This topic comes to us from HMA’s Anissa Lambertino, PhD, of our Chicago office, and Lori Raney, MD, of our Denver office, and Sarah Arvey, PhD, of our Austin office. May is Mental Health Month, and the first week in May is recognized as National Anxiety and Depression Awareness week. Anissa, Lori, and Sarah’s work, highlighted below, utilized geospatial mapping of prevalence of depression among Medicaid beneficiaries and treatment with FQHC locations in rural southeastern Ohio, revealing potential best practices.
Background
In the United States, sixty percent of the population with a diagnosable behavioral health condition do not receive any form of treatment. Behavioral health care access is especially difficult in rural areas where the geographical maldistribution of psychiatrists and other behavioral health specialists is most pronounced. In many rural areas, Federally Qualified Health Centers (FQHCs), also known as Community Health Centers (CHCs), are the backbone of primary care, bringing much needed services to these communities. CHCs often use creative approaches to address the shortage of specialty services in their regions including the use of innovative models of integrating behavioral health into their practices through expansion grants and local community partnerships with community mental health centers or community based organizations. In addition, the robust use of technology such as telepsychiatry and Project ECHO can help build the competence of primary care providers in identifying and treating mild to moderate mental illnesses including depression.
Mapping Hot Spots Reveals Potential Best Practices
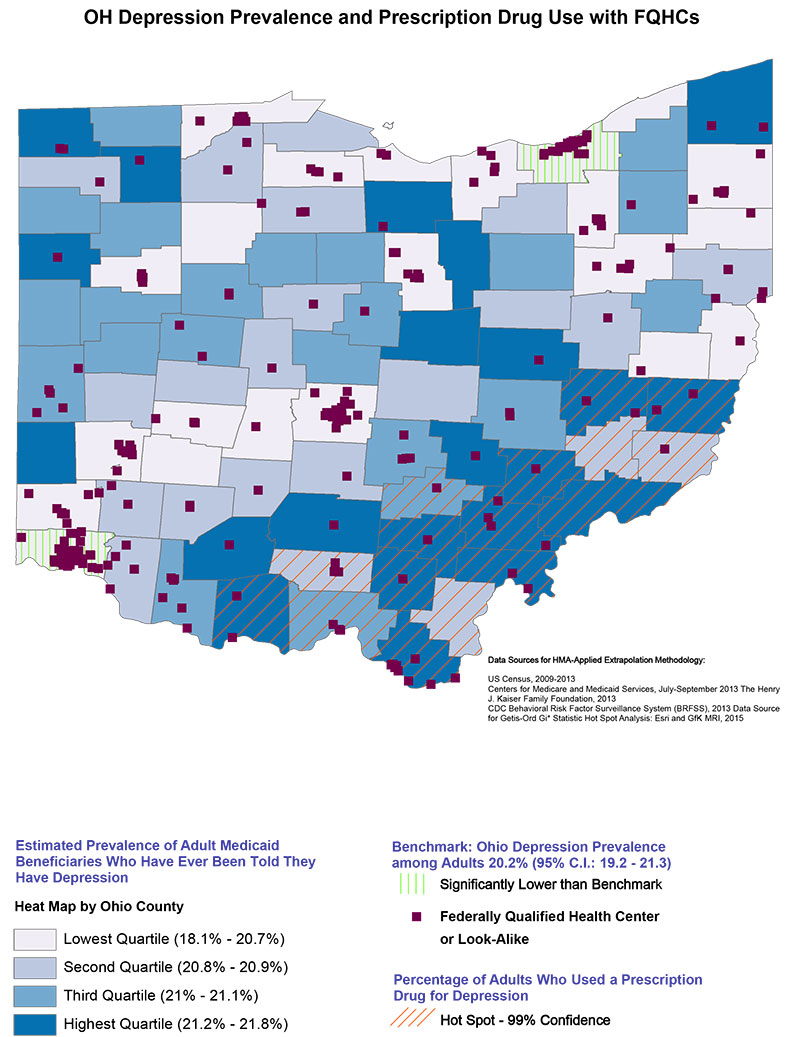
HMA created a geospatial mapping project (see map at end of In Focus section) that layered comparative prevalence of depression among Medicaid beneficiaries and treatment with FQHC locations. The mapping results showed that a cluster of providers in rural Ohio were screening and treating depression, suggesting best practices in the integration of primary care and behavioral health care. The initial mapping project was conducted to evaluate the prevalence of depression among Medicaid beneficiaries across Ohio counties. Using publicly available data from the US Census and Centers for Disease Control Behavioral Risk Factor Surveillance Survey, our mapping exercise exposed a surprising pattern of higher depression prevalence in the southeastern corner of the state; a rural area over 60 miles away from the urban cities of Cincinnati or Columbus. To determine if this higher prevalence depression correlated with treatment, market data for prescription drug use for depression was visually overlaid as a hot spot analysis onto the depression density map. A hot spot analysis identifies statistically significant clusters of low values (cold spot) and high values (hot spot). On the map, the hot spot analysis revealed a cluster of counties with significantly high prescription drug use for depression that matched closely with the geographical distribution of elevated depression, thus indicating that providers are appropriately treating depression in that rural Southeastern area of the state.
Because CHCs are often utilized in underserved areas and are federally mandated to screen for depression, we then overlaid the locations of Ohio CHCs onto the map to determine whether there was any pattern in integrated care delivery by provider groups. In doing so, another pattern emerged. Aa grouping of CHCs were identified in the same counties with a high prevalence of depression as well as the prescription drug hot spot in the southeast corner of the state, suggesting that this group of CHCs have an effective approach to diagnosing and treating depression. The mapping process revealed a pattern that could be used for further investigation into the findings. If the pattern uncovered a unique way of delivering depression screening and treatment in a geographically rural and underserved area it would be good news for the delivery system and could warrant replication in other places.
More Information
For more information on the Ohio Hot-Spotting project, contact:
Anissa Lambertino ([email protected]),
Lori Raney ([email protected]), or
Sarah Arvey ([email protected]).
For more information on HMA’s geospatial mapping and data informatics work, contact Anissa Lambertino.