This week's roundup:
- In Focus: Should You Put the PHE’s Medicaid Unwinding at the Top of Your To-Do List?
- Alabama Doubles Covered Physician Visits for Medicaid Enrollees Receiving Cancer Treatment
- California Medi-Cal Procurement Protests Continue
- California Releases Third-Party Monitoring RFI
- Delaware Names First Director of Value-Based Healthcare Delivery
- Illinois YouthCare Fails to Deliver Basic Medical Services to Foster Children, Investigation Finds
- Medicaid Expansion News: Kansas, North Carolina
- Elevance Files Appeal After Its Protest of Nebraska Medicaid Managed Care Awards is Denied
- Maryland Declines to Pursue Higher Damages Against Medicaid Behavioral Health ASO
- Ohio Delays Implementation of New Medicaid Managed Care Contracts to February 2023
- Oklahoma Re-releases Medicaid Managed Care RFP
- Wisconsin Releases External Quality Review, Quality Improvement Services RFP
- CMS Targets Gaps in Health Equity Data, To Gradually Release Equity Scores
- Sanford Health, Fairview Health Services Agree to Merge
The next HMA Weekly Roundup will be November 30, 2022.
In Focus
Should You Put the PHE’s Medicaid Unwinding at the Top of Your To-Do List?
While the current federal COVID-19 Public Health Emergency (PHE) declaration could be in place through the winter months, HMA’s team of experts see many reasons to put the PHE’s Medicaid unwinding planning at the top of your list now.
Without an extension, the PHE declaration will expire on January 11, 2023. U.S. Department of Health and Human Services (HHS) officials pledged to provide 60-days’ notice before ending the PHE. As a result, since HHS did not announce an extension by November 12, we can assume that HHS Secretary Xavier Becerra will extend the PHE beyond January.
However, congressional leaders are again considering proposals that would impact the PHE’s Medicaid policies. Such a change could advance during the lame duck session of Congress. For a variety of reasons, lawmakers could seek a statutory change that would de-link Medicaid’s continuous enrollment requirement, the 6.2 percentage point increase in the federal Medicaid match, and other Medicaid maintenance of effort policies from the PHE declaration. Congress could set a specific date for ending these Medicaid policies. Doing so would provide more certainty for planning for the end of the continuous Medicaid enrollment policy and its downstream implications for health insurance programs.
What can Medicaid agencies, health plans, providers and other stakeholders do now?
The transition from Medicaid’s continuous enrollment requirement to normal eligibility operations involves a myriad of policy decisions and operational changes that will impact enrollees. In turn, the end of Medicaid’s continuous coverage policy will also have great bearing on the business and operational strategies of managed care plans, providers and other stakeholders participating in the Medicaid and Marketplace programs.
HMA’s experts are working with state agencies, health plans, hospitals and health systems, and other stakeholders to identify options and workable solutions to prepare for these major changes. This work touches policy, organizational workstreams, systems, and payment. There are issues specific to Medicaid as well as the intersection with Marketplace, the Supplemental Nutrition Program (SNAP), and other public programs.
Combining our collective on-the-ground experience in states with our federal policy insights, experts from across the HMA family of companies list below themes and immediate actions stakeholders can consider. These action steps are focused on ensuring states, managed care plans, providers and other stakeholders are prepared to immediately respond to the end of the Medicaid continuous enrollment policy and work with individuals to provide information and other support they may need to stay enrolled in a coverage program.
- Monitor and prepare for federal activities, particularly during the lame duck session of Congress and into 2023. Healthcare policies are likely to feature prominently in Congress’ lame duck session in November and December. Decoupling the Medicaid continuous enrollment and enhanced Federal Medical Assistance Percentage (FMAP) policies from the PHE is one issue under consideration. Any statutory changes to these policies may also include new requirements for the unwinding process. Stakeholders will want to closely monitor these discussions.If Congress sets a statutory end date for the PHE’s Medicaid eligibility policies, this will provide the certainty needed for states to finalize PHE unwinding action plans with target dates for resuming normal eligibility operations. Notably, this may also drive conversations during states’ 2023 legislative sessions.Consider the impact to your state and your organization – and any decisions you’ll be faced with – if the enhanced FMAP is decoupled from the PHE. For example, if your state had the option to maintain continuous eligibility without the enhanced FMAP, would it do so? States and stakeholders will want to revisit their Medicaid unwinding plans, consider options for meeting any new requirements, and update existing plans accordingly. Also, stakeholders can offer to serve as a resource to your state Medicaid agency and/or Congressional delegation regarding lame duck legislative proposals pertaining to Medicaid and the PHE.
- Stay informed about state-specific landscapes. With statewide elections largely decided and expectations for a PHE end date sometime in the first part of 2023, now is the time for stakeholders to revisit when and how to engage with state Medicaid and other state agencies to support Medicaid eligibility unwinding plans. Stakeholders will want to solidify strategies and timing for engaging with states as unwinding plans are further solidified and eventually implemented.Stakeholders can also monitor changes to states’ eligibility and enrollment rules – including initiatives designed to simplify eligibility rules, enhance eligibility and enrollment systems, and adjust managed care rate setting policies, among others. Many states are utilizing the temporary federal Medicaid flexibilities to alleviate the significant eligibility unwinding workload. Federal agencies also continue to regularly publish new information for states and stakeholders to consider. Some states are implementing policies designed to improve the transition from Medicaid to Marketplace. Understanding the implications of such policies will help stakeholders anticipate how ending Medicaid’s continuous coverage requirement will directly affect them.
- Refresh strategies and messaging for outreach and assistance. While the PHE end date remains in flux, state plans for ending the Medicaid continuous coverage policy are still evolving. States are refining their beneficiary communication plans and may be developing updated guidance for stakeholders. Health plans, providers, and other stakeholders should align their messaging and outreach work accordingly and continue to build partnerships in communities across the state.However, outreach alone will not be enough to reach all Medicaid enrollees. Many will need assistance in understanding and complying with changes that come with the end of the continuous enrollment policy. For example, stakeholder-provided redetermination assistance will be key to minimizing the number of enrollees who lose coverage for failure to complete the redetermination process and state requirements for stakeholder assistance will vary state by state.
- Update projected impact of enrollee transitions between Medicaid and Marketplace programs. For states and stakeholders, especially health plans, it is time to update projections about 2023 Medicaid and Marketplace enrollment. This may also require new analysis and strategies to address the changing population acuity and resulting impact on capitation revenue. For healthcare providers, health systems, and other healthcare facilities, the end of the Medicaid continuous enrollment policy is expected to drive significant changes in payer mix, and it could reduce revenue as well as impact qualifications for special payment programs, the 340B program, among others. Understanding these dynamics can help with budgeting and implementation of specific patient outreach and support strategies.
- Develop strategies to translate experiences from Medicaid to Marketplace. Medicaid agencies, managed care plans, and providers have gained valuable insights about the needs of individuals who have remained continuously enrolled in Medicaid during the COVID-19 PHE. This is particularly true for Medicaid enrollees diagnosed with a mental illness, substance use disorder, or both. Medicaid providers and health plans have gained valuable insight on effective clinical care models, whole person care, partnerships with community-based organizations and reimbursement strategies that can better meet the needs of complex populations. Providers and plans can utilize these experiences to better support the millions of individuals who are expected to become eligible for Marketplace coverage after Medicaid’s continuous enrollment policy ends.
The HMA team continues to monitor the dynamic state and federal policy landscapes, including state planning documents and new federal guidance and informational tools. We have the ability to support stakeholders to prepare for the end of PHE and to support state and communities by modeling projected enrollment and payer mix changes across health coverage categories. Stakeholders should be using this time to address gaps in their plans for PHE unwinding and continue to identify and evaluate new options that may emerge to support beneficiaries in retaining health coverage.
For further questions please contact HMA Principals Jane Longo and Andrea Maresca, and Leavitt Partners Principal Bill Snyder.
HMA Roundup
Alabama
Alabama Doubles Number of Covered Physician Visits for Medicaid Enrollees Receiving Cancer Treatment. AL.com reported on November 14, 2022, that the Alabama Medicaid Agency will more than double the number of annual covered physician’s office visits from 14 to 32 for Medicaid enrollees receiving cancer treatment, effective January 1, 2023. The change applies to individuals receiving cancer treatment during the calendar year. Read More
Arkansas
Arkansas Governor Proposes $25 Million Increase in Fiscal 2025 Medicaid Budget. The Arkansas Democrat-Gazette reported on November 11, 2022, that Arkansas Governor Asa Hutchinson proposed increasing the state’s fiscal 2025 Medicaid budget by $25 million to $1.42 billion. Hutchinson did not propose a fiscal 2024 increase, noting that the state plans to draw on its more than $600 million Medicaid trust fund. The state expects the majority of the trust fund to be drawn down during the next biennium. Sarah Huckabee Sanders will be replacing Governor Hutchinson in 2023. Read More
California
California Medi-Cal Procurement Protests Continue. Health Payer Specialist reported on November 14, 2022, that Centene/Health Net alleged in a protest that Molina Healthcare engaged in disingenuous conduct during the California Medi-Cal Medicaid procurement by avoiding disclosure of all civil actions it was a party to. The protest was filed with the California Department of Health Care Services. Molina responded that it met the requirements of the request for proposals. Read More
California Releases Third-Party Monitoring RFI. The California Department of Health Care Services released on November 9, 2022, a request for information (RFI) on the development of a conflict avoidance plan (CAP) should the state’s Medi-Cal Rx contractor Magellan Medicaid Administration (MMA) be acquired by Prime Therapeutics. The RFI is also seeking information on monitoring an existing CAP put in place after Centene acquired MMA. Read More
Delaware
Delaware Names First Director of Value-Based Healthcare Delivery. Becker’s Payer Issues reported on November 9, 2022, that Delaware named Cristine Vogel as its first director of value-based healthcare delivery. Previously, Vogel served as the director of population health initiatives for Nuvance Health. Read More
Illinois
Illinois YouthCare Program Fails to Deliver Basic Medical Services to Current, Former Foster Children, Investigation Finds. The Chicago Sun Times reported on November 11, 2022, that the Illinois YouthCare program, which provides health care coverage to current and former foster children, has not delivered basic medical services, according to an investigation from the Illinois Answers Project. Centene is the health plan contracted to serve the state’s foster children. The YouthCare program serves approximately 36,700 individuals. Read More
Kansas
Kansas Governor to Prioritize Medicaid Expansion in Second Term. KWCH reported on November 14, 2022, that recently reelected Kansas Governor Laura Kelly, a Democrat, will make Medicaid expansion a priority in her second term. Expansion, which would cover approximately 150,000 individuals in the state, faces opposition from the Republican-controlled legislature. Read More
Maryland
Maryland Declines to Pursue Higher Damages Against Medicaid Behavioral Health ASO. The Daily Record reported on November 15, 2022, that Maryland health department officials declined to pursue $21 million in damages for non-performance against behavioral health administrative services only (ASO) contractor Optum Maryland. Instead, the state withheld $6 million in payments, fearing that more severe penalties might result in litigation and cause Optum to walk away from its contract. Optum Maryland handles Medicaid claims payments for about 260,000 individuals receiving mental health or substance use disorder treatments. Optum Maryland was awarded the five-year contract in 2019. Read More
Nebraska
Elevance Files Appeal After Its Protest of Nebraska Medicaid Managed Care Awards is Denied. Health Payer Specialist reported on November 11, 2022, that incumbent Elevance/Healthy Blue has filed an appeal with the Nebraska Department of Health and Human Services after failing to win a contract in the state’s recent Medicaid managed care award. Elevance’s original protest of the award was denied in October 2022. Read More
New Hampshire
New Hampshire Delegation Urges CMS to Protect Medicare Beneficiaries From Predatory Marketing Tactics. The New Hampshire Congressional delegation, on November 14, 2022, urged federal regulators to protect the state’s Medicare beneficiaries from aggressive and potentially predatory Medicare Advantage marketing tactics. The letter to the Centers for Medicare & Medicaid (CMS), which calls for proper disclosure of the type of coverage option a member is choosing, was signed by U.S. Senator Jeanne Shaheen (D-NH) and others in the delegation. Read More
North Carolina
North Carolina Legislative Leaders Further Delay Medicaid Expansion Talks to 2023. The Associated Press reported on November 9, 2022, that North Carolina legislative leaders are further delaying Medicaid expansion talks until 2023. Previously, the state House and Senate each passed separate versions of expansion legislation but could not agree on a single bill. Read More
Ohio
Ohio Delays Implementation of New Medicaid Managed Care Contracts to February 2023. The Ohio Department of Medicaid announced on November 15, 2022, that the implementation of new Medicaid managed care contracts will be delayed until February 1, 2023. Contracts were originally expected to be implemented on July 1, 2022, and then first delayed to October 2022 at the earliest. The state will also implement a new electronic data interchange in February 2023 as part of the state’s Next Generation Medicaid managed care program. A single pharmacy benefit manager was also implemented in October 2022. Read More
Oklahoma
Oklahoma Re-releases Medicaid Managed Care RFP. The Oklahoma Health Care Authority released on November 10, 2022, a request for proposals (RFP) to transition its Medicaid program to managed care, including medical, behavioral, and pharmacy. Governor Kevin Stitt signed legislation to transition the program, called SoonerSelect, to managed care in May 2022. Previously, the Oklahoma Supreme Court struck down the state’s planned transition to Medicaid managed care last year. At least three entities, including Medicaid managed care plans and provider-led entities like accountable care organizations, would be awarded contracts. Responses are due on February 8, 2023, and contract implementation is scheduled for October 1, 2023. The contract is expected to run through June 30, 2024, with five, one-year options. Read More
Texas
Texas Seeks Input on Transition of Medicaid, CHIP Vendor Drug Program to Managed Care. The Texas Health and Human Services Commission announced on November 9, 2022, that it is seeking public input on contract requirements for transitioning the state’s Medicaid vendor drug program to managed care. The program oversees outpatient drug benefits for Medicaid fee-for-service, Medicaid managed care, and the Children’s Health Insurance Program (CHIP), including management of a single program-wide formulary, preferred drug list, and prior authorization. Management of these functions will transfer to each Medicaid managed care plan on September 1, 2023. Public input is open until December 4.
Wisconsin
Wisconsin Releases External Quality Review, Quality Improvement Services RFP. The Wisconsin Department of Health Services released on November 10, 2022, a request for proposals (RFP) to conduct federal and state-mandated external quality reviews of services for the state’s Medicaid programs, including managed care and managed long-term care. The state is also seeking proposals related to quality review, case management record review, and quality improvement services for Medicaid managed care and fee-for-service (FFS) Medicaid, as well as utilization review services for FFS. Contracts will be implemented July 1, 2023, and run for three years with two, one-year renewal options. Proposals are due by December 20, 2022. Read More
Wyoming
Wyoming Would Benefit From Medicaid Expansion, Report Says. The Wyoming Tribune Eagle reported on November 16, 2022, that Medicaid expansion in Wyoming would increase coverage and save the state money, according to a report from the Center on Budget and Policy Priorities think tank. The report based its findings in part on results from Medicaid expansion in neighboring Montana. Read More
National
18 States Have Federally Approved Section 1115 Waivers that Address Social Determinants of Health. The Kaiser Family Foundation reported on November 15, 2022, that 18 states have federally approved Section 1115 waiver demonstrations with provisions that address Medicaid social determinants of health (SDOH). Another eight states have pending requests. Read More
Medicaid, CHIP Enrollment Approaches 90 Million in July 2022. The Centers for Medicare & Medicaid Services (CMS) reported on November 15, 2022, that Medicaid and Children’s Health Insurance Program (CHIP) enrollment approached 90 million in July 2022, with a 93.6 percent retention rate since 2018. The data, which appeared in a CMS brief, also includes information on real and perceived access to mental health and substance use services. Read More
CMS Targets Gaps in Health Equity Data, To Gradually Release Equity Scores. Fierce Healthcare reported on November 11, 2022, that the Centers for Medicare & Medicaid Services (CMS) is working to close gaps in the collection of health equity data and to gradually implement health equity scores, according to a CMS blog post. CMS released social determinants of health screening measures for hospitals in August 2022. Read More
Public Health Emergency Likely to Extend Past January 11. CNBC reported on November 11, 2022, that the U.S. Department of Health and Human Services (HHS) did not give 60 days advance notice of the end of the federal public health emergency (PHE) on November 11, indicating that the PHE will likely extend beyond January 11, 2023. The PHE was most recently extended by 90 days in October 2022. Read More
CMS Hopes to Spur Exchange Plans to Participate in Value-Based Care. Fierce Healthcare reported on November 10, 2022, that the Centers for Medicare & Medicaid Services (CMS) is hoping to spur Exchange plans into participating in value-based care arrangements, in part by aligning quality metrics across Medicaid, Medicare, and the Exchange. Further CMS efforts may include aligning data collection on improving equity across programs. Read More
States Work to Address Churn in Children on Medicaid. Kaiser Health News reported on November 10, 2022, that several states are working to implement policies that provide for continuous Medicaid enrollment of children eligible at birth to age six regardless of changes in family income. Oregon received federal approval to implement the policy in 2023. Others states seeking to implement a similar policy include Washington, California, and New Mexico. Read More
MACPAC Urges CMS to Focus on Health Equity, Improve Dual Eligible Integration in RFI Response. The Medicaid and CHIP Payment and Access Commission (MACPAC) urged federal regulators on November 4, 2022, to improve the collection and reporting of race and ethnicity data, focus on monitoring access to care, and strengthen dual eligible integration. MACPAC made the suggestions in response to a Centers for Medicare & Medicaid Services (CMS) request for information (RFI) seeking ideas on promoting efficiency and equity. MACPAC also called for the streamlining of provider enrollment policies and the need to study the effects of telehealth in Medicaid. Read More
MACPAC Supports CMS Proposed Rule Streamlining Medicaid Eligibility, Enrollment, Renewal Processes. The Medicaid and CHIP Payment and Access Commission (MACPAC) released on November 7, 2022, a letter supporting a proposed rule from the Centers for Medicare & Medicaid Services (CMS) aimed at streamlining Medicaid eligibility, enrollment, and renewal processes. MACPAC also urged CMS to be mindful of the looming task of unwinding the public health emergency before putting any further administrative burdens on states. Read More
Industry News
Sanford Health, Fairview Health Services Agree to Merge. Modern Healthcare reported on November 15, 2022, that Sanford Health and Fairview Health Services have agreed to merge to form a $14 billion health system. Sanford operates 47 hospitals and medical centers in the Dakotas and Minnesota, while Fairview operates 11 hospitals in Minnesota. Bill Gassen, president and chief executive of Sanford, will lead the system. Fairview Health chief executive James Hereford would serve as co-CEO for a year. The transaction is expected to close next year. Read More
Walmart Proposes $3.1 Billion Settlement in Opioid Lawsuits. The Associated Press reported on November 15, 2022, that Walmart has proposed to pay $3.1 billion across 43 states to settle lawsuits regarding the sale of opioids in its pharmacies. Other major pharmacies that have proposed multi-billion dollar settlements are CVS Health and Walgreens. Read More
Centre Partners, Health Enterprise Partners Invest in Toney Healthcare Consulting. Private equity firm Centre Partners and investment firm Health Enterprise Partners announced on November 14, 2022, a joint investment in Toney Healthcare Consulting (THCC), a healthcare consulting firm. THCC works with health plans on areas including utilization management, care management, and value-based care. Read More
CareMax Acquires Medicare Value-Based Care Business of Steward Health Care System. CareMax announced on November 11, 2022, that it completed its acquisition of the Medicare value-based care business of Steward Health Care System, which includes a Medicare Direct Contracting Entity and two Medicare Shared Savings Program accountable care organizations. CareMax now has a network of approximately 2,000 providers and more than 200,000 senior value-based care patients in 10 states. Read More
Bright Health to Exit FL Medicare Advantage Market. Modern Healthcare reported on November 9, 2022, that Bright Health Group will no longer offer Medicare Advantage (MA) plans in Florida in 2023. The company’s only MA offerings next year will be in California. Read More
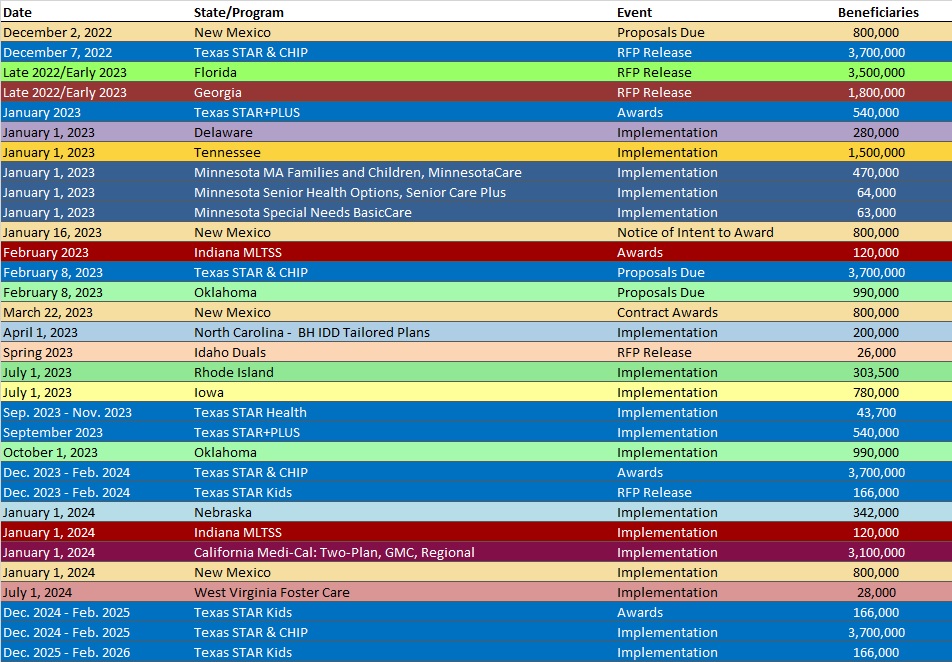
RFP Calendar
HMA News & Events
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Arizona Medicaid Managed Care Enrollment is Up 3%, May-22 Data
- Colorado RAE Enrollment is Up 5.3%, Aug-22 Data
- Florida Medicaid Managed Care Enrollment is Up 8.2%, Sep-22 Data
- Illinois Medicaid Managed Care Enrollment is Up 2%, Sep-22 Data
- Illinois Dual Demo Enrollment is Down 3.1%, Sep-22 Data
- Indiana Medicaid Managed Care Enrollment Is Up 7.2%, Aug-22 Data
- Iowa Medicaid Managed Care Enrollment is Up 5.2%, Sep-22 Data
- Michigan Medicaid Managed Care Enrollment is Up 2.3%, Jul-22 Data
- Michigan Dual Demo Enrollment is Down 2.3%, Jul-22 Data
- Minnesota Medicaid Managed Care Enrollment is Up 4.4%, Jul-22 Data
- Minnesota Medicaid Managed Care Enrollment is Up 4.5%, Aug-22 Data
- Nevada Medicaid Managed Care Enrollment is Up 3.4%, Jun-22 Data
- New Jersey Medicaid Managed Care Enrollment is Up 5.3%, Sep-22 Data
- New York Medicaid Managed Care Enrollment is Up 2%, Jun-22 Data
- New York CHIP Managed Care Enrollment is Down 2.2%, Jun-22 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- California Credentialing, Re-Credentialing Services RFSQ, Nov-22
- California Third Party Monitor RFI, Nov-22
- Oklahoma SoonerSelect Managed Care RFP, Nov-22
- Washington Beacon Health Options Behavioral Health Contract, 2018-23
- Wisconsin External Quality Review, Quality Improvement Services RFP, Nov-22
Medicaid Program Reports, Data, and Updates:
- Maryland Health Benefit Exchange Annual Report, 2018-21
- Michigan Medicaid HITECH Implementation Advanced Planning Documents, FY 2021
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.