
March 18, 2026
Connecting the Dots: Medicaid Community Engagement Requirements and State Readiness for 2027
HMA Insights – including our new podcast – puts the vast depth of HMA’s expertise at your fingertips, helping you stay informed about the latest healthcare trends and topics. Below, you can easily search based on your topic of interest to find useful information from our podcast, blogs, webinars, case studies, reports and more.

Connecting the Dots: Medicaid Community Engagement Requirements and State Readiness for 2027

The first quarter of 2026 marked a turning point in federal oversight of pharmacy benefit managers (PBMs), the intermediaries that manage prescription drug benefits for most health plans across the commercial insurance market, Medicare Part D, and other programs. New legislation, agency rulemaking, and enforcement activity collectively signal a new phase of oversight that could materially reshape PBM contracting, compensation, and transparency requirements.
Most notably, the following developments stand out:
Together, these actions signal a trend toward greater PBM accountability, with implications for plans, pharmacies, manufacturers, and consumers. This article provides a high-level overview of the major recent developments in the PBM reform policy landscape, along with key considerations for stakeholders.
Medicare Part D: Key Statutory Changes
Beginning in plan year 2028, CAA 26 makes significant changes for PBMs operating in Medicare Part D. Key provisions include:
Additional provisions that will take effect in beginning with plan year 2029 include:
Key considerations: The Centers for Medicare & Medicaid Services (CMS) has broad discretion in implementing these provisions, including setting pharmacy contracting standards, determining which PBM affiliates are subject to new requirements, and defining “fair market value.” PBMs will face expanded reporting and compliance obligations, while plans and other stakeholders will have opportunities to shape implementation through the regulatory process.
Commercial Health Insurance Market: Key Statutory Changes
For the commercial market, CAA 26 establishes similar transparency requirements for PBMs that serve fully insured and self-insured plans, with reporting required up to four times per year. Unlike Medicare Part D, the statute does not prohibit pricelinked compensation in the commercial market, but it does require detailed disclosure of PBM fees and revenue streams. For contracts with selfinsured plans, PBMs must remit 100 percent of rebates and fees tied to drug utilization, subject to specified limitations.
Key considerations: These provisions significantly expand federal oversight in the commercial market. PBMs will need to scale compliance infrastructure, while employers and other plan sponsors may seek enhanced analytical and actuarial support to interpret disclosures and assess PBM performance.
Medicaid Left Out, For Now.
Unlike prior legislative packages, CAA 26 does not include Medicaid-specific PBM reforms, such as prohibitions on spread pricing (i.e., a PBM charges a payer more than the amount it pays the dispensing pharmacy for a prescription) and expanded National Average Drug Acquisition Cost (NADAC) reporting.
Key considerations: These policies continue to have bipartisan support and could reemerge in future legislation. States, PBMs, and managed care plans should continue monitoring for renewed federal action on these policies.
DOL’s Proposed PBM Fee Disclosure Rule
DOL’s proposed rule, “Improving Transparency Into Pharmacy Benefit Manager Fee Disclosure,” would require PBMs serving self-insured ERISA plans to disclose information about rebates, manufacturer fees, pharmacy payments, and spread pricing. In late February, DOL extended the public comment period to April 15 to allow stakeholders to address how the proposed rule should align with the newly enacted CAA 26 provisions.
Key considerations: DOL could withdraw the proposal in favor of the statutory framework or could finalize the rule to take effect before the CAA 26 requirements begin. Either path would further increase near-term compliance for PBMs and plan sponsors, and stakeholders should monitor this space closely.
FTC Settlement with ESI
The FTC’s settlement with ESI resolves insulin-focused litigation against the PBM and imposes extensive requirements related to transparency, compensation, rebates and fees, and benefit design. The settlement also includes less common provisions, such as a commitment to reshore and increase disclosures related to ESI’s rebate group purchasing organization (GPO) functions.
Key considerations: If similar settlements are reached with other PBMs, the FTC could play an expanded role in shaping PBM market behavior, supplementing legislative and regulatory reforms with enforcement-driven standards.
State Efforts to Regulate PBMs
States continue to pursue PBM reforms, with dozens of laws enacted in recent years addressing licensure, reporting, pharmacy reimbursement, and contracting standards. Although the Supreme Court’s 2020 decision in Rutledge v. PCMA opened the door to certain state-level reforms, subsequent court decisions have narrowed the scope of permissible state regulation, particularly when ERISA preemption or Medicare Part D conflicts arise.
Key considerations: Stakeholders operating across multiple markets and states will continue to face a complex and evolving patchwork of requirements, underscoring the importance of ongoing policy tracking and compliance coordination.
Connect with Us
Recent federal and state actions suggest that PBM reform is entering a more operational phase defined by transparency and enforceable standards governing compensation, contracting, and market behavior. As implementation unfolds, stakeholders across the prescription drug supply chain will need to engage closely with regulators, assess new data flows, and adapt their business practices to a more prescriptive oversight environment.
For more information about the policies described in this article and the PBM policy landscape more broadly, please contact our experts Conor Sheehey or Stephen Palmer.

The Centers for Medicare & Medicaid Services (CMS) proposed 2027 Notice of Benefit and Payment Parameters (NBPP) marks a notable shift in Marketplace policy, expanding lower premium plan options, relaxing certain federal standards, and moving more implementation and oversight responsibility to states and Marketplaces. It also introduces eligibility and verification policies that could significantly affect enrollment, operations, and market stability.
To unpack what this could mean for plan year 2027 and beyond, Andrea Maresca spoke with Zach Sherman, Managing Director for Coverage Policy and Program Design at Health Management Associates (HMA); Lina Rashid, Principal at HMA; and Michael Cohen, PhD, Principal at Wakely, an HMA company, who, alongside colleagues, published a Policy Brief on state-level and consumer impacts, as well as a Wakely White Paper on the proposed rule.
Q: When you zoom out from the technical details, what are the big takeaways from the proposed 2027 NBPP for states, consumers, and issuers?
Lina Rashid: At a high level, the proposal reallocates risk and responsibility across the system. Consumers may see more lower premium options through expanded catastrophic plan eligibility and more flexible bronze plan design, but often with more cost-sharing, higher deductibles, or greater complexity. For consumers, affordability is about more than just premiums; it’s about how much healthcare costs for individuals and their families overall and the cost of care when they need it.
States are being given options to take on more oversight and operational responsibility but without additional federal funding. And issuers are being given more flexibility, but it comes with uncertainty regarding enrollment and risk mix.
Zach Sherman: The rule’s cumulative effect matters more than any one policy. Expanded catastrophic eligibility, higher out-of-pocket exposure, relaxed network standards, and tighter verification requirements all interact. Together, they raise questions about access, affordability, and whether Marketplaces are equipped to manage administrative and enrollment disruption.
Q: The paper highlights potentially significant enrollment effects. What’s driving that dynamic?
Michael: Two things stand out. First, the proposal implements statutory changes that remove advance premium tax credit (APTC) eligibility for certain lawfully present immigrants beginning in 2027. CMS estimates more than a million people could lose eligibility, and it’s reasonable to expect most of them will exit the individual market.
Second, the proposed income verification changes could generate millions of data matching issues (DMIs) that temporarily or permanently cut off access to advance premium tax credits. While CMS projects a relatively modest disenrollment effect, our analysis suggests losses could be meaningfully higher depending on how quickly issues are resolved. We estimate that approximately 4.7 million enrollees could receive DMIs under the proposal, and upward of 80 percent of them could temporarily or permanently lose access to APTCs, putting coverage at risk.
Zach: If consumers can’t afford the full premiums while resolving a data issue, many will drop coverage. That creates churn and administrative strain that Marketplaces must manage.
Q: How do these policies affect state Marketplaces and regulators specifically?
Zach: States are being asked to do more across multiple fronts. Network adequacy oversight is shifting toward states that conduct effective rate review. States may also choose or feel pressure to take on Essential Community Provider (ECP) review authority, including for new non-network plans. Accepting that responsibility requires legal authority, staff capacity, and technical infrastructure.
At the same time, states may need to stand up the State Exchange Improper Payment Measurement (SEIPM) program, which CMS acknowledges will increase administrative burden.
The proposed State Exchange Enhanced Direct Enrollment (SBE-EDE) option is also a significant shift. Rather than operating a centralized consumer enrollment platform, Marketplaces would focus on certifying, overseeing, and monitoring multiple third-party entities. As a former director of a state-based Marketplace program, I know this is a fundamentally different operational posture that comes with oversight and compliance costs.
Q: The proposal also introduces non-network plans. What should stakeholders be watching here?
Michael: Non-network plans may offer lower premiums, but they change how access works. Provider participation depends on the willingness to accept the plan’s payment as payment in full. On paper a plan may meet access standards, but in practice consumers could face difficulty finding care. That places additional oversight responsibility on states to determine whether access is sufficient in practice. If aggressively priced non-network plans disproportionately attract healthier enrollees, it can create financial risk for issuers and for the broader market.
Q: What does this mean for market stability going forward?
Zach: Stability will vary by state. States that invest in oversight, consumer assistance, and operational readiness—often a state-based Marketplace—may be better positioned to manage these changes. Others may see sharper enrollment declines or access issues. That divergence across states is an important signal from this proposal.
Q: What should states and stakeholders be doing right now?
Zach: States should be doing scenario planning, assessing which flexibilities to adopt, where to maintain higher standards, and whether they have the capacity to take on expanded responsibilities. These decisions will shape how the rule plays out on the ground.
Michael: Issuers should be stress testing pricing assumptions, risk adjustment exposure, and operational readiness. All stakeholders should remember that comments on the proposed rule are due March 13, 2026.
Lina: Notably, CMS is not done with regulatory reforms. The agency solicited comment on medical loss ratio (MLR) policies and paused Essential Health Benefit benchmark updates, as well as issues not covered in this proposed rule, such as revisions to the Section 1332 waiver and Section 1333 interstate compacts. States and issuers should be tracking what may come next, not just what’s in this proposal.

Outlook 2026: What CMS’s Proposed 2027 NBPP Signals for ACA Marketplaces, States, and Consumers

On February 9, 2026, the Department of Health and Human Services (HHS) released the proposed Notice of Benefit and Payment Parameters (NBPP) for 2027. The notice includes important proposed rules and parameters for the operation of the individual and small group health insurance markets in 2027 and beyond.
This paper summarizes key provisions in the proposed notice with a focus on the major changes to plan types, cost-sharing, network design and oversight, marketplace philosophy, and the shift of responsibilities from the federal government to states. It also evaluates any changes to returning policies from the Marketplace Affordability and Integrity rule from last year, which are currently being challenged in court, and codifies relevant statutory changes in the One Big Beautiful Bill Act.
The paper reviews the potential impact of these proposed policies on consumer affordability and access as well as the impact and associated level of effort on state regulators and marketplaces. Lastly, it touches on policies not included in this rule, including those highlighted as issues that may or will be addressed in future rulemaking as well as issues surprisingly not covered in this proposed rule, such as revisions to the Section 1332 waiver process as well as details on how a state could explore and pursue a 1333 interstate compact. Comments are due no later than March 13, 2026.

Fraud, waste, and abuse (FWA) in Medicaid non-emergency transportation (NEMT) remain a persistent challenge for state Medicaid programs and health plans because of the scale and complexity of the benefit. NEMT is a critical, mandatory benefit intended to ensure eligible Medicaid beneficiaries without reliable transportation can get to necessary medical appointments. Numerous investigations and audits, however, have revealed that some transportation providers bill for trips that never occurred, inflate mileage, fabricate tolls, or even recruit patients with kickbacks to generate fraudulent claims, diverting limited program funding away from legitimate care needs.
The NEMT benefit represents a small share of Medicaid costs—estimated at around 1 percent of total Medicaid spending. With the codification of NEMT as a required benefit in 2020, market analysts forecast NEMT will grow considerably, nearly doubling in market size from 2021 to 2028.
Comprehensive, nationwide estimates specific to NEMT FWA are limited. Federal and state audits like those in Indiana, New York, and Massachusetts, however, have uncovered millions of dollars in claims that did not comply with federal and state requirements, underscoring systemic vulnerabilities in oversight and documentation. For example, a 2022 federal audit of New York Medicaid NEMT found an estimated $84 million in unallowable federal reimbursements and another ~$112 million that may not have complied with requirements over two years.[1]
Furthermore, individual criminal cases have involved schemes of $1 million to more than $2 million in falsely billed transportation services. Isolated settlements and audits indicate that fraud and abuse can be substantial locally even if we lack a clear, reliable national aggregate estimate.
A 2025 report by Health Management Associates (HMA) about NEMT contracting approaches found an opportunity for states and health plans that administer non-emergency transportation to leverage technology and require or incentivize new strategies to improve program integrity and quality in NEMT going forward. Some of the identified strategies to address FWA include:
Since the publication of that report, several state Medicaid programs have issued NEMT procurements that maintain a strong emphasis on preventing FWA. For example, the 2025 Wisconsin NEMT RFP included provisions to promote greater collaboration between the Wisconsin Department of Health Services (DHS) Office of Inspector General (OIG) and NEMT broker, including “quarterly and ad hoc meetings to discuss open complaint investigations, red flag patterns, and establish safeguards for ongoing or suspected fraud, waste, and abuse” and imposed penalties for fraud incidents that go undetected by the broker.
FWA in Medicaid NEMT may represent a fraction of overall program spending, but the consequences are outsized: Every improper payment diverts resources away from beneficiaries who depend on transportation to access essential care. As states, health plans, and NEMT brokers modernize contract requirements, strengthen oversight, and embed technology-driven verification into their contracts and operations, the focus is shifting from retrospective recovery to proactive prevention, transparency, and accountability in transportation services.
Continued collaboration among Medicaid agencies, brokers, medical providers, and oversight entities will be critical for sustained progress. By pairing smarter contracting with real-time data tools and clear accountability, states and Medicaid health plans can better safeguard public dollars while ensuring that NEMT remains a reliable lifeline for the people it is designed to serve.
Learn more about how HMA Helps NEMT Stakeholders Overcome Challenges. If your organization is ready to talk about how HMA can help advance your NEMT goals, please contact one of our experts below.
Related Resources:
[1] US Department of Health and Human Services, Office of Inspector General. New York Claimed $196 Million, Over 72 Percent of the Audited Amount, in Federal Reimbursement for NEMT Payments to New York City Transportation Providers That Did Not Meet or May Not Have Met Medicaid Requirements. September 12, 2022. Available at: https://oig.hhs.gov/reports/all/2022/new-york-claimed-196-million-over-72-percent-of-the-audited-amount-in-federal-reimbursement-for-nemt-payments-to-new-york-city-transportation-providers-that-did-not-meet-or-may-not-have-met-medicaid-requirements/.

The Medicare Advantage (MA) program continues to evolve as plans respond to shifting policy signals, market pressures, and beneficiary expectations. A new paper from Wakely, an HMA Company—The Value Shift: How Medicare Advantage Benefits Are Evolving for 2026—provides a data-driven examination of how MA benefit designs are changing and what those changes signal about the future direction of the program.
This paper refreshes Wakely’s ongoing MA benefit analysis, updating prior findings with the latest 2026 plan enrollment data. It builds on Wakely’s established work examining benefit design, supplemental offerings, and the relationship between bids, rebates, and plan value, including The Value Shift: Inside the C-SNP Surge.
This article highlights findings from the proprietary value-add metric that Wakely developed to provide a comprehensive assessment of MA plan value. Although it can be used as a comparative metric to evaluate relative changes year over year, it is not intended to represent pricing.
From Benefit Expansion to Optimization
Over the past decade, MA plans have steadily expanded benefit offerings, supported by strong enrollment growth and favorable rebate dynamics. The 2026 benefit landscape suggests that plans have been taking a more measured approach (see Figure 1). Wakely’s analysis finds that plans are becoming more strategic in how benefits are designed and deployed, maintaining or enhancing benefits that are best aligned with quality performance, affordability, and target populations while pulling back in other areas.
Plans appear to be optimizing benefits to better align with member needs, quality performance, and financial parameters. Examples include refining supplemental benefits, adjusting cost-sharing structures, and rethinking how benefits support care management and health outcomes.
Figure 1. Change in Plan Value-Add from 2025 to 2026
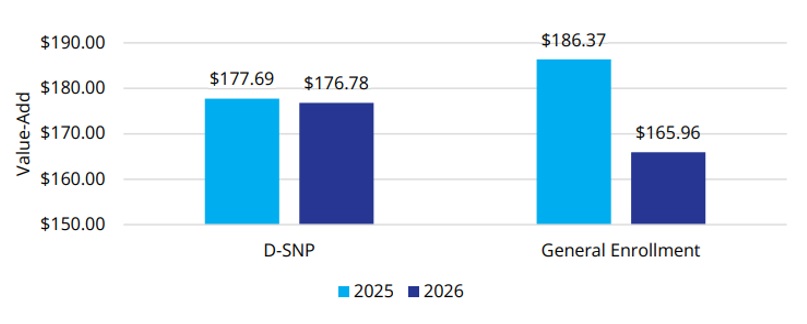
The shift reflects an MA market in which differentiation and long-term sustainability are increasingly important.
Supplemental Benefits: More Targeted, More Strategic
Supplemental benefits remain a defining feature of Medicare Advantage, but their role is evolving. Wakely’s paper highlights a move away from expanding the number of benefits toward targeted benefit offerings that are more clearly connected to member engagement and outcomes.
Plans are homing their focus on benefits that support daily living, chronic condition management, and access to care, particularly for populations with higher needs. This targeted approach suggests plans are thinking about value, operational complexity, and how benefits contribute to overall value propositions.
Between 2025 and 2026, the percentage of members with access to common supplemental benefits has, on average, stayed consistent or slightly decreased among the general enrollment population (Figure 2). The percentage of members who are enrolled in plans that offer over-the-counter (OTC) drug, transportation, and Flex Card benefits has decreased by 11 percent, 6 percent, and 4 percent, respectively. Conversely, the Dual Eligible Special Needs Plan (D-SNP) population saw an increase in member access to all supplemental benefit categories except transportation (an 8% decrease).
Figure 2. Percent of Enrollment in Common Supplemental Benefits
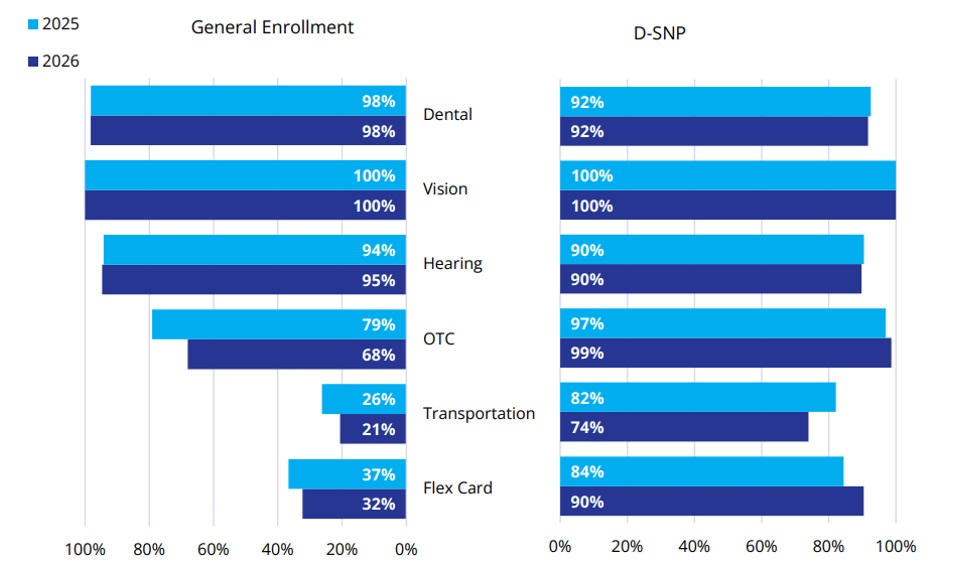
For stakeholders across the healthcare ecosystem, this trend underscores the importance of understanding not just what benefits are offered, but why.
Shifts in Cost Sharing and the Enrollee Experience
Wakely’s analysis also points to notable shifts in cost sharing and premium structures. There is continued attention to balancing affordability for members with the need to manage plan liability amid changing benchmarks and utilization patterns.
These decisions directly affect the member experience. Small shifts in copays, deductibles, or benefit limits can influence enrollment, retention, and satisfaction, particularly in competitive markets. As plans fine tune these levers, data-driven insights become critical to understanding how benefit changes may resonate with different member segments.
2026 Signals for Future Bid Cycles
The benefit trends identified in “The Value Shift” series suggest several broader signals for the MA market:
These dynamics have implications for MA organizations and for providers, policymakers, and partners seeking to understand how MA continues to shape care delivery and costs.
Value-Add Metric and Benefit Design Insights
In this paper, Wakely paired its actuarial and analytic expertise with tools that enable detailed benefit and market analysis. One of those tools, Wakely’s Medicare Advantage Competitive Analysis Tool (WMACAT), calculates a comprehensive value-add metric that integrates five core components into a consistent framework that allows for apples-to-apples comparisons across plans, markets, and years. In addition, Wakely’s Strategic Market Analysis and Ranking Tool (SMART) supports broader competitive assessments by layering enrollment weighting, geographic variation, and plan positioning into the analysis.
As an HMA company, Wakely’s work is complemented by broader policy, market, and strategy expertise, helping organizations connect benefit decisions to regulatory developments, operational considerations, and long-term goals.
For health plans and healthcare organizations navigating the next phase of Medicare Advantage, these combined capabilities can respond to questions such as:
Looking Ahead
MA benefit design remains an important signal of market direction by showing how plans are responding to policy change, market competition, and financial pressure. As plans shift from broad expansion to more targeted value strategies, the ability to measure, compare, and interpret benefit changes becomes essential as plans look ahead to the 2027 and 2028 bid cycles.
Wakely will continue to build on this work with upcoming analyses, including deeper dives into Part D design changes and the implications of the sunset of the Value-Based Insurance Design (VBID) program.
For information about this analysis and the Wakely tools, contact Dani Marino and Amanda Nelessen.

The Value Shift in Medicare Advantage: What 2026 Benefits Tell Us About the Market’s Next Chapter

The Centers for Medicare & Medicaid Services (CMS) 2027 Notice of Benefit and Payment Parameters (NBPP) proposed rule, published February 11, 2026, arrived at a pivotal moment for the Affordable Care Act (ACA) Marketplaces. The temporary enhanced premium tax credits (ePTCs), first expanded in 2021 and extended through 2025, expired at the end of last year, returning Marketplace subsidies to their original ACA structure in 2026. As we discussed in earlier articles (here and here), that shift is already affecting affordability, plan selection, and enrollment dynamics—particularly for consumers who are ineligible for premium assistance.
The proposed 2027 NBPP represents a significant reset for the Marketplace, reflecting CMS vision and policy priorities to strengthen program integrity while expanding plan design flexibility and consumer choice as a pathway to affordability, as well as policies to defer to state authority. Healthcare organizations and other interested stakeholders may submit comments on the proposed rule through March 13, 2026.
The remainder of this article addresses the key policy proposals and considerations for issuers, states, and consumer groups.
CMS’s Proposals
The proposed NBPP for 2027 sets standards for the Exchanges and ACA-compliant individual and small group markets and updates payment parameters for risk adjustment and risk adjustment data validation (RADV). The rule also implements changes approved under the 2025 Budget Reconciliation Act, (P.L. 119-21, OBBBA) and includes a range of policies spanning plan certification, eligibility and verification, and Exchange oversight.
Expanded Plan Design Flexibility
CMS proposes to discontinue standardized plan options in the Federally-facilitated Marketplace (FFM) and remove limits on the number of non-standardized plans offered by issuers on the FFM and state-based Marketplaces on the federal platform (SBE-FPs). Issuers would be permitted to decide whether to discontinue existing standardized or chronic condition plans or continue them with modified cost sharing.
Considerations: This change is designed to allow greater innovation in plan design. It also raises questions about the potential return of a more complex Marketplace shopping experience for consumers who will have to shift through more plans.
Certification of Non-Network QHPs
One of the most consequential proposals would allow “non-network” plans to be certified as qualified health plans beginning in 2027. These plans would not rely on contracted provider networks. Instead, they would set benefit payment amounts and require issuers to demonstrate that sufficient providers—including Essential Community Providers (ECPs) and mental health and substance use disorder providers—are willing to accept those amounts as payment in full.
Considerations: CMS positions non-network plans as a way to create lower premium options. For states and issuers, this proposal introduces new oversight and operational considerations related to access standards, consumer protections, the risk of balance billing or access gaps for consumers, and potential market instability.
Changes in Catastrophic and Bronze Cost Sharing
The proposed rule would further expand access to catastrophic plans by codifying hardship exemptions for individuals ineligible for advance premium tax credits (APTCs) or cost-sharing reductions (CSRs) because of projected income. CMS also proposes to allow multiyear catastrophic plans with contract terms of up to 10 consecutive years. In addition, CMS proposes new flexibility for certain bronze plan designs in the individual market. In both cases, CMS proposes to allow catastrophic and bronze plans to exceed the annual maximum out-of-pocket limit.
Consideration: These policies reflect CMS’s emphasis on affordability through lower premiums and expanded consumer choice, while shifting more financial risk to enrollees through higher cost sharing.
Network Adequacy and Essential Community Providers
CMS proposes to give states greater discretion in provider access for network adequacy and ECP certification reviews, including allowing federally funded exchange (FFE) states to conduct their own reviews if CMS determines they have sufficient authority and technical capacity. CMS also proposes to reduce the minimum percentage of ECPs that issuers must include in their networks from 35 percent to 20 percent.
Considerations: These changes reduce federal prescriptiveness and could lower issuer compliance costs but also place more responsibility on states to monitor access and ensure that vulnerable populations are not adversely affected.
Essential Health Benefits and State Mandates
The proposed rule would prohibit issuers from including routine non-pediatric (adult) dental services as an Essential Health Benefit (EHB). More significantly for states, CMS proposes changes to cost defrayal requirements for state-mandated benefits, requiring states to cover the cost of benefits considered “in addition to EHB” under specified criteria, even if those benefits are embedded in the state’s EHB benchmark plan.
Consideration: These changes could have direct budgetary implications for states, pricing implications for issuers, and could stunt or potentially decrease benefits for consumers.
Program Integrity and Increased Eligibility Verification
CMS includes a robust set of program integrity provisions, including:
Consideration: These policies continue CMS’s heightened scrutiny of enrollment activity and subsidy eligibility. CMS’s policies are likely to increase data matching issues (DMIs), which could increase burden on Marketplaces and enrollees, resulting in reduced enrollment.
Preparing for Policy Driven Changes in ACA Marketplaces
The 2027 NBPP underscores a clear policy shift away from extending federal subsidies toward advancing a Marketplace framework that emphasizes program integrity, state flexibility, and expanded plan design options as mechanisms to promote affordability and consumer choice.
The proposed rule sets the stage for significant strategic and operational decisions for issuers and states ahead of the 2027 plan year. Health Management Associates (HMA), including Wakely, an HMA company, works with issuers modeling enrollment and risk shifts and to assist in pricing decisions. States also should consider the need for new strategies and approaches to adapt to federal policy changes that are expected for ACA Marketplace programs.
For more information about the policies described in this article, support with scenario-based modeling of enrollment and data-informed strategy development for 2027 and beyond, please contact our experts Michael Cohen, Lina Rashid, or Zach Sherman.

In this conversation, Andrea Maresca, Senior Principal at Health Management Associates (HMA), caught up with Tim Courtney, Director, Wakely, and Jonathan Blum, Co-Founder & Managing Partner at Health Transformation Strategies, LLC, to unpack the biggest questions emerging from the Calendar Year (CY) 2027 Medicare Advantage (MA) and Part D Advance Notice. Of particular interest was the Centers for Medicare & Medicaid Services’s (CMS’s) proposed risk adjustment and diagnosis source changes, which are drawing significant attention across the industry.
Q: The headline is “flat” payments. How should the market interpret CMS’s projected rate change?
Tim Courtney: CMS projects a net average payment change of just +0.09 percent for CY 2027—about $700 million (M). The effective growth rate is about 4.97 percent, but it’s largely offset by risk model and normalization changes and the proposed diagnosis source policy.
Jon Blum: Exactly. It’s important to note that CMS’s impact projections are based on the change in its average payments. Its proposed policies will have much more far-reaching distributional impacts, depending on the diagnoses of their enrolled members. At the same time CMS recently proposed changes to its Star Ratings methodologies. Over time, we could see quite significant changes to the balance of Medicare Advantage payments distributed across the country that could significantly affect benefit offerings and premium amounts.
Q: What’s most surprising in the Advance Notice for 2027?
Blum: The diagnosis source tightening is the big one. CMS proposes excluding diagnoses from “unlinked Chart Review Records” from risk score calculation starting in CY 2027. That signals a continued progression by the agency toward encounter-anchored data integrity. Assuming this policy is finalized, Medicare Advantage plans must continue to invest in systems to respond to CMS’s program integrity focus.
Courtney: And it’s not only chart review. CMS also proposes excluding diagnoses from audio-only services for Part C and similarly for Part D. Operationally, that’s a big deal. Plans need to understand where diagnoses originate, how they’re supported, and what the downstream risk adjustment factor (RAF) impact looks like by segment and provider channel.
Q: The Wakely team estimates a different “feel” than CMS’s topline. What does Wakely’s analysis add?
Courtney: Wakely’s summary helps translate CMS components into both benchmark and plan payment change.
Blum: This point is really key. Wakely’s analysis flags that rebasing/repricing impacts aren’t fully reflected yet, which means county-level outcomes can diverge materially once the final Rate Announcement is released. The rebasing could be particularly volatile this year as CMS adjusts for rural emergency hospital payments and the removal of anomalous and suspect DME claims. Both adjustments vary by geographic area.
Q: How should plans think about bid strategy and benefit pressure for 2027?
Courtney: The tighter risk adjustment environment could squeeze rebates and supplemental benefit richness—especially if bids don’t adjust quickly. Wakely estimates risk-adjusted bid and rebate revenue is down roughly 0.35 percent under a set of simplifying assumptions, underscoring the margin sensitivity.
Practically this means plans should run a few scenarios: 1) RAF compression from diagnosis source changes, 2) normalization updates, and 3) Star-related shifts—even if the Star change is estimated to be small nationally.
Blum: I’d add provider contracting and clinical program return on investment (ROI) will likely be an even greater focus for Medicare Advantage plans. When risk score lift is constrained, the value of medical cost management and quality performance becomes more important. We have seen tremendous pushback by healthcare providers over the greater use of prior authorization, with some major health systems dropping their contracts with Medicare Advantage plans altogether. Medicare Advantage plans will have to carefully balance the need to reduce medical expenditures and maintain their provider networks to attract enrollment. Establishing strong partnerships with provider systems will be more important than ever.
Q: What do plans need most right now?
Courtney: This is where integrated strategy and actuarial and policy expertise really matter. HMA is supporting stakeholders with payment impact modeling, scenario analysis, and advisory services tied to benchmark rebasing, risk adjustment, Star Ratings, product strategy, and Part D payment policy, so clients can translate the Notice into concrete bid and operating decisions.
From Wakely’s side, the detailed benchmarking and methodology interpretation helps clients quantify what CMS’s technical updates mean in dollar terms and across geographies.
The CY 2027 Advance Notice is also a reminder that average impacts hide portfolio impacts. The plans that model “where the change hits” (diagnosis sources, provider channels, county mix, Stars trajectory) will be best positioned heading into April’s final Rate Announcement.
Blum: And from a policy lens, plans need to connect the dots. CMS’s proposed rate notice is both an articulation of its current priorities and continued progression toward more payment accuracy, encounter-linked data, and program integrity. Medicare Advantage plans should be both prepared to operationalize these policies and to work with the agency to ensure its policies better serve Medicare beneficiaries.
Medicare Advantage plan leaders will be those organizations that operationalize these policy directions early, constructively engage in the policy process, and form far stronger partnerships with health care providers.
You can find more insights on the important proposed changes in plan payments, risk adjustment, and other financial and regulatory requirements for 2027 in Wakely’s summary analysis, Advance Notice of Methodological Changes for CY 2027 MA Capitation Rates and Part C and Part D Payment Policies.

Outlook 2026: Medicare Advantage Advance Notice—What It Means for the 2027 Market

This webinar was held on March 11, 2026 at 12pm ET.
This webinar offered a timely, strategic overview of the recently released proposed 2027 Notice of Benefit and Payment Parameters and what it signals for the evolving coverage landscape. We unpacked the key policy changes, operational requirements, and market assumptions embedded in the rule, with a focus on implications for the individual and small group markets beginning in 2026 and extending beyond.
Participants gained insight into how proposed updates may affect plan design, rate development, risk adjustment, enrollment operations, and health insurance regulation dynamics. We also explored the broader policy direction reflected in the proposal and what organizations should be monitoring now to prepare for implementation and potential downstream impacts.
Learning Objectives:
You can also download the related Wakely Summary of Provisions in HHS’s Proposed 2027 Notice of Benefit and Payment Parameters and Other Key Regulations