This week, we reviewed updated reports issued by the Department of Health & Human Services (HHS) on Medicaid expansion enrollment from the “September 2016 Medicaid and CHIP Application, Eligibility Determination, and Enrollment Report,” published on December 1, 2016. Additionally, we review 2016 Exchange enrollment data from the HHS Office of the Assistant Secretary for Planning and Evaluation (ASPE) Issue Brief, “Health Insurance Marketplace 2016 Open Enrollment Period: February 2016 Enrollment Report,” and 2017 enrollment snapshot data through December 19, 2016, from the Centers for Medicare & Medicaid Services (CMS). Combined, these reports present a picture of Medicaid and Exchange enrollment at the end of 2016, with a look at progress towards 2017 Exchange enrollment.
Key Takeaways from Medicaid Enrollment Report
- Across all 50 states and DC, Medicaid and CHIP enrolled more than 73.1 million individuals as of September 2016.
- Medicaid and CHIP enrollment is up nearly 1.4 million members since December 2015, a 1.9 percent increase in enrollment.
- From December 2015 to September 2016, four states saw double-digit percentage growth in Medicaid and CHIP – Louisiana (26.2 percent); Alaska (25.9 percent); Montana (24.2 percent); and Arkansas (11.8 percent).
- Through these first three quarters of 2016, eight states (Utah, Washington, North Dakota, New Hampshire, Michigan, Massachusetts, Alabama, and Wisconsin) saw enrollment growth of less than 1 percent. Meanwhile, 10 states (Georgia, Illinois, DC, Mississippi, Wyoming, Delaware, New York, Maine, Oregon, and Vermont) saw enrollment decline across Medicaid and CHIP.
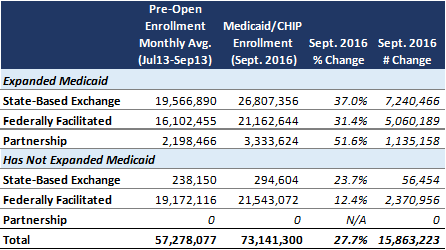
- Medicaid and CHIP enrollment is up more than 15.8 million (nearly 28 percent) from the “Pre-Open Enrollment” period, defined as July 2013 through September 2013.
- The top five states in percentage growth of Medicaid and CHIP enrollment under the Medicaid expansion are Kentucky (100.9 percent), Nevada (85.3 percent), Colorado (74.0 percent), Arkansas (68.5 percent), and New Mexico (67.9 percent).
- The top five states in percentage growth of Medicaid and CHIP among states that did not expand Medicaid are Tennessee (30.4 percent), North Carolina (26.6 percent), Idaho (23.7 percent), Florida (17.2 percent), and Georgia (13.6 percent).
- The top five states in total enrollment growth of Medicaid and CHIP are California (4.03 million), New York (732,386), Washington (667,613), Ohio (636,552), and Kentucky (612,239).
Table 1 – Overall U.S. Medicaid/CHIP Enrollment Growth – Pre-Open Enrollment Monthly Average through September 2016
Key Takeaways from 2017 Exchange Enrollment Snapshot Reports
- Final Exchange enrollments for the 2016 plan year, published in the Spring of 2016, showed Qualified Health Plan (QHP) enrollments of nearly 12.7 million across all 50 states and DC.
- As of December 19, 2016, there have been nearly 6.4 million QHP selections for the 2017 plan year in the 39 Federally Facilitated Marketplace (FFM) states. Of these, more than 4.3 million are for individuals renewing coverage, with just under 2.1 million new enrollees.
- Just a week prior, as of December 10, 2016, there were just over 4 million QHP selections in the FFM states. These nearly 1.4 million new plan selections include more than 670,000 individuals who signed up for coverage on December 15, 2016, the highest recorded in a single day.
- As of December 17, 2015, last year’s deadline for coverage beginning January 1, 2016, there were a cumulative 6.0 million QHP selections in FFM states. Of these, 3.6 million were renewing coverage, with 2.4 new enrollees.
- Across the 39 FFM states in the latest enrollment snapshot, QHP selections as of December 19, 2016, equate to roughly two-thirds (65.4 percent) of the final QHP selection total as of February 2016.
The table on the following page (Table 2) provides state-level data on Medicaid and Exchange enrollment.
Medicaid and Exchange Enrollment Data Sources
Link to CMS Medicaid Expansion Enrollment Report:
Link to ASPE Health Insurance Marketplace Enrollment Report:
Link to Biweekly Exchange Enrollment Snapshot:
Table 2 – Medicaid/CHIP Enrollment Growth Across All States (September 2016), Final 2016 Exchange Enrollment (February 2016), and Preliminary 2017 Exchange Enrollment (December 10, 2016)
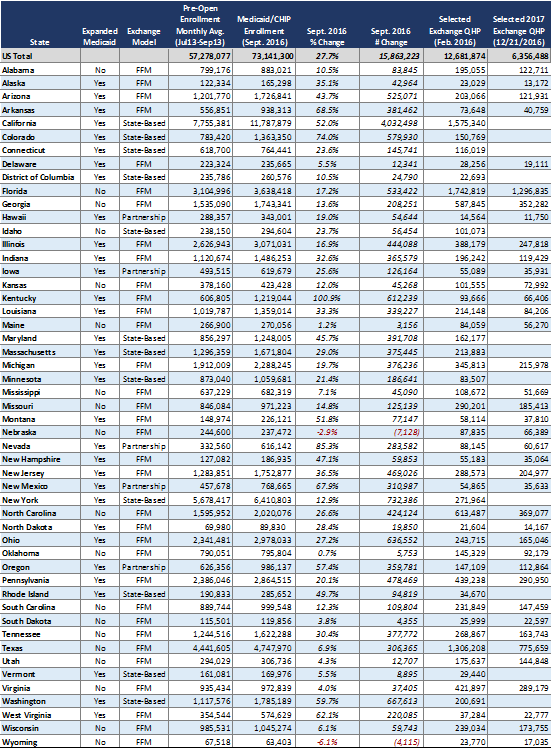
* Several states use the FFM marketplace for enrollment, despite being a state-based exchange; these states are HI, NV, NM, OR, listed in the above table as “Partnership.”
Note: Connecticut and Maine did not report Pre-Open Enrollment Period enrollment data to HHS for the report. HMA has substituted the December 2013 Medicaid enrollment total from the Kaiser Family Foundation, compiled by Health Management Associates (HMA) from state Medicaid enrollment reports for the Kaiser Commission on Medicaid and the Uninsured (KCMU).