule to Expand Medically Necessary Dental Services Covered by Medicare
- Medicare Rates Expected to Rise 2.5 Percent for Inpatient Psychiatric Facilities in Fiscal 2023
- Humana to Acquire Wisconsin-based MCO Inclusa
- LHC Group Agrees to Acquire Three Rivers Home Health
In Focus
Biden Approves Major Health Care Proposals but the Work Is Just Beginning for CMS and Stakeholders
This week, our In Focus section reviews the Inflation Reduction Act of 2022 (IRA), signed by President Biden on August 16, 2022. The IRA advances major health care policy changes, including updates to Medicare’s drug benefit, authority for Medicare to negotiate drug prices, and another temporary extension of the enhanced subsidies to purchase health care coverage on Marketplaces. While the IRA provides the framework, critical details and policy decisions will be left to the Centers for Medicare & Medicaid Services (CMS) to develop and finalize in the coming months and years as the implementation dates for these policy changes are staggered over the next several years.
The IRA addresses a range of policy topics across health care, climate, energy, and taxation. Regarding health care, the IRA makes structural changes to the Medicare Part D drug benefit and provides new authority for the Medicare program to address the pricing of prescription drugs in the Part B and Part D programs. The measure also extends the temporary enhanced assistance for health coverage purchased from Marketplaces, which was first approved in the American Rescue Plan Act (ARPA). In addition, the IRA updates vaccine coverage policies in Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP).
While the IRA provides a critical framework for the structural changes to the nation’s largest public health insurance programs, the U.S. Department of Health and Human Services will be responsible for building out the policy and operational components necessary to support implementation.
Notably, the CMS will lead implementation of the IRA’s Medicare and Marketplace provisions. The changes to the Part D benefit and the development of entirely new processes and policies to support the IRA’s drug pricing provisions require significant resources and consideration of direct as well as indirect impacts for the health care market. The agency can use a variety of regulatory tools to support implementation, including issuing standalone Requests for Input (RFIs), convening stakeholder engagement sessions, updating policy manuals, and undertaking notice and comment via the formal rulemaking process, among others.
CMS’ strategic plan emphasizes the value of stakeholder engagement, and this is likely to lead CMS to offer multiple opportunities for public input as it implements the Medicare provisions of the IRA. For example, the agency must develop the policy parameters for reforming the Part D benefit design and is likely to seek input from Medicare Advantage (MA) and MA Prescription Drug Plans (MA-PDPs), providers, vendors, and consumer advocacy groups among others to inform its approach. CMS will also need input from the stakeholder community as it establishes the timelines, reporting, and negotiating mechanisms impacting Part B and D prescription drug pricing and how it will implement the inflation penalty policies outlined in the IRA.
The IRA’s extension of the American Rescue Plan Act’s (ARPA) enhanced eligibility for premium assistance through 2025 provides more near certainty around eligibility and enrollment for this market. Health insurers may need to reconsider pricing strategies among other issues as they consider this new landscape. The policy may also lead to renewed momentum for CMS to engage with states and stakeholders on Marketplace policies and structures.
Many of the details around how the IRA’s health care policies will be implemented are unknown at this time. Stakeholders will want to monitor CMS’ progress and provide feedback with data-informed analysis and concrete and practical recommendations as these opportunities are announced.
An overview of many of the IRA’s health care provisions follows. Our team of experts can provide tailored analysis and support to clients as they begin to unpack the full breadth of the IRA’s policy changes and implications for Medicare Advantage and Part D plans, providers, vendors, consumer advocacy groups and other stakeholders.
- Part B and Part D Drug Pricing. Requires the Secretary of HHS to select a list of drugs eligible for negotiation, and enter into agreements with select manufacturers, negotiating a “maximum fair price” (MFP) for each selected drug in the Medicare program. The Secretary is required to negotiate on a certain number of drugs per year, 10 drugs in 2026; 15 drugs in 2027 and 2028, and 20 drugs in 2029 and subsequent years. Manufacturers who are not in compliance will face an excise tax and civil monetary penalties.
- Prescription Drug Inflation Rebates. Requires manufacturers to pay rebates for Medicare Part B and D drugs with prices rising faster than inflation. The rebate calculation would be based on units and pricing in Medicare and would determine an inflation-adjusted payment amount based on the percentage by which the price exceeds the inflation benchmark, as determined by the Consumer Price Index for All Urban Consumers (CPI-U). If a manufacturer fails to pay the rebate, then they would be subject to a civil monetary penalty either equal to or at least 125 percent of the rebate amount for the quarter.
- The Part D inflation rebate takes effect October 2022 for Part D drugs and biologics.
- The Part B inflation rebate begins January 2023 for single-source drugs or biologics and certain biosimilar products. The IRA also includes an inflation growth cap on beneficiary coinsurance in Part B, beginning April 2023.
- Part B Payment for Biosimilar Biological Products. Amends Medicare’s Average Sales Price (ASP) payment methodology in cases where the ASP during the first quarter of sales is unavailable to establish a payment rate for biosimilars. The IRA also updates Medicare Part B reimbursement for certain biosimilar products for a five-year period beginning on October 1, 2022, by increasing the add-on payment from six percent of the reference product’s ASP to eight percent of the reference product ASP.
- Medicare Part D Assistance for Beneficiaries and Benefit Design. Increases the qualifying income amount (federal poverty level (FPL)) for the full Low-Income Subsidies (LIS) under Part D, from 135 percent of the FPL to 150 percent of the FPL, starting in 2024. The IRA also adjusts the cost-sharing requirements in the Part D benefit by:
- Setting an annual out-of-pocket (OOP) limit for enrollees at $2,000 beginning in 2025;
- Capping monthly premium increases for a prescription drug plan in 2024 through 2029 at six percent per year. The Secretary may make a one-time adjustment to the beneficiary Part D premium contribution percentage in 2030 to ensure longer-term beneficiary premium reduction; and
- Adjusting the benefit coverage liabilities for the initial coverage phase and catastrophic coverage phase.
- Coverage for Insulin. Requires Medicare to cover select insulin products and not apply a deductible or impose cost-sharing more than $35 or 25 percent of the negotiated price (including all discounts) for a 30-day supply. Beginning in July 2023, Medicare must exempt from beneficiary deductibles insulin provided through durable medical equipment (DME) and ensure that coinsurance for a month’s supply of insulin administered through DME does not exceed $35. High-deductible health plans (HDHPs) will be able to cover selected insulin products with no deductible without impacting their status as a HDHP, starting in 2023.
- Medicare, Medicaid, and CHIP Coverage for Vaccines. Requires full coverage of Advisory Committee on Immunization Practices (ACIP)-recommended adult vaccines under Medicaid and CHIP without cost-sharing. The IRA also increases the Federal Medical Assistance Percentage (FMAP) by one percentage point, for adult medical assistance for such vaccines and their administration, during the first eight fiscal quarters on or after the date of the IRA’s enactment.
- Requires Medicare Part D provide full coverage without cost sharing of ACIP-recommended adult vaccines for plan years beginning on or after January 1, 2023.
- Enhanced Temporary Assistance for Marketplace Coverage. Extends the ARPA’s expansion of Advanced Premium Tax Credit (APTC) eligibility and amounts through 2025. ARPA modified the affordability percentages used for the calculation of APTC to increase subsidy amounts for individuals eligible for assistance.
Experts from HMA and HMA companies are supporting clients as they begin to strategize and formulate initial recommendations for federal agencies and plan for implementation. We will continue to monitor developments in this area and provide additional updates as more information becomes available. For more information contact:
Amy Bassano, Managing Director, Medicare
Julie Faulhaber, Managing Director, Medicare and Dual Eligibles
Kevin Kirby, Managing Director, The Moran Company
Zach Gaumer, Principal
Andrea Maresca, Principal, Federal Policy
Gain Knowledge and Networking Opportunities at HMA’s Annual Conference; More Than 300 Already Confirmed to Attend
More than 300 executives from health plans, providers, state and federal government, investment firms, community-based organizations, and others are already confirmed to attend HMA’s annual conference, October 10-11 at the Fairmont Chicago Millennium Park, offering significant networking opportunities along with best-in-class content.
This year’s event, The New Normal: How Medicaid, Medicare, and Other Publicly Sponsored Programs Are Shaping the Future of Healthcare in a Time of Crisis, will feature more than 45 speakers and cover state Medicaid priorities, managed care opportunities, Medicare policy, value-based payments, and much more.
Sponsorships and group discounts are available. For additional information, contact Carl Mercurio, [email protected].
HMA Roundup
Arizona
Arizona Works on New Health Plan Contracts for ALTCS-EPD Program. The Arizona Health Care Cost Containment System (AHCCCS) announced on August 11, 2022, that it is working on new health plan contracts for the Arizona Long Term Care System for Elderly and Physically Disabled (ALTCS-EPD) program. The state will hold meetings this month for input from AHCCCS members and providers. Read More
Colorado
Colorado Law to Promote Hospital Price Transparency Takes Effect. Fierce Healthcare reported on August 10, 2022, that Colorado implemented a law preventing hospitals and debt collectors from going after patients with unpaid medical bills if the hospitals’ website is not compliant with federal requirements for price transparency. Under the law, patients can file a lawsuit citing non-compliance, putting hospitals at risk for patient medical debt and legal fees. Critical access hospitals must have compliant websites before February 15, 2023. Read More
Delaware
Delaware Judge Denies Motion to Quash Audit of Medicaid Program. The Associated Press reported on August 10, 2022, that Delaware auditor Kathleen McGuiness got the OK from a state judge to subpoena information to conduct an audit of Medicaid beneficiary eligibility for the time period July 1, 2017, through June 30, 2020. McGuiness has been seeking to conduct the audit since May 2021. The state Department of Health and Social Services had filed a motion to quash a subpoena, which the judge denied. Read More
District of Columbia
District of Columbia Accepts Bids from 2 Medicaid Managed Care Plans. The Washington Informer reported on August 10, 2022, that Medicaid managed care contract bids submitted by AmeriHealth Caritas and Anthem/Amerigroup have been accepted by the District of Columbia for potential contract awards. Anthem/Amerigroup’s bid was initially disqualified, but the decision was later overturned by the District’s Contract Appeals Board. CareFirst Blue Cross Blue Shield Community Health Plan and MedStar Family Choice were the other two bidders. District law requires three Medicaid managed care organizations to move forward with awarding contracts. Read More
Florida
Florida Medicaid Will Not Cover Gender-Affirming Medical Treatments. Politico reported on August 11, 2022, that the Florida Agency for Health Care Administration issued a rule declaring that gender-affirming medical treatments are not covered by Medicaid, effective August 21, 2022. The rule applies to puberty blockers, hormone therapies, and surgical procedures as a treatment for gender dysphoria. Read More
Medicaid Plan Capitated Rates to Fall, Driven by Lower Utilization. Florida Politics reported on August 10, 2022, that Florida Medicaid managed care plans are likely to see a 4.5 percent reduction in capitated payment rates from the state effective October, driven by lower healthcare utilization during the COVID-19 pandemic, according to Medicaid director Tom Wallace. Managed dental plans will see an 8.7 percent rate reduction and children’s medical services 3.1 percent. Rates will rise 8.4 percent for managed long-term care plans, largely because of legislation requiring wage increases for long-term care workers. Read More
Georgia
Georgia to Give $350 Each to 3 Million Low-Income Residents. The Associated Press reported on August 15, 2022, that Georgia will give $350 each to more than three million low-income individuals enrolled in Medicaid, Child Health Insurance Program (CHIP), food stamps, or welfare. The funding will come from $1.2 billion in federal COVID-19 aid, which Governor Brian Kemp can direct as he sees fit. Read More
Guam
Guam Seeks Federal Approval of 1115 Waiver for Medicaid Drug Rebate Program Exemption. The Centers for Medicare & Medicaid Services announced on August 15, 2022, that Guam submitted a Section 1115 waiver request to be exempt from participation in the Medicaid Drug Rebate Program, as it would require the territory to carry and cover more drugs than it believes is feasible with the current pharmacy provider capacity. Public comments will be accepted through September 14, 2022. Read More
Illinois
Illinois Announces PACE Program Awardees. Illinois Governor JB Pritzker announced on August 15, 2022, the launch of the state’s Program of All-Inclusive Care for the Elderly (PACE) to expand options for community-based care and serve as an alternative to traditional nursing facility care for older adults in the state. The Illinois Department of Healthcare and Family Services has awarded eight organizations in five service areas of the state. The PACE program is available for adults aged 55 and older who are Medicare and Medicaid dual eligibles. PACE providers are anticipated to begin providing services in fiscal 2024. Read More
Massachusetts
Massachusetts Seeks Input on Improving Medicaid MCO/ACO Risk Adjustment Model. The Massachusetts Executive Office of Health and Human Services (EOHHS) released on August 12, 2022, a request for information (RFI) seeking input from stakeholders on improving its Medicaid MassHealth accountable care organization (ACO)/managed care organization (MCO) risk adjustment model. The RFI has a specific focus on how to adjust for social determinants of health and alternative sources of data that would help inform member needs beyond medical diagnoses. Responses are due on September 23. Read More
Minnesota
Minnesota Releases RFP for School-Linked SUD Services for Students. The Minnesota Department of Human Services released on August 15, 2022, a request for proposals (RFP) seeking a current Minnesota Health Care Programs provider agency to provide school-linked substance use disorder (SUD) services to students and families. The contract is anticipated to begin on January 1, 2023, and run through June 30, 2026. Proposals are due on October 17. Read More
Missouri
Missouri Medicaid Software Vendor Wins $23 Million in Lawsuit Against State. The Missouri Independent reported on August 16, 2022, that software integrator EngagePoint won more than $23 million in a six-year-old lawsuit that alleged breach of contract by the Missouri Department of Social Services. EngagePoint had been hired in 2013 to implement the Missouri Human Services Eligibility, Enrollment and Case Management System for state programs like Medicaid. Read More
Nebraska
Nebraska Delays Medicaid Managed Care Awards to August 31. Health Payer Specialist reported on August 10, 2022, that the Nebraska Heritage Health Medicaid managed care contract award announcements will be delayed until August 31, 12 days later than originally intended. Contracts are set to be implemented on July 1, 2023. Five plans submitted bids: Anthem, Centene, United, Medica, and Molina. Read More
New York
Health Centers Push for $1 Billion to Bolster Primary Care Mental Health Services. Spectrum News reported on August 12, 2022, that New York community health centers are pushing for a $1 billion plan to bolster primary care mental health services over the next five years. The funding would come from the state’s $13.5 billion Section 1115 Medicaid waiver amendment proposal, which will address social determinants of health. Read More
North Carolina
Legislators Fail to Reach an Agreement on Medicaid Expansion. Axios reported on August 15, 2022, that North Carolina legislators failed to reach an agreement during the legislative session to expand Medicaid due to an inability to agree on the Senate’s inclusion of loosened certificate of need laws. The North Carolina Healthcare Association, which represents hospitals in the state, lobbied against the Senate plan, in favor of the House proposal. Read More
South Dakota
South Dakota Sees Increase in Percentage of People in Medicaid Coverage Gap. The Mitchell Republic reported on August 11, 2022, that 42,500 individuals in South Dakota are in the Medicaid coverage gap, meaning they would be eligible if the state expanded Medicaid. That is 35 percent of the total number of individuals up to 133 percent of poverty, an increase of four percentage points between 2018 and 2020. South Dakotans will vote to expand Medicaid through a ballot initiative in November. Read More
Texas
Lawmakers Seek Reconsideration of Postpartum Medicaid Extension Proposal. InsuranceNewsNet/Allied News reported on August 12, 2022, that 128 Texas lawmakers sent a letter asking the Centers for Medicare & Medicaid Services (CMS) to reconsider the state’s Section 1115 waiver application to extend postpartum Medicaid coverage from two to six months. CMS indicated it would reject the application because the benefits would not be available to mothers who had an abortion. Read More
Virginia
Medicaid, CHIP Behavioral Health Utilization Rate 16 Percent in Fiscal 2022. Open Minds reported on August 11, 2022, that about 305,000 Virginia Medicaid and Children’s Health Insurance Program (CHIP) enrollees, or 16 percent of total program enrollment, received residential or outpatient behavioral health services in fiscal 2022, according to the Virginia Medicaid behavioral health dashboard. The state spent $1.2 billion on these services or $4,056 per person. Read More
National
HHS Approves Extension of Postpartum Medicaid Coverage to 12 Months in HI, MD, OH. The U.S. Department of Health and Human Services (HHS) announced on August 16, 2022, that it approved the extension of postpartum Medicaid coverage to 12 months in Hawaii, Maryland, and Ohio. The extensions will impact an additional 34,000 people annually. Read More
CMS Proposes Rule to Expand Medically Necessary Dental Services Covered by Medicare. Bloomberg Law reported on August 17, 2022, that the Centers for Medicare & Medicaid Services (CMS) proposed a rule that would expand Medicare coverage of medically necessary dental services that could have an impact on other types of covered medical services. The expanded coverage would include dental services that impact emergency department visits or hospitalizations, help avoid complications in treating Parkinson’s disease, prevent treatment interruptions for gastrointestinal diseases, or help avoid infections in patients with diabetes or recovering from hip and knee surgery. Read More
FTC Calls For End to Hospital Mergers Under State Certificate of Public Advantage Laws. Modern Healthcare reported on August 16, 2022, that Federal Trade Commission (FTC) called for an end to hospital mergers under certificate of public advantage (COPA) laws, which can result in mergers “likely to harm patients and employees.” The FTC is reworking its hospital merger guidelines and hopes stricter legislation will lead to fewer mergers that decrease competition. Read More
Some FQHC’s Saw Profit Margins of Over 20 Percent For Consecutive Years, KHN Analysis Finds. Kaiser Health News (KHN) reported on August 15, 2022, that nine federally qualified health centers (FQHC’s) had margins of 20 percent or more for at least three years since 2019, according to a KHN analysis. The report indicates that the high profit margins may indicate that federal scrutiny of FQHC spending is needed to ensure appropriate resource allocation. The industry average is 5 percent, according to a federally funded report. Read More
40 States Cover Around-the-Clock HCBS through Medicaid Waiver Programs, Analysis Finds. McKnight’s Senior Living reported on August 15, 2022, that in 2020, 40 states covered around-the-clock home and community-based services (HCBS), similar to those provided in assisted living communities, through Medicaid waiver programs, according to a Health Affairs analysis. The analysis also found that state Medicaid programs expanded the use of HCBS during the study period, with almost all of the service categories seeing an increase in coverage and spending. The analysis looked at Medicaid HCBS Section 1915(c) waivers and Section 1115 demonstration projects targeting older adults between 1998 and 2020. Read More
Part D Plans Choose High-Cost, Brand-Name Hepatitis C Drugs Over Generics, Report Finds. Fierce Healthcare reported on August 11, 2022, that some Medicare Part D plans did not include generic versions of hepatitis C drugs on their formularies, costing the Medicare program millions of dollars, according to a report from the U.S. Inspector General. The Part D program, including manufacturer rebates, may be incentivizing plans to choose name-brand hepatitis C drugs, according to the report. The Inflation Reduction Act, which is expected to be voted on by the House on August 12, is expected to encourage lower-cost drug choices. Read More
Medicare Rates Expected to Rise 2.5 Percent for Inpatient Psychiatric Facilities in Fiscal 2023. The Centers for Medicare & Medicaid Services (CMS) released on July 29, 2022, the fiscal 2023 Inpatient Psychiatric Facilities (IPF) Prospective Payment System rule, which CMS estimates will result in a net increase in payments for Medicare inpatient hospital services by 2.5 percent. Increases will be 2.5 percent in urban areas and 2.9 percent in rural areas. The rule, effective October 1, also establishes a policy to ease the impact of yearly IPF payment changes. Read More
Industry News
Humana to Acquire Wisconsin-based MCO Inclusa. Humana announced on August 12, 2022, an agreement to acquire Inclusa, a Medicaid managed long-term care organization serving 16,600 adults in Wisconsin through the Family Care program. Inclusa serves 68 of Wisconsin’s 72 counties. Read More
LHC Group Agrees to Acquire Three Rivers Home Health. LHC Group announced on August 16, 2022, an agreement to acquire Three Rivers Home Health, a home care provider in Georgia. The acquisition is expected to close in late 2022. Read More
Amazon Care to Add On-Demand Behavioral Health Services through Teletherapy Startup Ginger. Fierce Healthcare reported on August 10, 2022, that Amazon Care will add on-demand mental health services like behavioral health coaches, licensed therapists, and psychiatrists to its suite of healthcare services through an arrangement with teletherapy startup Ginger. Amazon Care currently offers virtual health visits, in-person primary care visits at patients’ homes or offices, and prescription delivery. Read More
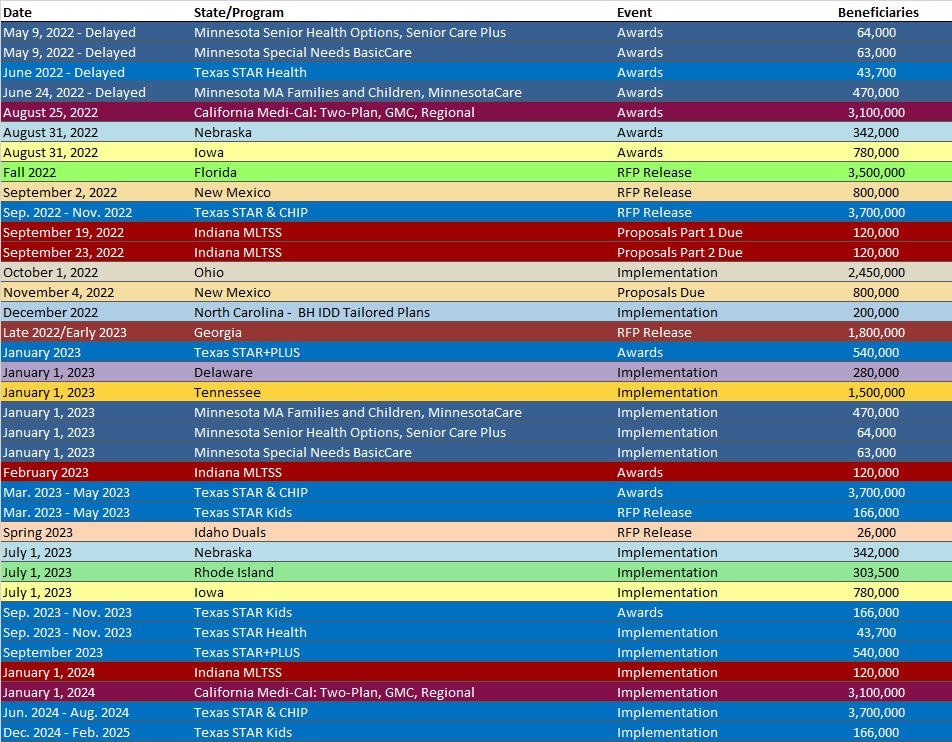
RFP Calendar
HMA News & Events
HMA WELCOMES
Swati Awsare, MD, Principal – San Francisco, CA
An innovative and evidence-based physician executive, Swati Awsare, MD utilizes best practices, process improvement and operational efficiencies to elevate clinical outcomes, patient experiences and organizational performance while reducing total cost of care.
Board Certified in Internal Medicine, Dr. Awsare’s clinical practice included outpatient primary care in addition to serving as an inpatient hospitalist. As an AHIP Certified Health Insurance Executive, Dr. Awsare has held clinical leadership roles in regional and national health plans serving Medicare, Medicaid and commercial members across medical, pharmacy and behavioral health services. She has also served in an integrated delivery system as a chief medical executive as well as a medical management and self-insured employer health benefits consultant.
Before joining HMA, Dr. Awsare led her own consulting company where she worked to elevate clinical and operational performance while improving population health to ensure high quality, evidence-based care in the most cost-effective settings. She has advised and provided leadership to clients in pharmaceutical, diagnostics, medical device, remote patient monitoring, telemedicine and the digital health technology sectors. Additionally, she has served as a chief medical officer on demand for the Employer Health Innovation Roundtable, the Health Plan Innovation Roundtable and the Provider Health Innovation Roundtables.
As a physician executive in diverse organizations, Dr. Awsare’s roles have included serving as the senior vice president and chief medical officer in Magellan Health’s Specialty Division, as chief medical executive of Health Plan Partnerships and Products with Sutter Health, as regional vice president and medical director with Anthem, Inc., and as a medical director with Aetna, Inc. She has deep experience optimizing Medicare Stars, Healthcare Effectiveness Data and Information Set (HEDIS), Value Based Care & Payment, Hierarchical Condition Categories (HCCs) & Risk Adjustment, utilization management, pharmacy, quality and accreditation performance.
Dr. Awsare earned a Doctorate in Medicine from the University of Southern California’s School of Medicine in Los Angeles as well as a Bachelor of Arts in psychology and a Bachelor of Science in Biological Sciences from the University of California, Irvine.
She is currently a guest lecturer on The Business of Medicine at California Northstate University’s College of Medicine. She also volunteers on the Cornell University Family Fellows Committee and as a premedical student mentor.
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Connecticut Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Delaware Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Georgia Medicaid Managed Care Enrollment is Up 5.8%, Aug-22 Data
- Georgia Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Louisiana Medicaid Managed Care Enrollment is Up 2.8%, May-22 Data
- Pennsylvania Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Rhode Island Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- South Dakota Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Tennessee Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Vermont Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Washington Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- West Virginia Medicaid Managed Care Enrollment is Up 3%, May-22 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Massachusetts Medicaid Risk Adjustment Model and the Use of Social Determinants of Health in Risk Adjustment RFI, Aug-22
- Minnesota School-Linked Substance Use Disorder Services for Students and Families RFP, Aug-22
- New York Medicaid External Quality Review, Utilization Review, Quality Improvement and AIDS Intervention Management System Activities Solicitation of Interest, 2019-22
- New York Office of Mental Health Managed Service Providers RFI, Aug-22
- Ohio Clark County Medicaid NEMT Provider RFP, Aug-22
- Vermont Long-Term Care Facilities Specialty Care RFP, Aug-22
Medicaid Program Reports, Data, and Updates:
- Iowa Medicaid Managed Care Rate Certification and Appendices, FY 2022
- Michigan Managed Health Plan Medical Risk Adjustment, 2021-22
- Oregon CCO Metrics Final Reports, 2017-21
- Texas Behavioral Health Presentations to Legislature, Aug-22
- Texas HHSC Women’s Health Programs Reports, FY 2018-21
- Texas Presentation to the House Select Committee on Health Care Reform, Aug-22
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.