This week's roundup:
- In Focus: CMS Announces Innovation in Behavioral Health Model
- Connecticut Proposes to Extend Medicaid Services to Incarcerated Individuals Prior to Release
- Florida to Submit Section 1115 Waiver Request to Expand CHIP Eligibility
- Florida Senate Passes Bill to Expand Healthcare Access, Resources
- Idaho House Committee Proposes Bill Setting Requirements on Medicaid Expansion
- Indiana Alters Waivers, Enhances Budget Monitoring to Address Medicaid Budget Shortfall
- Kansas Governor’s Proposed Fiscal 2025 Budget Includes Medicaid Expansion Funds
- Kentucky Senate Advances Bill to Limit Number of Managed Care Organizations
- Michigan Extends Due Date for Medicaid Managed Care Proposals
- New Hampshire Awards Medicaid Managed Care Contracts to Incumbents
- New York MCOs Oppose Proposed Competitive Medicaid Managed Care Procurement Process
- North Carolina Medicaid Expansion Enrollment Surpasses 314,000
- Rhode Island Medicaid State-directed Payments Approved by CMS
- Texas Extends Medicaid Postpartum Coverage to 12 Months
- Washington Updates State Action Plan to Remove Barriers to Health Services
- Medicaid Redetermination Updates: Florida, Georgia, Indiana, Mississippi, New Hampshire, Oklahoma, Vermont
- More Than 21.3 Million Have Selected ACA Marketplace Plans Since Enrollment Period Began
- Combined Medicaid, Medicare Spending on Dual Eligibles was $493.4 Billion in 2021, MACPAC, MedPAC Report Finds
- Centene Names Michael Carson as President, CEO of Medicare Business
In Focus
CMS Announces Innovation in Behavioral Health Model
This week, our In Focus section highlights the Innovation in Behavioral Health (IBH) model, which the Centers for Medicare & Medicaid Services (CMS) announced January 18, 2023. It is the third state-based alternative payment model that the CMS Center for Medicare and Medicaid Innovation (Innovation Center) has released in recent months. HMA wrote about the Transforming Maternal Health (TMaH) Model here and States Advancing All-Payer Health Equity Approaches and Development (AHEAD) Model here.
IBH Model Overview
This model is designed to improve the quality of care and health outcomes for people with moderate to severe behavioral health conditions through person-centered care that integrates physical health, behavioral health, and health-related social needs (HRSN). Its objective is to improve care through healthcare integration, care management, health equity, and health information technology.
CMS will select up to eight state Medicaid agencies for participation in this eight-year model that will begin in fall 2024. Participating states must partner with the agencies that are responsible for mental health and/or substance use disorder treatment to ensure coordination and alignment of policies. Model participants will develop and implement the IBH model in partnership with at least one Medicaid managed care organization or another intermediary as applicable.
Community-based behavioral health organizations and providers in selected states can choose to engage as practice participants in the model. Community-based providers can include safety net providers, community mental health centers, public or private practices, and opioid treatment programs. Practice participants will be responsible for coordinating with other members of the care team to comprehensively address behavioral and physical health needs and HRSN, such as housing, food, and transportation for patients. Practice participants will conduct HRSN screenings, refer patients to specialists and community-based resources, and more. They will be compensated based on the quality of care provided and improved patient outcomes.
Opportunities and Considerations
The model will include three pre-implementation years during which states and practice participants will receive Medicaid and Medicare funding for development and capacity building. Medicare will provide practice participants with a per-beneficiary-per-month payment in pre-implementation years to support health IT, electronic health records (EHR), practice transformation, new workflows, and staffing investment necessary to implement the model. Starting in year four, the Medicaid alternative payment model must be implemented, and Medicare will begin making performance-based payments.
Notably, the announcement materials do not indicate the maximum funding amount selected state Medicaid agencies are eligible to receive in IBH. The cooperative agreement funding for selected states will support implementation preparations, such as statewide health IT infrastructure, supporting practice participants, stakeholder convening, and developing the Medicaid alternative payment model.
What’s Next
The Innovation Center expects to release a Notice of Funding Opportunity (NOFO) in spring 2024. More details on the requirements, including payment methodologies and funding, are expected to be included in the NOFO.
The HMA Behavioral Health and federal policy teams will continue to monitor developments in IBH and analyze the opportunities for states and providers in this model. HMA experts are also assessing the relative opportunities of the IBH model alongside other Innovation Center opportunities and initiatives already underway in states.
The core design elements and objectives of the IBH are illustrative of the issues that HMA’s experts and industry leaders plan to discuss at HMA’s Spring Workshop, The HMA Spring Workshop: Getting Real About Transforming Healthcare Quality and Value.
For more information on the IBH model, contact Amy Bassano, Melissa Mannon, Barry Jacobs, and Jennifer Hodgson.
HMA Roundup
Connecticut
Connecticut Proposes to Extend Medicaid Services to Incarcerated Individuals Prior to Release. CT Insider reported on January 18, 2024, that the Connecticut Department of Social Services has proposed a policy that would allow incarcerated youth exiting the correctional system to be eligible for Medicaid coverage up to 90 days before their release. Incarcerated adults with mental health disorders, substance abuse issues, or certain other health conditions would also be eligible. According to state data, about 85 percent of the 12,000 adults who exit Connecticut jails and prisons each year would qualify. If approved, the policy would cost Connecticut an estimated $8 million the first year of implementation, $8.4 million the second year, and about $9 million the third. Read More
Delaware
Delaware Subcommittee Recommends Discontinuing Highmark Medicare Advantage Plan for State Retirees. Health Payer Specialist reported on January 22, 2024, that the Retiree Healthcare Benefits Advisory Subcommittee in Delaware recommended that the state refrain from automatically enrolling retired state workers in its Medicare Advantage plan run by Highmark. The state has extended coverage for retirees through the existing Highmark Medicfill Medicare Supplement Plan, through June 30, 2024. Read More
Florida
Florida to Submit Section 1115 Waiver Request to Expand CHIP Eligibility. The Florida Agency for Health Care Administration announced on January 23, 2024, that it will submit a request for a new Section 1115 demonstration, titled the “Children’s Health Insurance Program Eligibility Extension,” to extend eligibility for the state’s Children’s Health Insurance Program (CHIP) to children in households with income ranging from 200 percent of the federal poverty level up to 300 percent. Eligibility will come with premium requirements. The five-year waiver has a proposed effective date of April 2024. The public comment period will be open through February 21. Read More
Senate Passes Bill to Expand Healthcare Access, Resources. WMNF reported on January 18, 2024, that the Florida Senate passed a bill to expand healthcare access and resources. The bill will allocate funding towards filling medical residencies, supporting maternal healthcare, and diverting patients in emergency rooms to more appropriate care. Read More
Florida Disenrolls Over 911,000 Medicaid Beneficiaries During Redeterminations Since April. Health News Florida reported on January 19, 2024, that Florida has disenrolled over 911,000 Medicaid beneficiaries during redeterminations from April through December 2023, including about 420,000 children. Of those disenrolled, 56 percent were due to procedural reasons, and about 11 percent of kids were moved to the state’s Children Health Insurance Program. Read More
Georgia
DHS Faces Workplace Shortages During Medicaid Redeterminations. The Atlanta Journal Constitution reported on January 17, 2024, that the Georgia Department of Human Services (DHS) hired more than 1,200 workers and counting to support Medicaid redetermination processing but continues to face struggles with caseloads. DHS is also in the process of administratively rolling out Medicaid expansion. Read More
Georgia Disenrolls 503,547 Medicaid Beneficiaries During Redeterminations in 2023. The Georgia Department of Community Health reported that it has disenrolled 503,547 Medicaid beneficiaries during 2023 redeterminations from May through December. Of those disenrolled, 430,155 were due to procedural reasons. The state has renewed coverage for 337,426 Medicaid beneficiaries, and still has more than 1.5 million pending eligibility cases. Read More
Idaho
House Committee Proposes Bill Setting Requirements on Medicaid Expansion. The Idaho Capital Sun reported on January 22, 2024, that the Idaho House Health and Welfare Committee introduced legislation that would impose requirements on the Medicaid expansion program. HB 419 would make the expansion contingent on the federal government continuing to provide 90 percent of the funding, set a cap on Medicaid expansion enrollment, enforce an improper payment rate of five percent or less, limit eligibility assumptions, and implement work requirements for at 20 hours per week. The requirements would need to be met by July 1, 2025, or the program would be repealed. The bill has been referred to the Judiciary, Rules and Administration Committee. Read More
Indiana
Indiana Proposed Aged, Disabled Waiver Cuts Face Opposition. The Indianapolis Star reported on January 23, 2024, that Indiana is facing opposition from making cuts to several Aged & Disabled waivers to address the state’s $1 billion budget shortfall, including cessation of compensation to family or spouses acting as caregivers. More than 10,000 individuals signed an online petition to prevent the cuts. Although the state has not indicated how many families will be impacted by the cut, those impacted must find a caregiver outside of the family or transition to a new service model, which pays a fixed daily stipend to a caregiver, by July 1. The potential waiver changes will be open to public comment through February 16. Read More
Indiana Alters Waivers, Enhances Budget Monitoring to Address Medicaid Budget Shortfall. The Indiana Family & Social Services Administration (FSSA) announced on January 17, 2024, that it will make changes to various draft waivers and enhance Medicaid budget monitoring to address the projected need for additional Medicaid funding in the state. Specifically, the Aged & Disabled, PathWays, Traumatic Brain Injury, Community Integration and Habilitation, and Health & Wellness waivers will all undergo a second round of public comment regarding new changes and FSSA will further examine the Medicaid program to predict potential financial impacts of programmatic changes. Read More
Indiana Disenrolls 28,142 Medicaid Beneficiaries During December Redeterminations. State Affairs reported on January 19, 2024, that Indiana disenrolled 28,142 Medicaid beneficiaries, including 23,703 for procedural reasons and 4,439 due to eligibility during December eligibility redeterminations. The state has disenrolled a total of more than 330,000 Medicaid enrollees since redeterminations began in April. Read More
Kansas
Kansas Governor’s Proposed Fiscal 2025 Budget Includes Medicaid Expansion Funds. Kansas Governor Laura Kelly released on January 11, 2024, the fiscal 2025 executive budget proposal, which lays out $5.1 billion for all major health or social service federal programs, including Medicaid, Temporary Assistance to Needy Families, and foster care. The funding includes $715 million to expand Medicaid beginning January 1, 2025. Medicaid expansion would be budget neutral and would expand Medicaid services to an additional 150,000 individuals. Read More
Kentucky
Kentucky Senate Advances Bill to Limit Number of Managed Care Organizations. Beech Tree News reported on January 16, 2024, that the Kentucky Senate passed a bill that would reduce the number of managed care organizations (MCOs) contracted by the state Medicaid agency to a maximum of three. The reduction of contracted MCOs is expected to alleviate administrative challenges faced by health care providers, specifically in rural areas. The bill now heads to a House vote. If enacted, the legislation is slated to take effect on January 1, 2025. Read More
Maine
Maine Names Bobbi Johnson Director of OCFS, Announces Other Structural Changes. The Maine Department of Health and Human Services (DHHS) announced on January 18, 2024, that Bobbi Johnson has been appointed permanent Director of the Office of Child and Family Services (OCFS). Other structural changes aimed at improving outcomes for children and families include reorganization within DHHS behavioral health services and a transition of Children’s Behavioral Health Services from OCFS to the DHHS Office of Behavioral Health. A rapid management audit of the state’s Child Welfare Division will also produce recommendations by the end of March 2024. Read More
Michigan
Michigan Extends Due Date for Medicaid Managed Care Proposals. Health Payer Specialist reported on January 19, 2024, that Michigan is extending the due date for proposals on its Medicaid Managed Care Comprehensive Health Care Program contracts to January 26, 2024. Implementation is still anticipated for October 1, 2024. Read More
Mississippi
Mississippi Disenrolls 1,190 Medicaid Beneficiaries During December Redeterminations. The Mississippi Division of Medicaid reported that it has disenrolled 1,190 Medicaid beneficiaries during December redeterminations, 546 of which were due to procedural reasons. The state renewed coverage for 13,895 beneficiaries in December. The state has 42,531 pending eligibility cases for individuals whose renewal was due in December.
New Hampshire
New Hampshire Awards Medicaid Managed Care Contracts to Incumbents. At the New Hampshire Governor and Executive Council’s January 10, 2024 meeting, the state’s Department of Health and Human Services announced it was awarding contracts to incumbents AmeriHealth Caritas, Boston Medical Center/WellSense, and Centene/New Hampshire Healthy Families for the state’s Medicaid Care Management managed care program, which covers 190,000 individuals. Contracts run from September 1, 2024, through August 31, 2029. Read More
New Hampshire Disenrolls 1,406 Medicaid Beneficiaries During December Redeterminations. The New Hampshire Department of Health and Human Services reported that it has disenrolled 1,406 Medicaid beneficiaries during December redeterminations. Of those, 1,119 were due to procedural reasons. The state renewed coverage for 10,273 Medicaid beneficiaries. The state has 595 pending eligibility cases for individuals whose renewal was due in December.
New York
New York MCOs Oppose Proposed Competitive Medicaid Managed Care Procurement Process. Health Payer Specialist reported on January 24, 2024, that New York’s Medicaid managed care organizations (MCOs) are challenging a budget proposal from New York Governor Kathy Hochul that would implement a competitive bidding process for Medicaid managed care contracts, limit the number of plans permitted to operate per geographic region, and eliminate the one percent administrative rate increase given to plans. The proposal, intended to streamline the Medicaid program, could eliminate dozens of plans. Plans, represented by the New York Health Plan Association, have argued that the elimination of plans will complicate efforts to implement the state’s new Medicaid Section 1115 waiver aimed at improving health equity and will reduce access to care for beneficiaries. Read More
Legislators Challenge Governor’s Plans to Reduce Medicaid Spending. Spectrum News 1 reported on January 23, 2024, that New York legislators are pushing back against Governor Kathy Hochul’s intention to reduce Medicaid spending, which has grown by 40 percent over the last three years to $35 billion. Legislators argue instead of cutting the program, the state should restructure long-term managed care and provide coverage for undocumented individuals. A final spending plan is due April 1. Read More
North Carolina
North Carolina Medicaid Expansion Enrollment Surpasses 314,000. The Winston-Salem Journal reported on January 23, 2024, that enrollment in the North Carolina Medicaid expansion program was at 314,101 as of January 12. Of the enrolled individuals, 278,00 were automatically enrolled by the state and 36,101 signed up themselves. The program, which launched in December, is expected to cover about 600,000 members. The state enrollment dashboard shows 73,447 are ages 50 or older, and 100,767 are ages 19 to 29. Read More
Oregon
Oregon Health Authority Director Recuses From Pending SCAN Acquisition of CareOregon. Willamette Week reported on January 23, 2024, that the director of the Oregon Health Authority (OHA), Sejal Hathi, has opted to recuse herself from decision-making regarding the proposed California-based SCAN Group’s acquisition of CareOregon, which is currently under review by OHA. The Medicaid Advisory Committee had urged OHA to disapprove the transaction. Hathi previously notified the Oregon Government Ethics Commission about a potential conflict of interest regarding her personal friendship with the chief executive of SCAN Group, although it was concluded that since she had no financial stake in the merger her recusal was not required by law. Read More
Rhode Island
Rhode Island Medicaid State-directed Payments Approved by CMS. Rhode Island Governor Dan McKee and the Rhode Island Executive Office of Health & Human Services announced on January 18, 2024, that the Centers for Medicare & Medicaid Services (CMS) approved state-directed payments (SDPs) through contracted Medicaid managed care organizations for the current fiscal year. The payments will generate more than $100 million in Medicaid funding for Rhode Island hospitals to improve access and quality. Governor McKee will include SDPs in the fiscal 2025 budget, which will also require CMS approval. Read More
Texas
Texas Extends Medicaid Postpartum Coverage to 12 Months. The Office of the Texas Governor Greg Abbott announced on January 17, 2023, that the Centers for Medicare & Medicaid Services has approved Texas’ state plan amendment to extend postpartum Medicaid coverage from 60 days to one year, effective March 1, 2024. Read More
Vermont
Vermont Disenrolls 27,984 Since Redeterminations Began in April. The Mountain Times reported on January 17, 2024, that Vermont disenrolled 27,984 Medicaid beneficiaries between April and December, including 20,152 for procedural reasons and 7,832 due to eligibility. According to the Department of Vermont Health Access, 1,788 Medicaid beneficiaries were disenrolled during December redeterminations, including 1,429 for procedural reasons and 359 due to ineligibility. Read More
Washington
Washington Updates State Action Plan to Remove Barriers to Health Services. The Washington State Healthcare Authority announced on January 18, 2024, that the state has published an annual update to its Washington State Action Plan for Removing Barriers to Health and Human Services. The plan seeks to remove barriers to accessing benefits, allowing members to apply for multiple programs and immediately know their eligibility status. The update also enables the state to share information across organizations and proactively offer members other benefits they may qualify for. Read More
National
More Than 21.3 Million Have Selected ACA Marketplace Plans Since Enrollment Period Began. The Centers for Medicare & Medicaid Services announced on January 24, 2024, that more than 21.3 million people have selected an Affordable Care Act (ACA) Health Insurance Marketplace plan since the opening of the 2024 Marketplace open enrollment period on November 1. Approximately 5 million people are new Marketplace consumers for 2024, and about 16.3 million are returning consumers. Open enrollment is still open in four states and District of Columbia through January 31. Read More
Combined Medicaid, Medicare Spending on Dual Eligibles was $493.4 Billion in 2021, MACPAC, MedPAC Report Finds. The Medicaid and CHIP Payment and Access Commission (MACPAC) reported in January 22, 2024, that combined Medicare-Medicaid spending on dual eligibles was $493.4 billion in 2021. The information appeared in 2024 Data Book: Beneficiaries Dually Eligible for Medicare and Medicaid jointly produced annually by MACPAC and the Medicare Payment Advisory Commission (MedPAC). The data book also includes information on dual eligible demographics, utilization, and trends. Read More
U.S. Senate Finance Committee Investigates Medicare Advantage Marketing. Fierce Healthcare reported January 23, 2024, that the United States Senate Finance Committee, led by Committee Chair Ron Wyden (D-OR), has sent letters to five insurance brokers requesting information with respect to Medicare Advantage sales tactics. This includes how the the third party marketing organizations deploy insurance agents, generate leads, and market specific plans to seniors. The organizations under investigation include eHealth, GoHealth, Agent Pipeline, SelectQuote and TRANZACT. Read More
Legislators Introduce Bill to Implement Oversight of Opioid Settlements Totaling $50 Billion. KFF Health News reported on January 22, 2024, that Representatives Marcy Kaptur (D-Ohio) and Ashley Hinson (R-Iowa) introduced a bill, known as the Opioid Settlement Accountability Act, which would ban the federal government from utilizing state opioid settlement funds beginning in 2026 and require states to use the funding solely to address the opioid crisis. The settlement funding, which comes from drugmakers and pharmaceutical entities, totals more than $50 billion to be paid over the course of 18 years. The bill has been referred to the House Committee on Energy and Commerce. Read More
KFF Outlines State Fiscal Conditions, State Medicaid Program Impacts for Fiscal 2025 Budgets. KFF released on January 22, 2024, an issue brief outlining trends in state fiscal conditions during the current year, and how that is expected to affect state Medicaid programs, state budgets, and individuals in fiscal 2025. The report predicts that states may focus more heavily on cost containment initiatives to lower Medicaid spending due to fewer financial resources, including the expiration of the enhanced federal Medicaid funds. Read More
Medicaid Disenrollments Surpass 15 Million Following Redeterminations. KFF released on January 16, 2024, an update showing that more than 15 million Medicaid enrollees have been disenrolled since eligibility redeterminations resumed earlier this year. Disenrollment rates varied widely between states, ranging from 61 percent in Texas to 13 percent in Oregon and Maine. Approximately 71 percent of people have been disenrolled for procedural reasons across all states with available data. HMA also provides a dynamic 50-state projection model that can be used to anticipate Medicaid enrollment trends, for more information please contact Matt Powers. Read More
MACPAC Announces Topics for January 25-26 Meeting. On January 19, 2024, the Medicaid and CHIP Payment and Access Commission (MACPAC) announced the topics for its next meeting scheduled for January 25-26. Topics for discussion include Medicaid self-reported disability data collection, policy options for enhancing the transparency of Medicaid financing, Medicaid coverage of physician-administered drugs, and denials and appeals in Medicaid managed care. Read More
Industry News
Centene Names Michael Carson as President, CEO of Medicare Business. Centene Corporation announced on January 22, 2024, that Michael Carson has been named president and chief executive of its Medicare business, Wellcare. Carson previously served as chief executive of value-based primary and multi-specialty care start-up CareAbout. Read More
Cigna CFO Brian Evanko to Serve as President, CEO of Health Insurance Division. Modern Healthcare reported on January 17, 2023, that Brian Evanko will serve as president and chief executive of Cigna Healthcare, the company’s health insurance division. Evanko is currently chief financial officer of Cigna Group. Eric Palmer, president and chief executive of the company’s Evernorth Health Services division, will move to the executive vice president for enterprise strategy for Cigna Group. Evanko and Palmer will assume their new roles on February 5, 2024. Read More
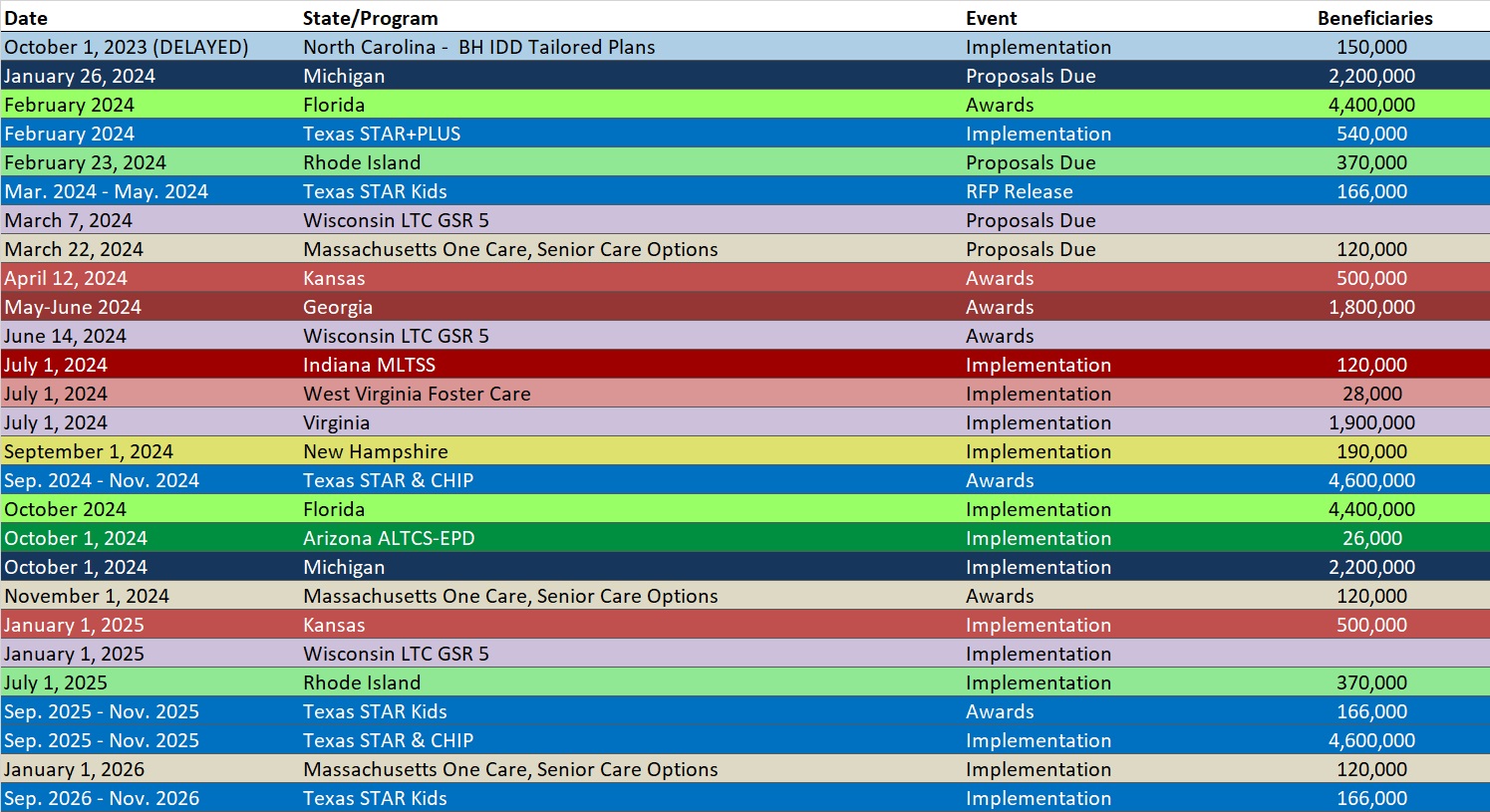
RFP Calendar
Company Announcements
MCG Press Release:
UC San Diego Health Wins 2023 Doyle Award: UC San Diego Health was recognized with the Richard L. Doyle Award for Innovation and Leadership in Healthcare for reducing unnecessary hospital readmissions, achieving $1 million in annual cost savings, and earning a three-year accreditation for Population Health Management from NCQA. Read More
HMA News & Events
Wakely, an HMA Company White Paper: