This week's roundup:
- In Focus: HMA Perspectives on the 2022 Federal Policy Landscape
- Arizona Medicaid Director to Step Down at the End of 2022
- Colorado Appoints Adela Flores-Brennan as Medicaid Director
- Centene Names Bill Wilson CEO of Delaware Medicaid Plan
- Kansas Begins Distributing $51 Million in Bonuses for Direct Care Workers at Medicaid HCBS Providers
- Massachusetts Receives Federal Approval to Extend MassHealth 1115 Waiver Through 2027
- Nebraska Awards Medicaid Managed Care Contracts to 3 Health Plans
- Nevada Releases Electronic Visit Verification System RFP
- Oregon 1115 Waiver Renewal Is Approved by Federal Regulators
- Texas Report Recommends Transitioning Medicaid-Only Services into Managed Care for Dual Eligibles
- Virginia Medicaid Provider Sets Up Neighborhood Clinics to Expand Access to Preventive Health Care
- OIG Calls For Increased Oversight of Medicaid Plan MLR Reporting
- DentaQuest Commits $275,000 to Initiative Connecting Children to Dental Care
In Focus
HMA Perspectives on the 2022 Federal Policy Landscape
This week, our In Focus section looks at the current federal policy landscape and trends and the legislative outlook for the remainder of 2022 and beyond. Experts from HMA continue to monitor developments in this area and provide additional updates as more information becomes available.
Legislative Branch
To date in 2022, Congress passed multiple comprehensive bills, including the Inflation Reduction Act (IRA), which was signed by President Biden on August 16, 2022. The IRA extends Exchange plan premium tax subsidies through 2025, institutes an out-of-pocket drug spending cap for Medicare beneficiaries, expands Medicare, Medicaid, and CHIP coverage protections for certain vaccines, allows Medicare to negotiate drug prices, and implements a penalty payment in the Medicare program for prescription drug prices that rise faster than the rate of inflation.
Going forward, stakeholders have an extensive list of immediate Medicare payment issues for Congress to tackle while lawmakers continue to consider fundamental reforms to the program. Priorities include mitigating Medicare payment reductions scheduled for 2023; providing relief to address inflationary cost pressures; extending the 5 percent bonus for physicians participating in Advanced Alternative Payment Models (APMs), which expires at the end of 2022 for Accountable Care Organizations (ACOs); and permanently expanding telehealth access and payment policies after the federal COVID-19 public health emergency (PHE) declaration expires. Many stakeholder groups are also urging the Senate to act on the House-approved legislation, Improving Seniors Timely Access to Care Act (H.R. 3173), to reform Medicare Advantage prior authorization policies.
Congress did not include major Medicaid proposals in the Inflation Reduction Act. Medicaid stakeholders want Congress to revisit certain Medicaid policies in one of the remaining legislative vehicles this year. Significant proposals of interest include closing the Medicaid coverage gap in non-expansion states, enhanced coverage for justice involved populations, and expanding support for home and community-based services (HCBS). States and some stakeholders have also sought more certainty in the timing and guardrails for ending the COVID-19 Public Health Emergency (PHE) policy that links enhanced federal Medicaid funding with the requirement for continuous Medicaid coverage.
Congressional leaders and key influencers are laying the groundwork for 2023 legislative efforts. Congress is likely to defer action on most major legislative issues until after the November mid-terms, including finalizing federal fiscal year 2023 funding for most departments. A change in control of either or both chambers of Congress will likely lead to greater scrutiny of the Biden Administration’s health care policies and actions, which have largely gone untested by this Congress.
Executive Branch
Executive orders have been a major source in driving federal workstreams in 2022. Following enactment of several major bills, implementation responsibilities have shifted to the Executive Branch and stakeholders will have multiple opportunities to further shape and support new programs, regulatory and policy updates, and funding opportunities. Executive orders passed include:
- Advancing Racial Equity and Support for Underserved Communities, January 21, 2021
- Promoting Competition in the American Economy, July 9, 2021
- Improving the Customer Experience, December 13, 2021
- Access to Affordable, Quality Health Coverage, April 5, 2022
- Equality for LGBTQI Individuals, June 15, 2022
- Protecting Access to Reproductive Healthcare Services, July 8, 2022
The Administration will continue to address COVID-19 emergency needs while stepping up efforts to support states, health plans, providers and other stakeholders as they prepare for the post-COVID environment. The current PHE declaration expires October 13, 2022, but since HHS has not signaled that it plans to end the PHE in October, another extension is likely until January 11, 2023. The next advance notification about the end of the PHE would be Nov. 12, 2022. Once the PHE declaration expires, numerous Medicare and Medicaid, TANF, and SNAP flexibilities will end, including Medicaid’s continuous coverage requirement and certain telehealth flexibilities, among others. Additional federal agency guidance is expected to support post-PHE transitions.
The Centers for Medicare & Medicaid Services (CMS) plans to advance new policy direction across several service and delivery areas, including strengthening long-term services and support and innovations via Section 1115 demonstration programs. CMS is expected to approve transformational 1115 proposals in additional states. Several state proposals focus, in part, on building capacity among local and regional entities and community-based organizations to address social drivers of health. Many state proposals are also strengthening behavioral health delivery systems and seek to meet enrollees’ urgent behavioral health needs. Additionally will want to monitor CMS’ regulatory efforts to align and strengthen managed care and fee-for-service (FFS) access and network adequacy policies as well as updates to the agency’s in lieu of services policy in managed care programs.
The Administration is also expected to accelerate work on its top policy priorities and regulatory agenda in advance of the next Presidential election, and this will require ongoing engagement among health care stakeholders.
For additional information on these and other policies, please contact Andrea Maresca, Amy Bassano, Zach Gaumer, Jon Kromm, or Kevin Kirby.
HMA Roundup
Arizona
Medicaid Director to Step Down at the End of 2022. The Arizona Health Care Cost Containment System (AHCCCS) announced on September 22, 2022, that Jami Snyder will be leaving her position at the end of 2022, after serving as Medicaid director since 2019. Previously, Snyder was AHCCCS deputy director and also served a stint as director of the Texas Medicaid program. Read More
Colorado
Colorado Appoints Adela Flores-Brennan as Medicaid Director. State of Reform reported on September 23, 2022, that the Colorado Department of Health Care Policy and Financing appointed Adela Flores-Brennan as state Medicaid director. Flores-Brennan was previously executive director of the Colorado Consumer Health Initiative. Read More
Delaware
Centene Names Bill Wilson CEO of Delaware Medicaid Plan. Health Payer Specialist reported on September 26, 2022, that Centene/Delaware First Health named Bill Wilson plan president and chief executive. Wilson previously served as chief financial officer of Managed Health Services, a Centene subsidiary in Indiana. Centene/Delaware First Health was awarded a statewide Medicaid managed care contract in July 2022. Read More
Kansas
Kansas Begins Distributing $51 Million in Bonuses for Direct Care Workers at Medicaid HCBS Providers. KZRG reported on September 27, 2022, that Kansas has begun distributing $51 million in bonuses for direct care workers at Medicaid home and community-based services (HCBS) providers. The Kansas Department for Aging and Disability Services will distribute the funds as one-time payments to the state’s three Medicaid managed care organizations, who will then disburse the funds to providers. Providers must pay their direct support staff no later than March 30, 2023. The state received 213 applications for bonuses to 28,574 direct support workers. Read More
Maryland
Maryland Seeks to Improve Certified Community Behavioral Health Center Model Quality, Reporting. State of Reform reported on September 16, 2022, that Maryland is seeking to enhance the state’s Certified Community Behavioral Health Center (CCBHC) model by improving quality and reporting measures, according to a meeting of the University of Maryland Institute for Innovation and Implementation. Stakeholders outlined how data from CCBHCs can be used to identify health disparities, improve health outcomes, and address mental health and substance use disorder. Maryland currently has five federally-funded CCBHCs that serve Anne Arundel, Baltimore, Baltimore City, Montgomery, and Prince George’s counties. Read More
Massachusetts
Massachusetts Receives Federal Approval to Extend MassHealth 1115 Waiver Through 2027. The Massachusetts Executive Office of Health and Human Services announced on September 28, 2022, that the state received federal approval to extend the MassHealth Section 1115 waiver through 2027. The renewal covers existing Medicaid programs as well as allowing new programs, including the Hospital Quality and Equity Initiative, increased coverage of social determinants of health, and a value-based primary care payment pilot. Read More
Minnesota
Minnesota Awards Grants Targeting Community Engagement, Employment for Individuals With Disabilities. The Minnesota Department of Human Services (DHS) announced on September 26, 2022, that 10 provider organizations will receive $2.9 million in grants aimed at helping individuals with disabilities access employment opportunities and better engage with their local communities. Funds will be provided over two years. Read More
Missouri
Lawmakers to Restart Debate on Extending Postpartum Medicaid Coverage to 12 Months. St. Louis Post-Dispatch reported on September 26, 2022, that Missouri lawmakers plan to restart debate on whether to extend postpartum Medicaid coverage from 60 days to 12 months. In May, a bill to extend coverage stalled in the state Senate after passing in the House. Twenty-three states and the District of Columbia have extended coverage, with eight additional states waiting on federal approval. Read More
Nebraska
Nebraska Awards Medicaid Managed Care Contracts to 3 Health Plans. The Nebraska Department of Health and Human Services announced on September 23, 2022, its intent to award contracts for the Heritage Health Medicaid managed care program to incumbents UnitedHealthcare and Centene/Nebraska Total Care, as well as new entrant Molina. Medica Community Health Plan and incumbent Elevance Health/Healthy Blue also submitted proposals. Implementation is scheduled for January 1, 2024, and the contract length is five years with two one-year renewal options. Read More
Nebraska Sees 14.5 Percent Decrease in Uninsured Rate Since Implementing Medicaid Expansion. The Omaha World-Hearld reported on September 25, 2022, that the uninsured rate in Nebraska fell 14.5 percent since the state implemented Medicaid expansion in October 2020. The state has also seen reductions in charity care and personal bankruptcy filings. Read More
Nevada
Nevada Releases Electronic Visit Verification System RFP. The Nevada Department of Administration released on September 19, 2022, a request for proposals (RFP) for an electronic visit verification system and services for personal care and home health care services. Responses are due on November 10, and awards are anticipated on December 16. The contract will begin after Board of Examiners approval on April 11, 2023, and will run for four years. Read More
Nevada Projects Public Option Plan Will Generate $1 Billion in Savings Over 10 Years. The Nevada Department of Health and Human Services (DHHS) announced on September 23, 2022, that the state’s public option plan could generate $300 to $400 billion in savings over five years and nearly $1 billion over 10, according to a DHHS webinar. The public option, which will be available on the Exchange in 2026, is expected to reduce premium costs and increase competition. Read More
New York
Partners Health Plan Selects DentaQuest to Administer Dental Benefits to Individuals With I/DD in New York. DentaQuest announced on September 22, 2022, that it was selected by Partners Health Plan to administer dental benefits and specialized services for individuals with intellectual and/or developmental disabilities (I/DD) in New York. DentaQuest serves 63 percent of Medicaid beneficiaries in the state. In the coming months, Partners Health Plan will pilot teledentistry and mobile dentistry programs through its partnership with DentaQuest to increase access to oral health care for members. Read More
North Carolina
CMS Approves Extension of Postpartum Medicaid Coverage in North Carolina, Dental Coverage for Pregnant, Postpartum Women Nationwide. The Centers for Medicare & Medicaid Services (CMS) announced on September 22, 2022, approval for North Carolina to extend Medicaid postpartum coverage to 12 months, covering an additional 28,000 people in the state. CMS also announced that all 50 states and the District of Columbia will offer Medicaid dental coverage to pregnant women as well as postpartum for at least 60 days. Read More
Oklahoma
Oklahoma Leads Nation In Medicaid Application Processing Speed, CMS Finds. KFOR reported on September 21, 2022, that Oklahoma has the fastest Medicaid application processing time in the U.S., according to a report from the Centers for Medicare & Medicaid Services (CMS). In the first three months of 2022, the state processed all applications – nearly 59,000 – in less than 24 hours. Read More
Oregon
Oregon 1115 Waiver Renewal Is Approved by Federal Regulators. Oregon Health Authority announced on September 28, 2022, that federal regulators approved the renewal of the state’s Section 1115 Medicaid waiver demonstration, effective October 1, 2022, through September 30, 2027. The renewal covers existing programs and also addresses initiatives related to continuous eligibility, coverage expansion, and social determinants of health (SDOH). Read More
Oregon Will Submit State Plan Amendment to Increase Funding for I/DD Services Through New Rate Model. The Oregon Department of Human Services announced on September 22, 2022, that the Oregon Health Authority (OHA) will submit a state plan amendment (SPA) aimed at increasing funding for intellectual and developmental disabilities (I/DD) services. The SPA, which would revise the state’s 1915(k) waiver with a new rate model, would be effective at least through the end of the public health emergency (PHE). OHA is looking to extend the model past the PHE with a permanent state plan submission. Public comments will be accepted through October 7. Read More
Tennessee
Tennessee Predicts 300,000 Medicaid Enrollees Could Lose Coverage When PHE is Lifted. The Nashville Post reported on September 26, 2022, that about 300,000 Tennesseans are expected to lose Medicaid coverage when the COVID-19 public health emergency (PHE) is lifted, according the Division of TennCare. The state is trying to mitigate wrongful coverage losses by urging individuals update their contact information and by readying a four-part plan involving planning, educating, renewing, and transitioning beneficiaries. TennCare also released an RFI in August 2022 to partner with an advocacy organization that can assist enrollees in completing and returning applications. Read More
Texas
Texas Report Recommends Transitioning Medicaid-Only Services into Managed Care for Dual Eligibles. Texas Health and Human Services Commission (HHSC) published on September 23, 2022, a report to the state Legislature recommending transitioning Medicaid-only services, services not covered by Medicare, for dual eligibles from fee-for-service into Medicaid managed care to resolve some of the administrative burden for providers. The transition would require amending current Medicaid managed care contracts, Medicare-Medicaid coordination rules, and the Medicaid state plan. Additionally, HHSC recommends requiring cost-sharing for Medicaid-only services for dual eligibles. The state will submit an addendum no later than October 1 that will provide the findings from a cost-effectiveness analysis study and recommendations. Read More
Virginia
Virginia Medicaid Provider Sets Up Neighborhood Clinics to Expand Access to Preventive Health Care. Healthcare Finance reported on September 26, 2022, that Virginia health system Sentara Healthcare has set up two neighborhood clinics and a mobile care van to provide preventive care for Medicaid beneficiaries and the uninsured. The clinics also allow Medicaid eligible-individuals to sign up for coverage. Sentara is hoping to save on uncompensated care costs by reducing the number of uninsured patients showing up for care. In 2021, Sentara provided $254 million in uncompensated care. Read More
West Virignia
West Virginia Reaches $147.5 Million Opioid Settlement with Walmart, CVS Pharmacy. NBC News/The Associated Press reported on September 21, 2022, that Walmart and CVS Pharmacy settled with the state of West Virginia for $65 million and $82.5 million, respectively, for the over supply of opioids. The state had also settled with Rite Aid for $30 million. Read More
National
OIG Calls For Increased Oversight of Medicaid Plan MLR Reporting. Health Payer Intelligence reported on September 27, 2022, that federal regulators should strengthen oversight of medical loss ratio (MLR) reporting by Medicaid managed care plans, according to a report from the U.S. Office of the Inspector General (OIG). The report found that 49 percent of MLR reports submitted to states by Medicaid plans were missing at least one element required for MLR calculations. Read More
Temporary Extension of Enhanced Payment Programs for Rural Hospitals Advances in Senate. Modern Healthcare reported on September 27, 2022, that the Senate advanced a spending bill that includes extensions of the Medicare Dependent Hospital (MDH) and the Low-Volume Hospital (LVH) programs through December 17. MDH boosts payments to rural hospitals with patient populations comprised of at least 60 percent Medicaid beneficiaries. LVH provides enhanced payments to hospitals with fewer than 3,800 discharges and located more than 15 miles from the nearest inpatient hospital. Read More
Improper Medicare Payments to Acute Care Hospitals Decline, OIG Audit Finds. Fierce Healthcare reported on September 26, 2022, a decline in improper Medicare Part B payment to acute care hospitals in the period from September 2016 through December 2021, according to an audit by the U.S. Office of the Inspector General (OIG). The reduction came after the Centers for Medicare & Medicaid Services (CMS) modified the way in which overpayments are identified. Overpayments fell to $39.3 million, compared to $51.6 million in the period from January 2013 through August 2016. Read More
CMS Expands Publicly Available Information on Medicare-Certified Nursing Home Ownership. The Centers for Medicare & Medicaid Services (CMS) announced on September 26, 2022, that additional information on the ownership of all Medicare-certified nursing homes has been made public in an effort to improve transparency, safety and quality, and accountability. The expanded information will allow stakeholders to identify common owners of nursing homes across locations. Read More
CMS Releases Implementation Guide for Medicaid Health Home State Plan Amendments. The Centers for Medicare & Medicaid Services (CMS) released on September 26, 2022, a state plan amendment (SPA) template and implementation guide for the Medicaid health home state plan option, which provides enhanced federal funding for new models aimed at coordinating medical, behavioral health, and long-term services and supports for children with chronic conditions. Read More
CMS Awards Contract to Digital Services Firm Fearless. The Daily Record reported on September 23, 2022, that the Centers for Medicare & Medicaid Services (CMS) awarded Baltimore-based digital services firm Fearless a MACPRO system contract to help streamline Medicaid and the Children’s Health Insurance Program (CHIP). The contract will run for four years and is worth $67 million. Read More
CMS Seeks Further Comments on Enhanced Medicaid Matching Fund Requirements. Bloomberg Law reported on September 23, 2022, that the Centers for Medicare & Medicaid Services (CMS) is reopening the public comment period for 30 days effective September 27 concerning requirements that states must follow to secure temporary enhanced federal Medicaid matching funds. Requirements include continuous eligibility for Medicaid beneficiaries. Read More
U.S. Senator to Target ‘Ghost’ Provider Networks. Fierce Healthcare reported on September 23, 2022, that U.S. Senator Ron Wyden (D-OR) is developing legislation that would hold health plans accountable for “ghost networks,” in which providers are listed in a plan’s network but do not actually offer care. A report released by the Government Accountability Office in March found that ghost networks were leading to barriers in accessing mental health services. Wyden, who chairs the Senate Finance Committee, is also drafting legislation to tackle the mental health workforce shortage. Read More
Providers Urge CMS to Change Proposed Reimbursement Policy for Physicians, Non-Physicians. Modern Healthcare reported on September 22, 2022, that more than 40 healthcare trade organizations are asking the Centers for Medicare & Medicaid Services (CMS) to re-examine a policy under which time spent with a patient would determine whether a physician or non-physician could bill for the visit when both see a patient, according to comment letters submitted to CMS. The proposed 2023 Medicare Physician Fee Schedule delays implementation of the policy until 2024 from January 2023. Providers fear the policy would result in pay cuts for facilities and urge CMS to create an alternative. Read More
OIG Reports Rise in Medicaid Capitated Payments for Individuals Enrolled in Two States. Health Leaders Media reported on September 21, 2022, a 60 percent increase in capitated payments made by states to Medicaid managed care plans for individuals enrolled in two states, according to a report from the Office of the Inspector General. The increase in improper payments was for the 12 months through August 2020. The report recommends that the Centers for Medicare & Medicaid Services monitor concurrent Medicaid enrollments. Read More
Black, Latina, Asian Women Have Higher Rates of Pregnancy Risk Factors than White Women, Study Finds. Fierce Healthcare reported on September 21, 2022, that pregnancy related complications have risen eight percent since 2018, with Black, Latina, and Asian women more likely than white women to experience complications, according to a report by the Blue Cross Blue Shield Association. The report is based on the Centers for Disease Control and Prevention’s Severe Maternal Morbidity measure. Read More
RWJF, NASHP Recognize Six States for Medicaid Innovations. Healthcare Innovation reported on September 21, 2022, that Arizona, California, Kentucky, Minnesota, North Carolina, and West Virginia were recognized by the Robert Wood Johnson Foundation (RWJF) and the National Academy for State Health Policy (NASHP) for Medicaid innovations in the following categories, respectively: Initiatives to Address Social Determinants of Health, Promising or Emerging Initiatives, Enrollment Innovations, Addressing Health Disparities, Improving Access to Care, and Care Coordination Initiatives for Vulnerable Populations. Read More
Industry News
DentaQuest Commits $275,000 to Initiative Connecting Children to Dental Care. DentaQuest announced on September 27, 2022, that it has committed $275,000 to the launch of TeamSmile Dental Home Project, which will connect children across the country with free, comprehensive dental care, including preventive and restorative treatments. The program is in partnership with dental advocacy group TeamSmile. Read More.
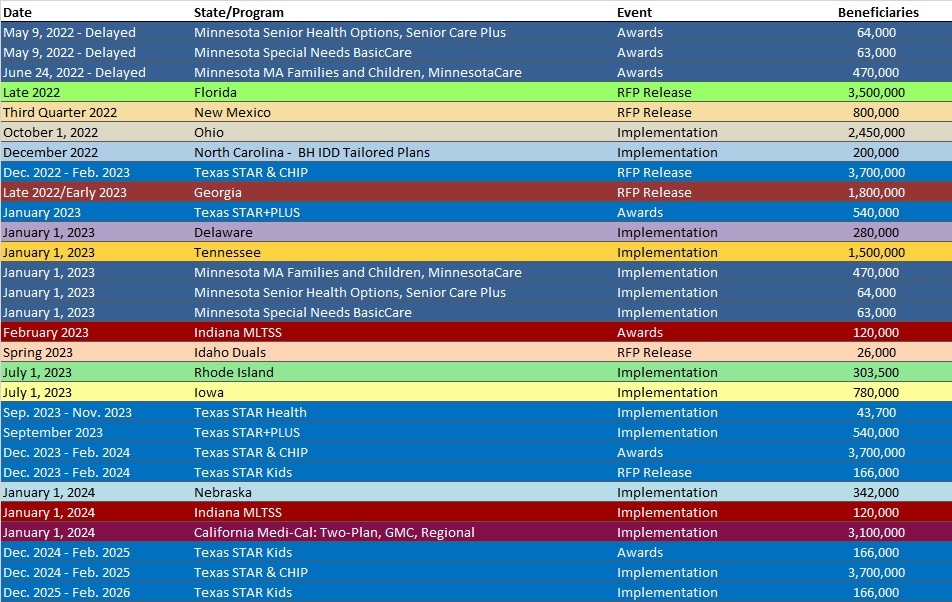
RFP Calendar
HMA News & Events
HMA WELCOMES
Mary Walter, Managing Director, Quality and Accreditation – Salt Lake City, UT
Mary Walter is an accomplished executive leader with more than 30 years of experience in healthcare including extensive work in managed care insurance the past 25 years, quality and oversight of every aspect of health plan operations. She is deeply entrenched in the commercial, Medicare, Medicaid and Marketplace quality space that includes strategy and execution in quality compliance, interventions, population health, HEDIS, Stars, risk adjustment, value-based care and pay for performance, risk management, accreditation, delegation oversight, vendor management, geographical expansion and more.
Mary has worked managing state Medicaid relationships, both commercial and government business, meeting employer group, CMS and state quality regulations, including various accreditation requirements. In addition, she has led health plan quality operations and developed key partnerships to create and execute high quality programs and projects. She has partnered with multi-faceted provider groups including integrated delivery, fee-for-service, and capitated network models as well as accountable care organizations, management services organizations and independent practice associations to carry out upside/downside risk value-based care and pay for performance programs to improve the quality of customer care outcomes.
Before joining HMA, Mary founded and served as president of Healthcare & Integration Solutions, LLC. (HCIS), where she provided her expertise on quality measures including state Medicaid audits, Stars and HEDIS performance, patient safety, and quality compliance. She also supplied insight on strengthening fiscal operations in areas including marketing and sales, budgeting, product and market expansion, and key performance indicators.
Mary has also served as vice president of clinical quality of U.S. Medical with Cigna Medicare and has held several quality leadership roles with the top payers including Coventry, Aetna (now CVS Health), UnitedHealthcare, Anthem, Kaiser Permanente, and Molina Healthcare.
In those positions and experience, she led strategy, execution, and growth of the clinical quality teams, where she elevated population health management strategy and quality compliance oversight. Her leadership resulted in a CMS All Star nomination by passing the CMS audits for organization determinations, appeals and grievances, special needs plan model of care, and supported first-tier, downstream and related clinical entities. In addition, she supported her leadership team to fully pass HEDIS, risk management and NCQA audits with top scores year over year. She also received top regional and national awards for the TeenScreen Depression and Suicide Prevention Program at Kaiser Permanente.
Mary earned a Bachelor of Science degree in exercise physiology, and a minor in health at Iowa State University. In addition, she is a registered nurse, earning a three-year diploma, practical nursing degree at Iowa Methodist School of Nursing in Des Moines. She also holds a certification in process improvement/LEAN six sigma as an Improvement Advisor from KP National Process Improvement Institute.
Jennifer Bridgeforth, Senior Consultant – Columbus, OH
Jennifer Bridgeforth is a dedicated executive with more than 17 years of experience in the healthcare industry. She is a subject matter expert in claims and billing; coding and payment integrity; fraud, waste, and abuse; risk and compliance; physician and facility compensation; and managed care operations.
She has expert knowledge of Medicare, Medicaid, TRICARE, clinical pharmacy, hospice and home health, behavioral health and substance use disorder, medication-assisted treatment and the opioid public health emergency (PHE), health equity and community strategies, and rural health. Her work experience spans various types of healthcare providers, health plans, and consulting.
Prior to joining HMA, Jennifer was director of Health Plan Administration for American Health Plans. In this role, she managed the day-to-day health plan payer functions for an Institutional Special Needs Plan and an Institutional Equivalent Special Needs Plan responsible for thousands of members, focusing on internal operational functions, oversight of partner third-party administrators, and other vendor services. She also oversaw multiple operational departments and vendors to ensure the health plan’s performance remained consistent with Centers for Medicare & Medicaid Services (CMS) regulatory requirements.
Jennifer previously worked as a healthcare consultant. She managed a team of consultants and client staff, completed risk and program assessments to ensure providers met Office of Inspector General (OIG) guidelines for effective compliance programs, and served as an interim C-suite member for healthcare organizations as needed, including the role of chief compliance officer. Earlier in her career, she worked as a project manager, business analyst and project coordinator, and as a fraud investigator and benefit integrity analyst for CMS.
She earned a Master of Business Administration, Healthcare Administration, from South University and a Bachelor of Arts, Healthcare Administration, from Ashford University. Jennifer has a Pharmacy Technician Certification from the Pharmacy Technician Certification Board, a Professional Coder Certification from the American Academy of Professional Coders, and a Professional Medical Auditor Certification from the American Academy of Professional Coders.
Currently, Jennifer is a doctoral student at Franklin University in Columbus, Ohio. Due to her passion and extensive knowledge related to behavioral health and the current opioid PHE, her tentative dissertation topic is “Parental Opioid Abuse and Its Impact on Children.”
Sarah Chughtai, Senior Consultant – Washington, DC
An experienced public health professional, Sarah Chughtai has served local health departments at the city and county level. She most recently worked for the National Association of County and City Health Officials (NACCHO).
While at NACCHO she led the management, development and implementation of a federally-funded public health portfolio. This included writing grant proposals, development of programmatic reports, short and long-term strategic planning, budget development, meeting facilitation, liaising with informatics professionals at the local, state, and federal level, and building partnerships between public health and healthcare.
Sarah has led several projects including improving local health department informatics capacity, death certification and mortality reporting in the U.S. Virgin Islands, syndromic surveillance technical assistance, and opioid surveillance support for medical examiners and coroners. Activities for the projects have included development of syndromic surveillance technical assistance models and tools; local health department implementation of FHIR based solutions, managing the design, implementation, and analysis of a national survey. She also managed national committees, such as the ePublic Health Informatics Workgroup and Informatics Champion Initiative, to provide input on policy at the local, state, and federal level on emerging issues in the field.
Sarah’s experience working at a national public health association has allowed her to serve as a subject matter expert in informatics and engage in cross-cutting work with other areas of public health. Sarah received a Master of Arts degree in Public Policy from Claremont Graduate University (CGU) in 2013.
Andrew Rudebusch, Senior Actuarial Consultant – Phoenix, AZ
Andrew Rudebusch is a seasoned actuarial consultant with more than eight years of experience in Medicaid capitation rate setting and managed care project leadership.
He is experienced in the creation of data visualization tools and performance metrics, data analysis, risk adjustment, and risk mitigation design and monitoring. He is a deft project manager with experience training and developing internal actuarial and analytics teams. A skilled communicator, Andrew fosters strong client relationships and has successfully led numerous stakeholder presentations.
Prior to joining HMA, Andrew served as a principal and project leader at Mercer. There, he developed managed care capitation rates for California’s Medicaid program, managed projects to create and maintain actuarial models, and worked closely with clients to identify and build solutions to actuarial problems.
Andrew has introduced and reviewed metrics to monitor encounter data completeness and quality, monitored claim cost and utilization trends by service and population, and has experience reviewing and performing efficiency adjustment analyses for pharmacy, professional, and emergency services.
He earned his Bachelor of Science degree in mathematics from Northern Arizona University.
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Hawaii Medicaid Managed Care Enrollment is Up 0.6%, Feb-22 Data
- Hawaii Medicaid Managed Care Enrollment is Up 1.2%, Mar-22 Data
- Hawaii Medicaid Managed Care Enrollment is Up 2%, Apr-22 Data
- Hawaii Medicaid Managed Care Enrollment is Up 2.3%, May-22 Data
- Indiana Medicaid Managed Care Enrollment Is Up 4.9%, May-22 Data
- Ohio Medicaid Managed Care Enrollment is Up 0.9%, Apr-22 Data
- Pennsylvania Medicaid Managed Care Enrollment is Up 3.5%, Jun-22 Data
- Tennessee Medicaid Managed Care Enrollment is Up 2.9%, Jun-22 Data
- Washington Medicaid Managed Care Enrollment is Up 2.6%, Jun-22 Data
- West Virginia Medicaid Managed Care Enrollment is Up 2.5%, Jun-22 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- California T-MSIS Standard Operating Procedures Testing Services RFO, Sep-22
- Florida Medicaid Managed Care Monthly Base Capitation Rates, Sep-22
- Nebraska Heritage Health Medicaid Managed Care RFP, Awards, Scoring, and Proposals, Sep-22
- Nevada Electronic Visit Verification System RFP, Sep-22
- Tennessee Medicaid Renewal Advocacy Services RFI, Aug-22
Medicaid Program Reports, Data, and Updates:
- Florida Medicaid Health Information Technology IAPD, 2011-21
- Florida Medicaid Managed Care Monthly Base Capitation Rates, Sep-22
- Florida Medicaid Managed Care Rate Certifications and Related Documents, SFY 2022-23
- Louisiana CHIP Annual Reports, SFY 2010-22
- Oregon HCBS State Plan Rate Change Public Notice, Sep-22
- Pennsylvania Managed Care External Quality Review Reports, 2021
- Texas Dually Eligible Individuals Enrolled in Medicaid Managed Care Report, Sep-22
- Utah HITECH Implementation Advanced Planning Document, Sep-21
- Wyoming Medicaid HITECH Implementation Advance Planning Document, 2014-2022
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.