HMA Weekly Roundup
Trends in Health Policy
This week's roundup:
- In Focus: The Family Glitch and Changes to Premium Tax Credit Eligibility

- Florida Governor Signs Medicaid Managed Care, Nursing Home Legislation

- Illinois Lawmakers Approve Medicaid Bill Expanding Certain Benefits, Coverage

- Louisiana Awards NEMT Contract

- Louisiana Legislature Passes Bill to Provide Medicaid Dental Coverage to Adults

- Massachusetts Releases Medicaid ACO RFR

- New York Files 1115 Waiver Amendment to Address Health Equity

- New York Medicaid Director Brett Friedman Steps Down

- Oregon Governor Establishes Taskforce to Develop Medicaid Bridge Plan

- Rhode Island Names Kristin Pono Sousa Medicaid Director

- HHS Extends Public Health Emergency for 90 Days to July 15

- Genuine Health Group Acquires Accountable Care Medical Group

In Focus
The Family Glitch and Changes to Premium Tax Credit Eligibility
This week, our In Focus section reviews the Biden Administration’s proposed rule revising eligibility standards for premium subsidies for families, released on April 5, 20221. The proposed rule would “fix” the family glitch and, therefore, dramatically increase the number of people eligible for premium tax credits. This brief describes what the regulation would do and the implications for the individual market.
What is the Family Glitch and What Changed
The Affordable Care Act provides premium subsidies to eligible individuals. One of the conditions for eligibility is not having an affordable offer from an employer-sponsored plan that meets minimum essential coverage requirements. If an employer offer is not affordable than individuals gain eligibility for premium subsidies. An Obama era regulation defined the affordability test to compare the cost of employee-only coverage to the family’s income. Only if the cost of the employer coverage exceeded a certain percentage, in 2022 the percentage was 9.61 percent of income, did the individual qualify for premium tax credits (PTC). The issue is that the cost of coverage to the family was not included in the affordability calculations. Consequently, if the cost of the family coverage exceeded the affordability threshold, but the employee only coverage was below the affordability threshold, the entire family was denied eligibility for premium tax credits. This “glitch” is referred to as the family glitch since family members were not included in affordability calculations.
The new proposed regulation would change the affordability calculations for individuals with employer sponsored insurance starting in 2023. Affordable offers would be judged two separate ways; determinations of affordability would be made for the employee and then separately for other family members (e.g., spouse and/or dependents). Consequently, the affordability determination will not change for employees, and family members will be more likely to gain eligibility for PTC for coverage in the individual market.
Potential Impact
There are both immediate and long-term implications if the rule is finalized. Most directly, an estimated 125,000 individuals currently enrolled in the individual market would gain eligibility for PTC2. The White House released an estimate that an additional 200,000 currently uninsured would take-up coverage as a result of the change to the family glitch. Over the long term, there could be migration from those with Employer-sponsored insurance (ESI) to the individual market, given the lower net premiums. In fact, the vast majority of those currently impacted by the family glitch currently have ESI coverage (an estimated 4 million people)3. Finally, given the potential for increased amount of outlayed PTCs, states that currently have 1332 waivers, could see additional Federal pass-through funds.
Please contact Michael Cohen at [email protected] with any questions or to follow up on any of the concepts presented here
1.https://www.federalregister.gov/documents/2022/04/07/2022-07158/affordability-of-employer-coverage-for-family-members-of-employees
2. https://www.urban.org/sites/default/files/publication/104223/changing-the-family-glitch-would-make-health-coverage-more-affordable-for-many-families_1.pdf
3. lbid
HMA Roundup
California
California Seeks to Raise Medi-Cal Asset Limit for Elderly, Individuals with Disabilities. Business Insider reported on April 9, 2022, that the asset limit for eligibility for Medi-Cal programs will increase from $2,000 to at least $130,000 per household for the elderly, individuals with disabilities, nursing home residents, and other special groups, effective July 1, pending federal approval. The asset limit would be eliminated by 2024. Read More
(Note: Updated April 13, 2022)
California Medicaid Plan to Fight $55 Million State Fine. Health Payer Specialist reported on April 8, 2022, that California-based LA Care Health Plan will fight a $55 million state fine over allegedly failing to respond to enrollee grievances in a timely fashion, according to chief executive John Baackes. LA Care has already appealed the fine, which was imposed by the California Department of Managed Health Care and the California Department of Health Care Services last month. Baackes said that if the appeal fails, the plan will fight the fine in court. Read More
Delaware
Delaware DHSS Launches Website Allowing Individuals to Compare Health Care Costs. The Delaware Department of Health and Social Services (DHSS) launched on April 7, 2022, a website called CostAware, which allows individuals to compare the average cost of five episodes of care at six Delaware hospital systems and seven episodes of care at five accountable care organizations. The website, which uses 2019 medical claims data, compares costs for hospital cardiac procedures, C-section birth, emergency department visits, knee and hip replacement, and vaginal delivery, as well as ACO costs for blood count, colonoscopy, doctor visits, hemoglobin A1c, head CT, lumbar spine MRI, and screening mammography. Read More
Florida
Florida Health Plan Misses Deadline to Challenge $9.1 Million Fine Over Claim Denials. Florida Politics reported on April 10, 2022, that Centene/Sunshine State Health Plan of Tampa missed the deadline for challenging a $9.1 million fine from the Florida Agency for Health Care Administration related to the failure to pay thousands of claims for children with serious, chronic conditions. The deadline to pay the fine is April 18. Read More
Florida Health System Settles Federal Lawsuit Over Medicaid Claims. Health News Florida reported on April 8, 2022, that BayCare Health System agreed to pay $20 million to settle a federal Medicaid false claims lawsuit, which alleged that Baycare made donations to the Juvenile Welfare Board of Pinellas County to increase its share of federal Medicaid matching funds. BayCare denied any wrongdoing. Read More
Governor Signs Medicaid Managed Care, Nursing Home Legislation. Health News Florida reported on April 7, 2022, that Florida Governor Ron DeSantis signed two pieces of Medicaid managed care legislation into law. The first (SB 1950) reduces the state’s 11 Medicaid managed care regions to nine ahead of an upcoming health plan procurement. The second (HB 855) requires the Agency for Health Care Administration to report plan performance by demographic group to help address disparities. DeSantis also signed a bill (HB 1239) that attempts to address nursing shortages by reducing the daily hours that certified nursing assistants are required to care for residents. Read More
Illinois
Lawmakers Approve Wide-Ranging Medicaid Bill Expanding Certain Benefits, Coverage. Health News Illinois reported on April 11, 2022, that the Illinois general assembly approved a Medicaid omnibus bill (House Bill 4343), which includes funding for youth mental wellness checks, lowering the age of eligibility for undocumented adults to 42 from 55, increasing psychiatric and perinatal services, and adding coverage of midwives and acupuncture services. The bill also directs the Illinois Department of Healthcare and Family Services to apply for federal approval for 12 months of continuous eligibility for adult Medicaid beneficiaries. Read More
Legislature Allocates $225 Million in Federal Relief Funds to Nursing Homes in Fiscal 2023 Spending Plan. Health News Illinois reported on April 11, 2022, that the Illinois legislature passed a fiscal 2023 spending plan, allocating $225 million of federal relief funds to nursing homes to help address staffing shortages. The bill also directs $58.7 million in federal relief funds to safety net hospitals (on top of $69.8 million in general funds), $30 million to ambulance service providers, and $49.2 million to behavioral health services. Read More
Senate Passes Nursing Home Payment Reform Legislation. WGEM reported on April 7, 2022, that the Illinois Senate unanimously passed legislation to reform nursing home Medicaid payment rates to incentivize increased staffing in facilities. The bill includes a 15-month transition period to the new payment model and will pay all facilities at the higher rate designated for well-staffed nursing homes for six months to incentivize hiring. It also provides for extra payments to facilities with more than 70 percent patients on Medicaid. Read More
Illinois Bill Would Tie Medicaid Nursing Home Payments to Quality, Staffing Levels. The Chicago Tribune reported on April 6, 2022, that Illinois lawmakers are expected to vote on a bill that would tie Medicaid nursing home funding to care quality and staffing levels. The bill is aimed at for-profit nursing homes with large Medicaid populations. Illinois Medicaid spends $2.5 billion per year to cover approximately 45,000 individuals in nursing homes. Read More
Louisiana
Louisiana Awards NEMT Contract. The Louisiana Department of Health (LDH) announced on April 12, 2022, its intent to award a contract to MediTrans for Medicaid non-emergency medical transportation (NEMT). The contract will be implemented July 1, 2022, and run for three years, with options to extend for up to two more years. The state also received proposals from incumbent Southeastrans, OneBunchHookUp, Veyo, and We Lift. Read More
Maryland
Legislature Passes Bill to Provide Medicaid Dental Coverage to Adults. 47 ABC reported on April 6, 2022, that the Maryland legislature has passed legislation to provide Medicaid adults with dental coverage, including diagnostic, preventive, restorative, and periodontal services. The bill, which would take effect on January 1, 2023, awaits signature by Governor Larry Hogan. Read More
Massachusetts
Massachusetts Releases Medicaid ACO RFR. The Massachusetts Executive Office of Health and Human Services (EOHHS) released on April 13, 2022, a request for responses (RFR) to procure MassHealth accountable care organizations (ACOs) under two models: Medicaid Accountable Care Partnership Plans (ACPPs) and Primary Care ACOs (PCACOs). ACPPs are paid capitation rates and bear risk for members’ cost of care, while PCACOs contract directly with MassHealth and are paid a monthly administrative rate. The new contracts will look to enhance expectations for primary care and behavioral health delivery; increase the focus on children, youth, and families; and create incentives to improve health equity. Responses are due on July 15, with contracts to run from April 1, 2023, through December 31, 2027, with an option to extend in any increments up to December 31, 2032. Read More
Nevada
Nevada Medicaid Enrollment Among Immigrants Is at All-Time High. Nevada Current reported on April 7, 2022, that the number of Nevada legal permanent residents enrolled in Medicaid increased 43 percent between March 2020 and February 2022 to a record high of almost 41,000, according to data from the Nevada Department of Health and Human Services. The increase is attributed to the roll back of the public charge rule and continuous eligibility during the pandemic. Read More
New York
New York Files 1115 Waiver Amendment Seeking Authority to Spend $13.5 Billion in Medicaid Funds to Address Health Equity. New York State Department of Health filed on April 13, 2022, an amendment to its Medicaid 1115 waiver seeking authority to spend $13.5 billion in Medicaid funds over five years for a demonstration project aimed at addressing health disparities and delivery system problems magnified by COVID-19. The state will conduct two virtual hearings on the waiver amendment. The public comment period is open until May 13. Read More
New York Medicaid Director Brett Friedman Steps Down. Crain’s New York reported on April 8, 2022, that New York Medicaid director Brett Friedman will be stepping down effective May 1. Amir Bassiri, the current deputy Medicaid director, will replace him. Read More
New York Enacts Fiscal 2023 Budget Raising Medicaid Spending Cap, Giving Providers 1 Percent Rate Hike. Crain’s New York reported on April 11, 2022, that New York enacted its final fiscal 2023 budget. The budget includes a 4.7 percent increase in the Medicaid global spending cap and a 1 percent increase in reimbursement rates for Medicaid providers. The bill also restores a provider rate cut of 1.5 percent from the prior administration. The rate increase is retroactive to April 1. Legislators previously rejected Governor Kathy Hochul’s proposal to introduce competitive bidding for Medicaid managed care plans. Read More
North Carolina
North Carolina Medicaid Expansion Committee Discusses Certificate of Need Reform. The Winston-Salem Journal reported on April 11, 2022, that North Carolina Senator Joyce Krawiec (R-Forsyth) proposed changing the state’s certificate-of-need (CON) laws as a way to expand access to health care at a meeting for the committee on Access to Healthcare and Medicaid Expansion. CON opponents say that adding competition would lead to new services and facilities, which could force providers to lower fees for high-risk procedures. Meanwhile, advocates say CON protects against for-profit groups picking the most profitable medical procedures and leaving not-for-profit systems with the sickest patients who may be uninsured. The committee will meet again on April 26. Read More
Oregon
Governor Establishes Taskforce to Develop Medicaid Bridge Plan. The Oregon Capital Chronicle reported on April 11, 2022, that Oregon Governor Kate Brown has established a task force to develop a bridge plan for individuals disenrolled from Medicaid when the federal public health emergency ends. The task force, which consists of 13 stakeholders appointed by Brown, will be co-chaired by state Representative Rachel Prusak (D-Tualatin) and state Senator Elizabeth Steiner Hayward (D-Portland). Read More
Pennsylvania
Pennsylvania Applies for 1115 Waiver Extension for Former Foster Youth, Substance Use Treatment. The Centers for Medicare & Medicaid Services announced on April 12, 2022, that Pennsylvania has applied for a five-year extension of a Medicaid Section 1115 waiver extension that allows the state to provider Medicaid coverage to former foster care youth under age 26 who were under the care of another state when they turned 18. The waiver also covers substance use disorder treatment for short-term residents at Institutions for Mental Disease. The waiver extension would run through September 30, 2027. The federal public comment period is open until May 12. Read More
Pennsylvania Expands Medicaid Postpartum Coverage to One Year After Giving Birth. WESA reported on April 11, 2022, that the Pennsylvania Department of Human Services has extended Medicaid postpartum coverage to one year after giving birth. Previously, Medicaid-eligible women were covered up to 60 days after giving birth. The state implemented this change through the authority created by the American Rescue Plan Act. Read More
Rhode Island
Rhode Island Names Kristin Pono Sousa Medicaid Director. EIN Newsdesk reported on April 6, 2022, that Rhode Island has named Kristin Pono Sousa as Medicaid program director, effective April 10. Sousa has served as interim director since December 2021. Read More
Wisconsin
Wisconsin Seeks Public Comments on Draft Waiver to Extend Postpartum Medicaid Coverage. The Wisconsin Department of Health Services announced on April 6, 2022, that it is seeking public comment for a draft waiver request to the Centers for Medicare & Medicaid Services to extend postpartum Medicaid coverage from 60 days to the last day of the month 90 days after the last day of pregnancy. Governor Tony Evers has recommended extending postpartum coverage to one year. Public comments can be submitted until May 6. Read More
West Virginia
West Virginia Medicaid Commissioner to Serve as President of NAMD Effective 2023. The West Virginia Department of Health and Human Resources announced on April 11, 2022, that Cindy Beane, who currently serves as commissioner of the state Bureau for Medical Services, will also serve as president of the National Association of Medicaid Directors (NAMD) effective in 2023. Beane will hold the title of NAMD president-elect effective immediately. Read More
National
Biden Administration Awards $43 Million in Grants to 93 Rural Health Care Providers, Community Groups. Kaiser Health News reported on April 13, 2022, that the Biden administration awarded $43 million in grants to 93 rural health care providers and community groups in 22 states. A total of $475 million has been set aside for rural health care organizations by the American Rescue Plan Act. Read More
11 States to Text Medicaid Enrollees About Reenrollment After PHE Ends. Kaiser Health News (KHN) reported on April 13, 2022, that only 11 states plan to contact Medicaid enrollees via text about reenrollment after the end of the public health emergency (PHE), according to a KHN report. Thirty-three states plan to use the U.S. Postal Service, and 20 will phone enrollees. The Centers for Medicare & Medicaid Services has recommended that states use texts in addition to other methods to notify Medicaid members of post-PHE eligibility redetermination requirements. Read More
HHS Extends Public Health Emergency for 90 Days to July 15. CQ Roll Call reported on April 13, 2022, that U.S. Health and Human Services Secretary Xavier Becerra extended the public health emergency (PHE) by 90 days to July 15, 2022. The Centers for Medicare & Medicaid Services has said it will give states 60 days notice before the end of the PHE. Read More
HHS to Collect Information on Medical Debt from Providers, Factor Into Grant Decisions. Modern Healthcare reported on April 11, 2022, that the U.S. Department of Health and Human Services (HHS) will request data from more than 2,000 providers on their medical bill collection practices, lawsuits against patients, financial assistance, financial product offerings, and third-party contracting or debt-buying practices. The information will be used when HHS makes grantmaking decisions, and some of it will become public, with potential violations being shared with enforcement agencies. The policy follows an executive order from President Biden to reduce the burden of medical debt. Read More
MACPAC Recommends Improving Oversight of State Directed Provider Payments in Medicaid Managed Care. The Medicaid and CHIP Payment and Access Commission (MACPAC) released on April 7, 2022, a draft chapter of its June report to Congress, including recommendations aimed at improving the oversight of state directed provider payments in Medicaid managed care programs. The recommendations address the transparency of existing directed payment information, collection of provider-level data on directed payment spending, and clarification of directed payment quality goals. Read More
CMS Will Phase Out Temporary COVID-19 Nursing Home Regulation Waivers. Modern Healthcare reported on April 7, 2022, that the Centers for Medicare & Medicaid Services (CMS) will phase out temporary COVID-19 nursing home regulation waivers in 30 or 60 days, depending on the waiver. The waivers included allow physicians to delegate certain tasks to nurses and physician’s assistants, permit telehealth visits, and waive certain training requirements, among others. CMS will continue to offer state-based, county-based, and facility-based temporary waivers. Read More
House Lawmakers Introduce Bill to Enable Medicaid Value-Based Drug Agreements. Fierce Healthcare reported on April 7, 2022, that a bipartisan group of House lawmakers introduced a bill aimed at enabling the use of value-based drug purchasing agreements in Medicaid. The goal of the Medicaid VBP Act is to reimburse drug makers based on outcomes for new treatments like gene therapy. Read More
CMS Proposes $320 Million Cut to Nursing Home Medicare Payments in Fiscal 2023. Modern Healthcare reported on April 11, 2022, that the Centers for Medicare & Medicaid Services (CMS) issued a proposed rule that would cut $320 million in Medicare Part A payments to nursing homes in fiscal 2023. The cut is meant to offset an unintended increase in payments during fiscal 2020 related to the transition to the Patient Driven Payment Model. The proposed rule also seeks feedback on establishing minimum staffing requirements for nursing homes and includes a plan to add three measures to the Skilled Nursing Facility Value-Based Purchasing Program. Read More
MedPAC Suggests Reducing Number of Risk Tracks in Medicare Alternative Payment Models. Modern Healthcare reported on April 8, 2022, that the Medicare Payment Advisory Commission (MedPAC) wants to streamline Medicare alternative payment models by reducing the number of risk tracks from seven to three. Sample tracks might be 50 percent upside-only shared savings for small organizations, 75 percent upside and downside shared savings for mid-sized organizations, and 100 percent upside and downside shared savings for large organizations. The proposed models, which would apply to the Medicare Shared Savings program and ACO REACH model, will be finalized in MedPAC’s June report. Read More
Industry News
Not-for-profit Hospitals Receive More in Tax Breaks Than They Spend on Charity Care, Study Says. Fierce Healthcare reported on April 12, 2022, that most non-profit hospital systems in the U.S. spent billions of dollars less on charity care and community investments than they received in tax breaks in 2018-19, according to a Lown Institute study. Hospitals dispute Lown’s findings. Read More
Enhanced Healthcare Partners Invests in Vytalize Health. Private equity firm Enhanced Healthcare Partners announced on April 13, 2022, an investment in Vytalize Health, a value-based care platform for primary care practices. Vytalize serves 280 primary care practices across 16 states. Read More
Genuine Health Group Acquires Accountable Care Medical Group. Genuine Health Group announced on April 7, 2022, the acquisition of Accountable Care Medical Group, a Florida-based provider group that operates accountable care organizations. Genuine Health has also recently acquired provider organizations Premier Care Associates and PreventiMed. Crestline Investors provided $160 million in September, which funded the acquisitions. Read More
Former Centene CEO Michael Neidorff Dies at 79. Forbes reported on April 7, 2022, that Michael Neidorff, the 79-year-old former chief executive of Centene, has died. Neirdorff had been head of Centene since 1996, before taking a medical leave of absence in February. Read More
CVS Health/Aetna Spends $185 Million to Support Affordable Housing in 5 States, DC in 2021. Health Payer Specialist reported on April 6, 2022, that CVS Health/Aetna spent $185 million supporting affordable housing in five states and Washington, DC, in 2021, up from $114 million in 2020. CVS Health/Aetna said it has spent $1.2 billion on social determinants of health over the past 20 years. Read More
Help at Home Acquires Edison Home Health Care, Preferred Home Care of New York. Help at Home announced on April 6, 2022, the acquisition of New York-based Edison Home Health Care and Preferred Home Care of New York, both of which provide home and community-based services in New York and Pennsylvania. The acquisitions add a combined 10,500 clients and 12,000 employees to Help at Home. Read More
RFP Calendar
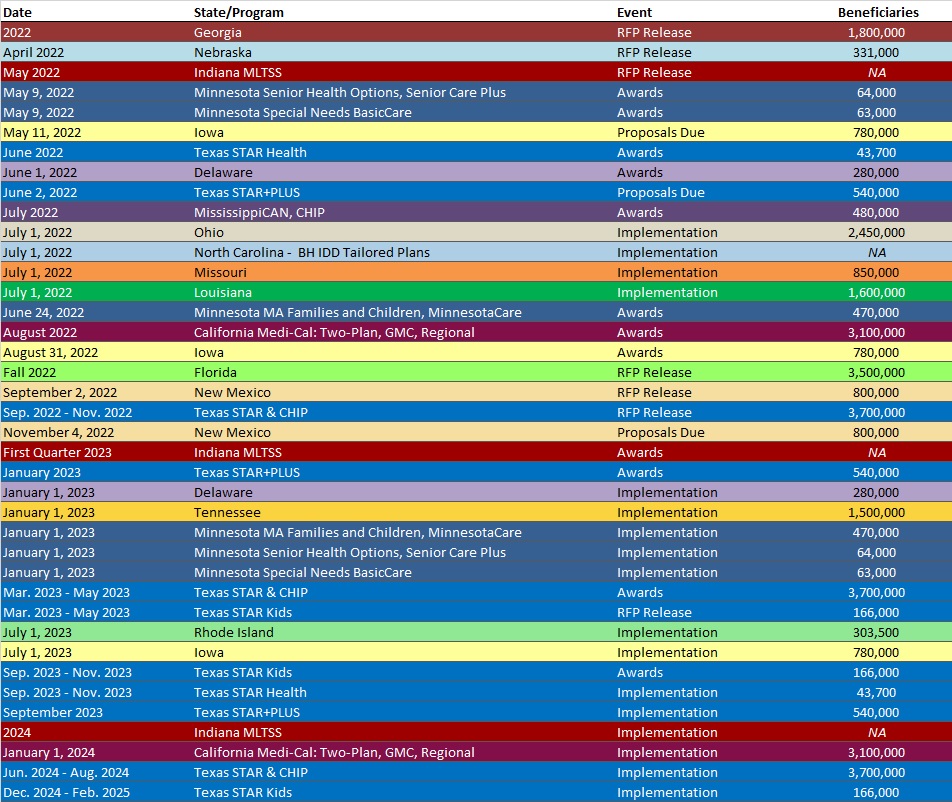
HMA News & Events
Illinois Action Plan Highlights HMA Substance Use Disorder Program. As part of an overall state strategy to reduce overdose deaths, Illinois recently released the State Overdose Action Plan (SOAP) that includes a key substance use disorder (SUD) program developed by HMA. HMA is working with the Illinois Division of Substance Use Prevention and Recovery (SUPR) to implement The Learning Collaborative to Support Medication Assisted Recovery (MAR) Implementation for Justice-Involved Individuals program. The program brings together criminal justice healthcare and custodial staff, drug court staff, county SUD and behavioral health programs, and county administrators to form an integrated learning collaborative and help jails develop the capacity to provide MAR in the jail. Read More
New This Week On HMA Information Services (HMAIS):
Medicaid Data
- Hawaii Medicaid Managed Care Enrollment is Up 12.1%, Nov-21 Data
- Hawaii Medicaid Managed Care Enrollment is Up 12.5%, 2021 Data
- Illinois Dual Demo Enrollment is Up 48.8%, 2021 Data
- Illinois Medicaid Managed Care Enrollment is Up 8.2%, 2021 Data
- Indiana Medicaid Managed Care Enrollment Is Up 2.6%, Feb-22 Data
- Iowa Medicaid Managed Care Enrollment is Up 2.3%, Mar-22 Data
- Maryland Medicaid Managed Care Enrollment Is Up 0.9%, Feb-22 Data
- Oklahoma Medicaid Enrollment is Up 2.4%, Feb-22 Data
- Pennsylvania Medicaid Managed Care Enrollment is Up 1.4%, Feb-22 Data
- Texas Dual Demo Enrollment is 36,757, Nov-21 Data
- Texas Medicaid Managed Care Enrollment is Up 10.7%, Nov-21 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Massachusetts MassHealth ACO RFR, Apr-22
Medicaid Program Reports, Data and Updates:
- Colorado Health Care Policy & Financing Performance Plan, FY 2020-22
- Georgia Plan for HCBS Implementation of the American Rescue Plan Act, 2021-22
- Louisiana Medicaid Financial Forecast Reports, SFY 2018-22
- Pennsylvania MLTSS Subcommittee Meeting Materials, 2021-22
- Texas OIG Quarterly Reports, 2019-22
- Vermont Medicaid HEDIS Scorecard, 2021
A subscription to HMA Information Services puts a world of Medicaid information at your fingertips, dramatically simplifying market research for strategic planning in healthcare services. An HMAIS subscription includes:
- State-by-state overviews and analysis of latest data for enrollment, market share, financial performance, utilization metrics and RFPs
- Downloadable ready-to-use charts and graphs
- Excel data packages
- RFP calendar
If you’re interested in becoming an HMAIS subscriber, contact Carl Mercurio.
