Over the course of three weeks CMS has made a series of Medicare announcements that arguably contain the most sweeping changes to the Medicare program proposed thus far by the Biden Administration. With final Medicare payment rules on the horizon, CMS is poised to further the Biden Administration’s directional imprint on the Medicare program. The recent releases include:
- A new opportunity focused on rural hospitals designed to preserve –and likely expand – access to services in rural communities;
- A proposed payment and policy rule for outpatient and ambulatory care services also lays the groundwork for new transparency and competition initiatives;
- Significant updates to most aspects of Medicare’s accountable care organizations; and
- New opportunities to support oncology providers in moving towards a whole person approach to services through the Enhancing Oncology Model.
For this blog our HMA experts focus on the 2,000+ page Calendar Year (CY) 2023 Medicare Physician Fee Schedule (PFS) proposed rule released to the public on July 7, 2022. The Medicare Physician Fee Schedule and its accompanying proposed policy changes is a significant tool CMS uses to advance annual updates in reimbursement policy and to consider other policy changes in traditional Medicare that have implications for the program writ large.
Generally, in the CY 2023 proposed rule the Administration is continuing to broaden and deepen the way it applies its health equity framework to the entirety of the proposals, strengthens access to behavioral health services, and reinvigorates value-based care through the Medicare Shared Savings Program’s (MSSP) Accountable Care Organizations (ACOs) structure.
The rule includes a myriad of other policy proposals. We highlight a few of the key ones below. For example, CMS must make updates to the physician fee schedule conversion factor which has ripple effects throughout the Medicare program. The agency is also proposing updates to reimbursement for certain telehealth services and coverage enhancements for hearing and dental services, among many others proposals.
Key Action Items for Stakeholders
All comments to the rule are due to CMS by September 6, 2022. CMS plans to publish the final rule in late fall 2022.
The public comment opportunity is essential for CMS to deepen its understanding of the impact of the proposals. The agency considers stakeholders’ concerns, questions, and other feedback as it makes decisions on which proposals to finalize, modifications to the proposals, or to defer implementation.
This is also an important window of opportunity during which stakeholders can analyze the impact of the proposals and the business decisions these may require, plan advocacy around the proposed changes, and prepare for implementation which generally will occur on January 1, 2023.
Many leading national provider organizations are making their concerns with the annual payment update a central piece of their advocacy agenda in Congress. These concerns will add to the long list of structural issues that Congress is expected to debate leading up to and well after this year’s mid-term elections. However, providers still need to weigh the inflation pressures and uncertainty surrounding Congress’ ability to intervene with new opportunities in the Medicare program and Medicare Advantage market.
Medicare Shared Savings Program
CMS proposes significant changes to the Medicare Shared Savings Program (MSSP), which aredesigned to accelerate provider and Medicare beneficiary participation in accountable relationships. Last year, CMS established a goal of all Medicare beneficiaries will be in a care relationship with accountability for quality and total cost of care by 2030. These proposals are designed to make further progress on achieving that goal. First, CMS proposes several changes to MSSP which respond to criticisms that the program is not sufficiently flexible to support Medicare providers who may have different levels of sophistication with respect to risk-sharing and available capital for practice transformation. Additionally, it reflects federal officials understanding of the impact social care services can have on Medicare beneficiary health and well-being.
Proposed changes to the MSSP include the following:
- Investment in New Accountable Care Organizations (ACOs): CMS proposes to provide a one-time fixed payment of $250,000 and quarterly payments for the first two years of the 5-year agreement period for certain ACOs. Eligible ACOs are those that are low revenue ACOs, inexperienced with performance-based risk Medicare ACO initiatives, new to MSSP and that serve underserved populations.
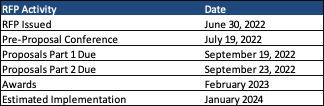
- The initial application cycle to apply for advance investment payments will occur during CY 2023 for a January 1, 2024, start date.
- The advance investment payments would increase when more beneficiaries who are dually eligible for Medicare and Medicaid or who live in areas with high deprivation or both, are assigned to the ACO.
- The advance investment payments would be recouped once the ACO begins to achieve shared savings in their current agreement period and in their next agreement period, if a balance persists. If the ACO doesn’t achieve shared savings, CMS would not recoup the funding.
- Funds would be available to address the social and other needs of people with Medicare.
- CMS would also provide greater flexibility in the progression to performance-based risk for new ACOs to ease the transition to and likelihood of success under risk arrangements. Specifically, for ACOs with agreement periods beginning on January 1, 2024, and in subsequent years, ACOs inexperienced with performance-based risk could participate a one-side risk model for up to 7 years.
- Current ACO Participants: For performance years beginning January 1, 2023, and in subsequent years, CMS may allow certain currently participating ACOs to elect to continue in their glide path agreement.
- CMS intends to incorporate an adjustment for prior savings that would apply in the establishment of benchmarks for renewing ACOs and re-entering ACOs
- CMS also is proposing several changes to the benchmark methodology to better support long term participation in MSSP and less capitalized ACOs for agreement periods beginning January 1, 2024. This includes adjusting the benchmark for prior savings and reducing the impact of the negative regional adjustment.
- CMS also plans to include a fixed, prospectively projected administrative growth factor (referred to in this proposed rule as the Accountable Care Prospective Trend (ACPT)), into a three-way blend with national and regional growth rates to update an ACO’s historical benchmark for each performance year (PY) in the ACO’s agreement period.
- CMS requested comments on alternative benchmarking policies: a) exclude the ACO’s own assigned beneficiaries from the assignable beneficiary population used in regional expenditure calculations, b) expand the definition of the ACO regional service area to use a larger geographic area to determine regional FFS expenditures, or c) both.
- Beginning on January 1, 2023, and subsequent years, CMS is planning to change the all-or-nothing approach to determining an ACO’s eligibility for shared savings based on quality performance to allow for scaling of shared savings rates for ACOs that fall below the 30th/40th percentile quality standard threshold required to share in savings at the maximum sharing rate. To be eligible ACOs must meet minimum quality reporting and performance requirements.
- CMS also plans to update MSSP quality-measurement policies, including a new health equity adjustment that would award bonus points for high quality measure performance and serving higher proportions of underserved or dually eligible beneficiaries.
Behavioral Health Changes
The CY2023 MPFS also seeks to enhance access to behavioral health services and strengthen the behavioral health model within the Medicare program. The proposals include:
- Creating an exception to supervision requirements, allowing marriage and family therapists, licensed professional counselors, addiction counselors, certified peer recovery specialists, and others to provide behavioral health services while being under general supervision rather than “direct” supervision.
- Paying psychologists and social workers to help manage behavioral health needs as part of the primary care team.
- Establishing new payments for team-based, comprehensive management and treatment of chronic pain.
- Enhancing the ability of ACOs to address social, behavioral, and physical health care needs, by making advanced shared savings payments to new, smaller ACOs. CMS states these funds could be used to hire behavioral health practitioners and address the social needs, such as food and housing.
- Clarifying Opioid Treatment Programs may bill Medicare for services performed by mobile units without obtaining a separate registration and increasing payment rates to Opioid Treatment Programs.
These proposed changes represent a major shift in traditional Medicare’s coverage of behavioral health services. If finalized and in combination with changes to coverage for telehealth services, these could have a meaningful impact for Medicare beneficiaries including those in rural communities. ACOs, health systems, and other providers may have greater opportunities to include behavioral health practitioners in their model of care.
Payment Issues
Payments to physicians through the PFS are proposed to decline by roughly 4 percent from CY 2022 to CY 2023. The bulk of this decline stems from CMS’s proposal to reduce the PFS conversion factor (CF) by nearly 4.5 percent. In dollar terms the proposed 2023 CF would be $33.08, which is $1.53 lower than the 2022 CF. This policy change to the CF reflects three dynamics, two of which are changes directly mandated by the U.S. Congress:
- Expiration of a statutory one-year 3 percent increase in payments,
- A statutory 0 percent payment update for CY 2023, and
- A budget neutrality adjustment across all billing codes resulting from modifications to PFS weights which increased the relative value of primary care billing codes.
Payment changes contained within the CY 2023 proposed rule result in differential impacts for individual physician service codes and physician specialties. While payment rates for many codes are proposed to decline uniformly by roughly 4 percent, payment rates for some services codes may decline more, such as for some physician inpatient hospital care codes that may decline more than 10 percent. In the context of physician specialty type, CMS estimates 5 percent payment increases on average for infectious disease and a 3 percent increases on average for internal medicine and geriatrics. By contrast, CMS estimates a 2 percent decline on average for clinical psychology and a 3 percent decline on average for radiology.
Notable Issues for Stakeholder Consideration
In addition to the major structural and financing issues discussed above, the wide-ranging rule contains numerous other policy proposals with direct and indirect implications on Medicare providers, and beneficiaries, and other stakeholders. Table 1 provides a snapshot of some of the issues that warrant further consideration.
Table 1. Other Notable Proposed Changes Impacting Health Care Providers and Stakeholders
| Topic | Summary |
| Telehealth | The Proposed Rule makes a number of potential changes to telehealth policies: Implements several of the policies mandated by the Consolidated Appropriations Act (CAA) of 2022, which extended telehealth flexibilities CMS adopted during the public health emergency (PHE) for 151 days after the end of the PHE. The rule also confirms Medicare telehealth services performed with dates of service occurring on or after the 152nd day after the end of the PHE will revert to pre-PHE rules and the appropriate place of service (POS) indicator will be required to be included on the claim.Permanently adds three new services to the list of reimbursable telehealth services: prolonged inpatient hospital, prolonged skilled nursing, and prolonged home services. Adds several additional services to the Medicare Telehealth Temporarily (through the end of CY 2023) adds several telehealth services: new therapy services, audiology, and new behavior assessment/treatment services. Temporarily (during PHE plus 151 days) requires practitioners to use billing modifier code ‘95’ and either provider of service code ‘02’ (not in home) or ‘10’ (home) for all telehealth services. At the end of the PHE-plus-151 days, billing requirements will revert to pre-PHE methods. Permanently (beginning in 2023) requires practitioners to use billing modifier ‘93’ for all audio-only services, and requires RHCs, FQHCs, and OTPs to use modifier ‘93’ for eligible mental health services furnished via audio-only services. However, CMS specifically did not propose to extend audio-only evaluation and management visits beyond the 151 days after the PHE. |
| Dental | Medicare pays for a limited number of dental services when the dental care is an integral part of a beneficiary’s medical treatment. CMS is proposing to add to the list of conditions where that may be appropriate such as dental exams and necessary treatments prior to organ transplants, cardiac valve replacements, and valvuloplasty procedures. CMS is also seeking feedback on other clinical conditions where the dental services are linked to the clinical success of the medical services. |
| Hearing | CMS is proposing to allow audiologists to perform and bill for certain diagnostic hearing tests for patients with non-acute conditions without a physician order. |
| Wound Care | CMS is proposing several policies to update payment, coding and billing for skin substitutes which are commonly used in the treatment of diabetic foot ulcers and venous leg ulcers. CMS is proposing to change the terminology of skin substitutes to ‘wound care management products’ in order to reflect how clinicians use these products, to provide a more consistent approach to coding for these products, and to treat and pay for these products as a physician supply instead of a separately paid product under the Average Sales Price methodology beginning on January 1, 2024. |
| MIPS | CMS continues to update and refine the quality measures used in the different aspects of the programs under MIPS including the addition of certain health equity related measures. CMS also is proposing five additional MIPS Value Pathways (MVPs) (Advancing Cancer Care, Optimal Care for Kidney Health, Optimal Care for Patients with Episodic Neurological Conditions, Supportive Care for Neurodegenerative Conditions, and Promoting Wellness) CMS also proposed several ways to reduce the burden for physicians participating in advanced alternative payment models (AAPMs) including permanently establishing the 8% minimally Generally Applicable Risk Standard for AAPM qualification and proposing to apply the eligible clinician limit to the entity participating in the medical home model rather than the parent organization. |
The HMA Medicare team will continue to analyze these proposed changes. We have the depth and breadth of expertise to assist with tailored analysis, to model policy impacts, and to support the drafting of comment letters to this rule.