This week, we reviewed the Oklahoma Health Care Authority’s (OHCA’s) request for proposals (RFP) for a new statewide Medicaid managed care program for individuals who are aged and individuals with disabilities (ABD). The program, called SoonerHealth+, will provide managed acute care, behavioral health, and managed long-term services and supports (MLTSS) to roughly 155,000 members, to be phased in over two years beginning in April 2018. Based on state fiscal year 2014 data, SoonerHealth+ spending per year could exceed $2.5 billion when fully implemented. Proposals are due on February 28, 2017.
Covered Populations, Services
SoonerHealth+ will enroll most individuals in the ABD category of eligibility in mandatory Medicaid managed care, including MLTSS. This includes:
- ABD members who are not eligible for Medicare;
- ABD members dually eligible for Medicaid and Medicare, with incomes below 100 percent of the federal poverty level (FPL);
- Children ages 18 or under receiving services under the Tax Equity and Financial Responsibility Act (TEFRA);
- Individuals meeting nursing facility level of care criteria, receiving home and community-based services (HCBS) through the ADvantage or the Medically Fragile waivers;
- Beginning April 2019 (year two of SoonerHealth+), individuals meeting ICF-ID level of care criteria in the Community or the In-Home Supports waivers; and
- Beginning April 2020 (year three of SoonerHealth+), individuals residing in institutional care settings, as well as children in the custody of the Oklahoma Department of Human Services or in Tribal custody.
As of June 2016, there were approximately 155,000 eligible members in the state – around 136,000 adults and just under 19,000 children. Included in the SoonerHealth+ covered populations are several HCBS waiver populations, with a little under 27,000 participants as of this year. There are roughly 5,000 additional members who are on waiver waiting lists who will be enrolled in SoonerHealth+.
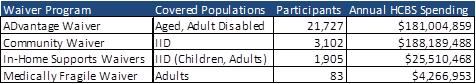
Source: SoonerHealth+ RFP; OHCA Annual Report 2015
Native Americans, if eligible, will be able to voluntarily enroll in SoonerHealth+, but will not be mandated or auto-assigned.
Excluded from SoonerHealth+ are any non-ABD Medicaid beneficiaries, individuals enrolled in a behavioral health home, members of a Program of All-inclusive Care for the Elderly (PACE) plan, participants in the Homeward Bound waiver, and individuals enrolled in the Living Choice/Money Follows the Person program.
While nearly all benefits will be covered for SoonerHealth+ members when fully implemented, non-emergency medical transportation (NEMT) is carved-out of SoonerHealth+ and provided under a separate vendor contract.
Contract Awards, Term of Contract
SoonerHealth+ will be implemented statewide across two regions – East and West – established to be roughly equal in population size. Bidders on the SoonerHealth+ RFP may bid to serve one or both regions. OHCA anticipates awarding three contracts per region, though may award as few as two or as many as four.
The initial contract term will run through June 30, 2019, with four one-year optional extensions, plus one additional six-month extension, taking the potential full life of the contract through December 31, 2023.
RFP Timeline
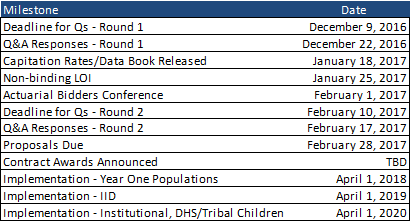
OHCA will conduct two rounds of questions and answers from prospective bidders, both before and after the release of the data book and capitation rates in mid-January 2017. A non-binding letter of intent (LOI) is due on January 25, 2017. Proposals are due to OHCA on February 28, 2017. At this time, contract award announcement timing is yet to be determined. As noted above, implementation is scheduled for April 1, 2018, with implementation for individuals with intellectual disabilities to follow in April, 2019, and full implementation to all populations in April, 2020.