This week's roundup:
- In Focus: Cut to the Point: A Summary of 2024 Star Rating Cut Point Changes
- Arizona to Release Medicaid PBM RFP ‘in the Coming Weeks’
- Medicaid Eligibility Redeterminations News: Arizona, Florida, Georgia, Mississippi, North Carolina, Texas, Wyoming
- Florida Launches Dental Provider Incentive Program
- Minnesota Eliminates Parental Fees for Medicaid Coverage of Children With Disabilities
- Nevada Governor Proposes Exchange Reinsurance in ‘Revision’ to Public Option Law
- New York Medicaid Spending Exceed Expectations, Report Finds
- North Carolina Receives Final Federal Approval for Medicaid Expansion
- Oregon Announces 3.4 Percent Increase in 2024 Capitation Rates for Medicaid Coordinated Care Organizations
- Oregon Releases RFP to Expand PACE Services
- Long-term Services, Supports Spending Falls as Percentage of Total Medicaid Expenditures, CMS Reports
- State Medicaid Programs Disenroll 8.8 Million Beneficiaries During First 6 Months of Redeterminations, KFF Finds
- Alignment Health, Walgreens to Jointly Market Medicare Advantage Plans in 2024
In Focus
Cut to the Point: A Summary of 2024 Star Rating Cut Point Changes
This week, our In Focus section highlights a white paper that Wakely, a Health Management Associates company, released in October 2023, “Cut to the Point: A Summary of 2024 Star Rating Cut Point Changes”. The paper reviews 2024 Medicare Star Rating data, including the Star Rating Technical Notes, which the Centers for Medicare & Medicaid Services (CMS) released October 13, 2023.
The data summarizes how Medicare Advantage Organizations (MAOs) performed on various quality measures during the 2022 measurement year and serves as an indication of changing Medicare Advantage spending in 2025 as a result of changes in Medicare Advantage Prescription Drug (MA-PD) Overall Star Ratings. The publication of the 2024 Star Rating Technical Notes provided an opportunity for Wakely to analyze measure-level cut point changes. This paper looks at the latest cut point changes to determine how the Tukey Outlier Deletion methodology and changes in the overall quality performance have affected Star Rating cut points.
Wakely will also host a webinar, Stars and Strikes: 2024 Star Ratings and the Impact of Tukey, at 2:30 pm ET on November 14, 2023. The webinar will cover the recently released 2024 Star Ratings, including an analysis of the expected impact on 2025 Medicare payments. Attendees should expect to hear discussions about the latest program changes and resulting impact on the contract-level star ratings, including implementation of the Tukey outlier deletion methodology. In addition, Wakely colleagues will cover the upcoming changes to the Star Rating program and discuss their potential impact on Medicare Advantage Organizations. Please register here.
For questions, please contact Suzanna-Grace Tritt, [email protected], or Lisa Winters, [email protected].
HMA Roundup
Arizona
Arizona to Release Medicaid PBM RFP ‘in the Coming Weeks’. The Arizona Health Care Cost Containment System announced on October 13, plans to release a request for proposals (RFP) for its Medicaid pharmacy benefit management (PBM) services program “in the coming weeks.” Read More
Arizona Seeks Approval for Medicaid Coverage of Native Healing Services. State of Reform reported on October 16, 2023, that the Arizona Health Care Cost Containment System (AHCCCS) is seeking federal approval of a Section 1115 waiver request to cover traditional Native healing practices using Medicaid funds. Native healing practices include using local roots, plants, and trees as medicine or ailments; and sweat lodges. Read More
Arizona Continues Housing, Health Opportunities Services Planning While Awaiting CMS Approval. State of Reform announced on October 13, 2023, that the Arizona Health Care Cost Containment System (AHCCCS) is developing a protocol for assessment of care planning and an implementation plan for the state’s proposed Housing and Health Opportunities Section 1115 waiver demonstration. The waiver, which allows use of federal Medicaid funds for housing vouchers, would go live on October 1, 2024, assuming it receives federal regulatory approval. Read More
Arizona Seeks 1115 Waiver Amendment to Allow Medicaid Payments to Parents Caring for Minor Children. The Arizona Health Care Cost Containment System (AHCCCS) announced on October 12, 2023, that it is seeking federal regulatory approval of a Section 1115 waiver amendment allowing the state to make Medicaid payments to parents who serve as caregivers for minor children. AHCCCS will accept comments through November 11. Read More
State Disenrolls 289,124 Medicaid Beneficiaries Since Redeterminations Began. AZPM reported on October 14, 2023, that Arizona has disenrolled 289,124 Medicaid beneficiaries since redeterminations began in April. The state has renewed coverage for 812,787 beneficiaries. Read More
California
California Governor Signs Law to Raise Healthcare Workers’ Minimum Wage. The Associated Press reported on October 13, 2023, that California Governor Gavin Newsom signed a new law to raise the minimum wage for healthcare workers to $25 per hour over the next decade. Almost half of low-wage healthcare workers and their families are on Medicaid or other government support programs, according to a study by the University of California-Berkeley Labor Center. Read More
California to Provide Medicaid Coverage to 700,000 Undocumented Immigrants. Modern Healthcare reported on October 17, 2023, California is expected to provide Medicaid coverage to an additional 700,000 low-income, undocumented immigrants beginning in January. Since 2016, California has been gradually opening up Medicaid to undocumented individuals. Read More
Colorado
Colorado Medicaid Communications to Members Contain Inaccuracies, Audit Finds. The Denver Gazette reported on October 16, 2023, that letters from Colorado Medicaid to its members often contain incorrect deadlines, contradictory and confusing messages, unclear guidance, or inaccuracies, according to an audit by the Colorado Office of the State Auditor. Out of 80 letters sent to Medicaid beneficiaries, 72 had at least one or more issues. Similar issues have been found in previous audits. Read More
Florida
Florida Launches Dental Provider Incentive Program. The Florida Agency for Health Care Administration announced on October 18, 2023, a Dental Provider Incentive Program, which will offer bonus reimbursements to dentists who meet certain preventive and diagnostic quality measures for children under age 21, effective October 1, 2024. Read More
Florida Disenrolls 92,576 Beneficiaries During September Redeterminations. The Florida Phoenix reported on October 17, 2023, that Florida disenrolled 92,576 Medicaid beneficiaries during September eligibility redeterminations. The state has disenrolled a total of 616,652 enrollees since redeterminations began in April. Read More
Officials Defend State’s Handling of Medicaid Redeterminations Process. WUSF reported on October 11, 2023, that officials from the Florida Department of Children Families, Agency for Health Care Administration, and Florida Healthy Kids Corporation defended the state’s handling of Medicaid eligibility redeterminations in a hearing before the state Senate Health and Human Services Appropriations Committee. The state faces a potential class action lawsuit filed by disenrolled members. Read More
Governor’s 2024 Legislative Agenda to Focus on Healthcare. The Orlando Medical News reported on October 4, 2023, that Florida Governor Ron DeSantis’s 2024 legislative agenda is expected to focus on healthcare initiatives, including provider access, affordability, and restrictions on pharmacy benefit managers. Republican legislators remain opposed to Medicaid expansion. Read More
Georgia
Georgia Reinstates Coverage for Nearly 18,000 Medicaid Beneficiaries. Rough Draft Atlanta reported on October 16, 2023, that Georgia has reinstated coverage for nearly 18,000 previously disenrolled Medicaid beneficiaries following ex parte renewal errors. U.S. Senators Raphael Warnock (D-GA) and Jon Ossoff (D-GA) joined other lawmakers in expressing concern about the state’s auto-renewal process in a letter to the Department of Health and Human Services. Read More
Kansas
Kansas Resumes Medicaid Eligibility Redeterminations Following Renewal Process Change. KCUR reported on October 12, 2023, that Kansas will resume sending Medicaid renewal notices following approval to conduct redeterminations by individual instead of by family. As of September, 26,362 beneficiaries have been disenrolled after being found to not be eligible and 55,912 had coverage ended but are currently in a 90-day reinstatement window. Read More
Minnesota
Minnesota Eliminates Parental Fees for Medicaid Coverage of Children With Disabilities. The Minnesota Department of Human Services announced on October 17, 2023, that it has stopped requiring parents to pay monthly Medicaid fees for children with disabilities who get coverage through the Tax Equity and Fiscal Responsibility Act option (TEFRA) or through assessments for Home and Community Based Services. Fees were based on family income levels. Read More
Mississippi
Mississippi Disenrolls 12,828 Medicaid Beneficiaries During September Redeterminations. Mississippi Today reported on October 17, 2023, that Mississippi disenrolled 12,828 Medicaid beneficiaries during September redeterminations, including 9,594 for procedural reasons. The state renewed coverage for 31,549 beneficiaries. To date, the state has disenrolled 81,454 beneficiaries. Read More
Missouri
Missouri Receives Federal Approval for Appendix K Application. Ozark Radio News reported on October 12, 2023, that the Centers for Medicare & Medicaid Services approved Missouri’s request to update its Section 1915(c) Home and Community-based Services (HCBS) waivers with the Emergency Preparedness and Response Appendix K, effective July 1, 2023, through six months after the end of the Public Health Emergency. The amendment includes an increase to the maximum lifetime limitation for the Community Transition service; updated rate methodology for Group Home Nursing; and updated rate methodology for Individualized Supported Living. Read More
Montana
Montana Receives Approval for Community-Based Mobile Crisis Services SPA. The Centers for Medicare & Medicaid Services announced on October 17, 2023, that it has approved the Montana community-based mobile crisis state plan amendment (SPA). The state can now utilize federal Medicaid funding to create mobile crisis intervention teams to provide Medicaid crisis services 24/7 to eligible individuals experiencing a behavioral health or substance use crisis. Read More
Nevada
Nevada Governor Proposes Exchange Reinsurance in ‘Revision’ to Public Option Law. The Center Square reported on October 13, 2023, that Nevada Governor Joe Lombardo’s promise to “substantially revise” the state’s public option law includes a proposed reinsurance program for Exchange plans, quality incentive payments, and loan repayment and scholarships for healthcare workers. The public option law, passed in 2021, requires all Medicaid plans in the state to submit a good-faith bid to offer a public option plan on the state Exchange effective January 2026. Read More
New York
New York Medicaid Spending Exceed Expectations, Report Finds. Empire Center reported on October 17, 2023, that New York Medicaid spending totaled $19.7 billion through six months of fiscal 2024 or about 16 percent higher than budget projections, according to a state comptroller’s report. Front-loaded budget projections expected the state to spend 62 percent of its annual Medicaid budget during the first half of the year; however, expenditures reported by the comptroller showed spending at 72 percent. Read More
North Carolina
North Carolina Receives Final Federal Approval for Medicaid Expansion. The Associated Press announced on October 13, 2023, that the Centers for Medicare & Medicaid Services gave North Carolina final approval to implement Medicaid expansion. The program, which goes live December 1, is expected to cover an additional 600,000 individuals. Read More
North Carolina Disenrolls 99,925 Medicaid Beneficiaries Through August Redeterminations. NC Newsline reported on October 12, 2023, that North Carolina has disenrolled 99,925 Medicaid beneficiaries during redeterminations from June through August. Of those disenrolled, 87,308 lost coverage due to procedural reasons and 12,617 lost coverage because they were no longer eligible. The state renewed coverage for 384,200 beneficiaries. Approximately 300,000 people in the Medicaid Family Planning program will automatically have full Medicaid coverage once Medicaid expansion begins on December 1. Read More
North Dakota
North Dakota Hospitals Form Clinically Integrated Network to Strengthen Rural Healthcare. Modern Healthcare reported on October 12, 2023, that 23 North Dakota critical access hospitals have formed a clinically integrated network, named the Rough Rider High-Value Network. The hospitals have received $3.5 million of state funding to help transition to value-based care, with the hospitals also planning to participate more heavily in alternative payment models such as the Medicare Shared Savings Program and accountable care organizations. Read More
Oregon
Oregon Announces 3.4 Percent Increase in 2024 Capitation Rates for Medicaid Coordinated Care Organizations. The Oregon Health Authority announced on October 17, 2023, a 3.4 percent increase in 2024 capitated rates to $518 per member per month on average for the state’s Medicaid coordinated care organizations. Read More
Oregon Releases RFP to Expand PACE Services. State of Reform reported on October 13, 2023, that Oregon has released a request for proposals (RFP) aimed at expanding the Program of All-Inclusive Care for the Elderly (PACE) statewide. Bids are due November 30, and the state intends to award one or more contracts. Contracts are expected to begin on December 31 for a maximum of 10 years. Read More
Oregon Enacts Law to Transition from Federal to State-based Exchange. Insurance Newsnet reported on October 12, 2023, that Oregon enacted legislation allowing the state to transition from the federal health insurance marketplace to a state-based Exchange. Eighteen states and the District of Columbia operate state-based Exchanges. Read More
Pennsylvania
Pennsylvania to Audit State Contracts, Oversight of Medicaid PBMs. The Pennsylvania Department of the Auditor General announced on October 11, 2023, that it will conduct an audit of state contracts and oversight of Medicaid pharmacy benefit managers (PBMs). The audit is expected to take 12 to 18 months to complete. Read More
Texas
Texas Disenrolls 332,104 Medicaid Beneficiaries During September Redeterminations. The Texas Department of State Health Services reported on October 10, 2023, that the state has disenrolled 332,104 Medicaid beneficiaries following September redeterminations. Approximately 161,996 lost coverage due to procedural reasons and 170,108 were found ineligible. 261,791 beneficiaries had their coverage renewed.
Wyoming
Wyoming Disenrolls 9,000 Medicaid Beneficiaries During September Redeterminations. The Wyoming Business Report reported on October 16, 2023, that Wyoming has disenrolled 9,000 Medicaid members, including approximately 7,800 for procedural reasons. Read More
National
Long-term Services, Supports Spending Falls as Percentage of Total Medicaid Expenditures, CMS Reports. The Centers of Medicare & Medicaid Services (CMS) reported on October 17, 2023, that Medicaid long-term services and supports (LTSS) spending as a percentage of total Medicaid expenditures decreased from 47 percent in fiscal 1988 to 33 percent in fiscal 2020, according to the annual Medicaid LTSS Annual Expenditures Report for fiscal 2020. The decline was due to an increase in spending on beneficiaries without disabilities who do not use LTSS. Overall, LTSS spending was $199.4 billion in fiscal 2020, up 20 percent from fiscal 2019. Read More
Enrollment in LTSS, HCBS Waiver Programs Rises in 2019, CMS Reports. The Centers for Medicare & Medicaid Services (CMS) reported on October 17, 2023, that enrollment in comprehensive long-term services and supports (LTSS) in home and community-based (HCBS) settings through section 1915(c) waiver programs was about 1.9 million in 2019, up 5.2 percent from 2018. Average program expenditures were $30,063 per member per year, up one percent from 2018. Read More
State Medicaid Programs Disenroll 8.8 Million Beneficiaries During First 6 Months of Redeterminations, KFF Finds. KFF reported on October 18, 2023, that state Medicaid programs have disenrolled 8.8 million beneficiaries during the first six months of eligibility redeterminations, representing nine percent of all Medicaid enrollees. An estimated 16 million Medicaid beneficiaries have had their coverage renewed. Read More
Some Medicare Advantage Plans Receive Lower Star Ratings for 2024. Modern Healthcare reported on October 16, 2023, that about 10 percent of Medicare Advantage plans experienced a drop in 2024 Medicare Advantage star ratings. In general, not-for-profit plans scored higher than for-profit plans. Forty-two percent of Medicare Advantage plans will have an overall rating of four stars or higher in 2024 and will receive quality bonuses, down from 51 percent in 2023. Read More
CMS Increases 2024 Medicare Part A & B Premiums, Deductibles. The Centers for Medicare & Medicaid Services (CMS) announced on October 13, 2023, that Medicare Part B premiums will increase $9.80 or 5.9 percent to $174.70 in 2024 and the annual deductible will be $240 in 2024, an increase of $14 from 2023. The Medicare Part A deductible will be $1,632 in 2024, an increase of $32 from $1,600 in 2023. CMS attributes the increases to higher health care spending. Read More
Congress Looks to Advance PBM Transparency Legislation. Modern Healthcare reported on October 12, 2023, that Congress appears increasingly likely to agree on pharmacy benefit management (PBM) transparency legislation. The House has already consolidated major elements of separate committee bills into the Lower Costs More Transparency Act of 2023. Senate committees have also advanced separate bills, which would address things like pricing transparency, clawbacks, spread pricing, and drug rebates. Read More
U.S. Senator Calls for Examination, Increased Oversight of Medicaid Plan Care Denials. The Washington Informer reported on October 11, 2023, that U.S. Senator Robert Casey (D-PA) is calling for an examination of the Medicaid managed care system and increased regulatory oversight of care denials. In a letter to the Office of the Inspector General (OIG), Casey cited data on care denials from a recent OIG report. Read More
Most Federal Population Health Surveys Fail to Ask About Intellectual Disability, Sexual Orientation. The Medicaid and CHIP Payment and Access Commission (MACPAC) reported in October 2023, that less than half of federal population health surveys include questions about intellectual disability, serious mental illness, primary language, English proficiency, sexual orientation, and gender identity. MACPAC contracted with The State Health Access Data Assistance Center to conduct the review, which analyzed 13 federal population health surveys. The majority of surveys did include questions on functional disability. Read More
Industry News
Alignment Health, Walgreens to Jointly Market Medicare Advantage Plans in 2024. Modern Healthcare reported on October 18, 2023, that Alignment Health, a Medicare Advantage plan, and Walgreens Boots Alliance have agreed to jointly market Medicare Advantage plans for 2024 in Arizona, California, Florida, and Texas. The plans will have zero premiums and zero copays for more than 10,000 prescription drugs at Walgreens pharmacies. Read More
BCBS-MI Finalizes Acquisition of BCBS-VT. Modern Healthcare reported on October 11, 2023, that Blue Cross Blue Shield of Michigan has finalized its acquisition of Blue Cross Blue Shield of Vermont in a non-cash deal. The combined companies, with 5.4 million members, will maintain separate headquarters, leadership, and workforces. Read More
CMS to Terminate Clear Spring Health Medicare Part D Contract Following Low Star Ratings. Health Payer Specialist reported on October 18, 2023, that the Centers for Medicare & Medicaid Services (CMS) is terminating Illinois-based Clear Spring Health’s Medicare Part D drug contract at the end of 2024, following deficient quality ratings for three consecutive years. CMS has also imposed sanctions, barring the plan from marketing and enrolling new members. Clear Spring covers about 100,000 Part D enrollees in Colorado, Georgia, Illinois, South Carolina, and Virginia. Read More
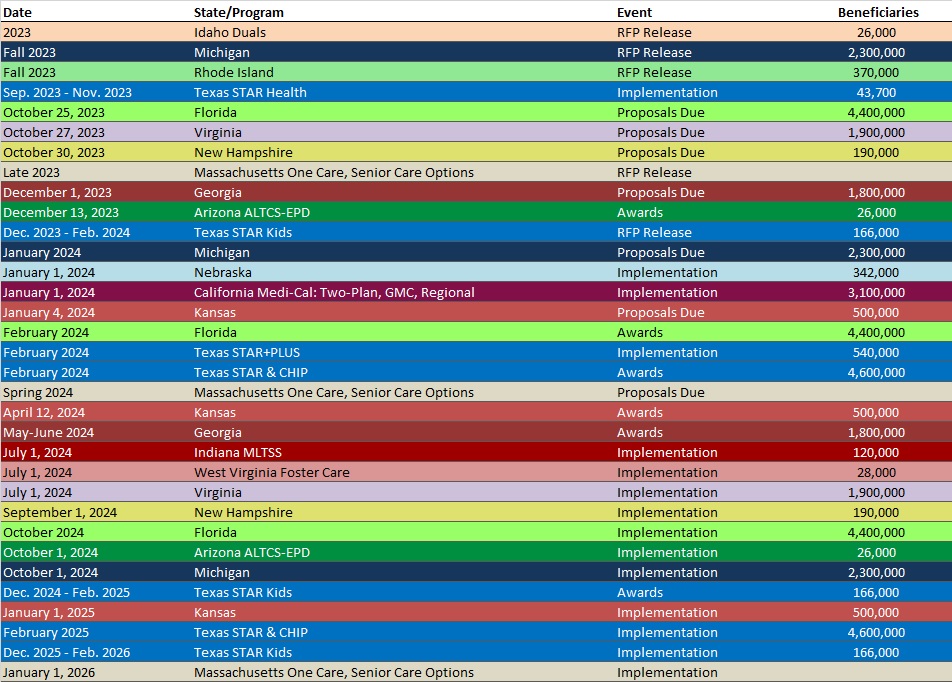
RFP Calendar
HMA News & Events
Upcoming HMA Webinar:
Opportunities for State Regulators to Shape Policy and Regulation of Treatment for Substance Use Disorder. Thursday, November 2, 2023, 12 p.m. ET. Rescheduled from June 20, 2023. Health Management Associates (HMA) is offering a 3-part series of webinars looking at the effect of proposed regulations on delivery of opioid treatment services to the population facing addiction issues. In this third and final webinar, HMA consultants will highlight opportunities for state regulators to shape policy and regulation of SUD treatment. New federal regulations encourage significant changes to how opioid treatment is provided, with the goal of expanding access and improving patient-centered care. State regulators will need to adapt their regulatory practices and work closely with Medicaid agencies and treatment providers so the new regulations can achieve their intended goals. This webinar will discuss how State Opioid Treatment Authorities (SOTAs), licensing entities, and state Medicaid agencies will need to work together to craft updated regulations, facility licensing, and reimbursement practices that advance person-centered care.
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Florida Medicaid Managed Care Enrollment is Up 2%, Mar-23 Data
- Florida Medicaid Managed Care Enrollment is Up 1.6%, Feb-23 Data
- Kansas Medicaid Managed Care Enrollment is Down 13%, Sep-23 Data
- Kansas Medicaid Managed Care Enrollment is Down 11.9%, Aug-23 Data
- Pennsylvania SNP Membership at 226,106, Mar-23 Data
- South Dakota SNP Membership at 3,146, Mar-23 Data
- South Dakota Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Washington SNP Membership at 110,213, Mar-23 Data
- Washington Medicaid Managed Care Enrollment is Up 0.5%, May-23 Data
- Washington Medicaid Managed Care Enrollment is Flat, Apr-23 Data
- Washington Medicaid Managed Care Enrollment is Flat, Mar-23 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Oregon PACE RFP, Sep-23
Medicaid Program Reports, Data, and Updates:
- Colorado Health Plan CAHPS Reports, 2017-23
- Colorado Medical Premiums Expenditure and Caseload Reports, FY 2015-23
- Michigan Medicaid Capitation Rate Certification Reports, CY 2019-24
- Mississippi PHE Medicaid Redeterminations Monthly Reports to CMS, Sep-23
- Nebraska Division of Behavioral Health Strategic Plans, 2017-24
- Oregon Medicaid Capitation Rate Certifications, CY 2020-24
- Pennsylvania Community HealthChoices Databooks, CY 2023-24
- Pennsylvania DHS Strategic Plans, 2019-23
- Pennsylvania Medical Assistance, CHIP Managed Care Quality Strategy, 2020-23
- South Dakota Medicaid State General Fund Savings Reports, SFY 2019-22
- Texas PHE Medicaid Redeterminations Monthly Reports to CMS, Sep-23
- Washington Medicaid Managed Care Service Area Matrices, 2020-23
- Wyoming Medicaid PMPM Expenditures and Utilization Reports, SFY 2015-22
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.