1290 Results found.

HMA develops brief exploring equity and innovation in children’s behavioral health systems
Lifting Voices is an initiative developed to inform the transformation of the youth behavioral health care system. The project leaders are parents of children who nearly died on multiple occasions from severe behavioral health conditions, and they are professionals with a deep understanding of the opportunities and challenges faced by behavioral health care policy makers and reformers. They share the belief that their knowledge, desperation, and resources afforded their children access to interventions that should be accessible to every youth who needs them. Their experience of the care delivery system has also inspired their commitment to highlight the urgent improvements necessary to support struggling children and parents affected by the nation’s youth behavioral health crisis.
To learn more about Lifting Voices, see the October 2023 report here.
HMA Principals and behavioral health policy and practice transformation consultants Heidi Arthur, LMSW and Ellen Breslin, MPP partnered with Sheilah Gauch, LISW, M.Ed., Principal and Clinical Director with the Dearborn Academy and Echo Lustig, B.A., young adult behavioral health advocate, to share findings from the first phase of the three-part Lifting Voices initiative at Putting Care at the Center, the annual conference of the Camden Coalition’s National Center for Complex Health and Social Needs Initiative. See: Putting Care at the Center 2023, Elevating behavioral health in whole-person care. Boston, MA, November 1-3, 2023. Please look for us at the Beehive poster station on:
- Thursday, November 2 from 2:45 pm – 4:30 pm ET
- Friday, November 3 from 8:45 am – 10:30 am ET

Using Virtual Research Data Center (VRDC) Data to Answer Big Questions
Health Management Associates (HMA) is utilizing Virtual Research Data Center (VRDC) data to do what HMA does best: solve publicly funded healthcare’s most challenging problems. The combination of our deep analytics expertise and our nationally renowned subject matter experts can help you solve your toughest challenges.

We are committed to helping clients meet their needs through:
Market Analysis
Want to know how many psychologists are treating Medicaid patients in a county? Or how many duals got NEMT in a year? We can tell you that. How many folks on Medicare got drugs for Memory Loss last year? We can tell you that too. The VRDC allows us to examine the Medicaid and Medicare populations with significant precision to inform your decisions.
Consulting Services
We love hard questions. Carefully designed smaller queries can add up to answer big questions like “Does access to Non-Emergency Medical Transportation help patients managing challenging chronic medical conditions?” or, “Are services critical to patient success being delivered equitably to patient populations?” HMA can help you answer your hardest questions by breaking them into smaller questions that add up to big results. Outcomes Survey (HOS) specific to BH, and align data performance to quality improvement efforts.
Quality Improvement and KPI Benchmarking
HMA’s team of quality experts can help you identify metrics that matter internally to your organization as well as to your payers and providers. We can run metrics against these Medicaid and Medicare data to prepare you to manage risk through deep data analysis and creation of benchmarks that help manage access, cost, quality, and utilization.
HMA’s access to VRDC data through this agreement include:
Data representative of 100 percent of Medicare and Medicaid beneficiaries and their medical experience expressed as claims
Data representative of 100 percent of Part D Drug Event (PDE) data
Detailed Long-Term Care data for all Medicare and Medicaid beneficiaries through the MDS dataset
We can help organizations including:
State and municipal departments of health and public health
Health plans
Provider organizations
Analytics and technology vendors
Private equity
Correctional health
Contact our experts:

Jim McEvoy
Senior Principal, Policy and Strategy

Florida releases procurement for statewide Medicaid prepaid dental program
This week, our In Focus section reviews the Florida Statewide Medicaid Prepaid Dental Program invitation to negotiate (ITN) released October 6, 2023, by the Florida Agency for Health Care Administration (AHCA). Contracts will serve 4.4 million Statewide Medicaid Managed Care (SMMC) members.
Background
The Florida Statewide Medicaid Prepaid Dental Program is a full-risk capitated dental program, which began rolling out by groups of regions in December 2018. The incumbent statewide Medicaid dental plans are DentaQuest, Liberty, and MCNA Dental.
Florida also is reprocuring its traditional managed medical assistance (MMA) program and managed long-term care program under SMMC. Awards for Medicaid managed care organizations (MCOs) are expected in February 2024.
ITN
Florida intends to award contracts to at least two plans. One of AHCA’s goals is to contract with plans that will support the HOPE Florida: Pathways to Prosperity initiative, which focuses on community collaboration between the private sector, faith-based community, not-for-profits, and government entities to break down traditional community silos. Through this program, AHCA seeks to:
- Improve oral health outcomes by implementing a quality continuum
- Enable personalized oral healthcare, particularly for people with special needs
- Strengthen the network of dental providers
- Integrate medical and dental care
In addition to the services currently provided, dental plans will cover authorized hospital outpatient and ambulatory surgery center (ASC) services as part of the new contracts. Plans will cover ancillary medical services provided secondarily to dental care in an ASC or outpatient hospital setting when medically necessary.
Dental plans will continue to operate statewide across all regions. Capitation rates for Medicaid and dually eligible members, however, are set regionally. Rates for medically necessary procedures are set at a statewide level. The new contracts will consolidate the 11 regions into nine as shown in the table below.
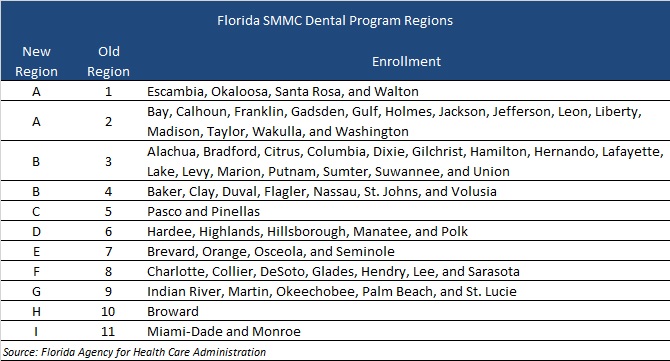
Timeline
Responses are due January 5, 2024, and notification of intent to award is anticipated to be released on March 29, 2024. Contracts will run from the execution date in 2024 through 2030.
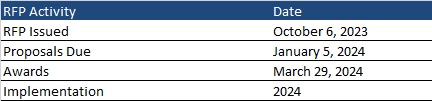
Evaluation
Technical proposals will be scored using a total weighted score of 6,600, as shown in the table below.
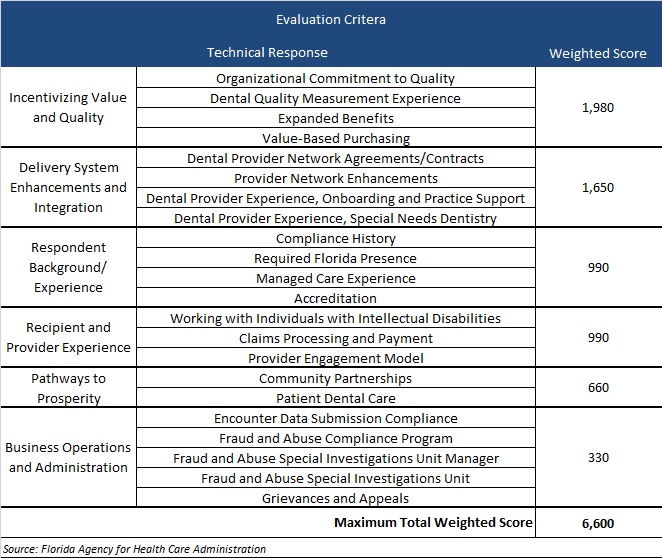

Consumer Assessment of Healthcare Providers Systems (CAHPS): Improving Member Experience
Medicare and Medicaid plans are faced with a barrage of regulations, including quality rankings. To improve rankings plans can, and should, work to improve their Consumer Assessment of Healthcare Providers Systems (CAHPS) scores.
The CAHPS annual survey measures member experience with providers and Medicare and Medicaid health insurance plans. It has also become a critical metric used by the Centers for Medicare and Medicaid Services (CMS).
Plans can work to improve CAHPS scores by developing a comprehensive improvement plan involving a holistic year-around approach that involves monitoring the member experience from enrollment through disenrollment. With score improvement comes incentive payments tied to high quality performance.
CAHPS SCORES ARE USED BY:
The National Committee for Quality Assurance (NCQA) to STAR rate health plans in accreditation scoring
Potential members to compare plan scores against one another on the NCQA website
Several state Medicaid programs that require plans to report these surveys and use scores as part of their incentive programs
CMS, which has increased its STAR rating, CAHPS-related measure from double weighted to quadruple weighted in contract year 2021
Medicare Advantage Prescription Drug (MAPD) plans, which use CAHPS to calculate 32% of the overall aggregate score
CAHPS COHORTS THAT ARE MEDICARE STAR MEASURES
PART C CAHPS MEASURES (WEIGHTS)
Getting needed care (4)
Getting appointment and care quickly (4)
Customer service (4)
Rating of healthcare quality (4)
Rating of health plan (4)
Care coordination (4)
Annual flu vaccine (1)
PART D CAHPS MEASURES (WEIGHTS)
Rating of drug plan (4)
Getting needed prescription drugs (4)
ADDITIONAL STAR MEASURES AND ACTIVITIES THAT RELATE TO MEMBER EXPERIENCE
PART C MEASURES (WEIGHTS)
Complaints about the health plan (2)
Member choosing to leave the plan (2)
Plan makes timely appeals decisions (2)
Reviewing appeal decisions (2)
Call center, language interpreter and TTY availability (2)
Health plan quality improvement (5)
PART D MEASURES (WEIGHTS)
Call center, language interpreter and TTY availability (2)
Complaints about the drug plan (2)
Member choosing to leave the drug plan (2)
Drug plan quality improvement (5)
Health Management Associates’ expert colleagues can help plans outline an organizational assessment of member experience and customize interventions and solutions to increase scores.

Our team of quality and accreditation experts can help organizations improve customer service and scores by:
Establishing a year-around effort
Using an organizational effort to break down department silos and improve cooperation between departments
Assessing core functions within the plan and contractors that contribute to member experience including marketing, enrollment, disenrollment, UM, QI, member service, grievances, appeals, etc.
Identifying and addressing patient frustrations with providers and plans before they become problematic
Leveraging information technology to make websites more user friendly
Addressing care and service gaps to ensure member outreach is calibrated and tailored throughout the year
Recognizing social determinants of health (SDOH) are often overlooked in access to care-related issues, such as lack of transportation or lack of funds for co-payments
Outlining techniques for obtaining point-of-service feedback to help address potential member experience issues before they arise
Contact our experts:

Mary Walter
Principal

Star Rating: We Can Help You Navigate to a Higher Level

What is the VALUE of a Star in your plan(s)?
What initiatives have you introduced to prepare for the changes in the Star Rating that may impact your overall Star Rating results?
What are you doing for health equity focus? What data are you collecting for health equity?
What do you think are your organization’s financial implications when Star Rating requirements change?
What are your Star Rating strategies for increasing your organization’s market share and viability?
What sort of interventions, data sources, analytics and reporting have you found to be successful to improving your Star Rating?
WE CAN HELP YOU BY:
Establishing a year-around effort to improve Star Rating performance
Assessing core functions within the plan and contractors that contribute to understanding members
Identifying and addressing customer concerns with providers and plans before they become problematic
Leveraging information technology to make websites more user friendly
Addressing care and service gaps to ensure member outreach is calibrated and tailored throughout the year
Working on health equity issues including sharing techniques for obtaining data
Leveraging all data and intervention efforts (such as risk and quality) to drive decision and focus
Contact our experts:

Mary Walter
Principal

HMA Can Help You Prepare for The Joint Commission (TJC) Accreditation and Certification
HMA’s team of experts have completed accreditation requirements with our clients as well as in our formal executive and operational leadership roles in the health care setting. We work closely with our clients and with TJC and other accreditation programs with a focus on improving healthcare quality and favorable outcomes. Our team of seasoned healthcare executive consultants bring more than 100 years of experience in clinical, quality, and operations, with proven results. HMA offers a full continuum of accreditation services for hospitals, ambulatory surgical centers (ASCs), Federally Qualified Health Centers (FQHCs) and behavioral health (BH) care settings. We work closely with FQHCs to provide assistance for certifications and advanced certifications in health equity (HE). HMA can offer onsite or virtual mock survey and gap analysis preparation for TJC accreditation, as well as tactical and advisory support to prepare our client leadership teams for a winning accreditation survey results and supporting the development of a sustainable plan to achieve year over year success!

Our experts can help you by:
Assessing core functions supporting the implementation of the latest TJC standards and interpretation of the standards
Building the business case for TJC accreditation
Guiding your team through the new HE standards
Creating quality and assessment improvement plan (QAPI) to lead to a successful survey
Continuous survey readiness support via a sustainable plan
And so much more across the continuum
Contact us at [email protected]
Contact our experts:

Trisha Bielski
Senior Consultant

Mary Walter
Principal

October 11, 2023
Florida Releases Procurement for Statewide Medicaid Prepaid Dental Program
