This week's roundup:
- In Focus: HMA Identifies Key Trends for Emerging Medicaid Section 1115 Demonstration Proposals
- California Delays Medi-Cal Managed Care Program Awards
- Connecticut HUSKY Health to Cover Additional Maternity Benefits in 2023
- Florida Medicaid Managed Care RFI Responses Stress Social Determinants, Providers, HCBS
- Georgia Proposal to Bypass Healthcare.gov Is Again Rejected by CMS
- Idaho Releases Quality Improvement Organization RFP
- Mississippi Awards MississippiCAN, CHIP Medicaid Managed Care Contracts to 3 Health Plans
- Missouri Commits to Trimming Medicaid Applications Backlog Under Federal Plan
- Ohio Pharmacists Express Concern Over Single PBM Program
- West Virginia Medicaid Must Cover Gender-Affirming Care, Federal Judge Rules
- U.S. Senate Passes Legislation Allowing Medicare to Negotiate Drug Prices, Extending Enhanced Exchange Subsidies
- CVS Is Reportedly Interested in Acquiring Signify Health
- UnitedHealth/Optum Acquires CareMount Medical
In Focus
HMA Identifies Key Trends for Emerging Medicaid Section 1115 Demonstration Proposals
As the urgent needs of COVID-19 Public Health Emergency (PHE) continue to subside, state Medicaid agencies are exploring pathways and concepts to further address the historic inequities and health disparities laid bare by the pandemic. These efforts are closely aligned with the current Administration’s policy objectives for the Medicaid program, specifically:
- Addressing health equity
- Improving access and coverage
- Promoting whole person care
For several decades, Medicaid Section 1115 demonstration programs have provided a powerful lever for federal and state policymakers to design, implement, and evaluate transformative initiatives. All states administer at least one Section 1115 demonstration program. Some demonstrations are narrowly tailored to address services or populations while others capture broader features pertaining to coverage, benefits, and payment and delivery system innovations.
Notably, a new wave of comprehensive and transformative Medicaid Section 1115 demonstration proposals is emerging.
Working closely with the Centers for Medicare and Medicaid Services (CMS), states are developing proposals that place individuals at the center of health care in an entirely new way – by recognizing their medical needs as well as the complexity of circumstances and environmental factors that shape the individual’s medical, physical, and behavioral care needs and outcomes.
Teams of experts from across the HMA family of companies are supporting state agencies, counties, health plans, providers, community and consumer organizations, and other stakeholders with translating federal goals and parameters into concrete proposals as these move through the stages of concept paper, application and negotiation, and implementation. Demonstrations will reflect each state’s unique political and policy landscapes, but the programs will be grounded in certain federal goals and expectations to enhance accountability and improve outcomes.
Our experts identified three trends in state 1115 demonstration programs. In this and subsequent In Focus posts we will share our team’s initial insights and considerations for stakeholders based on our collective “on the ground” expertise. We include illustrative examples from some states with approved and pending Section 1115 proposals.
Section 1115 Trend #1: States are advancing a new vision for Medicaid’s role in addressing health equity, influenced by social drivers and grounded in a community’s needs.
CMS is strongly encouraging states to consider initiatives that address health inequities and community specific social drivers of health. As evidenced by the current state initiatives, Section 1115 demonstration programs will be a primary — but not the only — pathway states utilize to design strategies to address health inequities driven by non-health systems and circumstances. Based on our work with states and stakeholders, it is critical that states ensure the services are directly linked to factors that impact health outcomes for Medicaid enrollees and that they have mechanisms to evaluate the impact of community and social care services.
Several state proposals already signal CMS’ current vision for using Section 1115 authority to test new types of assistance within service categories to include non-medical services, services tailored to populations, and assistance that is linked to desired outcomes. For example:
North Carolina’s Section 1115 pilot program will provide support to certain groups of consumers for an array of community supports ranging from housing related services and transportation access to interpersonal violence and access to food and nutrition services. The program includes help for consumers related to utility set up and moving costs, and support to connect with community services to address legal issues impacting housing and thereby impacting health.
CMS’ approval of the North Carolina and California programs is paving the way for conversations in other states, including New York, New Jersey, and Oregon among others. Negotiations on similar initiatives to address health equity in other states, include:

Conclusion
North Carolina and California offer important insights into what may be possible and as importantly, what may be beyond the bounds of CMS’ Medicaid authority. Chief among the outstanding issues for states and stakeholders is whether additional innovative programs for addressing health disparities among justice-involved populations is possible under Medicaid’s demonstration authority.
CMS may use the experience with initial states to provide more concrete information on these general parameters and expectations. Formal guidance would prove helpful to states and stakeholders seeking to apply new knowledge and experiences with health inequities into practice within the Medicaid programs.
HMA’s interdisciplinary teams of Medicaid, human services, and actuarial experts are assisting states as well as stakeholders as they conceptualize, develop, and implement Section 1115 programs. To learn more about our work and the breadth of our services please contact HMA consultant Andrea Maresca, Principal.
HMA Roundup
California
California Delays Medi-Cal Managed Care Program Awards. The California Department of Health Care Services (DHCS) announced on August 8, 2022, that it had delayed the award announcement for the state’s Medi-Cal managed care program contracts to August 25. The state, which previously expected to make an announcement on August 9, is procuring contracts for three of the state’s Medicaid managed care plan models in 24 counties. Implementation remains set for October 10, 2022. Read More
Connecticut
Connecticut HUSKY Health to Cover Additional Maternity Benefits in 2023. My Record-Journal reported on August 8, 2022, that the Connecticut HUSKY Health Medicaid program will cover doula care, breastfeeding support, and other maternity services effective summer 2023. The state has allocated an additional $830,000 to improve maternal health outcomes.
Connecticut Faces Lawsuit Over Disenrolling Medicaid Members During COVID-19. WSHU reported on August 9, 2022, that about 6,600 Connecticut residents were disenrolled from Medicaid during the COVID-19 pandemic. Disability Rights Connecticut is filing a federal lawsuit on behalf of three beneficiaries who claim they were wrongly disenrolled. Read More
Florida
Medicaid Managed Care RFI Responses Stress Social Determinants, Providers, HCBS. State of Reform reported on August 9, 2022, that responses to a request for information (RFI) concerning Florida’s upcoming statewide Medicaid managed care procurement stressed social determinants of health, improving the Medicaid provider experience, and improving home and community-based services (HCBS). The state received 57 responses from health plans, providers, and other stakeholders. Read More
Florida to Roll Out Opioid Addiction Care Network in Seven Counties. Health News Florida reported on August 4, 2022, that Florida will roll out an opioid addiction care network in seven counties beginning with Brevard County, according to Governor Ron DeSantis. The Coordinated Opioid Recovery (CORE) program, which will involve coordinated efforts of public and private organizations, will be led by newly appointed statewide director of opioid recovery Courtney Phillips, MD. Phillips is currently director of behavioral health for the Health Care District of Palm Beach County. The program, which is based on a pilot in Palm Beach County, will be coordinated by the state Department of Health, Department of Children and Families, and the Agency for Health Care Administration. Read More
Georgia
Georgia Proposal to Bypass Healthcare.gov Is Again Rejected by CMS. CQ News reported on August 10, 2022, that the Centers for Medicare & Medicaid Services (CMS) again rejected a plan by Georgia to allow individuals to shop for federally subsidized plans through private insurance websites and agents instead of through Healthcare.gov. After initially rejecting the proposal in April, CMS gave the state until July 28 to submit a corrective action plan. The state instead challenged the initial rejection. The proposal was part of a Section 1332 waiver application previously approved by the Trump administration. Read More
Idaho
Idaho Releases Quality Improvement Organization RFP. The Idaho Division of Purchasing released on August 5, 2022, a request for proposals (RFP) for a quality improvement organization to provide services including utilization management, case management, and external quality reviews for the state Medicaid program. Proposals are due October 7, 2022. Read More
Mississippi
Mississippi Awards MississippiCAN, CHIP Medicaid Managed Care Contracts to 3 Health Plans. The Mississippi Division of Medicaid announced on August 10, 2022, its intent to award contracts for its Mississippi Coordinated Access Network (MississippiCAN) traditional Medicaid program and the state Children’s Health Insurance Program (CHIP) to Centene/Magnolia Health Plan, Molina Healthcare, and TrueCare in partnership with CareSource. UnitedHealthcare and Anthem/Amerigroup Mississippi also submitted proposals. This is the first time the state has sought to jointly administer MississippiCAN and CHIP. The contracts will have an initial four-year term with two one-year renewal options. Read More
Missouri
Missouri Commits to Trimming Medicaid Applications Backlog Under Federal Plan. The Missouri Independent reported on August 9, 2022, Missouri has committed to a federally approved plan to address the state’s backlog of Medicaid applications. As of June, the state had 50,000 pending applications and took an average of 115 days to process an application, up from 106 days in May. The plan gives the state until September 30 to comply with federal standards. Read More
Missouri Medicaid Has Higher Pregnancy-Related Mortality Rate than Private Insurance, Report Finds. The Kansas City Star reported on August 5, 2022, that the pregnancy-related mortality rate for women on Medicaid averaged 34.6 deaths per 100,000 live births from 2017-19, according to the Missouri Department of Health and Senior Services. In contrast, the pregnancy-related mortality rate for women on private insurance averaged 15.1 deaths per 100,000 live births over the same period. Read More
Montana
Montana Loses 10 Percent of Nursing Home Beds in 2022. McKnight’s Long-Term Care News reported on August 4, 2022, that Montana has lost approximately 10 percent of its nursing home beds, driven by facility closures over the past six months. Nursing homes in the state have struggled with workforce shortages and financial losses. Read More
New York
New York Approves Changes to Prior Authorization Requirements for FFS Medicaid Preferred Drug Program. The New York State Department of Health announced on August 10, 2022, that changes to prior authorization requirements for drugs in the fee-for-service (FFS) Medicaid preferred drug program will go into effect on August 11. The decision impacts cholesterol absorption inhibitors, antimigraine agents, movement disorder agents, topical antifungals, dipeptidyl peptidase-4 inhibitors, glucagon-like peptide-1 agonists, antihyperuricemics, and anticholinergic/COPD agents. Additionally, changes to the criteria for name-brand drugs Spravato, Symbicort, and Dulera were also approved. Read More
New York to Host Webinars on Medicaid Pharmacy Carve-Out. The New York State Department of Health announced on August 9, 2022, it will hold a series of webinars on the transition of the Medicaid pharmacy benefit from managed care to fee-for-service. The pharmacy carve-out was originally scheduled to be implemented in April 2021, but was delayed until April 2023. The first webinar will be held on August 16, 2022. Read More
Long-Term Care Overpayments Top $700 Million, Audit Finds. The New York State Comptroller announced on August 5, 2022, that the New York Department of Health made more than $700 million in overpayments for members ineligible for Medicaid managed long-term care (MLTC), according to an audit of claims from 2015 through March 2021. DOH also made $2.8 billion in MLTC premium payments for beneficiaries that only received minimal services. The auditors recommend recovering as much of the overpayments as possible, developing a timely disenrollment process for members who are no longer eligible, and strengthening monitoring of the care provided to MLTC recipients. Read More
North Carolina
North Carolina Providers Experience Medicaid Claims Payment Delays. WRAL reported on August 7, 2022, that North Carolina Medicaid providers are experiencing claims payment delays, with some saying they are owed up to six-figure sums from Medicaid managed care plans. The state, which acknowledged problems, reported that plans had handled 17.2 million medical claims over 12 months, with 14 million paid and 3.2 million denied. Read More
Ohio
Ohio Pharmacists Express Concern Over Single PBM Program. The Ohio Capital Journal reported on August 9, 2022, that Ohio pharmacists are concerned about the adequacy of dispensing fees and transparency surrounding the state’s new single Medicaid pharmacy benefit management (PBM) program, which will take effect on October 1, 2022. Gainwell Technologies was awarded the single PBM contract in 2019. Read More
Oregon
Oregon Has 8,000 Medicaid Applications Past Federal Processing Deadline as of June 2022. The Oregonian reported on August 6, 2022, that Oregon had 8,000 Medicaid applications past the federal processing deadline as of June 2022, down from 12,000 as reported in February. Meanwhile, the families of long-term care applicants who have mistakenly been denied coverage blame deficiencies in the state’s new eligibility system and a lack of staff training. Read More
Texas
Application to Expand Medicaid Postpartum Coverage Is Denied by Federal Regulators. The Texas Tribune reported on August 4, 2022, that federal regulators rejected a Section 1115 waiver application filed by Texas to extend postpartum Medicaid coverage from two to six months. While the Centers for Medicare & Medicaid Services has not commented on the reason for the rejection, some state lawmakers point to language in the waiver application that could be understood to exclude women who have had an abortion. Read More
Texas Releases RFA for FQHC Incubator Program. The Texas Department of State Health Services announced on August 4, 2022, a request for applications (RFA) for the state’s Federally Qualified Health Center (FQHC) Incubator Program, which will distribute $20 million in grants using American Rescue Plan Act funds. FQHCs and FQHC look-alikes can receive up to $50,0000 each to expand existing services. Entities that provide primary care services can receive up to $1 million each to apply to become an FQHC. Applications are due by December 31, 2022. Read More
West Virginia
Medicaid Must Cover Gender-Affirming Care, Federal Judge Rules. The Associated Press reported on August 3, 2022, that West Virginia Medicaid must cover gender-confirming care, according to a ruling from U.S. District Judge Chuck Chambers in a class action lawsuit brought by transgender Medicaid beneficiaries in the state. The ruling said that exclusion of this care from Medicaid violated the Equal Protection clause of the 14th Amendment, the Affordable Care Act, and the Medicaid Act. Read More
National
HHS Awards $90 Million to Community Health Centers to Advance Equity through Improved Data Collection, Reporting. Health IT Analytics reported on August 9, 2022, that the U.S. Department of Health and Human Services (HHS) awarded $90 million to nearly 1,400 community health centers in an effort to advance health equity and improve care through enhanced data collection and reporting. The funding comes from the American Rescue Plan and is awarded through the Health Resources and Services Administration. HHS will also invest nearly $60 million to expand healthcare capacity in rural and tribal communities. Read More
Medicaid Enrollment Would Increase by 3.7 Million if All States Implemented Medicaid Expansion, Report Says. Health Payer Intelligence reported on August 9, 2022, that Medicaid enrollment would increase by 3.7 million if the 12 remaining non-expansion states implemented expansion, according to a Robert Wood Johnson Foundation and Urban Institute report. The finding is based on enrollment data from the U.S. Department of Health and Human Services. Read More
U.S. Senate Passes Legislation Allowing Medicare to Negotiate Drug Prices, Extending Enhanced Exchange Subsidies. Modern Healthcare reported on August 7, 2022, that the U.S. Senate passed legislation to allow Medicare to negotiate drug prices and extend enhanced Exchange subsidies. The Inflation Reduction Act also caps out-of-pocket drug costs for seniors on Medicare to $2,000 annually and to $35 monthly for insulin costs. The legislation now moves to the U.S. House. Read More
CMS Releases Chart Showing PHE Unwinding Flexibilities Granted to States. The Centers for Medicare & Medicaid Services released on August 5, 2022, a chart showing the approved section 1902(e)(14) waiver flexibilities granted to states to support the renewal process and ensure due process protections during the unwinding period following the end of the public health emergency (PHE). The PHE was recently extended through October 2022. Read More
House Committee Advances Bill Requiring Electronic Prior Authorization for Medicare Advantage Plans. Modern Healthcare reported on August 4, 2022, that the U.S. House of Representatives Ways and Means committee advanced a bill that would require Medicare Advantage insurers to establish real-time, electronic prior authorization programs. The definition of “real-time” would be established in a subsequent rule. Insurers would also be required to provide an annual list of things requiring prior authorization, data on denials and approvals, and disclosures on decision-making software they use. Insurers also would provide some of this information to providers, suppliers and beneficiaries. Read More
Industry News
Pine Tree Equity Announces Investment in Premier Physician Support Services. Pine Tree Equity IV announced on August 8, 2022, an investment in Premier Physician Support Services, a primary care medical services organization. Premier oversees 30,000 Medicare and Medicaid patients in 10 Florida counties through a network of 90 physicians. Read More
Health Plan Faces Federal Class Action Lawsuit Over Exchange Plans. Modern Healthcare reported on August 8, 2022, that Centene faces a federal class action lawsuit claiming that the company misled former Medicaid members into enrolling in Exchange plans, which were marketed with inaccurate provider networks, violated federal network adequacy standards, and improperly denied care to patients. Centene denies any wrongdoing.
CVS Is Reportedly Interested in Acquiring Signify Health. The Wall Street Journal reported on August 7, 2022, that CVS Health is interested in submitting a bid to acquire publicly traded Signify Health, which is exploring strategic alternatives. Initial bids are due this week. Signify Health has a market cap of about $6.5 billion. Read More
HCSC to Expand Medicare Advantage Footprint in 2023. FierceHealthcare reported on August 4, 2022, that Health Care Service Corporation (HCSC) will offer Medicare Advantage (MA) plans in 150 additional counties in Illinois, Montana, New Mexico, Oklahoma, and Texas. The expansion, which will focus on rural and underserved areas, will bring HCSC’s total MA footprint to 330 counties. HCSC will also be expanding its benefits to bolster dental, vision, prescription drug coverage, enhanced or alternative benefits, and lower out-of-pocket costs. Read More
Aetna to Offer Exchange Plans in Four Additional States in 2023. Fierce Healthcare reported on August 3, 2022, that CVS Health/Aetna is planning to offer Exchange plans in four additional states, including California, for enrollment effective in 2023. Aetna currently offers Exchange plans in eight states. Read More
Care Advantage Acquires National Home Healthcare. Care Advantage announced on August 2, 2022, that it has completed the acquisition of Virginia-based National Home Healthcare, a provider of Medicare certified, in-home skilled care. Care Advantage is a Searchlight Capital Partners portfolio company. Read More
UnitedHealth/Optum Acquires CareMount Medical. Mid Hudson News reported on July 31, 2022, that UnitedHealthcare’s Optum has acquired CareMount Medical, a New York-based accountable care organization. CareMount chief executive Scott Hayworth, MD, is now president of Optum’s Tri-State region. Read More
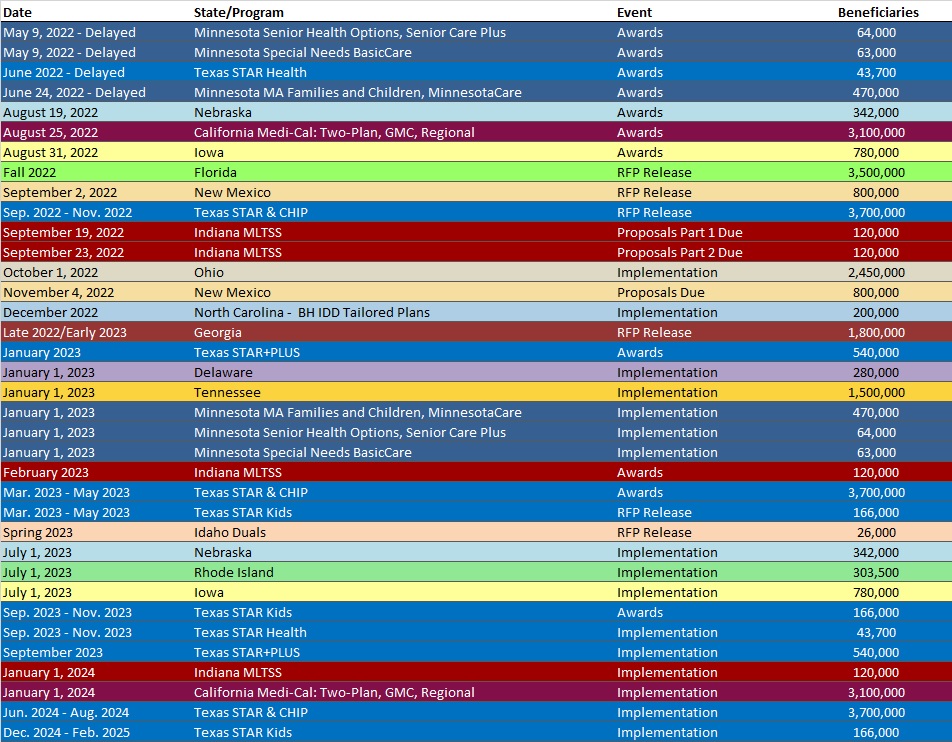
RFP Calendar
HMA News & Events
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Alabama Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Colorado RAE Enrollment is Up 2.8%, Apr-22 Data
- Colorado Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Florida Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Georgia Medicaid Managed Care Enrollment is Up 3.7%, May-22 Data
- Idaho Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Indiana Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Louisiana Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Maryland Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Mississippi Medicaid Managed Care Enrollment is Down 9.6%, May-22 Data
- Nebraska SNP Membership at 13,831, Mar-22 Data
- Puerto Rico Medicaid Managed Care Enrollment is Up 1.7%, Jul-22 Data
- Utah Medicaid Managed Care Enrollment is Up 2.2%, Jan-22 Data
- Utah Medicaid Managed Care Enrollment is Up 16%, 2021 Data
- Virginia SNP Membership at 61,482 Mar-22 Data
Medicaid Financials and Utilization Data:
- MLRs Average 85.8% at Colorado Medicaid RAEs, 2021 Data
- MLRs at Pennsylvania Medicaid MCOs Average 89.2%, 2021 Data
- MLRs at Washington Medicaid MCOs Average 87.1%, 2021 Data
- MLRs at West Virginia Medicaid MCOs Average 78.9%, 2021 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- California Medi-Cal Managed Care RFP: Two-Plan, GMC, and Regional Models, Aug-22
- Idaho Medicaid Quality Improvement Organization RFP, Aug-22
- Mississippi MississippiCAN and CHIP RFQ, Amendments, Scoring, and Award, 2021-22
- Texas FQHC Incubator Program RFA, Jun-22
Medicaid Program Reports, Data and Updates:
- Pennsylvania MLTSS Subcommittee Meeting Materials, 2021-22
- Utah Medicaid External Quality Review Reports, 2018-22
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.
Medicaid RFPs, RFIs, and Contracts:
- California Medi-Cal Managed Care RFP: Two-Plan, GMC, and Regional Models, Aug-22
- Idaho Medicaid Quality Improvement Organization RFP, Aug-22
- Mississippi MississippiCAN and CHIP RFQ, Amendments, Scoring, and Award, 2021-22
- Texas FQHC Incubator Program RFA, Jun-22
Medicaid Program Reports, Data and Updates:
- Pennsylvania MLTSS Subcommittee Meeting Materials, 2021-22
- Utah Medicaid External Quality Review Reports, 2018-22
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.