This week's roundup:
- In Focus: CMS’s 2024 Hospital Inpatient Regulation Proposes to Increase Payments to Hospitals, Support Safety Net Hospitals, and Modify the NTAP Program
- Arkansas Legislature May Hold Special Session on Medicaid Spending
- Florida House Passes Bill to Increase Income Threshold for KidCare Coverage
- Georgia to Recommend Rate Increase for Providers Caring for Individuals with Disabilities
- Illinois Receives Federal Approval for Additional Medicaid Funding in Schools
- Iowa House Passes Bill to Create Medicaid Eligibility Verification System
- Nevada to Review Medicaid HCBS Rate Setting Methodology
- Pennsylvania Releases RFP for a Medicaid, CHIP EQRO
- South Dakota to Implement Medicaid Expansion on July 1
- Wisconsin Releases RFI for Eligibility Determination System
- HHS Projects 6.8 Million Eligible Medicaid Beneficiaries Will Be Disenrolled During Redeterminations
- Biden Administration Encourages States to Apply for Medicaid Reentry 1115 Demonstration for Individuals in Carceral Settings
- Humana to Invest Another $40 Million in Affordable Housing
In Focus
CMS’s 2024 Hospital Inpatient Regulation Proposes to Increase Payments to Hospitals, Support Safety Net Hospitals, and Modify the NTAP Program
This week, our In Focus section reviews the policy changes proposed by the Centers for Medicare & Medicaid Services’ (CMS) on April 10, 2023, for the Fiscal Year (FY) 2024 Medicare Hospital Inpatient Prospective Payment System (IPPS) and Long-Term Acute Care Hospital (LTCH) Proposed Rule (CMS-1785-P). This year’s IPPS Proposed Rule includes several important policy changes that will alter hospital margins and change administrative procedures, beginning as soon as October 1, 2023.
Key provisions of the FY 2024 Hospital IPPS and LTCH Proposed Rule
For FY 2024, CMS proposes to make modifications to several hospital inpatient payment policies. We highlight six proposed policies that are among the most impactful for Medicare beneficiaries, hospitals and health systems, payors, and manufacturers:
- the annual inpatient market basket update,
- hospital wage index adjustments,
- New Technology Add-on Payment (NTAP) program policy changes,
- the agency’s call for input on how to best support Safety Net Hospitals,
- graduate medical education payments at rural emergency hospitals, and
- changes to many cardiovascular-related MS-DRGs.
Stakeholders will have until June 9, 2023, to submit comments to CMS on the contents of this regulation and request for information
1. Market basket update
Proposed Rule: Overall CMS’s Medicare 2024 Hospital Inpatient Proposed Rule will increase payments to acute care hospitals by an estimated $3.3 billion from 2023 to 2024; however, recent trends in economy-wide inflation may alter this estimate by the time the agency releases the Final Rule version of this regulation in August 2023. The primary driver of the estimated $3.3 billion increase in inpatient payments to hospitals is CMS’s proposed 2.8 percent increase in the annual update to inpatient operating payment rates.
HMA/Moran analysis: CMS’s 2.8 percent increase is largely based on an estimate of the rate of increase in the cost of a standard basket of hospital goods, the hospital market basket. For beneficiaries, increasing payment rates will eventually lead to a higher standard Medicare inpatient deductible and increased beneficiary out-of-pocket costs for many other services. For hospitals and health systems, payors, and manufacturers the proposed payment increase (2.8 percent) falls below economy-wide inflation (5-6 percent in recent months) and hospitals are already saying it is insufficient.[1] For this Proposed Rule, data from the third quarter of 2022 was used to calculate the 2.8 percent increase. Importantly, for the FY 2024 Final Rule, CMS will use data through the first quarter of 2023, which we know to include additional growth in economy-wide inflation. As a result, we anticipate the proposed 2.8 percent increase in payment rates may increase slightly by the time rates are finalized later in the year.
2. Hospital Wage Index Adjustments:
Proposed Rule: CMS proposes two wage index policies for FY 2024. First, CMS proposes to continue temporary policies finalized in the FY 2020 IPPS/LTCH PPS final rule to address wage index disparities affecting low-wage index hospitals, which includes many rural hospitals. Second, CMS proposes to include geographically urban hospitals that choose to reclassify into rural wage index areas in the calculation of state-level rural wage index and the calculation of the state-level wage index floor for urban hospitals (referred to as the rural floor policy).
HMA/Moran analysis: The two wage index policies proposed by CMS for FY 2024 will support rural hospitals. The first policy, to continue the low-wage index policy for an additional year beyond the original 4-year plan will allow hospitals with low wage indexes to boost their wage index and their payment rates across all MS-DRGs. Specifically, hospitals with wage indexes below 0.8615 (the 25th percentile across all hospitals) will automatically receive an increase in their wage index by CMS. This policy will bring additional millions of dollars to individual rural hospitals in FY 2024. The second policy, to include the labor data of geographically urban hospitals that choose to reclassify into rural wage index areas within the calculation of the state-level rural wage index and the state-level rural floor will largely benefit rural hospitals. In recent years several large geographically urban hospitals in several markets have chosen to reclassify into rural wage index areas to benefit their Medicare payments. In the past, CMS has not included the labor costs of these hospitals, which tend to have higher than average labor costs in their calculation of the state rural wage index or the rural floor wage index. In making this change, to include the labor costs of the geographically urban hospitals in these calculations, CMS will very likely increase the state-wide rural wage index. This will have the effect of increasing the wage index of many rural hospitals around the country. The overall impact of both proposed wage index policy changes for FY 2024 will be to increase inpatient payment rates to rural hospitals.
3. New technology add-on payments (NTAP):
Proposed Rule: Citing the increased number of applications over the past several years and noting the need for CMS staff to have time to fully review and analyze the applications, CMS proposes two changes to the NTAP application requirements. First, CMS proposes to require all applicants to have a complete and active FDA market authorization request in place at the time of NTAP application submission (if not already FDA approved). In addition, CMS proposes to move the FDA approval deadline from July 1 to May 1, beginning with applications for FY 2025.
HMA/Moran Analysis: CMS’ proposals to change the NTAP application process aim to ameliorate the problem of manufacturers withdrawing applications because they miss the FDA approval deadline. These withdrawals increase CMS’ workload, as the agency reviews some applications multiple times. However, while these proposals provide CMS with more time to review applications, they increase the amount of time some applicants will not receive NTAP payments, depending on the timing of the FDA approval process. The annual NTAP approval cycle and FDA approval deadline create difficulties for manufacturers with products that miss the deadline, which many stakeholders argue creates barriers to access for new technologies. Stakeholders have proposed a variety of potential solutions to these barriers, such as biannual or quarterly NTAP decisions, or extending the conditional approval pathway currently used for certain antibiotic products to all NTAP applications.
4. Safety Net Hospital Request for Information:
Proposed Rule: CMS is seeking public input on the unique challenges faced by safety-net hospitals and the patients they serve, and potential approaches to help safety-net hospitals meet those challenges.
HMA/Moran Analysis: In the 2024 Proposed Rule CMS poses a variety of questions to the public about how safety net hospitals and their patients can be better supported by the Medicare program, both in terms of payment and infrastructure investment. The agency specifically asks stakeholders their opinion on measures that could be used to define safety net hospitals and potentially make differential or additional payments to safety net hospitals. CMS names the safety net index (SNI) developed by the Medicare Payment Advisory Commission (MedPAC) in recent years and the Area Deprivation Index (ADI) developed by the National Institutes for Health (NIH) as the two leading options for defining and potentially reimbursing safety net hospitals. These two methods have several significant differences, including that the SNI is a hospital-level measure based in-part on the volume of cases at a given hospital associated with Medicare beneficiaries that are fully or partially eligible for Medicaid and the ADI is a geographic measure that correlates local socioeconomic factors with medical disparities. HMA has modeled the SNI for hospital stakeholders in the last year and has identified hospitals that would be potential winners and losers if an SNI approach were implemented by CMS.
5. Graduate Medicare Education Training in Rural Emergency Hospitals:
Proposed Rule: CMS proposed to allow Graduate Medical Education (GME) payments for training Rural Emergency Hospitals. Rural Emergency Hospitals are a new provider type established by the Consolidated Appropriations Act, 2021, to address the growing concern over closures of rural hospitals. If finalized, this proposal would allow hospitals converting to REH status and other hospitals newly designated as REHs to receive Medicare GME payments even though they do not have an inpatient facility.
HMA/Moran analysis: If finalized, the proposed policy to allow REHs to offer GME training and to be paid for GME training will enhance access to care in rural areas and will enable hospitals that convert to REHs to expand their capabilities. CMS’s proposal to allow REHs to receive payment based on 100 percent of the reasonable costs for GME training costs allows REHs to operate training programs and to focus new training programs on rural care and outpatient care. This policy, if finalized, will bring additional revenues to hospitals that decide to convert to REHs (thereby relinquishing their inpatient capacity) and will improve access to care for beneficiaries living in rural areas.
6. MS-DRG weights:
Proposed Rule: To set MS-DRG weights for FY 2024 inpatient cases, CMS proposed to use FY 2022 data, which is consistent with pre-pandemic CMS methods. In previous years, CMS had modified its MS-DRG weight calculation to account for high volumes of COVID cases. However, for FY 2024, CMS has returned to its longstanding method of using a single year of data to set MS-DRG weights. In addition, among the various changes CMS has proposed as a part of the 2024 MS-DRG weight setting process CMS has proposed significant changes to many MS-DRGs in the category for diseases and disorders of the circulatory system (Major Diagnostic Category 5).
HMA/Moran analysis: CMS’s return to using a single year of data without COVID modification will be welcomed by many stakeholders, but particularly for those with an interest in short-stay surgical cases. The modifications CMS proposes to make to the MS-DRGs within Major Diagnostic Category 5, which includes numerous cardiovascular MS-DRGs, are likely to be disruptive for many stakeholders initially but over the long term are likely to make CMS coding more consistent with standard clinical practice and per case resource use. For example, CMS is proposing to consolidate five cardiac defibrillator MS-DRGs into three, consolidate three Thrombolysis MS-DRGs into two, and overhaul the family of stenting MS-DRGs. We anticipate that these changes and other proposed by CMS may result in initial coding confusion for hospitals, but that they will slowly adapt throughout 2024.
HMA and The Moran Company work collaboratively to monitor legislative and regulatory developments in the inpatient hospital space and assess the impact of inpatient policy changes on the hospital sector. HMA’s Medicare experts interpret and model inpatient policy proposals and use these analyses to assist clients in developing their strategic plans and comment on proposed regulations. Moran annually replicates the methodologies CMS uses in setting hospital payments and models alternative payment policies to help support its clients’ comments to the rule. Moran also assists clients with modeling for DRG reassignment requests and to support NTAP applications. Typically, these projects run through the summer, to ensure readiness for October deadlines. Finally, many clients find it useful to model payments for different types of cases under different payment scenarios. For example, a client may be interested in how payments for COVID-19 cases may change after the expiration of the Public Health Emergency, and which hospitals will face the biggest payment cuts. Moran is available to help with these and other payment modeling questions—and works on many of these issues in tandem with HMA’s Medicare experts.
For more information or questions about the policies described below, please contact Zach Gaumer, Amy Bassano, Kevin Kirby or Clare Mamerow.
[1] American Hospital Association: CMS issues hospital IPPS proposed rule for FY 2024
HMA Roundup
Arkansas
Arkansas Legislature May Hold Special Session on Medicaid Spending. KUAR reported on April 16, 2023, that the Arkansas Legislature may hold a special session on Medicaid spending, according to Governor Sarah Huckabee Sanders. The session would cover multiple aspects of the program, including work requirements and redeterminations. Read More
Connecticut
Connecticut Legislature Proposes $3 Million to Extend Medicaid to Undocumented Individuals Under 16. The Connecticut News Junkie reported on April 18, 2023, that the Connecticut legislature’s Appropriations Committee released its fiscal 2025 budget proposal, which includes $3 million to extend Medicaid coverage to individuals 15 and under, regardless of immigration status. Currently, coverage is available to individuals 12 and under. Read More
Senate Committee Advances Bills to Allow Medicaid Coverage of Community Health Worker Services. The Connecticut Mirror reported on April 18, 2023, that the Connecticut Senate Human Services Committee passed two bills (Senate Bills 10 and 991) that would allow Medicaid to cover community health worker services. Senate Bill 10 is in appropriations and Senate Bill 991 is scheduled for a full Senate vote. Fifteen states currently reimburse for community health worker services. Read More
Florida
Florida House Passes Bill to Increase Income Threshold for KidCare Coverage. News Service of Florida reported on April 13, 2023, that the Florida House passed a bill (HB 121) that would increase the threshold for subsidized KidCare coverage to 300 percent of the federal poverty level. The Florida Senate Health and Human Services Appropriations Committee recently approved their version of the bill (SB 246). Read More
Florida Senate Committee Approves Bill to Increase Income Threshold for KidCare Coverage. Health News Florida reported on April 13, 2023, that the Florida Senate Health and Human Services Appropriations Committee approved a bill (SB 246) that would increase the threshold for subsidized KidCare coverage to 300 percent of the federal poverty level. KidCare allows families that do not qualify for Medicaid coverage to pay a low premium to insure their children. The current threshold is 200 percent of poverty. The House will take up their own version of the bill (HB 121). Read More
Georgia
Georgia to Recommend Rate Increase for Providers Caring for Individuals with Disabilities. GPB/Georgia Recorder reported on April 14, 2023, that the Georgia Department of Behavioral Health and Developmental Disabilities is expected to recommend a rate increase for providers who care for individuals with disabilities. State lawmakers are currently debating the proposed state budget. Read More
Illinois
Illinois Receives Federal Approval for Additional Medicaid Funding in Schools. The Centers for Medicare & Medicaid Services (CMS) announced on April 18, 2023, approval of the Illinois state plan amendment to increase Medicaid funding for school-based health care services, including mental health services. Schools will receive additional Medicaid funding for covered services for all children with Medicaid, rather than only those with an Individualized Education Program. The approval is part of ongoing efforts by the Biden administration to address the nation’s mental health crisis. Eleven other states – Arizona, California, Colorado, Connecticut, Georgia, Kentucky, Louisiana, Massachusetts, Michigan, Nevada, and North Carolina – have already increased Medicaid funding for school-based health care services. Read More
Iowa
Iowa House Passes Bill to Create Medicaid Eligibility Verification System. Radio Iowa reported on April 13, 2023, that the Iowa House passed Senate File 494, a bill that would direct the Department of Health and Human Services to create a computerized income, asset, and eligibility verification system for public assistance programs, including Medicaid. The bill now goes to Governor Kim Reynolds for her signature. Read More
Louisiana
Louisiana Fails to Enroll, Screen Medicaid Providers for Fifth Consecutive Year, Audit Finds. New Orleans City Business/The Center Square reported on April 17, 2023, that Louisiana for the fifth consecutive year failed to enroll and screen Medicaid providers in managed care networks in fiscal 2022. Instead, managed care plans continued to handle enrollment and screenings for some providers, in violation of federal law. Read More
Louisiana Projects Net Loss of 222,400 Medicaid Beneficiaries During Redeterminations. The Louisiana Illuminator reported on April 17, 2023, that Louisiana expects a net loss of approximately 222,400 Medicaid beneficiaries during the redeterminations process. Previously, the Department of Health said the number could be up to 355,000; however, the state has since noted that more than 100,000 beneficiaries are expected to join the program during the same period. Read More
Nebraska
Nebraska Senate Committee Advances Bill to Increase Hospital Payments for Medicaid Beneficiaries Needing Nursing Care. The Unicameral Update reported on April 17, 2023, that the Nebraska Senate Health and Human Services Committee advanced a bill (LB 227) that would reimburse hospitals at 100 percent of the statewide average nursing facility per diem rate for Medicaid beneficiaries who: 1. are admitted as an inpatient to the hospital; 2. require nursing facility care when discharged; 3. are unable to be transferred to a nursing facility; 4. no longer require acute inpatient care. A previous version of the bill would have raised the rate to 150 percent. Read More
Nevada
Nevada to Review Medicaid HCBS Rate Setting Methodology. Nevada announced on April 18, 2023, that it will review its rate setting methodology for Medicaid home and community-based services (HCBS). The department has contracted with Meyers and Stauffer to conduct the study, which will include a survey of provider costs.
New Hampshire
New Hampshire Mental Health Centers Urge Lawmakers to Increase Funding. The Concord Monitor reported on April 11, 2023, that New Hampshire community mental health centers are urging lawmakers to increase funding. The state House passed a budget that includes $9 million to ensure Medicaid rates will cover mental health services and $11 million to increase wages for providers, but mental health centers say they need up to $28 million.
New York
New York Dispute Over Redirecting Medicaid Funds from Counties Heads to Congress. Spectrum News reported on April 14, 2023, that U.S. Representative Nick Langworthy (R-NY) plans to introduce a bill to block New York from redirecting Medicaid funds from counties. The proposal is in response to New York Governor Kathy Hochul’s proposed budget, which would allow the state to use temporary enhanced federal Medicaid funding that is shared with counties for other purposes. Read More
North Carolina
North Carolina Is Late on 25 Percent of Payments for Emergency Solutions Grant Program, Audit Finds. The Carolina Journal reported on April 18, 2023, that the North Carolina Department of Health and Human Services was late on 25 percent of fiscal 2022 payments to subrecipients of the state’s Emergency Solutions Grant Program, which funds shelters for individuals who are homeless. Payments are supposed to be made within 30 days, according to federal rules. Read More
Pennsylvania
Pennsylvania Releases RFP for a Medicaid, CHIP EQRO. The Pennsylvania Department of Human Services released on April 18, 2023, a request for proposals (RFP) for a Medicaid and Children’s Health Insurance Program (CHIP) External Quality Review Organization (EQRO). IPRO is the current incumbent. In addition to an EQRO, the state is also seeking an organization to perform Healthcare Effectiveness Data and Information Set validation; calculate and report child core, adult core, and older adult core quality measures; develop quality improvement projects; and develop joint physical health, behavioral health, community health, and children’s health projects. Responses are due on June 5. Read More
South Dakota
South Dakota to Implement Medicaid Expansion on July 1. Capitol News Bureau reported on April 18, 2023, that South Dakota is on track to implement Medicaid expansion on July 1. Medicaid expansion was approved in November 2022 through a ballot initiative. An estimated 52,000 individuals will receive coverage. Read More
Virgin Islands
U.S. Virgin Islands Requests Section 1115 Waiver to Continue Medicaid FFS Drug Program. The Centers for Medicare & Medicaid Services announced on April 17, 2023, that the U.S. Virgin Islands submitted a request for a five-year Section 1115 waiver to maintain its current fee-for-service (FFS) Medicaid drug program and to not participate in the Medicaid Drug Rebate program. The federal comment period is open until May 16. Read More
Wisconsin
Wisconsin Releases RFI for Eligibility Determination System. The Wisconsin Department of Health Services released on April 17, 2023, a request for information (RFI) seeking responses for an eligibility determination system for public assistance programs, including Medicaid and the Children’s Health Insurance Program. Responses are due on May 26. Read More
Wisconsin to Complete Review of Humana’s Proposed Purchase of Inclusa Next Week. Wisconsin Health News reported on April 14, 2023, that the Wisconsin Office of the Commissioner of Insurance expects to complete its review of Humana’s proposed purchase of Inclusa, a managed care organization that administers Family Care, the state’s Medicaid long-term care program. The Department of Health Services held a listening session this week on the planned purchase. Read More
Wisconsin Holds ‘Listening Session’ on Planned Acquisition of My Choice WI by Molina Healthcare. Wisconsin Health News reported on April 14, 2023, that the Wisconsin Department of Health Services held a “listening session” this week on the planned purchase of My Choice Wisconsin by Molina Healthcare. Molina has not yet filed the proposed transaction for review with the Office of the Commissioner of Insurance. Read More
National
HHS Projects 6.8 Million Eligible Medicaid Beneficiaries Will Be Disenrolled During Redeterminations. USA Today reported on April 19, 2023, that a projected 6.8 million eligible Medicaid beneficiaries will still lose coverage during eligibility redeterminations, according to the U.S. Department of Health and Human Services (HHS), in part from processing mistakes by states, failure by members to complete paperwork, and inability to reach members who have moved. Arkansas, Arizona, Idaho, New Hampshire, and South Dakota will begin disenrolling beneficiaries this month. Read More
MedPAC Recommends Lowering Payments to Post-acute Care Settings. Modern Healthcare reported on April 18, 2023, that the Medicare Payment Advisory Commission (MedPAC) recommended lower payments to all post-acute care settings except long-term care hospitals. MedPAC also recommended smaller, site-neutral policies that could be phased out if a unified payment system is implemented. MedPAC made the recommendations during its monthly meeting. Read More
CMS to Require Exchange Plan Networks to Include Substance Use Disorder, Mental Health Providers. Modern Healthcare reported on April 17, 2023, that the Centers for Medicare & Medicaid Services (CMS) will require Exchange plan networks to include substance use disorder and mental health providers, according to a recently released final rule. The rule also limits the number of plan offers per insurer to 16. Read More
Biden Administration Encourages States to Apply for Medicaid Reentry 1115 Demonstration for Individuals in Carceral Settings. The Center for Medicaid and CHIP Services released on April 17, 2023, a letter encouraging states to apply for the new Medicaid Reentry Section 1115 Demonstration Opportunity aimed at helping improve care for individuals in carceral settings prior to their release. The demonstration will allow Medicaid to cover services for chronic health conditions, including substance use disorder, for up to 90 days prior to an individual’s release. In January, California was the first state to receive federal approval to provide Medicaid services to individuals in carceral settings. Read More
14 Million Medicaid Beneficiaries Could Lose Dental Coverage During Medicaid Redeterminations, Study Finds. Fierce Healthcare reported on April 17, 2023, that 14 million Medicaid beneficiaries could lose dental coverage following eligibility redeterminations, according to a study from the CareQuest Institute for Oral Health. The study found that even if individuals find new coverage it may not include dental care. Read More
Supreme Court to Hear Arguments in Medicare, Medicaid Pharmacy Overbilling Case. NPR reported on April 17, 2023, that the Supreme Court will hear arguments on whether SuperValu and Safeway pharmacies violated the False Claims Act by knowingly overbilling Medicare and Medicaid up to $200 million. Whistleblowers in the case allege that the pharmacies offered discounts on drugs to rival a large national competitor but continued to bill Medicaid and Medicare higher prices. If the pharmacies are found to have knowingly overstated prices, they may be liable for triple damages. A decision is likely to be made by summer. Read More
Safety-net Hospitals Struggle Financially. Modern Healthcare reported on April 17, 2023, that safety-net hospitals are struggling financially, in part because of a fragmented reimbursement system, rising costs, and aging infrastructure. Read More
Not-for-profit Hospital Revenues to Take Hit Following Medicaid Redeterminations, Analysis Finds. Fierce Healthcare reported on April 14, 2023, that not-for-profit hospital revenues will take a hit following Medicaid redeterminations, according to a Fitch Ratings analysis. The analysis also found that the end of continuous Medicaid enrollment will impact hospital operating costs. Read More
DOJ Requests Partial Stay of Ruling Invalidating Mandatory Coverage of Preventive Care. Fierce Healthcare reported on April 13, 2023, that the Department of Justice (DOJ) filed a request for a partial stay of a federal judge’s ruling that health plans do not have to cover preventive care at no cost to members. Coverage of preventive care at no cost to members is mandated under the Affordable Care Act. Read More
‘Dreamers’ Would be Eligible for Medicaid, Exchanges Under Biden Plan. The Hill reported on April 13, 2023, that the Biden administration announced a plan that would make Deferred Action for Childhood Arrivals (DACA) recipients, aka, “Dreamers,” eligible for Medicaid and Exchange coverage. The expansion would benefit approximately 580,000 individuals. Read More
Medicaid, CHIP Enrollment Increases by 21 Million from 2020-22, CMS Finds. The Centers for Medicare & Medicaid Services (CMS) released on April 13, 2023, the 2023 Medicaid and Children’s Health Insurance Program (CHIP) Beneficiary Profile and Infographic, which found that Medicaid and CHIP enrollment increased by about 21 million to more than 91.7 million from February 2020 to November 2022. The report also found that 15.7 percent of 2020 Medicaid expenditures were for children, 10.6 percent for non-expansion adults, 19.2 percent for expansion adults, 21.6 percent for individuals age 65 and older, and 32.8 percent for individuals with disabilities. Read More
U.S. House Committee Chairman Requests GAO Review of Medicaid Improper Payments. House Committee on Oversight and Accountability Chairman James Comer (R-KY) announced on April 12, 2023, that he is asking the U.S. Government Accountability Office (GAO) to review improper payments in the Medicaid program. He is also asking GAO to review actions the Centers for Medicare & Medicaid Services can take to improve the program’s integrity. Read More
CMS to Publish Final Guidance for Medicare Drug Negotiation Program in July. Reuters reported on April 12, 2023, that the Centers for Medicare & Medicaid Services (CMS) plans to publish final guidance for its Medicare drug price negotiation program in early July. CMS released a draft in March, and public comments will be accepted through April 14. CMS will select the first 10 drugs for negotiation in September, with prices going into effect in 2026. Read More
Industry News
Humana to Invest Another $40 Million in Affordable Housing. Fierce Healthcare reported on April 14, 2023, that Humana will invest another $40 million in affordable housing in 16 states: Arizona, Florida, Georgia, Illinois, Indiana, Kentucky, Louisiana, Michigan, Ohio, Oklahoma, South Carolina, Tennessee, Texas, Virginia, Washington, and Wisconsin. The funding brings Humana’s total investment in affordable housing to $90 million nationwide. Read More
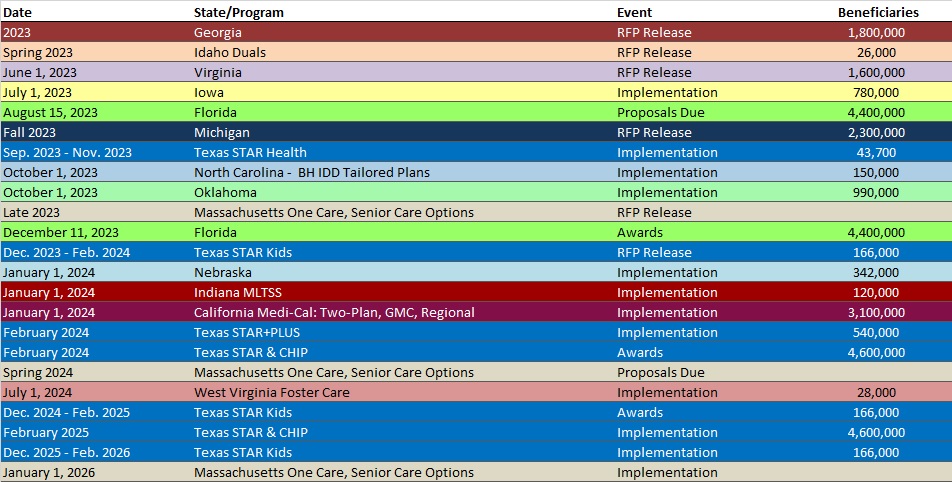
RFP Calendar
Company Announcements
MCG Announcements:
Mary Washington Healthcare Receives Richard L. Doyle Award for Improving Length of Hospital Stay. MCG Health, part of the Hearst Health network and an industry leader in technology-enabled, evidence-based guidance, has named Mary Washington Healthcare (MWHC) a recipient of its 2022 Richard L. Doyle Award for Innovation and Leadership in Healthcare. For their winning initiative, Mary Washington Healthcare, a Virginia-based healthcare system, safely reduced their observed to expected length of hospital stay for patients resulting in 1,600 fewer excess days per month.
HMA News & Events
Wakely, an HMA Company, White Paper:
Summary of Final Rate Notice, Part C, and Part D Bid Review Memo. The Wakely Summary of the CY2024 Final Announcement provides a thorough summary of the final Medicare Advantage (MA) Part C and Part D payment policies for 2024. We cover what has changed since the Advance Notice and provide an independent estimate of the potential revenue impact on MA plans in 2024. We also describe CMS’s responses to comments submitted related to the Advance Notice. These responses provide insight on current CMS positions and possible changes for future years. Read More
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- California Medicaid Managed Care Enrollment is Up 5.9%, Feb-23 Data
- Iowa Medicaid Managed Care Enrollment is Up 2.3%, Mar-23 Data
- Kentucky Medicaid Managed Care Enrollment is Up 1.6%, Mar-23 Data
- Michigan Medicaid Managed Care Enrollment is Flat, Feb-23 Data
- Michigan Dual Demo Enrollment is Down 5.6%, Feb-23 Data
- North Dakota Medicaid Expansion Enrollment is Up 4%, Mar-23 Data
- Oregon Medicaid Managed Care Enrollment is Up 1.4%, Feb-23 Data
- South Carolina Medicaid Managed Care Enrollment is Up 1.1%, Feb-23 Data
- South Carolina Dual Demo Enrollment is Down 7.8%, Feb-23 Data
- Tennessee Medicaid Managed Care Enrollment is Up 1.1%, Feb-23 Data
- Virginia Medicaid Managed Care Enrollment is Up 2.9%, Mar-23 Data
- Virginia Medicaid MLTSS Enrollment is Up 1.1%, Mar-23 Data
- Wisconsin Medicaid Managed Care Enrollment is Up 1.1%, Feb-23 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Ohio Medicaid Non-Emergency Transportation Services for Greene County RFP, Apr-23
- Pennsylvania EQRO RFP, Apr-23
- South Dakota Pre-Admission Screening and Resident Review (PASRR): Level I Reviews and Level II Mental Health Evaluations RFP, Apr-23
- Wisconsin Public Assistance Programs Eligibility and Enrollment System RFI, Apr-23
Medicaid Program Reports, Data, and Updates:
- Illinois Medicaid Annual Reports, 2013-22
- Kansas Medical Care Advisory Committee Meetings, 2019-22
- Louisiana Department of Health Financial Audit, Apr-23
- Massachusetts Health Safety Net Annual Reports, 2015-22
- Mississippi Medicaid Annual Reports, 2013-22
- North Carolina Medicaid Annual Report Charts, 2022
- South Carolina Medicaid Telehealth Report, 2023
- Wisconsin Medicaid HMO Quality Guide, 2023
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.