This week, our In Focus section reviews the request for proposals (RFP) issued by the Virginia Department of Medical Assistance Services (DMAS) for the Medallion 4.0 Medicaid managed care program. Medallion 4.0 will serve roughly 740,000 children, including those with special health care needs, families, and individuals in foster care and adoption assistance programs, with annual Medicaid managed care spending of more than $3 billion when fully implemented by the end of 2018. Proposals are due to DMAS on September 8, 2017.
Medallion 3.0 Shift to Medallion 4.0
The Medallion 3.0 program currently provides Medicaid managed care to around 784,000 members across seven regions in the state. However, around 86,000 current Medallion 3.0 members will shift to the new Commonwealth Coordinated Care Plus (CCC Plus) program on January 1, 2018. CCC Plus, a separate Medicaid managed care program providing managed acute care and long-term services and supports, was procured in the last year under a separate RFP.
When fully implemented, Medallion 4.0 will cover nearly 740,000 Medicaid and Family Access to Medical Insurance Security (FAMIS) eligible members, including infants, children and adults in the low income families with children (LIFC) group, pregnant women, FAMIS MOMS, foster care and adoption assistance, children with special health care needs, and teens. This figure includes roughly 30,000 new Medallion 4.0 members. Based on an average per-member-per-month capitation rate of $349, as provided in the RFP, annual capitation payments to MCOs under the Medallion 4.0 can be estimated at more than $3 billion.
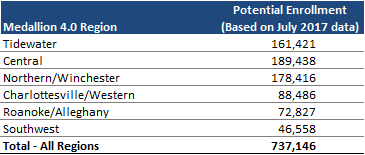
Source: DMAS RFP
Medallion 4.0 excluded categories of eligibility are CCC Plus enrollees, individuals in home and community based services (HCBS) waivers, members in the aged, blind, and disabled (ABD) category of eligibility (including SSI), dual eligibles, Program of All-Inclusive Care for the Elderly (PACE) members, as well as a number of smaller and limited benefit categories, as detailed in the RFP.
Medallion 4.0 will also mark the beginning of Medicaid managed care plans covering and coordinating new services, such as Early Intervention and non-traditional behavioral health services, previously carved out of Medallion 3.0.
Contract Terms, Considerations
DMAS intends to contract with at least three MCOs in each of the six regions. Bidders may propose to serve any number of regions, and do not need to submit separate bids for each region. Initial contracts will run for one year, with annual contract extension/renewal options available up to a maximum term of six years.
In December 2016, the Virginia Joint Legislative Audit and Review Commission (JLARC) released its report, Managing Spending in Virginia’s Medicaid Program. The RFP encourages bidders to review the report and indicate in their proposals how they will “participate in and comply with all initiatives” DMAS pursues in response to the report. HMA provided a summary of the JLARC report in the December 14, 2016, edition of the HMA Weekly Roundup which is available on our website, www.healthmanagment.com.
Contracted MCOs must maintain a minimum medical loss ratio (MLR) of 85 percent, with adjustment payments to be made to the state if actual MLRs are found to be less than the minimum.
RFP Timeline
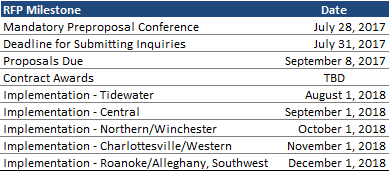
A mandatory preproposal conference will be held this Friday, July 28, 2017, with a deadline for submitting inquiries to follow on July 31. Proposals are due to DMAS on September 8, 2017. No date has been announced for potential contract awards.
Implementation of Medallion 4.0 will begin on August 1, 2018, to be phased in across the six regions through the remainder of the calendar year.
Current Medallion 3.0 Market
The Medallion 3.0 program, served by seven MCOs, is dominated by Anthem, Virginia Premier, and Optima Health, with combined market share of more than 80 percent.
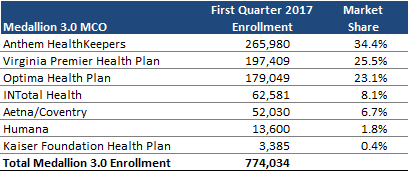
Source: HMAIS
DMAS awarded CCC Plus contracts in February 2017 to six MCOs: Aetna Better Health of Virginia, Anthem HealthKeepers Plus, Magellan Complete Care of Virginia, Optima Health, United Healthcare, and Virginia Premier Health Plan. Aside from United and Magellan Complete Care, all selected plans are incumbents in Medallion 3.0 plan. Beginning in August 2017, DMAS will begin implementation of the new CCC Plus program, which will provide integrated acute care and long-term services and supports (LTSS) to around 214,000 older adults and both children and adults with disabilities.
Link to Medallion 4.0 RFP
http://www.dmas.virginia.gov/Content_atchs/m4/RFP201703,MEDALLION4FINAL.pdf