This week's roundup:
- In Focus: CMS Proposes Significant Changes to Medicare Advantage and Medicare Prescription Drug Benefit Programs for 2025
- HMA Report Shows First-of-Its-Kind Actual Comparisons of State-by-State Medicaid Disenrollments vs. Projections
- Medicaid Eligibility Redeterminations News: Arkansas, Idaho, Florida, Iowa, Kentucky, Maine, Maryland, Mississippi, Nevada, Texas, Washington
- Idaho Legislative Task Force Agrees State Should Stick with Medicaid Value Care Organizations
- Indiana Submits 1915c Waiver Request to Transition Medicaid LTSS to Managed Care
- Iowa to Award Medicaid Dental Services Contracts to Delta Dental of Iowa, DentaQuest USA
- CareSource Names Chad Moore Kansas Market President
- Missouri Extends Medicaid Postpartum Coverage to 12 Months
- South Dakota Enrolls Less than 20 Percent of Eligible Medicaid Expansion Population
- Tennessee Releases RFP for TennCare Select Prepaid Inpatient Health Plan for Children
- States Expect Medicaid Enrollment Decrease, Spending Increase in Fiscal 2024, KFF Medicaid Director Survey Finds
- Fourteen Insurers to Exit Medicare Advantage Markets in 2024, KFF Data Show
- Centene Names Susan Smith as Chief Operating Officer
The next HMA Weekly Roundup will be November 29, 2023.
In Focus
CMS Proposes Significant Changes to Medicare Advantage and Medicare Prescription Drug Benefit Programs for 2025
This week, our In Focus section reviews a wide-ranging proposed rule issued by the Centers for Medicare & Medicaid Services (CMS) on November 6, 2023. The rule would update various policies governing Medicare Advantage (MA, or Part C), the Medicare Prescription Drug Benefit (Part D), Medicare cost plans and Programs of All-Inclusive Care for the Elderly. These proposed policy reforms would implement changes related to Star Ratings, marketing and communications, agent/broker compensation, health equity, dual eligible special needs plans (D-SNPs), utilization management, network adequacy, and other programmatic areas. The proposals reflect the agency’s continuing focus on increasing program transparency, improving health equity, reducing the cost of care for Medicare beneficiaries, and expanding access to behavioral health services.
MA and Part D stakeholders are encouraged to provide CMS with feedback and analysis regarding the potential impact of these changes. Comments on the proposed rule are due by January 5, 2024. The final rule would take effect in contract year 2025.
Improving Access to Behavioral Health Care Providers
CMS proposes regulatory changes intended to improve access to behavioral healthcare by adding certain provider specialties to the MA network adequacy standards as follows.
- CMS proposes to add a new facility-specialty type to the existing list of facility-specialty types evaluated as part of its plan network adequacy reviews. The new facility-specialty type, outpatient behavioral health, would be included in network adequacy evaluations, including marriage and family therapists (MFTs), mental health counselors (MHCs), opioid treatment programs, community mental health centers, and/or other behavioral health and addiction medicine specialists and facilities.
- MFTs and MHCs will be eligible to enroll in Medicare and start billing for services beginning January 1, 2024, because of the new statutory benefit category established in the Consolidated Appropriations Act (CAA) of 2023. CMS proposes to make corresponding changes to its network adequacy requirements for MA organizations.
- For purposes of the network adequacy requirements, the new facility-specialty type would be evaluated using time and distance and minimum number standards in the proposed regulation.
Increased Transparency for Special Supplemental Benefits for the Chronically Ill
In 2018, Congress enacted new authorities pertaining to supplemental benefits for MA members with chronic health conditions. CMS refers to this category of benefits as Special Supplemental Benefits for the Chronically Ill (SSBCI). These services are available only to enrollees with ongoing conditions and who meet certain criteria established in the statute. In contrast to the general policy that MA benefits should be offered uniformly to all plan members, MA plans may offer SSBCI tailored to a qualifying individual’s specific medical diagnosis and needs.
Supplemental benefits, including SSBCI, are generally funded with MA plan rebate dollars. CMS notes that the number of MA plans that offer SSBCI—and the number and scope of SSBCI that individual plans provide—has increased since their introduction in 2019.
Under the proposed rule:
- MA organizations would be required to demonstrate, through relevant and acceptable evidence, that an item or service offered as SSBCI has a reasonable likelihood of improving or maintaining the health or overall function of chronically ill beneficiaries. MA plans also must, by the date on which they submit a bid to CMS, include a bibliography of evidence supporting this position. According to CMS, this expectation would shift the burden of proof from the agency to MA organizations, requiring plans to demonstrate compliance with this standard and that SSBCI items and services are evidence-based.
- MA plans must follow their written policies based on objective criteria for determining enrollee eligibility for SSBCI when making determinations.
- Require that MA plans document denials of SSBCI eligibility rather than its approvals.
- CMS would codify its authority to review and deny approval of an MA organization’s bid if the plan cannot demonstrate, through relevant and acceptable evidence, that its proposed SSBCI has a reasonable expectation of improving or maintaining the health or overall function of a chronically ill enrollee.
- CMS also would codify its authority to review SSBCI offerings annually for compliance and in light of the available evidence.
According to CMS, these proposals, if implemented, would better ensure that the benefits offered as SSBCI are reasonably expected to positively affect the health and well-being of chronically ill beneficiaries and guard against the use of MA rebate dollars for SSBCI that unsubstantiated.
In addition, CMS is proposing new policies to improve transparency regarding SSBCI so that beneficiaries are aware that SSBCI are only available to enrollees who meet the eligibility criteria. More specifically, CMS proposes to:
- Modify the current requirements for the SSBCI disclaimer that MA organizations must use whenever SSBCI are mentioned. The SSBCI disclaimer would have to list the relevant chronic condition(s) that qualify for the benefits that MA organizations offer.
- Establish specific font and reading pace parameters for the SSBCI disclaimer in print, television, online, social media, radio, other voice-based ads, and outdoor advertising, including billboards. Finally, it would clarify that MA organizations must include the disclaimer in all marketing and communications materials that mention SSBCI.
Requiring Mid-Year Enrollee Notification of Available Supplemental Benefits
As noted previously, over the past several years, the number of MA plans offering supplemental benefits has increased. The benefits offered are broader in scope and variety, and an increasing amount of MA rebate dollars are being directed toward these benefits. At the same time, plans have reported that the number of enrollees who use many of these benefits is low.
- CMS proposes requiring MA plans to notify enrollees mid-year of the unused supplemental benefits available to them. The notice would list any supplemental benefits that a beneficiary does not use during the first six months of the year (January 1−June 30).
- At present, MA plans are not required to send any communication specific to an enrollee’s usage of supplemental benefits. This policy is intended to educate enrollees on their access to supplemental benefits and encourage greater use of these benefits.
Enhancing “Guardrails” for Agent and Broker Compensation
For many years, CMS has set upper limits on the compensation that agents and brokers can receive for enrolling Medicare beneficiaries in MA and Part D plans. CMS believes that many MA and prescription drug payment plans, as well as third-party entities with which they contract, make structured payments to agents and brokers that circumvent these compensation caps.
- In this regulation, CMS proposes to generally prohibit contract terms between MA organizations and agents, brokers, or other third party marketing organizations (TPMOs) that may interfere with the agent’s or broker’s ability to objectively assess and recommend the plan that best-suited to a beneficiary’s healthcare needs; to set a single reimbursement rate for all plans; to revise the scope of items and services included within agent and broker compensation; and to eliminate the regulatory framework that currently allows for separate payment to agents and brokers for administrative services.
- The agency would make conforming changes to the Part D agent broker compensation rules.
Requiring an Annual Health Equity Analysis of Utilization Management Policies and Procedures
CMS proposes several regulatory changes to the composition and responsibilities of an MA organization’s utilization management (UM) committee.
- The new rules would require that a member of the UM committee have expertise in health equity and that the UM committee conduct an annual health equity analysis of the use of prior authorization.
- The proposed analysis would examine the impact of prior authorization on enrollees with one or both of the following social risk factors (SRFs): receipt of the low-income subsidy, dual eligibility for Medicare and Medicaid (LIS/DE), or a disability.
- The proposed analysis must compare metrics related to the use of prior authorization for enrollees with the specified SRFs with enrollees without the specified SRFs. The results of the analysis must be made publicly available on the MA organization’s website in an easily accessed manner.
Enhancing Enrollees’ Right to Appeal an MA Plan’s Decision to Terminate Coverage for Non-Hospital Provider Services
Beneficiaries enrolled in traditional Medicare and MA plans have the right to a fast-track appeal by an independent review entity (IRE) when their covered skilled nursing facility (SNF), home health agency (HHA), or comprehensive outpatient rehabilitation facility (CORF) services are being terminated. At present, quality improvement organizations (QIOs) function as IREs and conduct these reviews.
Furthermore, MA enrollees do not have the same access to QIO review of a fast-track appeal as traditional Medicare beneficiaries.
CMS proposes to:
- Require that QIOs, instead of MA plans, review untimely fast-track appeals of an MA plan’s decision to terminate HHA, CORF, or SNF services
- Fully eliminate the provision requiring the forfeiture of an enrollee’s right to appeal a termination of services decision when they leave the facility
According to CMS, these proposals would align MA regulations with the parallel reviews available to beneficiaries in traditional Medicare and expand the rights of MA beneficiaries to access the fast-track appeals process.
Increasing the Percentage of Dually Eligible Managed Care Enrollees Who Receive Medicare and Medicaid Services from the Same Organization
In the proposed rule, CMS expresses concern that a significant number of dually eligible enrollees receive Medicare services through one managed care entity and Medicaid services through another (misaligned enrollment), rather than from one organization (aligned enrollment. The proposed rule states that in the long run, “for dually eligible individuals who are in Medicare and Medicaid managed care, we believe that we should continue to drive toward increasing aligned enrollment until it is the normative, if not only, managed care enrollment scenario…. For dually eligible individuals that elect MA plans, we are focused on increasing enrollment in integrated D-SNPs: fully integrated dual eligible special needs plans (FIDE SNPs), highly integrated dual eligible special needs plans (HIDE SNPs), and applicable integrated plans (AIPs) [pages 286-287].”
To move in this direction, CMS offers several interconnected proposals as follows:
- Replace the current quarterly special enrollment period (SEP) with a monthly SEP for dually eligible individuals and others enrolled in the Part D low-income subsidy program to elect a standalone PDP
- Create a new integrated care SEP to allow dually eligible individuals to elect an integrated D-SNP on a monthly basis
- Limit enrollment in certain D-SNPs to individuals who are also enrolled in an affiliated Medicaid managed care organization (MCO)
- Limit the number of D-SNP plan benefit packages an MA organization, its parent organization, or an entity that shares a parent company with the MA organization, can offer in the same service area as an affiliated Medicaid MCO
According to CMS, these initiatives would increase the percentage of dually eligible MA enrollees who are in plans that are also contracted to cover Medicaid benefits, thereby expanding access to integrated materials, unified appeal processes across Medicare and Medicaid, and continued Medicare services during an appeal.
Impose New Contracting Standards for Dual Eligible Special Needs Plan (D-SNP) Look-Alikes
Under existing regulations, CMS does not contract with and will not renew the contract of a D-SNP look-alike; that is, an MA plan that is not a SNP but in which dually eligible enrollees account for 80 percent or more of total enrollment. CMS proposes to lower the D-SNP look-alike threshold from 80 percent to 70 percent in 2025 and to 60 percent in 2026. CMS states that this proposal is intended to help address the continued proliferation of MA plans that serve high percentages of dually eligible individuals without meeting D-SNP requirements.
Other Topics in the Proposed Rule
In addition, the proposed rule calls for:
- Providing greater flexibility for Part D plan sponsors to substitute biosimilar products during the plan year
- Limiting out-of-network cost sharing for D-SNP PPOs
- Standardizing the MA risk adjustment data validation appeals process
- Expanding permissible data use and data disclosure for MA encounter data including for support for Medicaid and state Medicaid agencies to better coordinate care for dually eligible individuals
The Health Management Associates Medicare team will continue to analyze these proposed changes. We have the depth and breadth of expertise to assist with tailored analysis, to model policy impacts, and to support the drafting of comment letters to this rule. For more information or questions about the policies described, contact Amy Bassano ([email protected]), Julie Faulhaber ([email protected]), Andrea Maresca ([email protected]), or John Richardson ([email protected]).
HMA Report Shows First-of-Its-Kind Actual Comparisons of State-by-State Medicaid Disenrollments vs. Projections
Health Management Associates (HMA) released on November 13, 2023, a report showing actual state-by-state Medicaid beneficiary disenrollment figures to date, compared to state-by-state modeled projections made earlier this summer. The report was authored by multiple HMA colleagues along with Katherine Hempstead from the Robert Wood Johnson Foundation. States have 14 months starting no later than March 2023 to complete Medicaid eligibility redeterminations. Updated data and projections from the HMA model will be available in December. Read More
HMA Roundup
Arizona
Arizona Seeks Public Comment on Proposed Merger of Centene Medicaid Plans. The Arizona Health Care Cost Containment System (AHCCCS) announced on November 9, 2023, that it is seeking public comment on a proposed merger of two Centene Medicaid plans. Under the arrangement, Centene would transition the 80,626 members enrolled in its Care1st Health Plan of Arizona to its Arizona Complete Health-Complete Care Plan, which serves 372,445 acute members and individuals with serious mental illness (SMI). Public comments will be accepted through December 7. Read More
Arkansas
Arkansas DHS Announces Changes to Executive Leadership Structure. The Arkansas Department of Human Services (DHS) announced on November 14, 2023, several changes to its executive leadership structure. Effective today, Janet Mann will serve as deputy secretary for programs, Melissa Weatherton will serve as director of specialty Medicaid services under Mann, and Misty Eubanks will serve as deputy secretary for operations and budget. DHS is expected to name an interim chief financial officer (Eubanks’s prior position) and an interim director for the Division of Developmental Disabilities Services (Weatherton’s prior position) at a later date. Mann was previously deputy secretary for health. Read More
Arkansas Disenrolls 5,734 Medicaid Beneficiaries During October Redeterminations. The Arkansas Department of Health has disenrolled 5,734 Medicaid beneficiaries during October redeterminations, including 4,470 for procedural reasons. The state has renewed coverage for 38,547 beneficiaries.
Florida
Florida Dispute Over Moving Children With Complex Conditions Out of Nursing Homes Continues As DOJ Files Brief. Health News Florida reported on November 14, 2023, that the U.S. Department of Justice (DOJ) filed a brief in support of a federal judge’s July ruling that Florida should allow children with complex medical needs to reside in their homes or communities rather than in nursing homes. Florida is challenging the July ruling, arguing that the level of support needed to allow children to stay in their homes or their communities is not feasible for the state’s Medicaid program. A Miami appeals court is anticipated to hear arguments regarding the dispute during the week of January 22, 2024. Read More
Senate Holds Healthcare Workshop Ahead of 2024 Legislative Session. WLRN reported on November 13, 2023, that Florida Senate President Kathleen Passidomo (R-Naples) released a memo informing senators that the Florida Senate Policy Committee, chaired by Senator Colleen Burton (R-Lakeland), will hold a workshop this week to begin drafting legislation aimed at addressing significant challenges to the state’s healthcare system. Topics include increasing access to care, addressing healthcare workforce shortages, and promoting innovation expanded use of telehealth. The Florida legislative session begins January 9, 2024. Read More
Florida Disenrolls Approximately 260,000 Children Since Medicaid Redeterminations Began. Health News Florida reported on November 14, 2023, that the Florida Department of Children & Families has disenrolled approximately 260,000 children since Medicaid eligibility redeterminations began in April. About 25,000 of the children have enrolled in Florida’s children’s health care program. Read More
Idaho
Idaho Legislative Task Force Agrees State Should Stick with Medicaid Value Care Organizations. The Idaho Press reported on November 9, 2023, that most members of an Idaho legislative task force agree that the state should stick with its Medicaid value care organization (VCO) program, rather than transition to a comprehensive Medicaid managed care system using managed care organizations (MCOs). The Idaho Medicaid Managed Care Task Force, which was somewhat divided on whether to shift to Medicaid MCOs, instead recommended increasing the role of legislators in overseeing the state’s 11 VCOs. Read More
Idaho Submits Section 1115 Behavioral Health Waiver Amendment to Reimburse Spouses, Parents for Care Provision. The Centers for Medicare & Medicaid Services announced on November 8, 2023, that Idaho has submitted a request to amend its Behavioral Health Transformation Medicaid Section 1115 waiver to reimburse spouses and parents of minor children for providing personal care services to eligible individuals. The federal comment period will be open through December 8. Read More
Division of Medicaid to Request More Than $5 Million to Bolster Staffing. The Moscow-Pullman Daily News reported on November 15, 2023, that the Idaho Division of Medicaid plans to request more than $5 million in fiscal 2025 to fill 62 new positions focused on supporting rate setting, policy, contract management and outcomes measurement. The budget request, which would include state and federal funds, is in response to recent recommendations from the state’s Medicaid Managed Care Taskforce. Total budget request for the Division of Medicaid is expected to be $5.5 billion. Read More
Idaho Reenrolls 13,000 Medicaid Beneficiaries. The Idaho Capital Sun reported on November 15, 2023, that approximately 13,000 of the 121,000 individuals disenrolled from Idaho’s Medicaid program were reenrolled between April and August 2023. The state reported that more than half of the disenrolled individuals (77,000) were removed for procedural reasons. More than 30 percent of individuals leaving Medicaid had enrolled in an Exchange plan as of late September. Read More
Indiana
Indiana Submits 1915c Waiver Request to Transition Medicaid LTSS to Managed Care. WFYI reported on November 10, 2023, that the Indiana Family and Social Services Administration (FSSA) is seeking public comments on a proposed waiver to transition Medicaid long-term services and supports (MLTSS) to managed care. The PathWays for Aging waiver program would enroll individuals aged 60 and older who are currently served by the state’s Aged and Disabled Waiver. FSSA will also hold online sessions to discuss proposed changes to four of the state’s other home and community-based services waivers: Family Supports Waiver, Community Integration and Habilitation waiver, Traumatic Brain Injury waiver, and Aged and Disabled (which will be renamed Health and Wellness). Read More
Iowa
Iowa to Award Medicaid Dental Services Contracts to Delta Dental of Iowa, DentaQuest USA. The Iowa Department of Health and Human Services (HHS) announced on November 13, 2023, its intent to award Medicaid managed dental contracts to Delta Dental of Iowa and DentaQuest USA. Incumbents are Delta Dental and MCNA Dental. The contracts, which are set to begin July 1, 2024, cover the Iowa Dental Wellness Plan and Healthy and Well Kids in Iowa (Hawki).
Iowa Disenrolls 5,523 Medicaid Beneficiaries During October Redeterminations. The Iowa Department of Health and Human Services has disenrolled 5,523 Medicaid beneficiaries during October redeterminations, including 1,045 for procedural reasons. The state has renewed coverage for 40,885 beneficiaries.
Kansas
CareSource Names Chad Moore Kansas Market President. CareSource announced on November 9, 2023, that Chad Moore has been named Kansas market president, where the company is bidding on a state Medicaid managed care contract through its CareSource HealthAlliance. Proposals for the procurement are due January 4, 2024. Moore was previously vice president of network development at CareSource. Read More
Kentucky
Kentucky Disenrolls 12,613 Medicaid Beneficiaries During October Redeterminations. The Kentucky Department of Public Health disenrolled 12,613 Medicaid beneficiaries during October redeterminations, including 69 for procedural reasons. The state has renewed coverage for 89,854 beneficiaries.
Maine
Maine Disenrolls 15,778 Medicaid Beneficiaries From May Through October Following Eligibility Redeterminations. The Maine Department of Health and Human Services (DHHS) on November 9, 2023, reported the disenrollment of 15,778 Medicaid members from May through October, 2023, following eligibility redeterminations, including 4,797 for procedural reasons. The other 11,000 individuals were referred to the Exchange. The state renewed Medicaid eligibility for 138,008 individuals. Read More
Maryland
Maryland Disenrolls 8,195 Medicaid Beneficiaries Following October Redeterminations. Maryland Matters reported on November 14, 2023, that that the Maryland Department of Health disenrolled approximately 8,200 Medicaid beneficiaries in October, the lowest number since the state restarted eligibility redeterminations in April. The figure does not include procedural disenrollments, which have been paused until November pending changes to the state’s ex parte renewal system. Read More
Maryland Seeks Waiver Amendment to Speed Medicaid Eligibility Redeterminations, Extend Four Walls Exemption. The Centers for Medicare & Medicaid Services (CMS) announced on November 9, 2023, that Maryland is seeking federal approval of an amendment to its Maryland Health Choice Section 1115 demonstration to allow use of Supplemental Nutrition Assistance Program data to speed Medicaid eligibility redeterminations. The amendment would also continue the state’s exemption from the “Four Walls” requirement, thereby permitting reimbursement of telehealth services at the standard rate. The federal public comment period is open through December 9, 2023. Read More
Mississippi
Mississippi Disenrolls 8,674 Medicaid Beneficiaries During October Redeterminations. The Mississippi State Department of Health has disenrolled 8,674 Medicaid beneficiaries during October redeterminations, including 6,152 for procedural reasons. The state has renewed coverage for 30,403 beneficiaries.
Missouri
Missouri Extends Medicaid Postpartum Coverage to 12 Months. The Centers for Medicare & Medicaid Services announced on November 14, 2023, approval of Missouri’s plan to extend postpartum Medicaid and Children’s Health Insurance Program (CHIP) coverage to 12 months. Up to 18,000 additional Missourians will now be eligible for Medicaid postpartum coverage for a full year. Missouri is the 40th state to be approved for the extended coverage. Read More
Nevada
Nevada to Resume Procedural Medicaid Disenrollments in January. The Nevada Current reported on November 12, 2023, that Nevada will resume procedural terminations in January 2024 for Medicaid beneficiaries with a November renewal date. Nevada had previously paused procedural disenrollments and reinstated coverage for 114,000 Nevadans who had been potentially incorrectly disenrolled for procedural reasons. Those individuals will be enrolled for another 12 months. Read More
New Jersey
New Jersey Releases Coordinated Specialty Care, Community Integration Program RFP. The New Jersey Department of Health Services released on November 8, 2023, a request for proposals (RFP) to implement Coordinated Specialty Care (CSC) and Community Integration (CI) programs for individuals with early serious mental illness (ESMI), funded by the Substance Abuse and Mental Health Services Administration’s (SAMHSA) Community Mental Health Block Grant. The state will award contracts to six provider agencies, with each agency implementing both a CSC program (for individuals aged 15 to 35) and a combined CSC-CI program (for individuals aged 15 and older). Responses are due December 13, and awards will be announced February 8, 2024. Contracts will begin March 15, 2024, and expire September 30, 2025, with the option to renew for an additional three years. Read More
New York
New York Fines Medicaid Managed Care Plans $2.6 Million for Failing to Cover Behavioral Health Services. New York Governor Kathy Hochul announced on November 9, 2023, that five of the state’s Medicaid managed care health plans were fined more than $2.6 million after a review found they inappropriately denied claims or failed to pay for specialty behavioral health services at the rates required by law. The companies penalized are Affinity Health Plan, Amida Care, EmblemHealth, MetroPlus HealthPlan, and MVP HealthPlan. Read More
Oregon
Oregon Seeks Public Feedback on Proposed CareOregon, SCAN Group Merger. The Lund Report reported on November 14, 2023, that the Oregon Health Authority is seeking additional public feedback on the proposed merger involving Portland-based, not-for-profit Medicaid coordinated care organization CareOregon and California-based, not-for-profit Medicare plan SCAN Group. The deal would involve CareOregon and SCAN becoming arms of a new not-for-profit entity called HealthRight. CareOregon serves 500,000 Medicaid members. Read More
South Dakota
South Dakota Enrolls Less than 20 Percent of Eligible Medicaid Expansion Population. South Dakota Public Broadcasting reported on November 14, 2023, that South Dakota has enrolled just 10,000 or 20 percent of eligible Medicaid expansion individuals since rolling out the program three months ago, drawing criticism from state legislators during an interim budget hearing. The state Department of Social Services expects expansion enrollment to reach up to 57,000 over two years. Read More
Tennessee
Tennessee Releases RFP for TennCare Select Prepaid Inpatient Health Plan for Children. The Tennessee Department of Finance and Administration released on November 6, 2023, a request for proposals (RFP) for the state’s TennCare Select Prepaid Inpatient Health Plan (PIHP) program for approximately 52,000 children who receive Supplemental Security Income assistance or long-term services and supports or who live in areas with limited provider access. The incumbent is Blue Cross Blue Shield of Tennessee. Responses are due February 13, 2024, and notification of intent to award is scheduled for May 14, 2024. The contract, which will go into effect July 1, 2025, is for three years with up to seven one-year renewal options. Read More
Texas
Texas Disenrolls Nearly 1.3 Million Medicaid Beneficiaries Following Redeterminations from April Through October. The Texas Department of Health and Human Services announced the disenrollment of 1.25 million Medicaid beneficiaries following eligibility redeterminations from April through October 2023, including 817,067 for procedural reasons. The state has renewed coverage for 748,866 beneficiaries and referred 432,996 individuals to the federal Exchange. Read More
Washington
Washington Disenrolls 50,142 Medicaid Beneficiaries During September Redeterminations. The Washington State Health Care Authority announced on October 10, 2023, the disenrollment of 50,142 Medicaid beneficiaries following September redeterminations, including 18,785 for procedural reasons. Since June, 393,222 beneficiaries have lost coverage. Read More
Wisconsin
Wisconsin Reintroduces Bill to Allow Access to Dental Therapists. WISPolitics reported on November 14, 2023, that Wisconsin legislators reintroduced a bill to allow dental therapists to practice in the state. Findings from a Wisconsin Primary Health Care Association (WPHCA) brief show that less than 40 percent of Medicaid-enrolled children received any dental services and less than one-third of Medicaid members have received an oral health exam or preventative services in 2022. Read More
National
States Expect Medicaid Enrollment Decrease, Spending Increase in Fiscal 2024, KFF Medicaid Director Survey Finds. The Kaiser Family Foundation (KFF) on November 14, 2023, released its 23rd Annual Budget Survey of State Medicaid Directors, covering enrollment projections, expenditures, reimbursement policies, and other key aspects of state Medicaid programs. Based on responses from state officials, national Medicaid enrollment will decline by 8.6 percent in fiscal 2024 driven by eligibility redeterminations. Changes in enrollment are expected to lead to a 3.4 percent decrease in total Medicaid spending in fiscal 2024; although the state share of Medicaid spending is expected to increase by 17.2 percent due to the expiration of enhanced federal matching funds on December 31, 2023. Read More
Medicaid Managed Care Expenditures Exceed $441 Billion in Fiscal 2022, KFF Finds. Kaiser Family Foundation (KFF) released data showing that national Medicaid managed care expenditures for fiscal 2022 totaled more than $441 billion. KFF reported that total Medicaid expenditures topped $804 billion in fiscal 2022. Read More
CMS Releases Final Rule Requiring Transparency of Nursing Homes Ownership Arrangements. The Centers for Medicare & Medicaid Services (CMS) released on November 15, 2023, a final rule requiring nursing homes enrolled in Medicaid or Medicare to publicly disclose information regarding their owners, operators, management, and entities that lease or sublease property to the facilities. The requirement is intended to increase transparency in response to a recent report from the Department of Health and Human Services Office of the Assistant Secretary for Planning and Evaluation that found that private equity ownership is associated with poorer staffing conditions and decreases in quality of care. Read More
White House Launches Initiative to Boost Women’s Health Research. Fierce Healthcare reported on November 13, 2023, that the White House is launching a women’s health research initiative, which aims to improve how the federal government addresses and funds research into the health of women. Multiple agencies will convene within 45 days to deliver recommendations on how to advance women’s health research. Read More
SAMHSA Report Finds Most States Lack Value-based Care Policies For Substance Use Disorder Treatment. The Substance Abuse and Mental Health Services Administration (SAMHSA) released a report indicating that eight states have “well developed and ongoing” value-based care initiatives for substance use disorder (SUD) treatment, 20 states have little or no evidence of value-based care policies, and 22 states have “medium evidence.” The review also found 24 states had SUD performance measures for Medicaid quality payment incentives. The report highlights care fragmentation, workforce issues, quality and outcome measurement, technology, and underinvestment, as barriers to implementing value-based payments for SUD services. Read More
Acute Hospital Care at Home Waiver Program Produces Promising Initial Results, Study Finds. Home Healthcare News reported on November 13, 2023, that since the launch of the Acute Hospital Care at Home (AHCAH) waiver, more than 11,000 Medicare, Medicaid, and Medicare-Medicaid dually eligible enrollees received inpatient hospital services at home between November 2021 and March 2023, with just 7.2 percent transferred back to the hospital, according to a research letter published in JAMA. Currently, 128 health systems and 304 hospitals in 37 states are approved to participate in the waiver program, which Congress has authorized through December 31, 2024. Read More
ACA Risk Adjustment Program Is Functioning as Intended, Study Shows. Fierce Healthcare reported on November 9, 2023, that the Affordable Care Act’s (ACA) risk adjustment program is functioning as intended, according to an analysis conducted by Oliver Wyman for the Blue Cross Blue Shield Association. The analysis also found that small insurers or new entrants are not disadvantaged by the program. Read More
HRSA Is Hit With Federal Lawsuit Over 340B Offsite Clinic Registration Policy. Modern Healthcare reported on November 9, 2023, that more than a dozen health systems are claiming that the Health Resources and Services Administration (HRSA) overstepped its authority by reinstating a pre-COVID policy requiring hospitals to register offsite clinics and list them on Medicare cost reports to qualify for 340B drug discounts, according to a federal lawsuit. The lawsuit, filed in the U.S. District Court for the District of Columbia, argues HRSA’s new rule is costing covered entities hundreds of millions of dollars and delays access to 340B discounts for offsite clinics. Read More
Senate Finance Committee Advances Bill to Address PBM, Mental Health Policies. Congressional Quarterly reported on November 8, 2023, that the Senate Finance Committee advanced legislation that addresses mental health care policies, pharmacy benefit managers (PBMs), and Medicare and Medicaid payment policies. The bill would delay planned cuts through 2026 to disproportionate share hospitals (DSH), which serve a large number of Medicaid enrollees, mitigate planned cuts to Medicare physicians, and partially extend the alternative pay model bonus beyond 2023. The legislation also includes stricter policies around ensuring that total costs to patients do not exceed the net price of a drug, and require that Medicare Advantage plans maintain accurate provider directories. Read More
Senators Introduce Bill to Provide Medicaid Coverage to Foster Children in Mental Health Treatment Centers. The Ripon Advance reported on November 8, 2023, that Senators Thom Tillis (R-NC) and Marco Rubio (R-FL) introduced a bill that would extend Medicaid coverage to foster care children receiving mental health and substance use services in a Qualified Residential Treatment Program (QRTP). The bill would provide an exemption from the current federal Institutions for Mental Disease (IMD) exclusion, which prohibits Medicaid payment to certain QRTPs and other facilities with more than 16 beds that provide mental health services. Read More
Industry News
Fourteen Insurers to Exit Medicare Advantage Markets in 2024, KFF Data Show. Kaiser Family Foundation (KFF) released on November 8, 2023, that 14 insurers are exiting Medicare Advantage markets in 2024, bringing the total number of Medicare Advantage plans to 3,959. Insurers exiting markets include ApexHealth, Ascension Complete, Catholic Health Care System, Health Choice Generations Utah, Imperial Insurance Companies, Integrated Health Plan, Lasso Healthcare, Mary Washington Medicare Advantage, Orange County Health Authority, Oscar, ParkerCare New York, ProMedica Medicare Plan, University of Utah Health Insurance Plans, and Vantage Health Plan. Read More
Centene Names Susan Smith as Chief Operating Officer. Centene Corporation announced November 15, 2023, that Susan Smith has been named chief operating officer (COO), effective January 1, 2024. She will be responsible for core business operations, population health, the enterprise transformation office, provider experience and quality. Smith has worked at Centene since June 2023, serving as senior vice president of clinical, quality and enterprise solutions. Read More
UnitedHealth Group Faces Lawsuit Over Algorithm Applied to Medicare Advantage Claims. STAT News reported on November 14, 2023, that the families of two deceased UnitedHealthcare Medicare Advantage members have filed a class-action lawsuit claiming UnitedHealth Group and its subsidiary NaviHealth used algorithmic technology to wrongfully deny payment for care. The lawsuit, filed in U.S. District Court of Minnesota, argues that UnitedHealth Group inappropriately limits the number of days it will pay for a patient’s stay in a rehabilitation facility. UnitedHealth reports that the technology does not impact coverage determinations. Read More
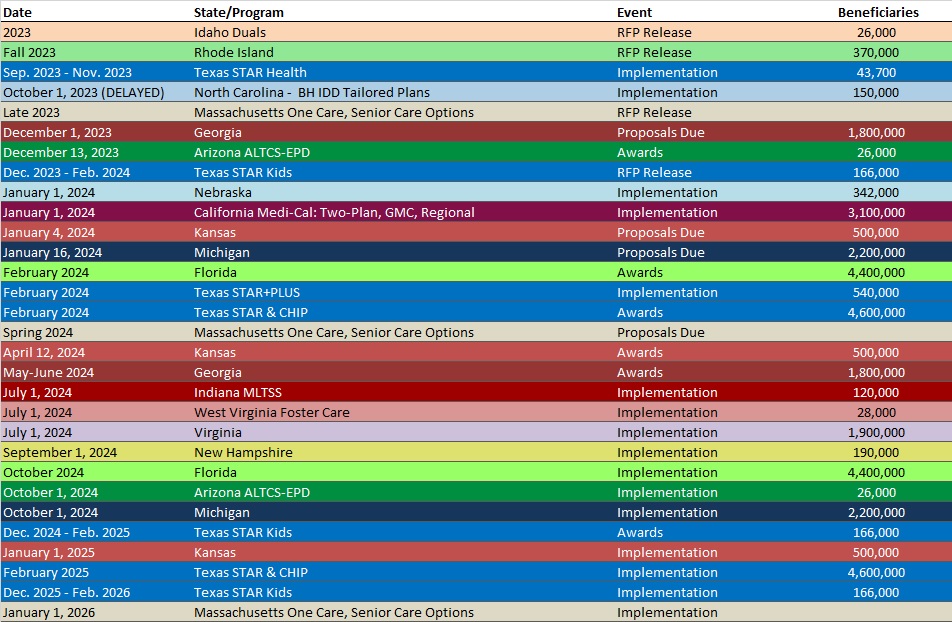
RFP Calendar
HMA News & Events
Health Management Associates Expands Footprint in North Carolina, New Orleans. Health Management Associates (HMA), a leading independent, national healthcare consulting firm today announced that it is establishing offices in North Carolina and New Orleans. In North Carolina, HMA will have a presence in Raleigh and Charlotte with plans to continue building out the North Carolina team in the coming months. The Focus Group, based in New Orleans, joined HMA in 2022, and HMA continues to expand its footprint there adding new colleagues from the area to its roster of experts. They will share office space at The Focus Group’s current Poydras Street location. “Our firm’s continued growth is designed to support the current and future needs of our clients across the country,” said Doug Elwell, HMA’s chief executive officer. “We are excited to plant roots in North Carolina and expand our talented team in New Orleans as we help clients successfully navigate the toughest challenges facing healthcare and human services.” Read More
Leavitt Partners, an HMA Company Exclusive:
Leavitt Partners’ Liz Wroe Talks About the Potential Impact of a Government Shutdown on Health Care Priorities. As Congress heads toward a government shutdown, many in health care are left wondering what this means for them. Liz Wroe, Principal at Leavitt Partners, an HMA company, outlines the effects on various parts of the health care industry and more in this video. The presentation is designed to help organizations and businesses dependent on federal funds plan for this disruption. Watch Now
Wakely, an HMA Company White Papers: