On October 31, 2025, the Centers for Medicare & Medicaid Services (CMS) announced the final rule for the calendar year (CY) 2026 Medicare Physician Fee Schedule (PFS), which finalizes payment policies proposed earlier this year. The rule continues the administration’s focus on developing value-based payment strategies, enhancing care management, and developing innovative payment models. It emphasizes a shift from historical processes and methods of reimbursing clinician services, while also introducing payment policies that include a shift toward site neutrality and cost containment.
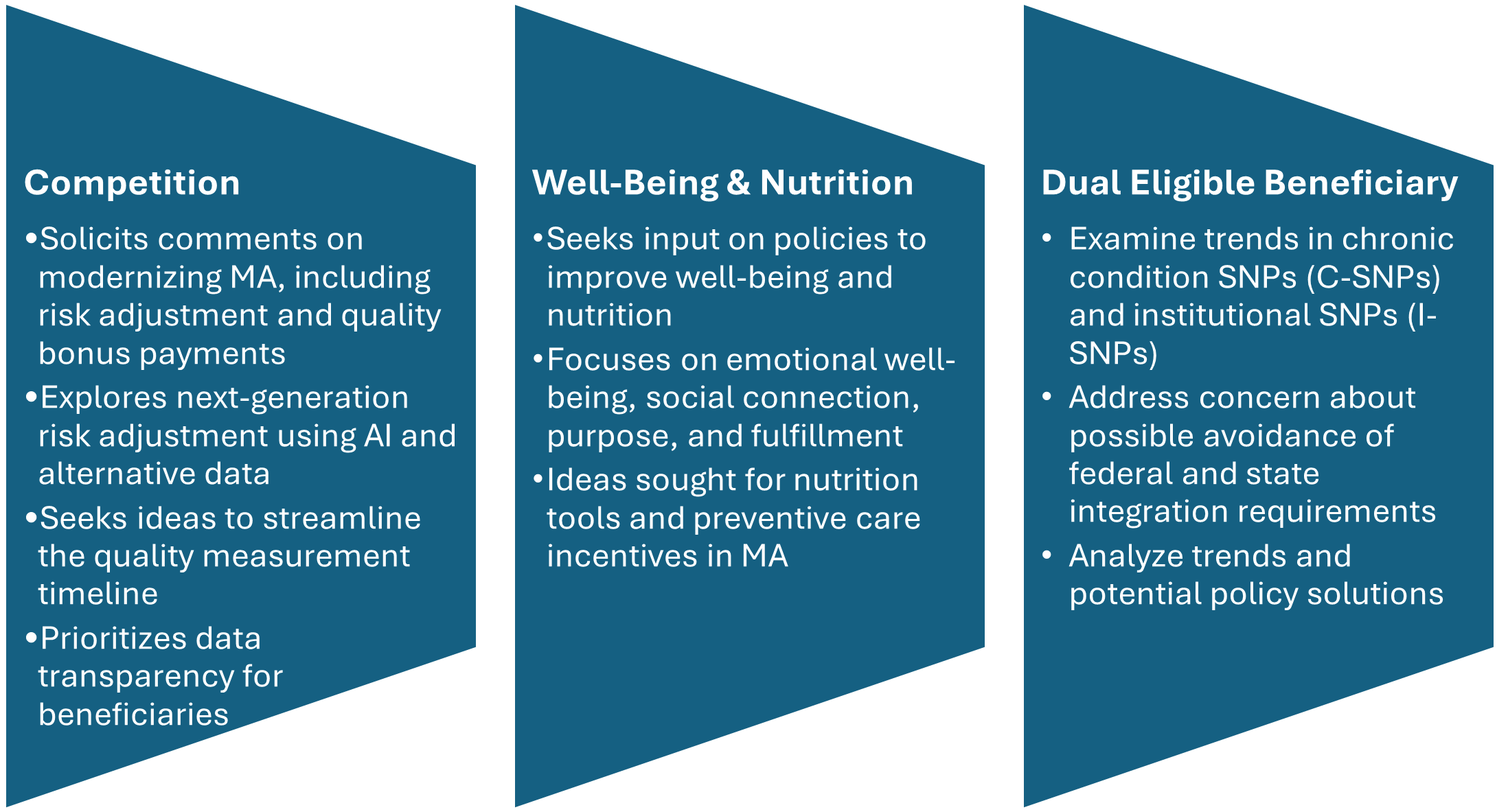
The final CY 2026 rule implements immediate policy changes and signals several areas on which CMS might focus its attention in future rulemaking. Through its responses to public comments and the rationale provided for finalized policies, CMS highlights potential shifts in priorities and emerging directions for Medicare payment policy, reflecting the views of the Trump Administration moving forward. Stakeholders should be attentive to these signals, as they provide valuable insights into where CMS could direct further reforms and adjustments in the coming years.
Health Management Associates (HMA) Medicare experts are reviewing the finalized policies and have identified the highlights outlined in this article. Stakeholders should consider the effect on payment in 2026 as well as the longer-term practice reforms, investments, and analysis that may be required to deliver high-quality services and remain sustainable.
Enhanced Care and Chronic Disease Management
CMS finalized new billing codes to support behavioral health integration and the Psychiatric Collaborative Care Model (CoCM) services delivered to patients who also receive Advanced Primary Care Management (APCM) benefits, along with an add-on code for in-home primary care to reflect added complexity. CMS also retains and repurposes the social determinants of health (SDOH) risk assessments billing code to align with the administration’s focus on addressing the root causes of chronic illness.
Takeaway: These changes are designed to support better care coordination, integration of physical and mental health services, and proactive management of patient risk factors. They indicate CMS’s intent to expand care management strategies beyond traditional settings and into future payment methodologies.
Establishing Specialty Care Models
The rule finalizes the mandatory Ambulatory Specialty Model (ASM) to test value-based payments for specialists who focus on heart failure and lower back pain. ASM adopts a framework similar to the Merit-based Incentive Payment System Value Pathways (MVP) and shares certain quality and cost measures with existing MVPs for heart disease and musculoskeletal care.
The model applies performance-based payment adjustments of up to 12 percent, covering 25 percent of Core-Based Statistical Areas (CBSAs) and metropolitan divisions, and is projected to save $177 million over its test period. ASM will run from 2027-2031, with payment adjustments applied during payment years from 2029-2033.
Takeaway: Stakeholders should plan for CMS’s continued interest in developing mandatory models and opportunities for specialists to participate in Innovation Center efforts.
Emphasis on Rebalancing the Payment System and Site Neutrality
Efficiency Adjustment
Citing the need to account for efficiencies gained in non-time-based services such as procedures, radiology services, and diagnostic tests, CMS finalized a 2.5 percent efficiency adjustment to work Relative Value Units (RVUs) for certain services and procedures, applied every three years. The agency notes it will monitor the three-year cadence and may refine the frequency in future rulemaking.
In response to public comments, CMS added several services to the exemption list in this final rule, including codes that introduced to the fee schedule in 2026, certain time-based services in physical medicine and rehabilitation, remote therapeutic monitoring (RTM), and drug administration, as well as time-based services on the CMS telehealth list.
Takeaway: The move signals a notable shift from the agency’s historical reliance on survey data provided by the American Medical Association (AMA)/Specialty Society Relative Value Scale (RVS) Update Committee (RUC) to establish practitioner time in PFS rate setting. Stakeholders should consider how CMS could build on this new approach in future rulemaking.
Site Neutrality
Site neutral policies will now use hospital outpatient data to set payment rates for certain services, including radiation oncology treatment delivery and some remote monitoring. In addition, the rule establishes the same payment rate in both physician office and hospital outpatient settings for certain supplies, including skin substitute products, and by implementing changes in the physician practice expense methodology.
By tackling practice expense reimbursement, CMS intends to recognize higher costs incurred by physicians who operate a freestanding office than by physicians who furnish care in the facility setting (i.e., indirect practice expenses). This methodology lowers practice expense payments to hospital-based physicians, resulting in double-digit cuts for many specialists in facility settings, while independent and group practice physicians generally will see increases.
Takeaway: The site neutrality changes underscore a broader long-term strategy advanced across multiple administrations to reduce payment disparities and discourage shifting care to higher-cost settings. While some providers will see payment increases and others will experience cuts, these adjustments are part of CMS’s effort to rebalance incentives and move toward value-based models. Stakeholders should recognize that this is not an isolated change, but a signal of continued policy evolution designed to align payment with efficiency and quality.
Strategies to Update PFS Practice Expense Payments
Although CMS implemented major methodology changes to allocate more indirect practice expense (PE) costs to services performed in physician offices and less to those in facility settings, the agency finalized a “status quo” approach. Specifically, the agency will continue using the existing practice expense per hour (PE/HR) values and cost share weights, despite being almost two decades out of date.
Takeaway: CMS indicates interest in revisiting practice expense data in future cycles, which may effect payment.
Positive PFS Conversion Factor Update
All providers and suppliers paid for services under the PFS will benefit from a positive update to the conversion factor, with Advanced Alternative Payment Model (APM) participants receiving a higher increase and one-time incentive payment. Specifically, under the final rule, two conversion factors will be available in CY 2026.
- CMS will pay for services furnished by providers who participate in APMs using a conversion factor of $33.5675—a 3.77 percent increase (or $1.221) from the 2025 amount of $32.3465.
- CMS will compensate providers who do not participate in a qualifying APM using conversion factor of $33.4009—a 3.26 percent ($1.0544) from CY 2025.
Both conversion factors reflect the 2.50 percent overall update required by statute, a 0.49 percent budget neutrality adjustment to account for RVU changes, and an updated factor of 0.75 percent for qualified APMs or 0.25 percent for non-qualifying APMs. CY 2026 is the final year in which eligible clinicians can receive an additional APM incentive. Qualifying clinicians will receive a one-time payment of 1.88 percent of their paid claims for covered professional services based on their performance two years earlier.
Takeaway: These updates provide short-term financial relief. The higher increase and bonus for APM participants signal CMS’s continued push toward alternative payment models, even as the incentive sunsets. Stakeholders should plan for a future in which APM participation remains a key strategy for maintaining revenue stability.
Telehealth-Related Flexibilities
CMS will implement several policy changes that will collectively extend the footprint of telehealth services in Medicare and expand access for Medicare beneficiaries. These changes directly impact Traditional Medicare beneficiaries, physicians’ offices, hospitals, and Federally Qualified Health Centers (FQHC) and Rural Health Clinics (RHC).
- All services on CMS’s Medicare telehealth coverage list are now permanently covered if they are separately payable and can be delivered via two-way audio-video.
- CMS permanently removed frequency limitations on certain telehealth services, including follow-up inpatient and nursing facility services.
- FQHCs and RHCs can serve as distant site telehealth providers for all services—not just mental health services—through December 31, 2026.
- Virtual supervision is permanently allowed for nonsurgical services conducted in real time via two-way audio-video. This policy will apply across all settings, including FQHCs and RHCs requiring an on-site supervising physician.
- Teaching physicians can be virtually present for resident services delivered in all training settings when care is provided via telehealth.
- New services added to the Medicare telehealth coverage list, including certain psychological rehabilitation services, caregiver training services, and risk assessment services.
Takeaway: These changes solidify that telehealth has become an integral part of Medicare service delivery. By eliminating the distinction between temporary and permanent coverage, removing frequency limits, and allowing virtual supervision and teaching physician presence, CMS advances telehealth as a core component of its long-term strategy to improve access, care coordination, and efficiency. In addition, the change aligns with CMS’s commitment to modernizing payment policies to support virtual care models. Stakeholders should plan for continued growth and innovation in this space in future rulemaking cycles.
Other Final Policies
- Addressing Rising Expenditures for Skin Substitutes: CMS addresses rising expenditures for skin substitute products, which are being adopted and used at a rapid rate. Specifically, the agency reclassifies most of these products as supplies billed incident-to physician services, paid at a uniform rate in both office and hospital outpatient settings rather than as Part B drugs. CMS projects that this change will save Medicare $19.6 billion in 2026 and standardize payment to providers who use these products. The policy takes effect on January 1, 2026. Accompanying these changes is the launch of a new model to test clinical review for certain services, including skin substitutes, in fee-for-service Medicare.
- Medicare Shared Savings Program: CMS finalizes its proposal to limit the amount of time an accountable care organization (ACO) can participate in an upside-only risk track, provide more flexibility on the number of beneficiaries assigned to an ACO in its early year of operation, and refine quality measures and improve beneficiary attribution to better reflect care standards.
- Drugs and Biological Products Incident-to Physician Services: The final rule addresses reimbursement for drugs paid incident-to a physician’s service, including policies related to the Inflation Reduction Act provisions, continued implementation of discarded units refund requirements, changes and clarifications to average sales price (ASP) reporting, and payment for procedures required to manufacture cell-based gene therapies.
- Coding and Payment for Technology-Based Services: CMS pays for digital mental health treatment (DMHT) devices that have Food and Drug Administration (FDA) clearance or authorization and are furnished in conjunction with professional services, including initial education and onboarding. CMS expands these payment policies for DMHT used to treat of attention deficit hyperactivity disorder when providers adhere to established billing requirements. The agency recognizes that behavioral health conditions are common chronic diseases and that the field of digital therapeutics is evolving.
Contact an HMA Medicare Expert Today
HMA policy and rate setting experts are analyzing the details and impacts of the proposed rule and will provide additional updates on key Medicare policies as they become available. Our team can support stakeholder development of policy and data-oriented comments pertaining to this rule and on any other Medicare topic of interest. Contact our experts below to discuss your priorities and approach.