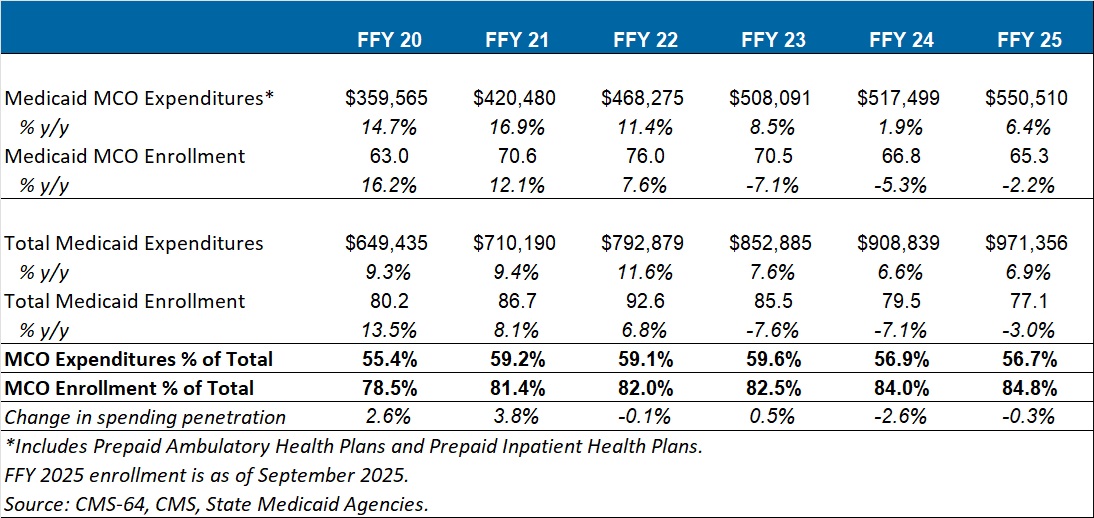
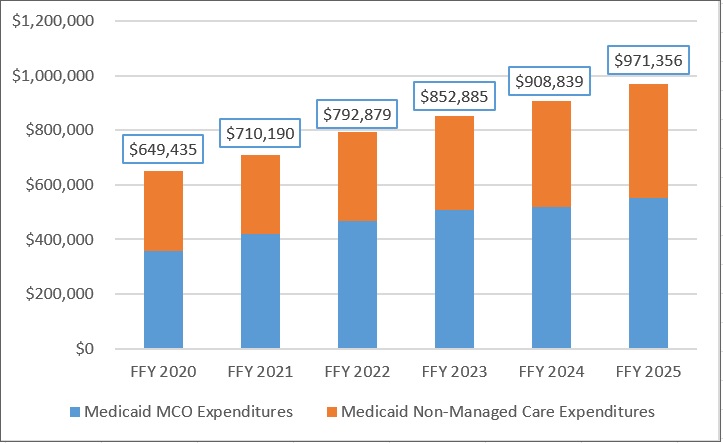
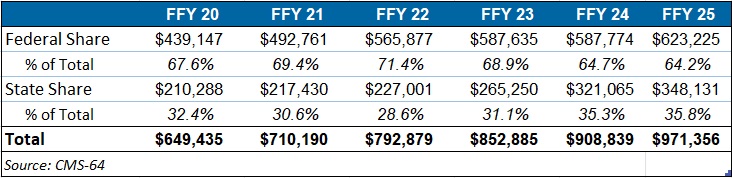
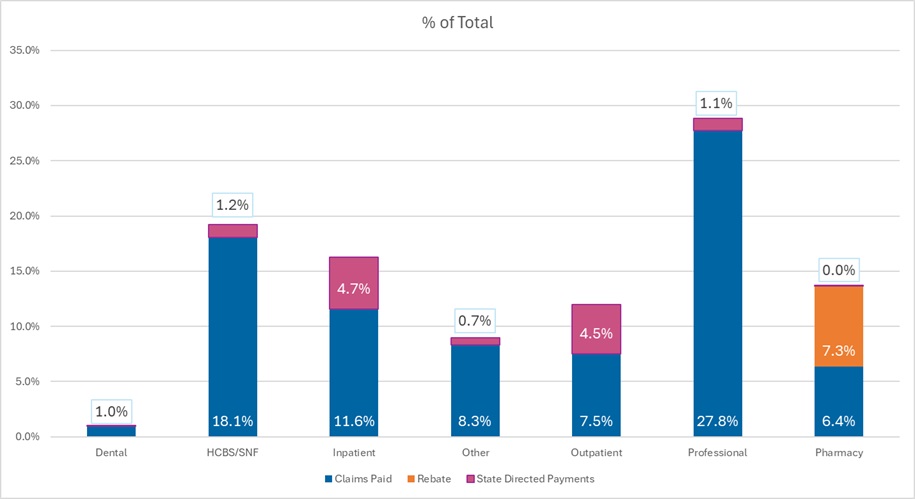
This week Health Management Associates (HMA), draws on its database of monthly Medicaid managed care enrollment to present its latest quarterly analysis, offering a snapshot of enrollment trends across 37 states.
The analysis comes at a critical time. As states prepare for Medicaid eligibility policy changes that take effect in 2027—including more frequent eligibility determinations and expanded work and community engagement requirements—current enrollment trends provide an early signal of how policy decisions and administrative practices are already influencing coverage levels.
The HMA Information Services (HMAIS) analysis shows that Medicaid managed care accounted for 85.6 percent of total Medicaid enrollment in December 2025. This analysis, available to HMAIS subscribers, uses data from nearly 300 health plans in 41 states. The report provides by-plan enrollment plus corporate ownership, program inclusion, and for-profit versus not-for-profit status, with breakout tabs for publicly traded plans.
Key Insights from Q4 2025 Data
The 37 states included in this review have released monthly Medicaid managed care enrollment data through public websites or in response to a public records request from HMA. The report includes the most recent data obtained and illustrates the effect of state-level choices around eligibility and administration. Key findings include:
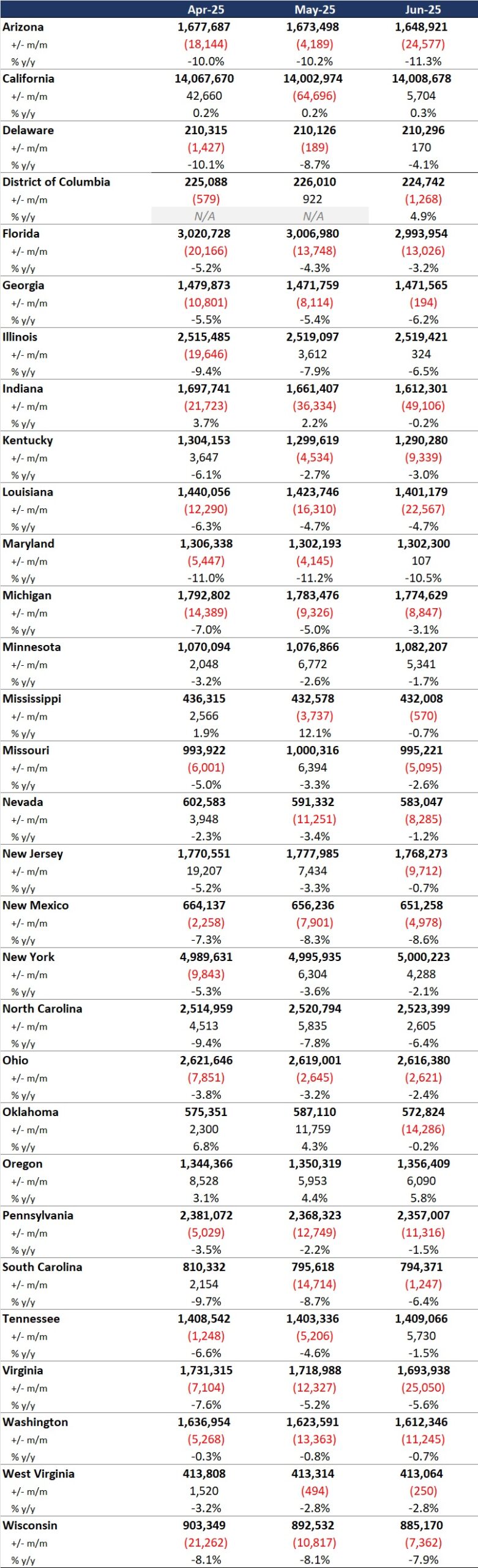
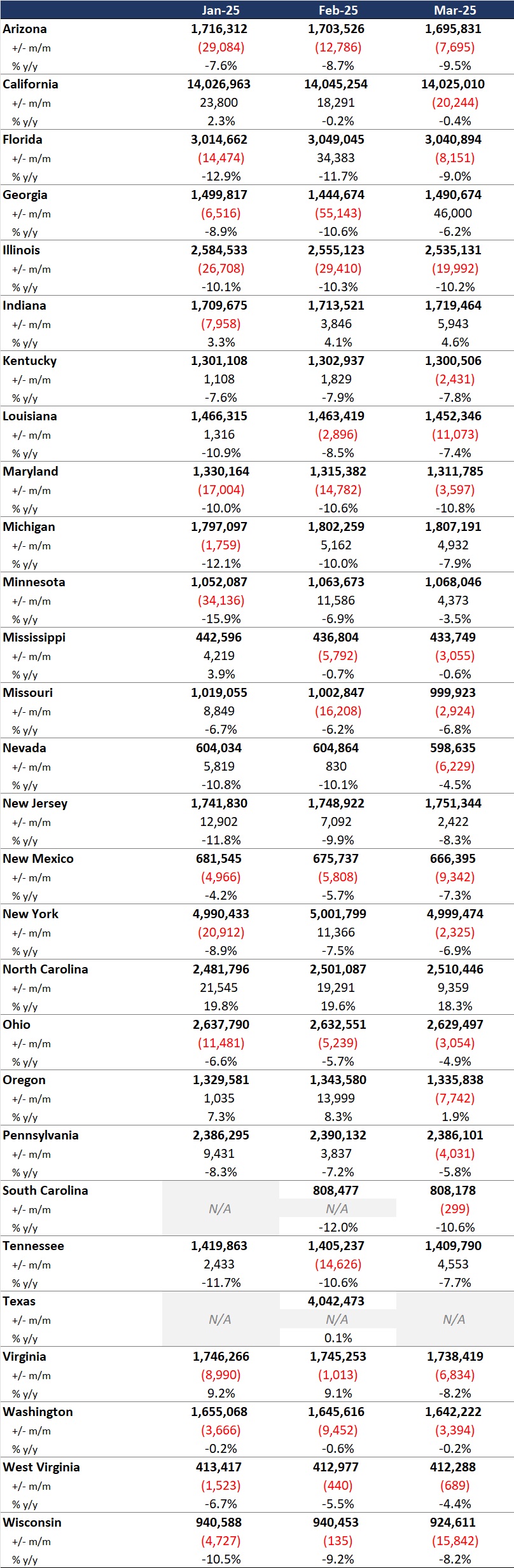
- As of December 2025, Medicaid managed care enrollment across the 37 states declined by 2.2 million members year over year, falling to 62.5 million—a 3.4 percent decrease.
- Of the 37 states, eight—Colorado, Delaware, Mississippi, Missouri, New Jersey, North Carolina, North Dakota, and Oregon—did not experience year-over-year managed care enrollment declines, and instead showed flat enrollment or modest gains. With the exception of Mississippi, these are all Medicaid expansion states.
- Arizona and Indiana experienced double-digit percentage declines. Notably, Indiana began requiring enrollees to actively respond to renewal mailers, which aligns with enrollment declines that began in March 2025.
- Among the expansion states in the analysis, enrollment declined by 1.7 million (-3.3%) to 50.8 million. The seven non-expansion states experienced a similar decline (-3.6%), bringing enrollment to 11.7 million enrollees.
Data Considerations. The data have some important limitations. States report enrollment figures at different points during the month, with some data reflecting beginning of the month totals and others capturing end of the month enrollment. In addition, some state datasets encompass all Medicaid programs offering managed care plans, whereas others reflect only a subset of the managed Medicaid population. As a result, the findings should be viewed as indicative of broader trends rather than a comprehensive state-by-state comparison.
Market Share and Plan Dynamics
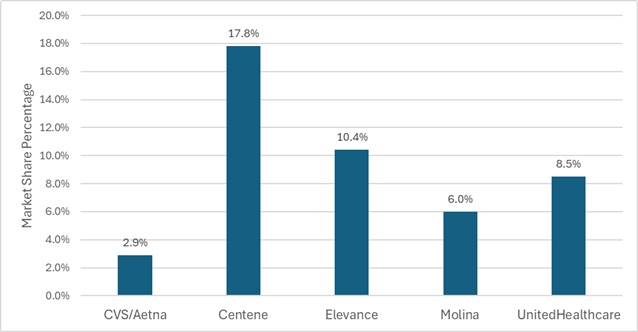
Using our data repository for 300 health plans across 41 states, HMAIS analyzes corporate ownership, program participation, and tax status among Medicaid managed care plans. As of December 2025, Centene maintained the largest share of the national Medicaid managed care market at 17.8 percent, followed by Elevance (10.4%), United (8.5%), and Molina (6.0%) (see Figure 1). These figures highlight continued concentration among large national plans, even as overall enrollment declines.
Figure 1. National Medicaid Managed Care Market Share by Number of Beneficiaries for a Sample of Publicly Traded Plans, December 2025
What to Watch
Enrollment trends observed in the fourth quarter (Q4) of 2025 and continuing into 2026 indicate increasing state attention to eligibility policy and program integrity. State legislative activity, budget pressures, and federal regulatory developments are prompting many states to assess and strengthen certain aspects of their programs related to eligibility, particularly as they prepare to implement redetermination and work and community engagement requirements.
Several states are already moving toward implementation. Nebraska is scheduled to launch Medicaid work requirements on May 1, 2026, while Montana plans to begin implementation on July 1, 2026. With additional federal guidance still emerging, most other states are working toward compliance ahead of January 2027 deadlines. In expansion states, policymakers retain authority to tighten administrative processes, alter optional benefits, or adjust provider payment levels—actions that may materially affect enrollment.
These developments underscore why Medicaid managed care enrollment trends deserve close attention. Declines in enrollment are often an early indicator of broader system impacts, including rising uncompensated care for providers, shifts in payer mix, and increased financial pressure on safety‑net systems. For managed care organizations, even modest enrollment changes can mask more significant shifts in risk profiles, geographic concentration, or service needs.
Connect with Us
HMA is home to experts who know the Medicaid managed care landscape and how it is evolving. HMAIS’s Medicaid enrollment data, financials, procurement tracking, and a robust library of public documents equips stakeholders with timely, actionable intelligence.
For more information about the HMAIS subscription, contact Andrea Maresca and Alona Nenko.