This week, our In Focus section reviews the Hawaii QUEST Integration (QI) Medicaid Managed Care request for proposals (RFP), issued by the Hawaii Department of Human Services (DHS) on August 26, 2019. DHS intends to contract with four health plans. All four will serve Medicaid and Children’s Health Insurance Program (CHIP) members in Oahu, while two will also operate statewide. The two plans with the highest scoring technical proposals will serve beneficiaries statewide. The Quest Integration program is worth $2.2 billion annually.
376 Results found.

Strategies to Support Postpartum Visits for Women in Medicaid
This week, our In Focus section comes from HMA Community Strategies (HMACS) Senior Associate Diana Rodin and HMA Managing Principal Sharon Silow-Carroll who authored a recent article in the Journal of Women’s Health drawing on data from the recently completed five-year evaluation of the Strong Start for Mothers and Newborns II Initiative to identify promising approaches to support women in Medicaid to attend postpartum visits. Nationally, less than 60 percent of women enrolled in Medicaid or the State Children’s Health Insurance Program attend a scheduled postpartum medical visit, and some states have much lower rates.[1],[2]

HMA Colleagues Author Journal Article on Strategies to Support Postpartum Visits for Women in Medicaid
HMA Community Strategies (HMACS) Senior Associate Diana Rodin and HMA Managing Principal Sharon Silow-Carroll have authored an article drawing on data from the recently completed five-year evaluation of the Strong Start for Mothers and Newborns II Initiative to identify promising approaches to support women in Medicaid to attend postpartum visits.

Jonathan Blum to Join HMA as Managing Principal
Jonathan (Jon) Blum will join HMA as a managing principal on Aug. 31 working out of the Washington, DC office.
He has more than 20 years of senior-level experience working in public and private healthcare financing organizations, including the Centers for Medicare and Medicaid Services (CMS).

CMS Medicare Fee-For-Service FY2020 Proposed Rules: Hospital Outpatient Department and End-Stage Renal Disease
This week, our In Focus section reviews the new Centers for Medicare & Medicaid Services (CMS) Medicare Fee-For-Service FY 2020 proposed rules. On July 29, 2019, CMS issued the Calendar Year (CY) 2020 proposed rules for the Physician Fee Schedule (PFS), the hospital outpatient department (HOPD) and ambulatory surgical center (ASC) prospective payment systems (PPS), and the End-Stage Renal Disease (ESRD) PPS. These proposed regulations include payment rate and policy changes for the upcoming calendar year. The comment deadline for all three of these proposed rules is September 27, 2019.

CMS Releases Section 1332 Waiver Application Resource Tools
This week, our In Focus section reviews the new 1332 State Relief and Empowerment Waiver resources released by the Centers for Medicare & Medicaid Services (CMS) on July 15, 2019. The new resources, intended to help states better understand regulations and reduce burdens associated with waiver application, include four waiver concept papers on how states can take advantage of the flexibility to wave certain Affordable Care Act (ACA) requirements, as well as their respective application templates. CMS has also released an updated application checklist of required elements.

California 2019-20 Budget Overview
This week, our In Focus section reviews the California fiscal 2019-20 budget. California Governor Gavin Newsom signed his first budget, and much of its related legislation on June 27, 2019. The budget appropriates $214.8 billion ($147.8 billion General Fund) in total spending with $19.2 billion in reserves. The total reserves includes $16.5 billion in the Rainy Day Fund, $1.4 billion in the Special Fund for Economic Uncertainties, $900 million in the Safety Net Reserve, and nearly $400 million in the Public School System Stabilization Account.

Dual Eligible Financial Alignment Demonstration Enrollment Update
This week, our In Focus section reviews publicly available data on enrollment in capitated financial and administrative alignment demonstrations (“Duals Demonstrations”) for beneficiaries dually eligible for Medicare and Medicaid (duals) in nine states: California, Illinois, Massachusetts, Michigan, New York, Ohio, Rhode Island, South Carolina, and Texas. Each of these states has begun either voluntary or passive enrollment of duals into fully integrated plans providing both Medicaid and Medicare benefits (“Medicare-Medicaid Plans,” or “MMPs”) under three-way contracts between the state, the Centers for Medicare & Medicaid Services (CMS), and the MMP. As of May 2019, approximately 372,600 duals were enrolled in an MMP. Enrollment was flat from May of the previous year.

HMA, CMCS Launch Resource for Medicaid Innovation Program
A team of HMA consultants, led by Izanne Leonard-Haak and Matt Roan, have collaborated with organizations under a Centers for Medicaid and CHIP Services (CMCS) contract to provide support to CMCS on the Medicaid Innovation Accelerator Program.

Kentucky Releases Medicaid MCO RFP
This week, our In Focus section reviews the Kentucky Medicaid managed care organizations (MCOs) request for proposals (RFP), issued by the Kentucky Finance and Administration Cabinet on May 16, 2019. The Kentucky Cabinet for Health and Family Services (CHFS), Department for Medicaid Services (DMS) will select up to five Medicaid MCOs to manage health care services for more than 1.2 million people, starting July 2020. Contracts are estimated at more than $7 billion.

Medicaid Plan Profit Margin Dips to 0.5 Percent in 2018, Continuing Multi-Year Decline, HMAIS Analysis Shows
This week, our In Focus summarizes the findings of an HMA Information Services analysis of Medicaid managed care plan profitabilty, based on data from annual statutory filings made with the National Association of Insurance Commissioners (NAIC). For information on how to subscribe to HMA Information Resources, contact Carl Mercurio.
Underwriting Margin
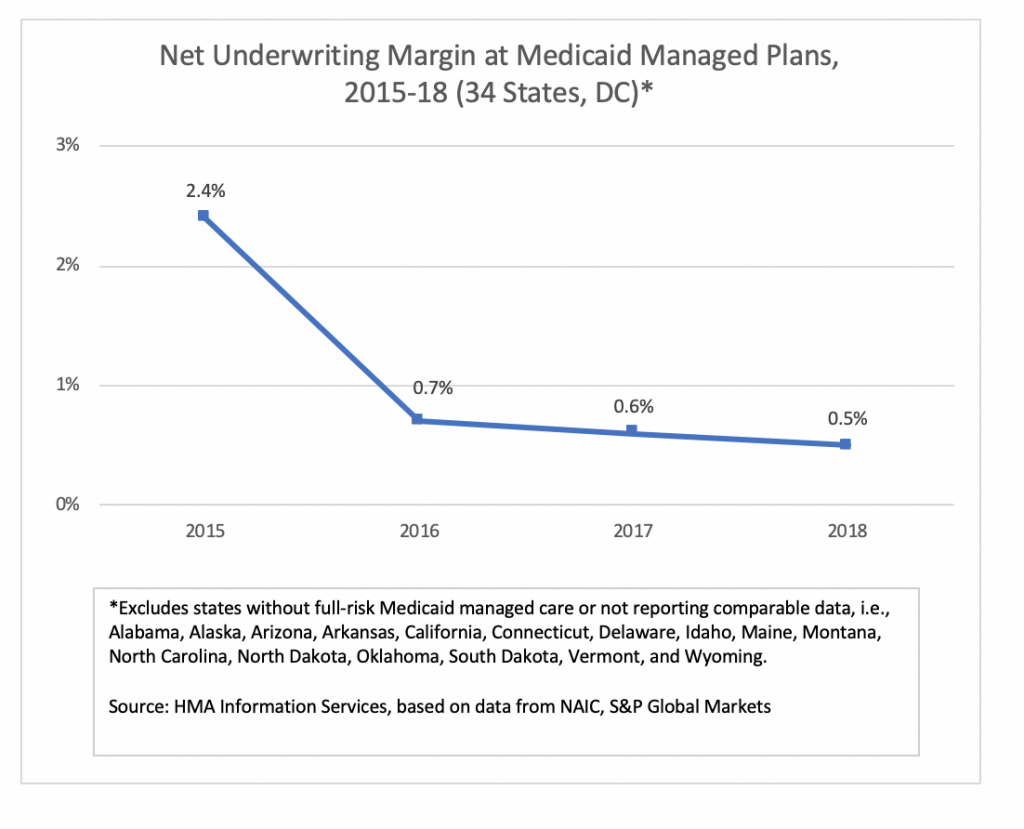
An analysis by HMA Information Services, a division of Health Management Associates, shows that Medicaid managed care plans in 34 states and Washington, DC, posted a net underwriting margin of 0.5 percent in 2018, down 10 basis points from 0.6 percent in 2017. For-profit plans posted higher underwriting margins than not-for-profit plans.
Overall, margins have fallen consistently since hitting a four-year high of 2.4 percent in 2015. The data include financial information for about 210 Medicaid managed care plans, with total membership of 37 million in 2018 and revenues of about $188 billion. Net underwriting profit in 2018 was about $911 million, compared to more than $990 million in 2017.
States in which the aggregate Medicaid managed care margin was below the national average in 2018 (based on plans reporting NAIC statutory filings) included Florida, Hawaii, Louisiana, Massachusetts, Mississippi, New Jersey, New Mexico, Rhode Island, Texas, and Virginia.
Not included in the tally are most Medicaid plans in California and Arizona, which don’t report financial information through NAIC. In addition, some of the largest plans in New York don’t report financial information through NAIC.
Medical Loss Ratio
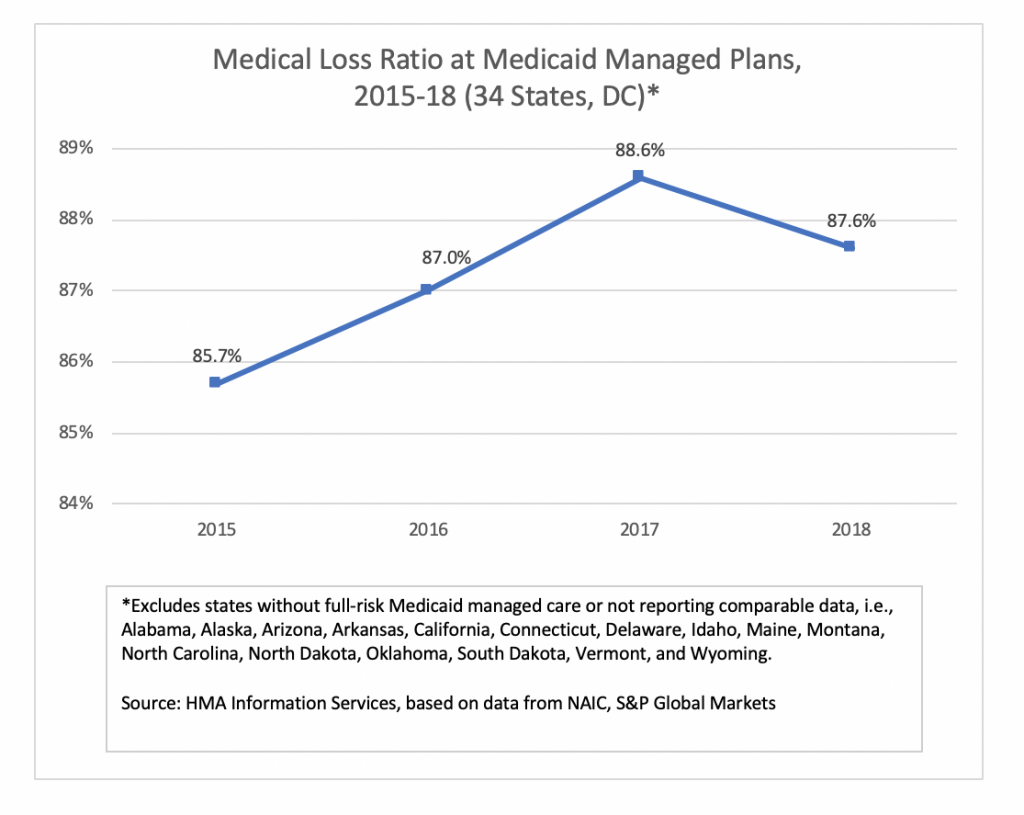
Medical loss ratio (MLR) among Medicaid managed care plans in 34 states and Washington, DC, was 87.6 percent in 2018, down about 100 basis points from 2017. The MLRs calculated by HMAIS are blended and may include traditional Medicaid, expansion, and aged, blind and disabled populations, depending on the state. The improvement in average MLR was offset by an increase in administrative costs, resulting in the drop in underwriting margin.

Medicaid and Exchange Enrollment Update – January 2019
This week, our In Focus section reviews updated information issued by the Department of Health & Human Services (HHS) Centers for Medicare & Medicaid Services (CMS) on Medicaid expansion enrollment from the “January 2019 Medicaid and CHIP Applications, Eligibility Determination, and Enrollment Report,” published on April 25, 2019. Additionally, we review 2019 Exchange enrollment data from the “Health Insurance Exchanges 2019 Open Enrollment Period: Final State-Level Public Use File,” published by CMS on March 25, 2019. Combined, these reports present a picture of Medicaid and Exchange enrollment in 2019, representing 72.4 million Medicaid and CHIP enrollees and 11.4 million Exchange enrollees.