This week's roundup:
- In Focus: CMS Plans to Improve Incentives for Medicare Providers in Accountable Care Arrangements
- California Exchange Plan Premium Hikes Softened by State Financial Support
- Medicaid Eligibility Redeterminations News: Indiana, Massachusetts, Minnesota, Montana, Washington, West Virginia, Wisconsin
- Molina Healthcare Names Aaron Dunkel as President of Kansas Operations
- Michigan Ends Cost Sharing in Medicaid Expansion Program
- Nevada Releases Medicaid Managed Care RFI
- Oklahoma Health Care Authority CEO Kevin Corbett to Resign
- Medicaid Disenrollment Rates Vary Widely Among States, Report Finds
- Community Health Systems to Sell Three Hospitals to Tampa General Hospital in $290 Million Deal
- United’s Optum Health Names Amar Desai as CEO
In Focus
CMS Plans to Improve Incentives for Medicare Providers in Accountable Care Arrangements
This week, our In Focus section is the second in a summer series of analysis and insights from Health Management Associates (HMA) on recent Medicare payment and policy developments. This week we dig deeper into the potential changes to the Medicare Shared Savings Program (MSSP) that were included in the 2024 Medicare Physician Fee Schedule proposed rule released earlier this month. Specifically, we highlight the impact these modifications could have on financial and operational decisions across the healthcare industry.
The proposed rule builds on the changes CMS finalized last year with the goal of increasing participation in the MSSP. The recommended changes are designed to appeal to more clinicians who treat a high proportion of underserved individuals. CMS estimates that the proposal will increase participation in MSSP by 10−20 percent. These changes are technical in nature and include:
- Expanding the physician lookback window for beneficiary assignment (also known as the pre-step) for primary care service to 24 months from 12 months
- Adding a third step to the claims-based beneficiary assignment methodology to recognize the role of nurse practitioners (NPs), physician assistants (PAs), and clinical nurse specialists (CNSs) in delivering primary care services
- Modifying the definition of “assignable beneficiary” to reflect the changes above
The overall impact of these modifications, which augment the existing methodology, is to increase the number of beneficiaries assigned to accountable care organizations (ACOs) under MSSP. More assignable beneficiaries could mean:
- More ACOs will meet minimum beneficiary requirements.
- Changes in assignable population may affect the hierarchical condition category (HCC) risk scores for the national assignable population, as well as the factors used to normalize risk scores and other risk adjustments.
- Changes in population distribution within regions that result in adjustments to ACO market share, benchmark trends, and update factors.
For ACOs participating in multiple programs, expanded assignment rules for MSSP, combined with the MSSP superseding other programs in assignment, may have downstream effects on programs in terms of assignment and performance.
Following is a more detailed explanation of the proposed changes.
24-Month Lookback for Primary Care Services
Extending the lookback for primary care services with a physician to 24 months from 12 will allow providers to capture additional primary care services codes related to the COVID-19 public health emergency (PHE) for benchmark and performance years. If the assignment window for a benchmark or performance year includes any month(s) during the PHE, then the additional primary care services codes must apply to all months in that window.
Three-Step Assignment Process
CMS plans to update its current two-step claims-based beneficiary assignment process to a three-step process, which would be effective for performance years beginning January 1, 2025. The proposed third step only would apply to beneficiaries who do not meet the pre-step requirement contingent upon whether they received at least one primary care service during the expanded window for assignment from an ACO-participating primary care or specialist physician or received at least one primary care service from a non-physician ACO healthcare professional during the 12-month assignment window.
Assignable Beneficiary Definition
The proposed rule includes updates to the definition of an assignable beneficiary to reflect the expanded 24-month lookback window for assignment and the new third step of a primary care service within the 12-month assignment window from a non-physician ACO professional (i.e., NP, PA, CNS).
The table below compares the current and proposed assignment processes.
Comparison of the Two- and Three-Step Processes
| Step | Current Two-Step Beneficiary Assignment Process | Proposed Three-Step Beneficiary Assignment Process |
| Pre-Step Requirement to Identify Assignable Beneficiary | CMS identifies beneficiaries who received at least one primary care service from a primary care physician or a physician with a primary specialty designation participating in an ACO in the 12-month lookback window. CMS determines whether these individuals are eligible for assignment to an ACO. | CMS identifies beneficiaries who received at least one primary care service from a primary care physician or a physician with a primary specialty designation participating in an ACO in the 24-month lookback window. |
| Step 1
|
Determine if beneficiaries received the plurality of their primary care services from primary care physicians, NPs, PAs, and CNSs in the participating ACO. | No change |
| Step 2 | If not assigned in Step 1, determine whether beneficiaries received the plurality of primary care services from specialists in the participating ACO. | No change |
| Step 3 | Not applicable | For beneficiaries not assigned through Steps 1 and 2:
· Determine if beneficiary received at least one primary care service with a non-physician ACO professional (e.g., NP, PA, or CNS) in the ACO during the applicable 12-month assignment window; AND · Confirm beneficiary received at least one primary care service with a primary care physician or specialist who is an ACO professional in the ACO and who is a primary care physician or a non-physician ACO professional (i.e., NP, PA, CNS) during the applicable 12- month expanded window for assignment. |
Financial Considerations
The proposed rule outlines that the expenditure lookback will remain 12 months. With a 24-month primary care service window and a 12-month expenditure lookback, ACO revenues could change. As a result, minimum savings rates could drop and the per-member per-month amount might change. In addition, the extended lookback could affect the regional average risk-adjusted spending, expenditure thresholds, and more.
Enhanced MSSP Track
CMS is seeking comment on a new track in MSSP with a higher level of risk and potential reward (e.g., somewhere between 80−100 percent). The purpose of the new MSSP track is to encourage ACOs that would not have otherwise participated in MSSP because of limitations on upside rewards. Higher potential rewards may also incentivize ACOs to develop new strategies, focus on specialty care integration, and reduce healthcare fragmentation to achieve savings.
CMS is seeking comment on the following:
- Policy/model design elements that could be implemented so that CMS could offer a higher risk track without increasing program expenditures
- Approaches to protect ACOs that serve high-risk beneficiaries from expenditure outliers and reduce incentives for ACOs to avoid high-risk beneficiaries
- The impact that higher risk sharing could have on care delivery redesign, specialty integration, and ACO investment in healthcare providers and practices
The HMA Medicare and value-based care experts will continue to analyze these proposals alongside other policy and reimbursement changes that affect Medicare providers. We have the depth and breadth of expertise to assist with tailored analysis, to model policy impacts, and to support clients that intend to draft comment letters on this proposed rule. For more information or questions about these policies and other changes in the 2024 Medicare physician fee schedule proposed rule, contact Amy Bassano ([email protected]), Andrea Maresca ([email protected]), and Melissa Mannon ([email protected]).
HMA Roundup
Alaska
Alaska Extends Postpartum Coverage to 12 Months. KINY Radio reported on July 19, 2023, that Governor Mike Dunleavy signed legislation extending postpartum Medicaid coverage to 12 months and raising the income eligibility threshold for pregnant women on Medicaid from 200 percent of poverty to 225 percent. The change will add about 450 pregnant women to Medicaid in the state annually.
Arkansas
Arkansas to Allocate $2 Million to Assisted Living Facilities. The Arkansas Advocate reported on July 21, 2023, that the Arkansas Department of Human Services (DHS) will allocate $2 million in federal pandemic relief funds to Medicaid assisted living facilities in the Living Choices Assisted Living Waiver. Facilities will need to submit detailed cost reports to DHS in order to participate. Read More
California
California Exchange Plan Premium Hikes Softened by State Financial Support. Becker’s Payer Issues reported on July 24, 2023, that California will eliminate deductibles and reduce copays for some Covered California Exchange plans through an $82.5 million state-funded initiative. The initiative is meant to offset Exchange plan premium increases averaging 9.6 percent in 2024.
Managed Care Tax to Boost Medicaid Reimbursement Rates for Providers. KFF Health News reported on July 21, 2023, that California will direct a majority of the money generated from the renewal of a managed care tax to increase Medicaid reimbursement rates for providers. An estimated $19.4 billion will be generated between 2023 and 2026, with $11.1 billion going directly to Medi-Cal and $8.3 billion going to the general fund to offset state Medicaid spending. Industry leaders are hoping to lock in a rate increase through a 2024 ballot initiative. Read More
Connecticut
Connecticut Allows Nursing Homes to Retain, Reinvest Medicaid Savings. JD Supra reported on July 20, 2023, that Connecticut Governor Ned Lamont signed legislation allowing not-for-profit nursing homes to retain Medicaid savings, provided the funds are reinvested in “strengthening quality, investing in deferred maintenance, and making asset improvements.” Read More
Indiana
Indiana Disenrolls 35,595 Medicaid Beneficiaries Following June Redeterminations. Indiana Capital Chronicle reported on July 25, 2023, that Indiana disenrolled 35,595 Medicaid enrollees during June redeterminations. Of those disenrolled, 30,751 lost coverage for procedural reasons and the remaining 4,844 were deemed ineligible. In April, Indiana had 52,985 disenrollments, followed by 53,684 in May. Read More
Kansas
Molina Healthcare Names Aaron Dunkel as President of Kansas Operations. Health Payer Specialist reported on July 24, 2023, that Molina Healthcare has named Aaron Dunkel as president of the company’s Kansas operations, in part to lead the organization’s efforts to win a Medicaid managed care contract in the state for 2025. Dunkel was most recently executive director of the Kansas Pharmacists Association and previously served with the Kansas Department of Health and Environment. Read More
Massachusetts
Massachusetts Disenrolls More Than 33,000 Medicaid Beneficiaries During June Redeterminations. WBZ News Radio reported on July 26, 2023, that Massachusetts has disenrolled more than 33,000 Medicaid beneficiaries during June redeterminations. Nearly 70 percent of those removed were found ineligible. Around 12,300 were disenrolled for failing to provide requested information, and another 2,500 failed to respond at all. Read More
Massachusetts Releases Quality, Training RFR for Children’s Behavioral Health Initiative. The Massachusetts Executive Office of Health and Human Services (EOHHS) released on July 24, 2023, a request for responses (RFR) for a vendor to support training and quality efforts in the MassHealth Children’s Behavioral Health Initiative (CBHI). Responses are due August 11. CBHI covers an enhanced continuum of home and community-based behavioral health services, requires primary care physicians to screen children for behavioral health conditions, and standardizes behavioral health assessments. Read More
Michigan
Michigan Ends Cost Sharing in Medicaid Expansion Program. Crain’s Detroit Business reported on July 19, 2023 that Michigan Governor Gretchen Whitmer enacted legislation that ends cost sharing in the state’s Medicaid expansion program, Healthy Michigan. State data suggest that less than 25 percent of copays and contributions have been collected. Read More
Minnesota
Minnesota Extends Deadline for July Medicaid Eligibility Renewal Forms. The Minnesota Department of Human Services announced on July 26, 2023, that it has extended the deadline for Medicaid eligibility renewal forms originally due on July 31 until the end of August. Individuals who have already been determined to be ineligible will still lose coverage on August 1. Read More
Montana
Montana Disenrolls 19,244 Medicaid Beneficiaries During May Redeterminations. The Montana Free Press reported on July 24, 2023, that Montana disenrolled 19,244 Medicaid enrollees during May redeterminations. Another 9,919 enrollees were still being processed. The state renewed coverage for 11,171 beneficiaries. Read More
Nevada
Nevada Releases Medicaid Managed Care RFI. The Nevada Department of Health and Human Services released on July 25, 2023, a request for information (RFI) for the state’s next Medicaid managed care procurement. Incumbents are Centene, Elevance/Anthem, Molina, and United. Responses are due on October 10, 2023. Read More
New Hampshire
New Hampshire Seeks Counties to Pilot Community Programs Aimed at Helping Dual Eligibles Avoid Institutional Care. The New Hampshire Department of Health and Human Services, Division of Long-Term Services and Supports, released on July 26, 2023, a request for proposals (RFP) seeking counties to pilot comprehensive community-based care systems aimed at helping Medicare-Medicaid dual eligibles avoid entering institutional care. The state released a second RFP seeking a vendor to study whether such an initiative is feasible in New Hampshire.
New York
New York Section 1115 Waiver Amendment to Include Plan to Invest in Primary Care. Crain’s New York Business reported on July 21, 2023, that New York is working on a Section 1115 Medicaid waiver amendment that will likely include a plan to invest in primary care and to move forward with value-based payment models. The state is currently in negotiations with the Centers for Medicare & Medicaid Services to finalize the amendment, which also includes housing, nutrition, and transportation initiatives. Read More
New York Provides $3.5 Million to Create 13 Additional CCBHCs. Crain’s New York Business reported on July 21, 2023, that New York state will provide $3.5 million to create 13 additional certified community behavioral health clinics (CCBHCs). The state currently has 13 CCBHCs and plans to have 39 by 2025. Read More
North Carolina
North Carolina Governor Urges Lawmakers to Implement Medicaid Expansion, Pass Fiscal 2024 Budget. North Carolina Governor Roy Cooper released on July 20, 2023, a statement urging state lawmakers to implement Medicaid expansion by passing the fiscal 2024 budget. The state enacted Medicaid expansion legislation in March, with a provision delaying implementation until a budget is adopted. The Governor has previously urged lawmakers to separate expansion from the budget. Read More
Ohio
Ohio Representative Introduces Legislation to Support Self-Directed Medicaid Services. WFMJ reported on July 19, 2023, that Ohio State Representative Al Cutrona (R-Canfield) has introduced legislation to broaden the use of self-directed Medicaid services. Read More
Oklahoma
Oklahoma Health Care Authority CEO Kevin Corbett to Resign. The Oklahoma Health Care Authority (OHCA) announced on July 19, 2023, the resignation of chief executive Kevin Corbett, effective July 31, 2023, or until a successor is appointed. Corbett, who has headed OHCA since 2019, had simultaneously served as state secretary of Health and Mental Health and led the state’s transition to Medicaid managed care. Read More
Pennsylvania
Pennsylvania to Receive $42 Million in Federal ‘Money Follows the Person’ Funding. The Pennsylvania Department of Health Services announced on July 21, 2023, that the state will receive approximately $42 million in federal funding through the Money Follows the Person program, which supports community-based healthcare services for individuals who are elderly or disabled. The program has helped over 6,000 individuals transition from institutional care to community services in Pennsylvania since 2008. Read More
Virginia
Virginia to Release Medicaid Managed Care Request for Proposals on August 1. Virginia has indicated that a request for proposals (RFP) for its Medicaid managed care program will be released on August 1. Incumbents are Aetna, Elevance/Anthem, Molina, Sentara Healthcare/Optima/Virginia Premier, and UnitedHealthcare. Read More
Virginia Paid Insurers Nearly $22 Million to Cover Deceased Medicaid Enrollees, Audit Finds. The Richmond Times-Dispatch reported on July 24, 2023, that Virginia paid managed care companies nearly $22 million to cover approximately 12,000 deceased Medicaid enrollees from 2019 through 2021, according to a federal audit. The audit recommended that Virginia recover payments, refund the federal share, and improve its Medicaid eligibility system, which the state says it is already in the process of doing. Read More
Washington
Washington Disenrolls 114,000 Medicaid Beneficiaries During June Redeterminations. State of Reform reported on July 21, 2023, that Washington disenrolled about 114,000 Medicaid beneficiaries during June redeterminations. Read More
West Virginia
West Virginia Disenrolls 61,813 Medicaid Enrollees Following Redeterminations. MetroNews reported on July 23, 2023, that West Virginia has disenrolled 61,813 Medicaid beneficiaries since eligibility redeterminations began in April. More than 36,500 of the disenrollments were for procedural reasons. Read More
Wisconsin
Wisconsin Disenrolls 60,500 Medicaid Beneficiaries During June Redeterminations. The Milwaukee Journal Sentinel reported on July 21, 2023, that Wisconsin disenrolled more than 60,500 Medicaid beneficiaries during June redeterminations. The state renewed coverage for more than 29,300 beneficiaries. Read More
National
CMS Approves Use of Mobile Crisis Intervention Teams for Medicaid Crisis Services in California, Kentucky. The Centers for Medicare & Medicaid Services (CMS) announced on July 20, 2023, approval of proposals from California and Kentucky to provide Medicaid crisis services using community-based mobile crisis intervention teams. There are now six states that have expanded access to community-based mental health and substance use crisis care through the American Rescue Plan. Read More
AHIP, Provider Groups to Partner on Best Practices Playbook for Value-based Care. Health Payer Specialist reported on July 26, 2023, that insurer group AHIP has partnered with the American Medical Association and the National Association of Accountable Care Organizations to develop a best practices playbook for the design and implementation of value-based care arrangements. The initial focus will be data collection and sharing, followed by payment methodologies, care coordination, quality, patient engagement, and delivery of care. Read More
CMS Releases Guide to Improving Access, Treatment of Mental Health, Substance Use Disorder for Medicaid, CHIP Members. The Centers for Medicare & Medicaid (CMS) released on July 25, 2023, the Medicaid and CHIP Mental Health (MH) and Substance Use Disorder (SUD) Action Plan Overview and Guide, which outlines strategies to improve services and support for individuals with these conditions. The plan focuses specifically on broadening access to prevention and treatment services, increasing the availability of home and community based services and improving quality of care for individuals with MH conditions and SUD. Read More
New Rules to Require Insurers to Study, Remedy Any Lack of Parity Between Physical, Behavioral Access. The Associated Press announced on July 25, 2023, that the Biden Administration has proposed regulations requiring insurers to study whether members have equal access to physical and behavioral health care and to remedy any shortfalls. The rules are intended to increase access to behavioral health services by reinforcing compliance with the Mental Health Parity and Addiction Equity Act. The regulations will be subject to 60 days of public comment. Read More
CMS Releases 2021 Medicaid Managed Care Enrollment, Program Characteristics Information. CMS announced on July 25, 2023, the release of the 2021 Medicaid Managed Care Enrollment and Program Characteristics and Data Tables. Enrollment data is broken down by program, population, and state. The data reflects annual enrollment as of July 1. Read More
Hospitals Urge Congress to Further Delay Cuts to Medicaid Disproportionate Share Hospital Payments. KFF Health News reported on July 25, 2023, that hospitals are asking Congress to once again delay scheduled cuts to the Medicaid Disproportionate Share Hospital (DSH) payments program. The cuts, mandated by the Affordable Care Act, would be $8 billion annually for four years unless Congress acts by October. Read More
Medicaid Disenrollment Rates Vary Widely Among States, Report Finds. Becker’s Payer Issues reported on July 24, 2023, that Medicaid disenrollment rates vary widely from state to state, according to a report from KFF. The report, which analyzed 32 states and DC, found that rates ranged from 82 percent in Texas to 10 percent in Michigan. The differences may be in part because some states are focusing early redeterminations efforts on individuals likely to be no longer eligible, the report says. Read More
House Passes CHOICE Bill Targeting Cost of Health Insurance, Expanding Association Plans. Modern Healthcare reported on July 24, 2023, that the House passed a bill aimed at reducing the costs of health insurance in part by expanding access to association health plans, allowing employers to fund Health Reimbursement Accounts, and loosening employer self-insurance rules. The Custom Health Option and Individual Care Expense (CHOICE) Arrangement Act, which is sponsored by Representative Kevin Hern (R-OK), will likely face Democratic opposition in the Senate because it would loosen consumer protections and bypass basic benefits rules. Read More
340B Remedy Payments Proposal Would Favor Hospitals Providing Less Uncompensated Care, Analysis Shows. Modern Healthcare reported on July 24, 2023, that hospitals providing less uncompensated care would receive the largest payments under a proposed plan to remedy prior cuts in the 340B drug program, according to a Modern Healthcare analysis. The Centers for Medicare & Medicaid Services would pay 1,600 hospitals about $9 billion under the plan. Read More
Johnson & Johnson Files Federal Lawsuit Opposing Medicare Drug Negotiations. The New York Times reported on July 23, 2023, that Johnson & Johnson filed a federal lawsuit to block the Biden administration’s plan to begin Medicare drug price negotiations, arguing the plan is unconstitutional. Merck, Bristol Myers Squibb, and Astellas Pharma have filed similar lawsuits. Read More
Biden Administration Turns to Employers to Help Offset Impact of Medicaid Coverage Losses. Modern Healthcare reported on July 20, 2023, that the Biden Administration has asked employers to give workers who lose Medicaid coverage more time to apply for employer-sponsored health insurance. Specifically, the administration is asking employers, insurers, and plan sponsors to extend the typical 60-day window for sign ups through July 31, 2024. Read More
Joint Commission Further Trims Accreditation Standards. Modern Healthcare reported on July 20, 2023, that the Joint Commission is removing 200 more standards from its accreditation programs. The changes are effective August 27, 2023. Read More
Senators Introduce PBM Oversight Bill. The Hill reported on July 20, 2023, that Senators Tom Carper (D-DE) and Chuck Grassley (R-IA) introduced legislation aimed at increasing oversight of pharmacy benefit managers (PBMs), including pricing and formulary decisions. Read More
CMS Orders Several States to Pause Medicaid Eligibility Redeterminations. Modern Healthcare reported on July 20, 2023, that the Centers for Medicare & Medicaid Services (CMS) has ordered several states to pause Medicaid eligibility redeterminations and is working with about six states to correct ongoing violations of federal standards. CMS did not name the states. Read More
MACPAC Supports Proposed Medicaid Drug Rebate Program Rule. The Medicaid and CHIP Payment and Access Commission (MACPAC) submitted comments in July 2023 supporting a proposed Medicaid Drug Rebate Program rule. The proposed rule, from the Centers for Medicare & Medicaid Services, is designed to clarify definitions, increase price transparency, and address drug misclassifications. Read More
Industry News
Community Health Systems to Sell Three Hospitals to Tampa General Hospital in $290 Million Deal. Modern Healthcare reported on July 25, 2023, that Community Health Systems will sell three Florida hospitals to Tampa General Hospital in a deal estimated at $290 million. The transaction is expected to be finalized later this year, subject to regulatory approval. Read More
Acadia Healthcare, Nebraska Methodist Form Joint Venture. Acadia Healthcare Company announced on July 24, 2023, that it has formed a joint venture with Nebraska Methodist Health System to build a 96-bed behavioral health hospital serving metro Omaha-Council Bluffs, IA. The hospital will be affiliated with Methodist Jennie Edmundson Hospital. Read More
United’s Optum Health Names Amar Desai as CEO. Modern Healthcare reported July 19, 2023 that United’s Optum Health has named Amar Desai, MD, as chief executive, effective immediately. He replaces Wyatt Decker, who was named UnitedHealth Group’s chief physician for value-based care. Desai returns to Optum after a stint at CVS Health. Read More
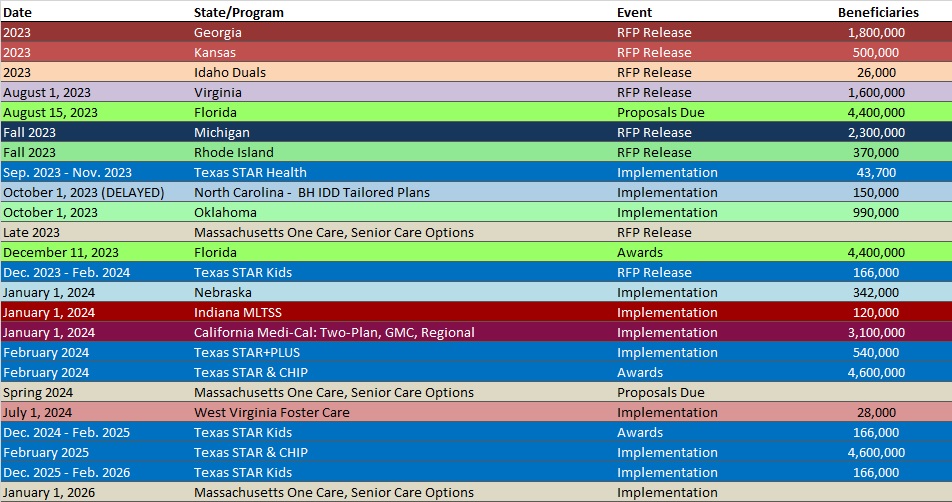
RFP Calendar
HMA News & Events
Upcoming HMA Conference:
HMA Conference Early Bird Rate to Expire July 31. The Early Bird rate of $1,695 per person to register for the sixth annual HMA conference in Chicago, October 30-31, will expire on July 31. After that the rate goes to $1,895. This year’s conference, Innovations in Publicly Sponsored Health Care: How Medicaid, Medicare, and Marketplaces Are Driving Value, Equity, and Growth, will take place at the Fairmont Chicago Millennium Park. Last year’s HMA conference attracted 500 attendees. View the entire agenda and register.
Upcoming HMA Webinar:
Medicaid 1115 Justice Waivers and Special Populations: Meeting the Needs of Justice-Involved Youth. Youth in detention often have complex medical, behavioral health, developmental, social, and legal needs and have been exposed to adverse childhood experiences. Part 5 of this series on 1115 Medicaid Justice Demonstration Waivers: Bridging Healthcare, will delve into differences of care and services for youth so that a whole-person approach can be applied to their successful reentry to the community. Thursday, August 17, 2 pm ET. Click here to register.
NEW THIS WEEK ON HMA INFORMATION SERVICES (HMAIS):
Medicaid Data
Medicaid Enrollment:
- Arizona Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Arkansas Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Connecticut Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- District of Columbia Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Hawaii Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Iowa Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Kansas Medicaid Managed Care Enrollment is Down 7.6%, Jun-23 Data
- Kansas Medicaid Managed Care Enrollment is Down 6.5%, May-23 Data
- Kansas Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Kentucky Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Maine Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Massachusetts Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Michigan Medicaid Managed Care Enrollment is Up 1.2%, Apr-23 Data
- Michigan Dual Demo Enrollment is Down 1.2%, Apr-23 Data
- Michigan Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Minnesota Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Mississippi Medicaid Fee for Service vs. Managed Care Penetration, 2014-21
- Nevada Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- New Hampshire Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- New Mexico Medicaid Fee for Service vs. Managed Care Penetration, 2014-22
- Oklahoma Medicaid Enrollment is Up 0.9%, Jun-23 Data
Public Documents:
Medicaid RFPs, RFIs, and Contracts:
- Massachusetts Children’s Behavioral Health Initiative Support Services RFR, Jun-23
- Nevada Medicaid Managed Care RFI, Jul-23
- New Hampshire County Pilot to Delay or Defer Institutional Care RFP, Jul-23
- New Hampshire Feasibility Study to Develop Programming that Defers and Delays Institutional Care for Dual Eligible Individuals RFP, Jul-23
- Utah Medicaid Dental Services RFP and Award, 2022
Medicaid Program Reports, Data, and Updates:
- California PHE Medicaid Redeterminations Monthly Reports to CMS, May-23
- District of Columbia Medicaid Renewal Community Meeting Presentations, Jul-23
- Indiana PHE Medicaid Redeterminations Monthly Report to CMS, Jun-23