This week, our In Focus section reviews the statewide North Carolina request for applications (RFA) for Behavioral Health and Intellectual/Developmental Disability (BH IDD) Tailored Plans released by the North Carolina Department of Health and Human Services (DHHS) on November 13, 2020. BH IDD Tailored Plans are part of the statewide effort to transition to Medicaid managed care and are one of the four types of integrated Medicaid managed care plans the state will contract with to serve Medicaid and NC Health Choice beneficiaries. The other three are Standard Plans, the Statewide Specialized Foster Care Plan, and the Eastern Band of Cherokee Indians Tribal Option.
BH IDD Tailored Plans will serve populations with severe behavioral health conditions, IDD, and traumatic brain injury (TBI), beginning July 1, 2022, across seven regions. Plans will coordinate physical health, behavioral health, long-term services and supports (LTSS), pharmacy services, and unmet health-related resource needs for members. Standard plans will serve less severe behavioral, IDD, and TBI populations. BH IDD Tailored Plans will also be responsible for managing these services to non-Medicaid underinsured and uninsured populations.
Only existing Local Management Entity-Managed Care Organizations (LME/MCOs), which currently cover behavioral health members in the state, can apply for the first round of BH IDD Tailored Plan contracts during the first four years, after which any non-profit PHP may also bid for a contract. LME/MCOs will only be able to apply to the regions they currently service; however, the state may provide an opportunity to be considered for an empty region.
The current LME/MCOs are:
- Alliance Behavioral Healthcare
- Cardinal Innovations Healthcare Solutions
- Eastpointe
- Partners Behavioral Health Management
- Sandhills Center
- Trillium Health Resources
- Vaya Health
Medicaid Transformation
North Carolina Medicaid, a predominantly fee-for-service model, will transition to managed care on July 1, 2021 after delays over funding and a failed attempt to include Medicaid expansion. The state awarded statewide contracts for the program to AmeriHealth Caritas North Carolina, Blue Cross and Blue Shield of North Carolina, UnitedHealthcare of North Carolina, and WellCare of North Carolina. A regional PHP contract was also awarded to provider-led Carolina Complete Health, a partnership between the North Carolina Medical Society and Centene.
Timeline
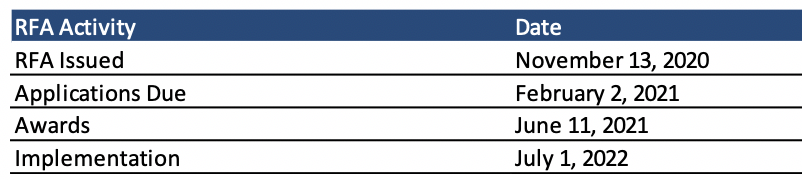
Applications for BH IDD Tailored Plans are due February 2, 2021, with contract awards expected on June 11, 2021. Implementation begins July 1, 2022.
Evaluation
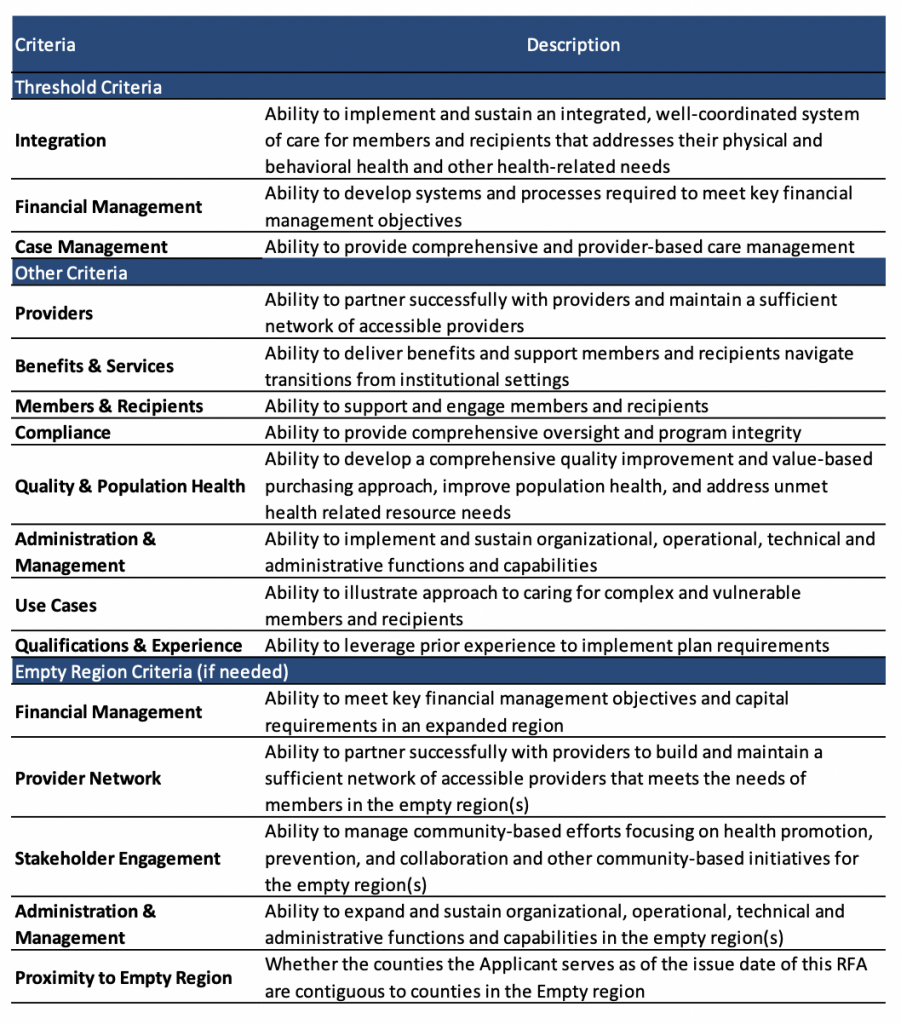
North Carolina will award five to seven regional contracts, ensuring BH I/DD Tailored Plan coverage in all counties. Applicants will first be evaluated on whether they meet the minimum qualifications then on their responses based on the criteria below.