
June 21, 2023
CMS Releases National Healthcare Expenditure and Enrollment Projections through 2031
HMA Insights – including our new podcast – puts the vast depth of HMA’s expertise at your fingertips, helping you stay informed about the latest healthcare trends and topics. Below, you can easily search based on your topic of interest to find useful information from our podcast, blogs, webinars, case studies, reports and more.

CMS Releases National Healthcare Expenditure and Enrollment Projections through 2031

This week, our In Focus section highlights a Health Affairs Forefront post, “To Treat Residents With OUD, Nursing Facilities Must Improve Practices and Reduce Stigma,” published June 8, 2023. Health Management Associates (HMA) consultants Dina Besirevic, Kamala Greene Genece, Debbi Witham, David F. Polakoff, and Barry J. Jacobs wrote the article.
The HMA colleagues note that two recent healthcare industry trends are converging to change the admission criteria and clinical practices that some skilled nursing facilities (SNFs) use. Driving one movement is the opioid epidemic in which increased prevalence of fentanyl and its medical complications are spurring the need for posthospital discharge SNF admissions. The other stems from the low occupancy rates in many SNFs since the pandemic. As a result, more SNFs are considering filling beds by admitting individuals with opioid use disorder (OUD) for the first time.
In many respects, this a positive development. The need for skilled nursing care, such as medication-assisted treatment (MAT), for individuals with OUD has never been greater. A March 23, 2023, US Drug Enforcement Administration public safety alert reported that recently analyzed fentanyl samples in 48 of the 50 states had been adulterated with xylazine, or “tranq,” a veterinary sedative added to prolong an opioid high. According to the Substance Abuse and Mental Health Services Administration (SAMHSA), extensive xylazine use commonly causes severe skin wounds requiring weeks of intravenous antibiotics and skilled wound care to prevent amputations. Providing well-managed post-acute care for these patients could lead to improved outcomes.
But admitting and treating individuals with OUD now poses multiple challenges for SNF staffs and administrators. Many of these healthcare workers lack training in OUD pharmacological and support care. Some have stigmatizing attitudes toward individuals with OUD. To address these concerns, SNFs across the country have developed different practice models. Examples include:
HMA’s experts in OUD and SNFs are working collaboratively to assist SNFs interested in exploring the clinical, financial, and operational opportunities and challenges with this emerging line of business. For questions or inquiries, please contact our experts below.

To Treat Residents with OUD, Nursing Facilities Must Improve Practices and Reduce Stigma

This week, our In Focus checks in on the Medicaid unwinding work and key issues HMA experts are watching as more states resume their normal policies and processes for determining eligibility. A total of 19 states started disenrollments effective for April or May coverage, and 22 additional states plan to start ending coverage this month. States are scheduled to submit the next monthly report by June 8, 2023.
Background
As explained in earlier In Focus articles, (January 12, 2023; November 12, 2022; and April 6, 2022) federal COVID-19 relief laws allowed states to receive higher federal funding for Medicaid as long as the state did not terminate Medicaid coverage for anyone enrolled in Medicaid during the public health emergency (PHE). One result of the continuous coverage policy was sustained growth in Medicaid enrollment; more than 21 million additional individuals were continuously enrolled in Medicaid for up to three years between February 2020 and March 2023. In December 2022, Congress ended the Medicaid continuous coverage policy after March 31, 2023. States were allowed to begin processing redeterminations as early as February 2023 and start disenrolling ineligible individuals as early as April 2023.
Preparations for the Medicaid unwinding have been under way for well over two years. The Centers for Medicare & Medicaid Services (CMS), states, Medicaid health plans, providers, beneficiary advocates, and other interested stakeholders have been working to ensure that the policies, outreach, and assistance are in place to support this massive eligibility renewal and redetermination initiative.
What Do We Know… Or Not Know?
Most of the available forecasts project between 10-15 million enrollees will lose Medicaid coverage. The Health Management Associates (HMA) insurance mix model projects that more than 10 million of the approximately 90 million Medicaid enrollees are at risk for disenrollment. HMA’s model illustrates the variety in state approaches to managing the resumption of eligibility redeterminations as well as key insights related to the differential impact by Medicaid eligibility categories.
In addition, the total number of “procedural terminations” currently is difficult to determine. Lack of consistent public reporting creates gaps in the data about the number of individuals disenrolled because they did not provide a timely response to the state’s request for more information (or for other procedural reasons). As Medicaid stakeholders know, the procedural disenrollment number is critical because these individuals could still be eligible for the program.
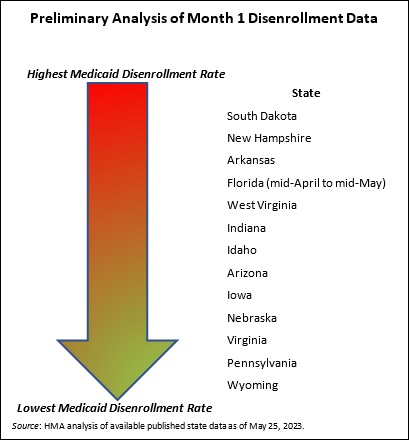
What to Watch
HMA’s experts are working with states, Medicaid health plans and their partners, providers, and advocacy organizations to identify and implement solutions to some of the known challenges. We also are looking ahead to forthcoming data, qualitative input, and other important developments that may inform federal and state policies and operations beyond the unwinding period.
Medicaid agencies, health plans, all types of Medicaid providers, and advocacy organizations should continue to analyze their immediate needs during the Medicaid unwinding. They should also be planning to identify and incorporate lessons from this transition period, as well as preparing for policy and operations changes in the post-unwinding environment.
On June 8, 2023, the Health Care Payment Learning & Action Network (LAN) will hold a virtual meeting focused on accountable primary care. The LAN — an initiative supported by the Centers for Medicare & Medicaid Services (CMS) Innovation Center — is a group of public and private health care leaders that provide thought leadership, strategic direction, and ongoing support to accelerate our care system’s adoption of alternative payment models (APMs). During the session, CMS Administrator Chiquita Brooks-LaSure and the Innovation Center’s Deputy Administrator and Director Liz Fowler will share their vision for accountable primary care.
Over the past several months CMS leaders have discussed their intent to accelerate the transition to value-based care and more accountable primary care. They have identified key principals and hinted at certain components of a potential new primary care model. Additionally, the Innovation Centers’ earlier strategy documents have highlighted the imperative to include payers beyond Medicare, importantly Medicaid and commercial insurers, in models to achieve person-centered accountable and equitable care.
This meeting is notable because the Innovation Center’s models can drive transformational shifts in health care delivery and payment across public and private payers at the system and practice levels. Providers, health systems, insurers, and other interested stakeholders will want to closely monitor the LAN discussion for more information about CMS’ evolving thinking and future opportunities related to a potential model for accountable primary care. HMA experts are available to work with health care organizations and stakeholders to interpret and respond to developments flowing from the LAN session.
Read more about LAN meeting registration and information.
If you have any questions, contact our experts below.

On May 31, the House passed H.R. 3746 – the Fiscal Responsibility Act of 2023, otherwise known as the “debt ceiling” bill, which increased the federal debt limit, established new discretionary spending limits, rescinded unused funds, and expanded work requirements for federal programs. It was passed by the Senate on June 1 and will soon be signed into law. What does all this have to do with healthcare workforce? Well, part of the rescindment plan comes from $28 billion in unused pandemic funding, with a substantial portion of those funds that were allocated for healthcare workforce efforts. This includes funds set to be used for mental health and substance use disorder training, grants to improve mental health and burnout in the healthcare workforce, and additional educational and training grants for promoting future workforce. Overall, part of $28 billion specifically includes removal of $1.7 billion from the Centers for Disease Control and Prevention (CDC) and $13.4 billion from the Department of Health and Human Services (DHHS), including $10.4 billion from public health and social services emergency funds.

So, what does this mean for the healthcare workforce? It means healthcare organizations will need to continue to optimize their current and future workforce plans, without additional funding that could provide some relief.
At Health Management Associates (HMA), our healthcare workforce experts have not only partnered with health system leaders to identify real-world solutions, we have directly experienced the same challenges, because our team includes physicians, nurses, advanced practice providers, and former health system operations and financial executives who share the same lived experiences.
HMA offers a number of workforce solutions to healthcare communities across the spectrum. We cannot fill all your staffing gaps tomorrow; however, we can give you an innovative, model-of-care plan designed to lower costs, increase revenue, and position organizations for long-term financial success and operational sustainability.
With HMA’s Delivery System Optimization Team, organizations will benefit from:
What organizations receive is:
Today’s healthcare workforce challenges are unwavering, especially given the recent passage of the “debt ceiling” bill. From significant workforce shortages, to rising costs and competition, to decreasing employee engagement and burnout, today’s health systems face tremendous challenges. But by understanding workforce and health system needs and identifying gaps and inefficiencies, employers can fully utilize the employees they have to their highest potential and deliver care more effectively and efficiently. Here at HMA, our delivery system optimization team can help health care communities struggling with workforce challenges do just that.
Contact our healthcare delivery system experts, who can partner with your organization to design a custom workforce solution for you.

This has been rescheduled from June 20, 2023
Health Management Associates (HMA) is offering a 3-part series of webinars looking at the effect of proposed regulations on delivery of opioid treatment services to the population facing addiction issues. In this third and final webinar, HMA consultants will highlight opportunities for state regulators to shape policy and regulation of SUD treatment.
New federal regulations encourage significant changes to how opioid treatment is provided, with the goal of expanding access and improving patient-centered care. State regulators will need to adapt their regulatory practices and work closely with Medicaid agencies and treatment providers so the new regulations can achieve their intended goals. This webinar will discuss how State Opioid Treatment Authorities (SOTAs), licensing entities, and state Medicaid agencies will need to work together to craft updated regulations, facility licensing, and reimbursement practices that advance person-centered care.
HMA experts will be joined by Allegra Schorr, VP, West Midtown Medical Group and President of the Coalition of Medication-Assisted Treatment Providers and Advocates (COMPA). COMPA represents New York State’s Opioid Treatment Programs (OTPs), as well as providers offering office-based medication-assisted treatment, currently providing addiction treatment to over 43,000 New Yorkers.
Learning Objectives:
Other webinars in this series:
Watch the replay of Part 1 on Opioid Treatment Providers
Watch the replay of Part 2 on Opioid State Payers Aligning Incentives for Treatment

Health Management Associates Selected as CalAIM Technical Assistance Vendor

This webinar was held on June 15, 2023.
HMA’s webinar series, 1115 Medicaid Justice Demonstration Waivers: Bridging Healthcare, focused on helping stakeholders optimize the continuity of care for persons in carceral settings and during their transition back to the community.
Part 3 focused on optimizing key partnerships before, during and after transition from a carceral setting into the community to ensure the best outcomes for individuals eligible for 1115 approved waiver services.
Learning Objectives:
Other webinars in this series:

Innovations in Publicly Sponsored Healthcare: How Medicaid, Medicare, and Marketplaces Are Driving Value, Equity, and Growth
Pre-Conference Workshop: October 29, 2023
Conference: October 30−31, 2023
Location: Fairmont Chicago, Millennium Park
Health Management Associates has announced the preliminary lineup of speakers for its sixth annual conference, Innovations in Publicly Sponsored Healthcare: How Medicaid, Medicare, and Marketplaces Are Driving Value, Equity, and Growth.
Hundreds of executives from health plans, providers, state and federal government, investment firms, and community-based organizations will convene to enjoy top-notch content, make new connections, and garner fresh ideas and best practices.
A pre-conference workshop, Behavioral Health at the Intersection of General Health and Human Services, will take place Sunday, October 29.
Confirmed speakers to date include (in alphabetical order):
Publicly sponsored programs like Medicare, Medicaid, and the Marketplaces are leading the charge in driving value, equity, and growth in the U.S. healthcare system. This year’s event will highlight the innovations, initiatives, emerging models, and growth strategies designed to drive improved patient outcomes, increased affordability, and expanded access.
Early bird registration ends July 31. Group rates, government discounts, and sponsorships are available.