This week's roundup:
- In Focus: Mental Health and Addiction Crises Top the Federal Policy Agenda in 2023
- Online Registration for HMA Quality Conference Ends February 21
- Alabama Legislative Committee Puts Hold on Inmate Health Contract
- Florida CHIP Enrollment Likely to Increase as Medicaid Redeterminations Begin
- Indiana House Passes Bill to Continue Medicaid Coverage of Children’s Out-of-State Hospital Care
- Michigan Governor Proposes $210 Million to Increase Wages for Direct Care Workers in Fiscal 2024 Budget
- Minnesota Lawmakers Develop Proposal for MinnesotaCare Public Option
- Missouri Representative Proposes Higher Income Limit for Ticket to Work Medicaid Program
- Montana Lawmakers Consider Bill to Allow Physician Assistants to Practice Unsupervised
- New Mexico Awards MMIS Contract to Conduent
- New York Awards $658 Million in Grants to Expand Healthcare Access
- North Carolina House Committees Advance Bill to Expand Medicaid, Increase Hospital Reimbursements
- Tennessee Governor Proposes Expanding Medicaid Eligibility Limits for Pregnant Women, Caretakers
- Virginia to Release Medicaid Managed Care RFP in June 2023
- Virginia to Release Medicaid NEMT RFP in April 2023
- West Virginia Awards Medicaid Managed Care for Foster Care Youth Contract
- CMS Approves Programs to Provide Nutritional Supports for Medicaid Enrollees
- Consonance Capital Partners Acquires Embark Behavioral Health
- Wakely Summary of 2024 MA Advance Notice
In Focus
Mental Health and Addiction Crises Top the Federal Policy Agenda in 2023
This week our In Focus section reviews President Joseph R. Biden’s 2023 State of the Union Address (SOTU) to Congress. The President highlighted specific actions that Congress, and the Administration have taken over the last two years to advance his health care priorities.
During his first SOTU address in 2022, President Biden announced the creation of a “Unity Agenda”, which included priority policy areas with potential for bi-partisan support. The President highlighted several steps the Administration has taken to advance the “Unity Agenda” including:
- The bipartisan effort to enact the Mainstreaming Addiction Treatment (MAT) Act, which removed the federal requirement for practitioners to have a waiver (known as the X-waiver) to prescribe medications, like buprenorphine, for the treatment of opioid use disorder
- The Cancer Moonshot announcements for almost 30 new programs, policies, and resources to close the screening gap, tackle environmental exposure, decrease preventable cancers, advance cutting-edge research, support patients and caregivers, and more.
- Addressing mental health needs through the expansion of Certified Community Behavioral Health Clinics and launch of the 988-suicide prevention hotline.
In his SOTU and accompanying White House materials, the President also proposed new policies and initiatives to further advance his health care agenda. These actions include a combination of issues that would require Congressional approval as well as actions regulatory agencies can already advance. Congress and the Administration are expected to build on previous bipartisan achievements to tackle the nation’s dual crises with addiction and mental health.
Notably, the policies outlined in the SOTU foreshadow an active regulatory agenda over the next 18 months as the Administration seeks to solidify key aspects of the President’s health care agenda ahead of the next Presidential election.
The Administration’s planned actions include the following:
Opioids
- Calling on Congress to pass legislation to permanently schedule all illicitly produced fentanyl-related substances into Schedule I.
- SAMHSA will provide enhanced technical assistance to states who have existing State Opioid Response funds, and will host peer learning forums, national policy academies, and convenings with organizations distributing naloxone beginning this spring.
- By this summer, the Federal Bureau of Prisons will ensure that each of their 122 facilities are equipped and trained to provide in-house medication-assisted treatment (MAT).
- This spring CMS will provide guidance to states on the use of federal Medicaid funding to provide health care services—including treatment for people with substance use disorder—to individuals in state and local jails and prisons prior to their release. California is the first state to receive approval for a similar initiative.
Mental Health
- CDC plans to launch a new campaign to provide a hub of mental health and resiliency resources to health care organizations in better supporting their workforce.
- The Department of Education (ED) will announce more than $280 million in grants to increase the number of mental health care professionals in high-need districts and strengthen the school-based mental health profession pipeline.
- HHS and ED will issue guidance and propose a rule to make it easier for schools to provide health care to students and more easily bill Medicaid for these services.
- The Administration is scheduled to propose new mental health parity rules this spring.
- HHS will improve the capacity of the 988 Lifeline by investing in an expansion of the crisis care workforce; scaling mobile crisis intervention services; and developing additional guidance on best practices in crisis response.
- HHS also plans to promote interstate license reciprocity for delivery of mental health services across state lines.
- HHS intends to increase funding to recruit future mental health professionals from Historically Black Colleges and Universities and to expand the Minority Fellowship Program.
- The Department of Veterans Affairs (VA), working with HHS and Defense, will launch a program for states, territories, Tribes and Tribal organizations to develop and implement proposals to reduce suicides in the military and among veterans.
- VA will also increase the number of peer specialists working across VA medical centers to meet mental health needs
Cancer Moonshot
- The President called on Congress to reauthorize the National Cancer Act to overhaul cancer research and to extend the funding for biomedical research established in the 21st Century Cures Act.
- The Administration will take steps to ensure that patient navigation services are covered by insurance. This could require legislation depending on which type on insurance an individual has.
Health care costs
- Urging Congress to pass legislation to cap insulin prices in all health care markets. Expanding the $35 insulin cap to commercial markets will require the 60 votes in the Senate.
Home and community services
- Working with Congress to approve legislation to ensure seniors and people with disabilities can access home care services and to provide support to caregivers.
HMA and HMA companies are closely monitoring these federal policy developments. We can assist healthcare stakeholders in responding to the immediate opportunities and challenges that arise and contextualize these actions for longer-term strategic business and operational decisions.
If you have questions about these or other federal policy issues and how they will impact your organization please contact Andrea Maresca ([email protected]) or Liz Wroe ([email protected]).
Online Registration for HMA Quality Conference Ends February 21
Don’t forget to register for the HMA Quality Conference, A Deep Dive on What’s Next for Providers, Payers, and Policymakers: Focus on Quality to Improve Patients’ Lives, Monday, March 6, 2023, at the Fairmont Chicago, Millennium Park hotel. Online registration ends Tuesday, February 21. Walk-in registration will be available on-site.
Keynote speaker is Lee Fleisher, MD, Chief Medical Officer, Director, Center for Clinical Standards and Quality, Centers for Medicare and Medicaid Services. Featured speakers will include executives from American College of Surgeons, ANCOR, CareJourney, CareOregon, Commonwealth Care Alliance, Council on Quality and Leadership, Denver Health, Institute on Public Policy for People with Disabilities, Intermountain Health, NCQA, Reema Health, Kaiser Permanente, Social Interventions Research and Evaluation Network, UnitedHealth Group, United Hospital Fund, 3M, and others.
Attendees will learn about evolving healthcare quality initiatives and participate in substantive workshops where they will discuss solutions and quality frameworks being used to create a more equitable health system.
Visit the conference website for a complete agenda and Register Now
Sponsorships and group discounts are available. For additional information, contact Carl Mercurio, [email protected].
HMA Roundup
Alabama
Alabama Legislative Committee Puts Hold on Inmate Health Contract. AL.com reported on February 2, 2023, that the Alabama legislature’s contract review committee placed a temporary hold on the state’s $1.06 billion contract with YesCare/CHS AL for medical and mental health care services for incarcerated individuals in the state. The legislative committee continues to have questions about the procurement process. Read More
California
California Reaches $18.3 Million Settlement with Pharmacy in Medicaid Fraud Lawsuit. Mobi Health News reported on February 10, 2023, that The Pill Club, an online birth control pharmacy, agreed to pay $18.3 million to settle a Medicaid fraud lawsuit with California. The whistleblower complaint alleged that the pharmacy billed Medicaid for face-to-face counselling when providers did not have direct, real-time contact with patients, and that the pharmacy dispensed female contraceptives that were not requested. Read More
California Whole Person Care Program Saved $383 Per Person Per Year, UCLA Review Finds. The Associated Press reported on February 9, 2023, that the California Whole Person Care pilot program, which ran from 2016 through 2021, saved $383 per patient annually by reducing hospitalizations and emergency room visits, according to a review from the UCLA Center for Health Policy Research. The program was aimed at high-risk Medicaid beneficiaries, including individuals who are homeless, recently released from prison, suffering from multiple chronic health conditions, or struggling with addiction or other severe behavioral health needs. Read More
California Reaches $215 Million Settlement With PBM Over Pharmacy Charges. Kaiser Health News reported on February 8, 2023, that Centene has agreed to pay California more than $215 million to settle allegations that the company’s pharmacy benefit management operation overcharged the state. California is the 17th state to settle PBM litigation with Centene. Read More
Florida
Florida CHIP Enrollment Likely to Increase as Medicaid Redeterminations Begin. Florida Politics reported on February 13, 2023, that enrollment in Florida KidCare, the state Children’s Health Insurance Program (CHIP), will likely increase as the state begins disenrolling individuals from Medicaid, according to estimates from the state Office of Economic & Demographic Research. Specifically, enrollment in the Healthy Kids component, covering children age six to 20, is expected to increase by more than 22,000 starting in June; and enrollment in the Children’s Medical Services component covering medically complex individuals is expected increase in January. Read More
Florida Judge Dismisses Lawsuit Over Minimum Wage for Direct Care Employees. WLRN/News Service of Florida reported on February 7, 2023, that a Florida administrative law judge ruled that the state is not required to initiate a formal rule-making process to define which Medicaid providers are entitled to a $15 hourly minimum wage for providing “direct care.” The Florida Assisted Living Association and the Florida Ambulance Association filed a lawsuit against the state Agency for Health Care Administration claiming that language in the state budget mandating a minimum wage for direct care employees was not adequately defined. Read More
Hawaii
Hawaii Governor Proposes $45 Million to Increase Medicaid Reimbursement Rates Over Two Years. Hawaii Governor Josh Green, on February 13, 2023, asked state legislators for funds to increase Medicaid reimbursement rates to 100 percent of Medicare over two years. The cost would be $25 million in fiscal 2024 and $20 million in fiscal 2025. Green is also proposing $12.3 million to provide additional resources for mental health services and $5 million for a new facility for individuals with behavioral health issues. Read More
Idaho
Idaho Representative Proposes Legislation to Repeal Medicaid Expansion. Big Country News Connection reported on February 12, 2023, that Idaho Representative John Vander Woude (R-Nampa) introduced a bill to repeal Medicaid expansion, which would impact about 67,000 expansion members. Woude is chairman of the House Health and Welfare Committee.
Indiana
Indiana House Passes Bill to Continue Medicaid Coverage of Children’s Out-of-State Hospital Care. NWI Times reported on February 13, 2023, that the Indiana House of Representatives passed legislation allowing Medicaid to cover children’s out-of-state hospital care through June 30, 2025. The bill now moves to the state Senate. Read More
Michigan
Michigan Governor Proposes $210 Million to Increase Wages for Direct Care Workers in Fiscal 2024 Budget. Michigan Governor Gretchen Whitmer published on February 8, 2023, her fiscal 2024 budget proposal, which includes $210 million to increase wage support for direct care workers in nursing homes. She is also proposing almost $130 million for additional Medicaid health access and equity; $62 million to fund Healthy Moms, Healthy Babies; and $6.2 million to fund the Medicaid Plan First! Program to expand access to family planning services and cancer screening. Read More
Minnesota
Minnesota Lawmakers Develop Proposal for MinnesotaCare Public Option. The Associated Press reported on February 8, 2023, that Minnesota lawmakers are developing a public option proposal that would allow all state residents to buy into MinnesotaCare, the health insurance program for people who do not qualify for Medicaid. The current eligibility cutoff for MinnesotaCare is 200 percent of poverty. Read More
Missouri
Missouri Representative Proposes Higher Income Limit for Ticket to Work Medicaid Program. The Springfield News-Leader reported on February 15, 2023, that Missouri Representative Melanie Stinnett (R-Springfield) is proposing a bill (House Bill 970) that would raise the income limit for the state’s Ticket to Work Health Assurance Program, which provides Medicaid coverage to employed individuals with disabilities. Read More
Montana
Montana Lawmakers Consider Bill to Allow Physician Assistants to Practice Unsupervised. Kaiser Health News reported on February 10, 2023, that Montana lawmakers are considering a bill (House Bill 313) that would allow physician assistants to practice without physician supervision and without a supervision agreement. The bill is intended to help with the current health care provider shortage. More than 750 physician assistants practice in the state, with almost 96 percent working in rural areas. Read More
New Mexico
New Mexico Awards MMIS Contract to Conduent. Conduent announced on February 14, 2023, that it was selected by the New Mexico Human Services Department for a modular, cloud-based Medicaid Management Information System (MMIS), including data exchange and reporting, pharmacy benefit management, and self-directed home and community-based services. The Conduent system will replace the state’s current MMIS. Read More
New Mexico Behavioral Health Plan Must Face Whistleblower Lawsuit, Judge Rules. Bloomberg Law reported on February 9, 2023, that a U.S. District Court Judge ruled that a whistleblower lawsuit brought by La Frontera Center against United Behavioral Health should not be dismissed. The lawsuit alleges that United unlawfully failed to return Medicaid payments it was not entitled to receive. Read More
New York
New York Awards $658 Million in Grants to Expand Healthcare Access. New York State Governor Kathy Hochul announced on February 15, 2023, the award of $658 million in grants across 127 projects statewide through the Statewide Health Care Facility Transformation Program. The aim of the program is to reduce health care costs and improve outcomes by expanding access to inpatient, primary, preventive, and other ambulatory care. The program has awarded $1.68 billion in funding thus far and will award an additional $1.15 billion through future funding rounds. Read More
New York Lawmakers to Introduce Single Payer, Universal Health Care Bill. Spectrum News reported on February 9, 2023, that New York lawmakers are negotiating with unions in hopes of introducing a universal health care bill in the next few weeks. The bill, which has been in the works for a few years, would replace health plans in the state with single-payer coverage. Read More
North Carolina
North Carolina House Committees Advance Bill to Expand Medicaid, Increase Hospital Reimbursements. The Center Square reported on February 14, 2023, that the North Carolina House Health and Finance Committees advanced legislation to expand Medicaid coverage to roughly 500,000 adults. The bill would also develop a Healthcare Access and Stabilization program, which increases reimbursements for acute care hospitals through hospital assessments. Read More
North Carolina Failed to Collect $3.1 Million in Drug Manufacturer Rebates, OIG Audit Finds. The Center Square reported on February 14, 2023, that North Carolina failed to invoice for and collect $3.1 million in drug manufacturer rebates from 2016 through 2019, according to an audit report from the U.S. Office of the Inspector General (OIG). The audit found that internal controls at the North Carolina Department of Health and Human Services did not ensure manufacturers were invoiced and that the state claimed improper reimbursements for certain drugs. Read More
North Carolina House Republicans Introduce Medicaid Expansion Bill. WRAL reported on February 8, 2023, that North Carolina House Republicans introduced a Medicaid expansion bill. A prior attempt to pass Medicaid expansion legislation stalled when the House and Senate could not reconcile differences in their respective bills. Read More
Pennsylvania
Pennsylvania Health Plan to Offer CHIP Coverage Statewide. Geisinger announced on February 13, 2023, that it will offer Pennsylvania Children’s Health Insurance Program (CHIP) coverage statewide, effective immediately. Coverage for medical, dental, vision, and pharmacy services is available to all uninsured children up to age 19 regardless of household income. Read More
Tennessee
Tennessee Governor Proposes Expanding Medicaid Eligibility Limits for Pregnant Women, Caretakers. The Chattanooga Times Free Press reported on February 9, 2023, that Tennessee Governor Bill Lee’s fiscal 2024 proposed budget calls for increasing the Medicaid income eligibility limit to 250 percent of poverty for pregnant individuals and to 100 percent of poverty for parents and caretakers. The expansion would extend coverage to 25,000 people. Lee also proposed allocating funds to provide dental coverage to adult Medicaid enrollees and to support individuals with intellectual and developmental disabilities. Read More
Virginia
Virginia to Release Medicaid Managed Care RFP in June 2023. The Virginia Department of Medical Assistance Services announced on February 14, 2023, plans to release a request for proposals (RFP) for its Medicaid managed care program on June 1, 2023. The state’s Medicaid managed care program, known as Medallion 4.0, and Children’s Health Insurance Program, known as FAMIS, serve over 1.6 million lives. Incumbents are Aetna, Anthem, Molina, Sentara Healthcare/Optima/Virginia Premier, and UnitedHealthcare. Read More
Virginia to Release Medicaid NEMT RFP in April 2023. The Virginia Department of Medical Assistance Services announced on February 14, 2023, plans to release a request for proposals (RFP) for its Medicaid non-emergency medical transportation (NEMT) program on April 30, 2023. Read More
West Virginia
West Virginia Awards Medicaid Managed Care for Foster Care Youth Contract. Aetna Better Health of West Virginia announced on February 7, 2023, that it was again awarded the contract for the West Virginia Mountain Health Promise Medicaid managed care program, covering physical and behavioral health services for roughly 30,000 children and youth in the foster care system. Aetna has been the incumbent since 2020. The contract will run from July 1, 2023, through June 30, 2024, with three one-year renewal options. The program also serves youth up to age 26 who aged out of foster care while on Medicaid and eligible children in the serious emotional disorders waiver program. Read More
Wyoming
Wyoming House Passes Medicaid Postpartum Coverage Extension Bill. The Wyoming Tribune Eagle reported on February 8, 2023, that the Wyoming House passed legislation to extend Medicaid postpartum coverage from two months to one year through 2027. The Senate will consider the bill next. Read More
National
CMS Reports on Early Outcomes of Substance Use Disorder Demonstrations. The Centers for Medicare & Medicaid Services (CMS) released on February 15, 2023, four rapid cycle reports, which provide insight into the implementation and early outcomes of Section 1115 Substance Use Disorder (SUD) demonstrations. One report looked at features of state approaches to improve Medicaid SUD treatment delivery systems and found that more than 75 percent of demonstration states added or expanded coverage of at least one SUD benefit category. Another looked at implementation challenges and found that one of the most common operational challenges was lack of provider knowledge about Medicaid structure, billing, and operational requirements. Read More
U.S. Representative Proposes Legislation to Eliminate Federal Medicaid Funding Cap for Territories. Marianas Variety reported on February 15, 2023, that Representative Gregorio Kilili Camacho Sablan (D-Northern Mariana Islands) and 18 co-sponsors introduced legislation to eliminate the cap on federal Medicaid funding for U.S. territories. The bill has been referred to the U.S. House Committee on Energy and Commerce. Read More
CMS to Test 3 New Models Aimed at Lowering Prescription Drug Prices. The Centers for Medicare & Medicaid Services (CMS) announced on February 14, 2023, that it will test three new models aimed at reducing Medicare drug costs: Medicare $2 Drug List, Cell and Gene Therapy Access Model, and Accelerating Clinical Evidence Model. Read More
Community Health Plans Experience Challenges in Reaching Medicaid Beneficiaries, Survey Shows. Health Payer Intelligence reported on February 14, 2023, that 90 percent of Association for Community Affiliated Plans (ACAP) have experienced challenges in reaching Medicaid members, according to a Kaiser Family Foundation (KFF) brief. Lack of up-to-date beneficiary contract information could impact eligibility redeterminations. The brief was based on survey responses from 29 community plans and a roundtable discussion. Read More
CMS Proposes Rule to Disclose Private Equity, REIT Ownership of Nursing Homes. Modern Healthcare reported on February 13, 2023, that the Centers for Medicare & Medicaid Services (CMS) proposed a rule requiring nursing homes to disclose if they are owned or operated by private equity firms or real estate investment trusts (REITs). Public comments on the rule will be accepted through April 14. Read More
DOJ Recovered $1.7 Billion from False Health Care Claims Cases in Fiscal 2022. Benefits Pro reported on February 13, 2023, that the U.S. Department of Justice (DOJ) recovered more than $1.7 billion from false health care claims cases in fiscal 2022. The total is for federal funds only. Cases involve Medicaid, unnecessary services and substandard care, Medicare Advantage, drug pricing, and kickbacks. Read More
Exchanges Plans Denied 17 Percent of In-Network Claims in 2021. Health Payer Intelligence reported on February 13, 2023, that non-group Exchange plans denied nearly 17 percent of 296 million in-network claims in 2021, according to a Kaiser Family Foundation analysis. Reasons for in-network claims denials included uncovered services, lack of prior authorization, and medical necessity. Read More
Federal Judge Bars Disenrollment of Medicaid Members Eligible for Medicare Savings Program. Connecticut Insider reported on February 13, 2023, that a federal judge in Connecticut ordered the U.S. Department of Health and Human Services (HHS) to reverse a November 2020 rule that allowed the disenrollment of Medicaid members eligible for the Medicare Savings Program. A federal judge had previously issued a temporary injunction. Read More
Medicare Plans, CMS Differ Over Impact of 2024 Advance Notice on Rates. Fierce Healthcare reported on February 13, 2023, that health plans and federal regulators differ over the likely impact of the 2024 Advance Notice, which outlines proposed changes in Medicare Advantage and Part D payments. While insurance industry group AHIP argues that the rule will cut Medicare Advantage rates by 2.3 percent, the Centers for Medicare & Medicaid Services (CMS) projects a one percent net increase. Read More
CMS Approves Programs to Provide Nutritional Supports for Medicaid Enrollees. The Wall Street Journal reported on February 12, 2023, that the Centers for Medicare & Medicaid Services (CMS) has approved waiver demonstrations that allow Medicaid funding to be spent on groceries and nutritional counseling programs. Programs in Arkansas, Massachusetts, and Oregon have been approved thus far. Read More
U.S. Senate Considers Bill to Increase Medicaid Funding for HCBS. NorthcentralPA reported on January 28, 2023, that the U.S. Senate is considering a bill that would increase Medicaid funding for home and community-based services (HCBS). The Better Care, Better Jobs Act, introduced by Senator Bob Casey (D-PA), would give states a permanent 10 percent increase in federal Medicaid matching funds for HCBS, subject to certain requirements like strengthening HCBS access and expanding the HCBS workforce. More than 650,000 individuals are on waiting lists to receive HCBS, according to the Senate Special Committee on Aging. Read More
Industry News
AHIP Expresses Concerns Over Medicare Advantage Proposed Rule. America’s Health Insurance Plans (AHIP) announced on February 14, 2023, that it submitted comments to the Centers for Medicare & Medicaid Services (CMS), warning that proposed Medicare Advantage and Part D rules would bring “new uncertainties and risk” to the programs. Read More
Cigna Becomes The Cigna Group, Launches Separate Segments for Healthcare, Pharmacy Services. Becker’s Payer Issues reported on February 13, 2023, that Cigna is rebranding itself as The Cigna Group. The company is branding its health benefits segment Cigna Healthcare and its pharmacy segment Evernorth Health Services (which will house Express Scripts, Express Scripts Pharmacy, Accredo, eviCore, MDLIVE, and myMatrixx). Read More
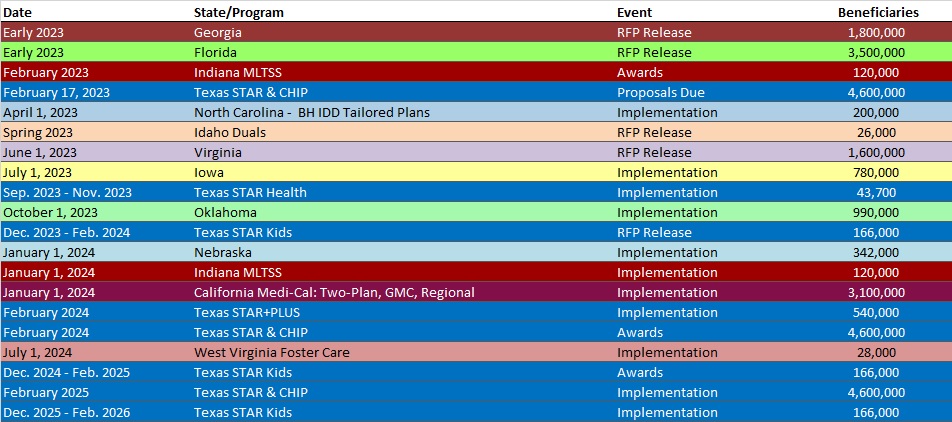
RFP Calendar
HMA News & Events
WAKELY, AN HMA COMPANY, WHITE PAPERS