This week we reviewed two active Medicaid managed care procurements – in the District of Columbia and Massachusetts – and a Medicaid managed care request for information issued by Texas. On December 22, 2016, the District of Columbia issued a request for proposals (RFP) to rebid Medicaid managed care organization (MCO) contracts for the DC Healthy Families and Alliance programs. One day prior, on December 21, 2016, Massachusetts issued a request for responses (RFR) from MCOs interested in participating in the MassHealth managed care program, with a focus on preparing for Medicaid ACO implementation, as well as the planned carve-in of managed long-term services and supports (MLTSS). Finally, also on December 22, 2016, Texas issued a request for information (RFI) ahead of an upcoming statewide reprocurement of the STAR+PLUS Medicaid managed care program.
DC Healthy Families, Alliance Program RFP
On December 22, 2016, the District of Columbia’s Department of Health Care Finance (DHCF) issued a request for proposals (RFP) to rebid the District’s Medicaid managed care organization (MCO) contracts. The awarded contracts will provide Medicaid managed care to most Medicaid and CHIP-eligible beneficiaries under the DC Healthy Families Program, as well as residents with incomes below 200 percent of the federal poverty level (FPL) who are not eligible for Medicaid under the DC Alliance Program. Finally, contracted MCOs will also provide coverage to the Immigrant Children’s Program for eligible individuals age 21 or younger, up to 300 percent of FPL, who are not eligible for Medicaid due to citizenship or immigration status. As of July 2016, more than 167,000 Medicaid beneficiaries and over 12,000 Alliance beneficiaries were enrolled with a MCO. HMA-collected figures put June 2016 enrollment at 174,200 in DC Healthy Families and 12,300 in the Alliance program.
Scope of RFP
Based on June 2016 enrollment data and the rate analysis provided by DHCF, annualized spending for the DC Healthy Families Program and Alliance Program under the RFP exceeds $860 million, based on more than 174,000 DCHFP members and more than 12,300 Alliance members. This equates to a blended per-member-per-month (PMPM) rate of more than $380.
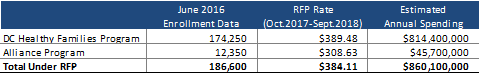
Source: HMAIS Data; Mercer Analysis for DHCF.
RFP Timing
The District issued the RFP on December 22, 2016, with proposals due to DHCF less than three weeks later, on January 11, 2017. Based on this accelerated timeline, the District may be favoring incumbent health plans. However, DHCF indicated at the December 29, 2016, bidders’ conference that the due date could be extended if potential bidders requested an extension. While no implementation date is specified, contract start dates would likely be tied to the District’s fiscal year, beginning October 1.
Term of Contract
DHCF will award contracts for an initial term of one year, with four optional one-year extensions. Total contract length will not exceed five years.
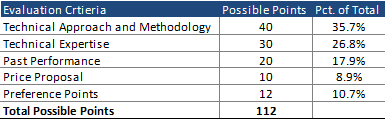
Evaluation Criteria
Responses will be primarily evaluated on technical criteria and past performance. Bidders are asked to provide a price bid based on actuarially sound rates set by DHCF. Additionally, entities that qualify as small, local, disadvantaged, or veteran-owned business can quality for additional “Preference” points.
Current Medicaid Managed Care Market
There are three MCOs currently serving the DCHFP and Alliance managed care programs, with AmeriHealth Caritas the largest, at nearly 55 percent of the market. Maryland-based MedStar, which also operates Medicaid health plans in Maryland, is owned by the MedStar Health System. Trusted Health Plan, formerly known as Thrive Health Plan, scored highest out of five total bidders in the 2013 RFP as a newly formed MCO. Unsuccessful bidders in 2013 included incumbent United Healthcare and Maryland-based Riverside Health.
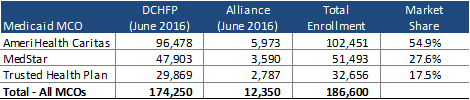
Source: HMAIS Data
MassHealth Managed Care Organization RFR
On December 21, 2016, the Massachusetts Executive Office of Health and Human Services (EOHHS) issued a request for responses (RFR) for Medicaid managed care organizations (MCOs) to serve MassHealth, the state’s Medicaid program, which operates under a Section 1115 Medicaid Demonstration waiver. Out of 1.8 million MassHealth members, around 1.3 million are served by one of four managed care programs: the MassHealth MCO Program; the Primary Care Clinician (PCC) Plan; the One Care program (the state’s capitated dual eligible Financial Alignment Demonstration; and the Senior Care Options (SCO) program. This RFR applies to the roughly 850,000 MassHealth MCO Program members.
MassHealth Managed Care Overview
As of September 2016, MassHealth reports indicated nearly 1.34 million MassHealth members were in some form of managed care. Of these just over 900,000 were in one of the three risk-based managed care programs that include the MassHealth MCO Program, SCO, and OneCare. The PCC program is an enhanced fee-for-service (FFS) program that provides a care coordination fee to primary care providers.
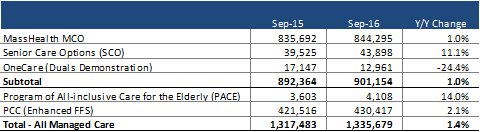
Source: MassHealth Enrollment Snapshot Report, September 2016
The MassHealth MCO Program covered under this RFR accounts for the majority of MassHealth managed care enrollment, covering children and adults through age 64, and includes individuals with disabilities. MassHealth members age 65 or older may voluntarily enroll in the SCO program or OneCare, dependent on eligibility. As noted above, this RFR does not include SCO or OneCare.
Scope of RFR
This RFR includes two notable changes under the MassHealth MCO program around the implementation of Medicaid Accountable Care Organization models and the carve-in of long-term services and supports (LTSS) benefits.
- Contracted MCOs will have new responsibilities and requirements around the support of the Medicaid ACO model implementation, detailed further below. The RFR specifically states the intention to support the uptake of Alternative Payment Models in the MassHealth MCO Program, including MCO-administered ACOs.
- Based on current timelines, MassHealth intends to add LTSS benefits for MassHealth MCO Program members around the start of 2020, around the third year of the contracts resulting from this RFR. There are roughly 63,000 members (7.5 percent) under age 65 in the MassHealth MCO Program who have a disability, as of September 2016. MassHealth has not provided spending or rate data for the RFR at this time, but based on some estimates of MassHealth LTSS spending from 2015, we estimate the potential impact of the LTSS carve-in at $900 million to $1.3 billion in annual managed care spending. FY 2015 spending for managed care capitation payments was approximately $4.3 billion.
Additionally, bidders have the option to submit a proposal to serve the Special Kids Special Care (SKSC) Program, which provides care to children (up to age 22 ½) who have complex health care needs. As of December 2016 there were 102 SKSC program members. While bidding on SKSC is not a prerequisite for bidding on the MassHealth MCO Program, plans may not submit a bid for the SKSC program only.
Medicaid ACO Model Overview
In preparation for the full launch of ACO models in 2017, MassHealth will conduct an ACO pilot with a small set of ACOs in 2016. In November 2016, MassHealth selected six provider networks to participate in a new accountable care organization (ACO) pilot program, initially covering around 160,000 members. Participants include some of the largest hospitals and health systems in the state, including Partners HealthCare, Steward Health Care System, UMass Memorial Health Care, Boston Medical Center, and Boston Children’s Hospital. Community Care Cooperative, a newly formed network of community health centers, will also participate in the ACO pilot.
The pilot will not change the payment model for any members that receive care and are currently enrolled in MCOs. Additionally, the pilot will utilize a retrospective shared savings and risk model for Primary Care Clinician (PCC) Plan members. The demonstration renewal plan offers flexibility for providers with three possible ACO models to choose from. The three models cater to a spectrum of provider capabilities.
| Model A: Integrated ACO/MCO model | Model B: Direct to ACO model | Model C: MCO-administered ACO model |
|---|---|---|
| Fully integrated: an ACO joins with an MCO to provide full range of services Risk-adjusted, prospective capitation rate ACO/MCO entity takes on full insurance risk | ACO provider contracts directly with MassHealth for overall cost/ quality Based on MassHealth/ MBHP provider network ACO may have provider partnerships for referrals and care coordination Advanced model with two-sided performance (not insurance) risk | ACOs contract and work with MCOs MCOs play larger role to support population health management Various levels of risk; all include two-sided performance (not insurance) risk |
In this new model, MCOs will be expected to take on additional roles. The expanded responsibility will include delivery and coordination of LTSS, facilitation of analytics and reports for population management, assisting ACOs in the integration of Behavioral Health Community Partners (BH CPs) and LTSS Community Partners.
RFP Timing
EOHHS issued the RFR on December 21, 2016, with proposals due on March 15, 2017. No target date has been set for contract award announcements. Implementation is tentatively set for December 18, 2017; however, timing may be dependent on contracting with Medicaid ACOs under a separate procurement.
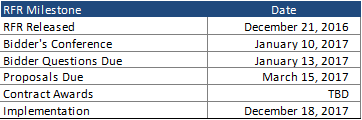
Contract Awards
EOHHS intends to contract with no more than three bidders per region, and bidders must propose to serve a minimum of two of the five managed care regions. Contract award preference may be given to plans who serve more regions, although it is not clear at this time whether all regions or a majority of regions would be needed to qualify for the preference.
Term of Contract
The initial contract term under this RFR is from approximately July 2017, or the date of execution, through December 31, 2022. Additionally, EOHHS may extend contracts for up to five additional years, through December 31, 2027.
Current Medicaid Managed Care Market
As of the end of 2015, Neighborhood Health Plan was the largest MCO in the state, with more than one-third of all members. Both Tufts Health Plan and Boston Medical Center Health Plan have market shares of 22 to 25 percent. MassHealth MCOs have reported financial issues in the past year, with both Neighborhood Health Plan (owned by Partners HealthCare) and Health New England’s parent company (Baystate Health) reporting significant financial losses in the second half of 2016. Neighborhood Health Plan temporarily froze enrollment in October 2016.
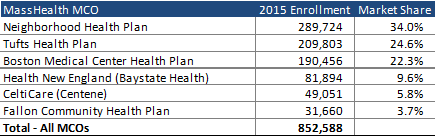
Source: HMAIS Data
Texas STAR+PLUS Medicaid Managed Care RFI
On December 22, 2016, The Texas Health and Human Services Commission (HHSC) released a Request for Information (RFI) for organizations interested in serving the STAR+PLUS Medicaid managed care program. STAR+PLUS members include adults with disabilities who meet a nursing facility level of care and require home and community based services. STAR+PLUS covers more than 540,000 Medicaid beneficiaries, accounting for more than $8 billion in annual spending, based on FY 2016 rates. The RFI seeks responses from interested organizations, particularly around improved strategies that are innovative, cost-effective, and improve outcomes in the delivery of acute care and long-term services and supports (LTSS). Responses and questions are due January 30, 2017.
On November 15, 2016, HHSC announced that it would be reprocuring STAR+PLUS contracts statewide, after previously announcing the upcoming RFP would be for the Dallas and Tarrant service areas only. HHSC will maintain existing service areas under the statewide RFP. The target implementation date for new STAR+PLUS contracts is January 1, 2019.
STAR+PLUS Overview
The STAR+PLUS Medicaid managed care program integrates the delivery of acute care services, pharmacy services, and long-term services and supports (LTSS) to individuals age 65 and older and to individuals under age 65 who have a disability, many of whom qualify for Supplemental Security Income (SSI) or SSI-related benefits. STAR+PLUS services and supports are delivered through five MCOs who contract with HHSC.
Enrollment in STAR+PLUS is mandatory for most adults receiving SSI, as well as adults who do not receive SSI (non-SSI), but who qualify for the STAR+PLUS HCBS program. Enrollment in STAR+PLUS was voluntary for children and young adults under the age of 21 who receive SSI and SSI-related Medicaid benefits until implementation of the STAR Kids managed care program on November 1, 2016. STAR+PLUS MCOs began covering most nursing facility services for members age 21 and older as of March 2015.
Current STAR+PLUS Medicaid Managed Care Market
As of September 2016, there were nearly 545,000 STAR+PLUS members across five MCOs. Centene’s Superior Health Plan, Anthem’s Amerigroup, and United Healthcare combine to cover nearly three quarters of all STAR+PLUS members. Both Superior and Amerigroup also have significant market presence in across all Medicaid managed care programs in the state. There are an additional 13 Medicaid MCOs who do not participate in the STAR+PLUS program.
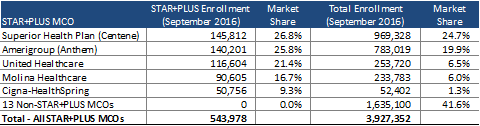
Source: HMAIS Data