1261 Results found.

How One Organization Unlocked Exceptional Financial Gains Through Revenue Cycle Optimization
A recent case study highlighted how Health Management Associates (HMA) worked with a medical supply firm to identify gaps in their revenue cycle, and by working with us have seen improvements in denial rates and reimbursement. Advanced Diabetes Supply (ADS)/ US Medical Supply (USMed) came to HMA for help with its revenue cycle goals. What began as a revenue cycle gap assessment at one ADS office in California was expanded to be repeated for the Florida office. As a result, HMA helped ADS produce 12% YoY increase in cash collections, resulting in more than $38 million in additional revenue, and a $16 million reduction in outstanding A/R within six months.
A leading provider of diabetes supplies, ADS faced challenges in optimizing their revenue cycle processes. By partnering with HMA, they embarked on a transformative journey that resulted in streamlined operations and improved financial performance. The case study highlights the key strategies implemented by ADS and HMA, including the adoption of advanced technologies, process re-engineering, and staff training. These initiatives not only addressed existing inefficiencies but also paved the way for future growth and innovation.
Organizations need efficient revenue cycle management to ensure sustainability and growth in the constantly changing and competitive healthcare landscape. As healthcare reimbursement can involve many complex processes, it creates opportunities for gaps and process breakdowns. HMA helps organizations implement the processes, training, and technology necessary to close process gaps, improve cash flow, determine root causes for gaps, and reduce denials.
HMA experts have decades of experience in every facet of the revenue cycle. They come from all sides of the healthcare industry, including providers, payers, managed care organizations, and more.
Delve deeper into this inspiring success story by downloading the full case study and watching the accompanying video featuring a conversation with Melanie Montero, SVP at Advanced Diabetes Supply.

Evolving Medicaid Work Requirement Policies: Essential State Actions to Prepare
On May 22, 2025, the US House of Representatives advanced a comprehensive legislative package that includes expansive changes to healthcare spending and tax policies. The One Big Beautiful Bill Act, H.R. 1, will be subject to further revision in the Senate – and potentially again in the House – before it can be sent to the president for his signature. If enacted, the legislation would have significant implications for the Medicaid program, including a nationwide work and community engagement requirement. The House-passed bill establishes a deadline of December 31, 2026, for implementation, but individual states could move earlier.
As state legislatures pass work requirement bills, governors consider executive actions, and Congress contemplates revisions to the Medicaid work mandate, vetting key implementation issues may significantly affect the direction of related policies. Even before implementation, states must test operations, enable systems, and establish connections to beneficiaries to reduce potential implementation missteps, inappropriate disenrollments, and litigation risks.
If the goal of Medicaid work requirement policies is to stimulate connections between health benefits and employment/workforce, building state and federal capacities to support these approaches is critical to effectuating that change. In the remainder of this article, Health Management Associates (HMA), experts focus on the operational dynamics that need to be discussed, tested, and built as states begin introducing work and community engagement initiatives.
Federal Policies and Early State Actions on Work Requirements
The House bill would require all states to implement work and community engagement requirements for adults without dependents for at least 80 hours per month.[1] Employment, work programs, education, or community service (or a combination of those activities) would satisfy the requirement.
The work requirements in the House-passed legislation would apply only to individuals between the ages of 19 and 64 without dependents, and the following groups are exempted:
- Women who are pregnant or entitled to postpartum medical assistance
- Members of Tribes
- Individuals who are medically frail (i.e., people who are blind, disabled, with chronic substance use disorder, has serious or complex medical conditions, or others as approved by the Secretary of the US Department of Health and Human Services)
- Parents of dependent children or family caregivers to individuals with disabilities
- Veterans
- People who are participating in a drug or alcoholic treatment and rehabilitation program
- Individuals who are incarcerated or have been released from incarceration in the past 90 days
In addition, individuals who already meet work requirements through other programs, such as Temporary Assistance for Needy Families (TANF) or the Supplemental Nutrition Assistance Program (SNAP), would be exempt. However, the House-passed version would make the eligibility verification and work requirements for SNAP more stringent and shift program costs to these states, which would affect cross-functional eligibility. The legislation also includes temporary hardship waivers for natural disasters and areas with an unemployment rate greater than 8 percent (150 percent of the national average).
Though the federal budget package has received a great deal of attention, at least 14 states already have moved forward (see Table 1) in advance of the current federal debate by passing laws and submitting work requirement demonstration requests to the Centers for Medicare & Medicaid Services (CMS).
Table 1. A Review of 2025 States’ Approaches to Work Requirements in Medicaid
| Status | State | Population Criteria | Requirements | Exemptions/ Notes | Public Comment |
| Work Requirement Request Submitted | Arizona | Ages 19−55 | 80 hours/month | Multiple exemptions; 5-year lifetime limit | Closed |
| Work Requirement Request Submitted | Arkansas | Ages 19−64; covered by a qualified health plan (QHP) | Data matching to assess whether on track/not on track | No exemptions | Closed |
| Work Requirement Amendment Request Submitted | Georgia | Ages 19−64; 0-100% FPL | 80 hours/month | Already has approval but is requesting reporting be changed from monthly to annually and adding more qualifying activities | Federal comment period open through June 1, 2025 |
| Work Requirement Request Submitted | Ohio | Ages 19−54; expansion adults | Unspecified hours | Limited list of exemptions | Closed |
| Legislation Passed | Idaho | Ages 19−64 | 20 hours/week required | Limited list of exemptions | — |
| Legislation Passed | Indiana | Ages 19−64; expansion adults | 20 hours/week required | Limited list of exemptions | — |
| Legislation Passed | Montana | Ages 19−55 | 80 hours/month required | Multiple exemptions | — |
| Ballot Initiative Passed | South Dakota | Expansion adults | — | 2024 ballot initiative asking voters for approval for state to impose work requirements for expansion adults passed | — |
| Legislation Pending | North Carolina | — | — | Pursue requirements that are CMS approvable | — |
| Work Requirement Request Draft | Iowa | Ages 19−64; expansion adults | 100 hours/month required | Limited list of exemptions Separate bill would end expansion if work requirements are withdrawn/ prohibited (80 hr./mo.) | Closed |
| Work Requirement Request Draft | Kentucky | Ages 19−60; no dependents; enrolled more than 12 months | Connected to employment resources | Multiple exemptions | State comment period open through June 12, 2025 |
| Work Requirement Request Draft | South Carolina | Ages 19−64; 67%−100% FPL | Specified activities (work specific is 80 hours/month) | Limiting participation to 11,400 individuals based upon available state funding | State comment period open through May 31, 2025 |
| Work Requirement Request Draft | Utah | Expansion adults ages 19−59 | Register for work, complete an employment training assessment and assigned job training, and apply to jobs with at least 48 employers within 3 months of enrollment | Several exemptions, largely aligned with federal SNAP exemptions | State comment period open through May 22, 2025 |
| Anticipated Waiver Request | Alabama | Non-expansion population | — | Potential to resubmit previous work requirement demonstration request | — |
Key Questions to Guide State Policy Decisions
Considerable research and findings from previous Medicaid work requirement initiatives can help prepare policymakers to implement a potential new phase of Medicaid work requirement policies. Some previous findings include the high cost of administration relative to potential savings, the importance of systems that support foundational items like logging an enrollee’s compliance activities and exemptions, as well as developing an efficient appeals process. The Medicaid and CHIP Payment and Access Commission (MACPAC), General Accounting Office, National Institutes for Health, and multiple researchers have published assessments regarding previous experiences that could prove useful in policy making.
HMA experts have experience identifying key issues and considerations, analyzing options, and implementing critical issues and for state leaders and stakeholders who will be responsible for implementing work requirements. Several of these issues are described below and in more detail in the HMA blog, Building State Capacities for Medicaid Work and Community Engagement Requirements.
- Exemptions, particularly medical frailty definitions and assessments. The federal government and states will need to identify individuals classified as “medically frail” and make them exempt from the mandates. Medically frail individuals include those with chronic, serious, or complex medical conditions. Various methods can be employed to identify these people.
- Developing and streamlining systems and processes to promote continued coverage for eligible individuals. The Medicaid unwinding from the COVID public health emergency taught policymakers lessons about the complexities of Medicaid systems, patient engagement, and reliable methods of member outreach. State Workforce Commissions and Departments of Labor are clear partners, as they manage integrated eligibility systems and data-sharing agreements across programs like SNAP and TANF, which also serve many Medicaid participants. These and other partnerships will need further exploration.
- Clinical and utilization data that promote eligibility assessment. Many, but not all, individuals with chronic diseases may be exempt from the requirements. Knowing the health status and chronic conditions of the populations affected and the conditions that qualify people for exemption are variables as implementation questions, like the definition of medically frail, are addressed.
- Anticipated need for effective Medicaid managed care engagement in work requirements/community engagement initiatives. Approximately 80 percent of Medicaid expansion enrollees are members of comprehensive managed care organizations (MCOs). States will need to review the scope of existing vendor contracts as well as determine the need for new services, roles, third-party reporting, oversight, and potential exemptions for emergencies. Work requirements can disrupt MCO risk pool stability and care coordination. MCOs have a financial incentive to drive down inappropriate disenrollments and are uniquely positioned to support state responsibilities, including maintenance of up-to-date contact information.
- Measuring impact and adapting policies as needed. Dynamic metrics that provide actionable information to federal and state policy makers will support effective oversight and monitoring.
Connect with Us
HMA helps stakeholders—including state agencies and their partners—manage the challenges of implementing new Medicaid or CHIP initiatives, with a focus on ensuring efficient integration and improvements in outcomes. Our teams are adept at developing materials for and supporting stakeholder engagement from design to implementation, which is a critical aspect for work and community engagement initiatives and other potential new eligibility and renewal requirements.
For support tracking federal and state level developments and enhancing your organization’s strategy and preparations for new Medicaid requirements, contact our featured experts below.
[1] U.S. Congress. House. One Big Beautiful Bill Act. H.R.1. 119th Cong., 1st sess. Introduced May 20, 2025.

May 28, 2025
Building State Capacities for Medicaid Work and Community Engagement Requirements

What If Mental Health Checkups Were as Normal as Mammograms?
Monica Johnson, managing director at Health Management Associates, takes us through her compelling journey from frontline caregiver to national leader in behavioral health policy. In this episode of Vital Viewpoints on Healthcare, Monica reflects on the national rollout of the 988 crisis line as one of the most transformative shifts in creating a stigma-free behavioral health system of care that meets people where they are to support whatever crisis they may face. Monica shares personal stories and strategic insights that illuminate why policymakers must ensure these systems prioritize the local needs of patients and providers. We explore the future of crisis care, the enduring need for bold federal-state collaboration, and why it’s time to normalize mental health checkups.

The Changing Behavioral Health Landscape in a Time of Fiscal Uncertainty; Learn more at HMA’s Behavioral Health Town Hall May 29
It is hard to keep abreast of the changes being made to the healthcare system at the Federal level, and how these changes will impact behavioral health (BH) services. The current reprioritization of funding by the Department of Health and Human Services (HHS) and the proposed changes in the budget bill pending in Congress will significantly reshape Medicaid and critical behavioral health programs. States and local organizations will need to sharpen their understanding of this new funding landscape, so they are able to focus on addressing critical needs for prevention and treatment of mental health and substance use disorders.
Register today – HMA’s Behavioral Health Town Hall, Thursday, May 29 at 12 p.m.
With Federal funding levels in question, States and their stakeholders need to consider how they are funding BH initiatives. We’ll address participant questions and topics we know are top of mind, for example:
What steps can states take to ensure sustainable funding for critical programs? Are states strategically utilizing their Medicaid programs to preserve BH specific program dollars for other purposes? What efficiencies and enabling technologies can organizations adopt to support their mission? How should state and local entities be thinking about the opioid settlement dollars to maximize support for services and initiatives that face uncertain future financial support?
In addition, Congress is debating changes to Medicaid eligibility and funding policies that may result in shifts in key aspects of the program. States can start planning now for changes to their processes and for outreach and education campaigns that will be essential in supporting individuals with mental health and substance use disorder diagnoses. Payers should be planning for changes in enrollment and enrollee risk profiles while providers should expect changes in their payer mix and a need for enhanced collaboration with community organizations. Are there different models that can be pursued to effectively navigate these shifts? How will all of this uncertainty affect the BH workforce? Stakeholders need to be prepared to engage in downside risk arrangements, think about their patient/consumer engagement strategies and integrating digital BH tools that are the focus of the CMS Innovation Center agenda.
You probably have questions that we didn’t even list here. Here is your chance to ask them: Join HMA on Thursday, May 29 at 12 p.m. at a dynamic and interactive Behavioral Health Town Hall where HMA experts Heidi Arthur, Rachel Bembas, Allie Franklin, Teresa Garate, Monica Johnson, and Sara Singleton will be available to answer your questions live on a wide range of critical topics, including:
- Federal policy, personnel, and funding changes;
- Emerging strategies for addressing social determinants of health, substance use disorder and crisis coordination (including 988);
- Leveraging cross-sector partnerships to build ecosystems of care across communities promoting coordination and collaboration;
- Behavioral health revenue cycle management and alternative payment models; and
- Innovations in addressing workforce shortages, integrated service delivery, digital mental health tools, and best practices for community mental health service delivery.
Whether you’re navigating regulations, searching for new funding, designing service delivery systems, or just trying to understand what happens next, this town hall is your chance to ask questions, share insights, and discuss real-world solutions with industry experts.

CMS Seeks Input on the Future of Digital Health: What the Health Technology Ecosystem RFI Means for Stakeholders
This week, in our In Focus section, health IT experts at Leavitt Partners, an HMA Company, review the recently released Request for Information (RFI) from the Centers for Medicare & Medicaid Services (CMS) and the Assistant Secretary for Technology Policy/Office of the National Coordinator for Health (ASTP/ONC), titled Health Technology Ecosystem (CMS-0042-NC). The RFI, published May 16, 2025, signals a renewed federal focus on advancing digital health tools, improving data interoperability, and supporting patient-centered innovation.
Notably, this RFI aligns with the vision laid out in Leavitt Partners’ Kill the Clipboard policy blueprint, developed in collaboration with a broad coalition of healthcare stakeholders. The paper outlines a future in which patients and providers benefit from seamless digital experiences, real-time data exchange, and reduced administrative burden. The RFI reflects many of the same priorities—such as expanding FHIR® Application Programming Interfaces (APIs), improving provider directories, and promoting digital identity solutions—that were highlighted in the paper as essential to modernizing the healthcare system.
Why This RFI Matters
The RFI invites public input on how CMS and ASTP/ONC can strengthen the digital health ecosystem for Medicare beneficiaries. It builds on years of federal investment in interoperability. The agencies are now seeking feedback on how to reduce barriers to data access, promote innovation in digital health products, and align technology with value-based care goals.
This is a pivotal opportunity for stakeholders to shape the future of digital health policy—especially as CMS continues to explore how APIs, digital identity, and patient-facing tools can improve care delivery and outcomes.
Key Themes in the RFI
The RFI is broad in scope, but several themes stand out, including:
- Addressing Patient and Caregiver Needs: The RFI asks patients which digital tools would be most helpful to them and their caregivers in managing their health needs, navigating care, and accessing all relevant health information in one place. It asks what features are most needed, what is missing from current apps, and how CMS can support adoption, especially for Medicare beneficiaries with limited digital experience. CMS is exploring how to make more data—beyond claims and clinical data—available through APIs. It also explores the role that CMS should play in reviewing and measuring the real-world impact of these tools on outcomes and costs. They also are considering how to promote the use of secure, standardized digital identity credentials (e.g., Login.gov, ID.me) to streamline patient access. Feedback also is sought on how TEFCA, FHIR APIs, and health information exchanges (HIEs) can better support seamless data exchange.
- Provider Adoption of Digital Health Tools: CMS is exploring how to help providers, especially those in rural areas, adopt digital health tools by addressing barriers like workflow integration, data access, and interoperability. CMS is also looking to improve administrative functions like scheduling and intake through third-party apps. In addition, CMS is seeking to understand which FHIR APIs and capabilities are already being supported or utilized in provider systems. They are also interested in understanding how providers might accept standardized digital identity credentials from patients and any challenges that might inhibit its adoption. ASTP/ONC is also seeking information on revisions to the information blocking requirements.
- Engaging Payers: The RFI invites payers to share how they can support interoperability and digital innovation, including through the use of APIs, digital identity credentials, and real-time access to clinical quality data. CMS is also interested in how payers can reduce provider burden, support value-based care (VBC), and contribute to a more connected digital health infrastructure. Feedback is requested on TEFCA participation, payer-to-payer data exchange, and the potential for a nationwide provider directory.
- Advancing VBC Organizations: The RFI emphasizes the role of digital health in supporting alternative payment models (APMs) and accountable care organizations. CMS is seeking feedback on which digital capabilities are most essential for success in VBC—such as care coordination, quality measurement, and patient engagement—and how certification criteria and data standards can better align with these needs. The agencies are also exploring how to reduce complexity for APM participants while maintaining flexibility and data access.
- Enabling Technology Vendors, Data Providers, and Networks: The RFI requests feedback from developers, data aggregators, and HIEs on how to unlock innovation through better access to CMS data, improved API standards, and streamlined certification processes. The RFI asks which technical and policy changes would enable more effective digital health products, recommendations to improve interoperability across networks, and means of supporting the viability of data exchange infrastructure.
Implications for Stakeholders
This RFI is more than a technical exercise; it is a strategic signal. The Trump Administration is maintaining momentum behind VBC and digital transformation. Stakeholders should consider:
- Submitting comments to CMS by the June 16, 2025, deadline.
- Assessing internal readiness to adopt or develop digital tools that align with CMS’s vision.
- Engaging in policy discussions regarding digital identity, data standards, and patient access.
- Monitoring related RFIs, including the Food and Drug Administration RFI exploring the potential use of HL7 FHIR standards to support the submission of study data derived from real-world data sources—such as electronic health records, claims, and registries—for regulatory purposes.
Next Steps
Health Management Associates, Inc. (HMA), encourages healthcare organizations to review the RFI and consider how their experiences, innovations, and challenges can inform CMS’s next steps. This is a rare opportunity to influence the infrastructure that will shape digital healthcare for years to come.
For support in drafting comments or understanding how this RFI intersects with your organization’s strategy, contact our Leavitt Partners health IT experts below.

CMS Announces New Innovation Agenda: Here’s What You Need to Know
On May 13, 2025, the Centers for Medicare & Medicaid Services (CMS) published its new strategic direction for the CMS Innovation Center. The strategy builds on the lessons of the first 15 years of the Innovation Center, while presenting a significant pivot in policy direction, which emphasizes evidence-based prevention, consumer engagement, and tech-enabled care, while prioritizing financial performance over broad participation.
The new strategy provides high-level direction on the Trump Administration’s vision for the next phase of value-based payment reform under the leadership of CMS Administrator Dr. Mehmet Oz and Innovation Center Director Abe Sutton. They intend to “double down on our commitment to value-based care and take the learnings from the[se] previous investments to build a health system that empowers people to drive and achieve their health goals and Make America Healthy Again.” Notably, the strategy also aligns with goals central to the Trump Administration’s Make America Healthy Again initiative.
This new direction affirms the administration’s commitment to continue advancing value-based care and opens additional opportunities for organizations seeking to enhance the delivery of services that drive positive outcomes. Health Management Associates (HMA), experts will be tracking the implementation of the Innovation Center’s new strategy, including expected forthcoming models, movement toward greater levels of downside risk, and changes to existing models to align with the administration’s priorities. In this article, our experts review the strategy and provide insights on key takeaways for stakeholders.
New Strategy Overview
CMS leaders view the Innovation Center agenda as a framework for accelerating healthy behaviors, leveraging the agency’s authority to test new approaches designed to incentivize and engage stakeholders. According to CMS officials, the Innovation Center “will work expeditiously toward the future of health—building a system in which people are empowered to achieve their health goals and providers are incentivized to compete to deliver high-quality, efficient care and improve the health outcomes of their patients.”
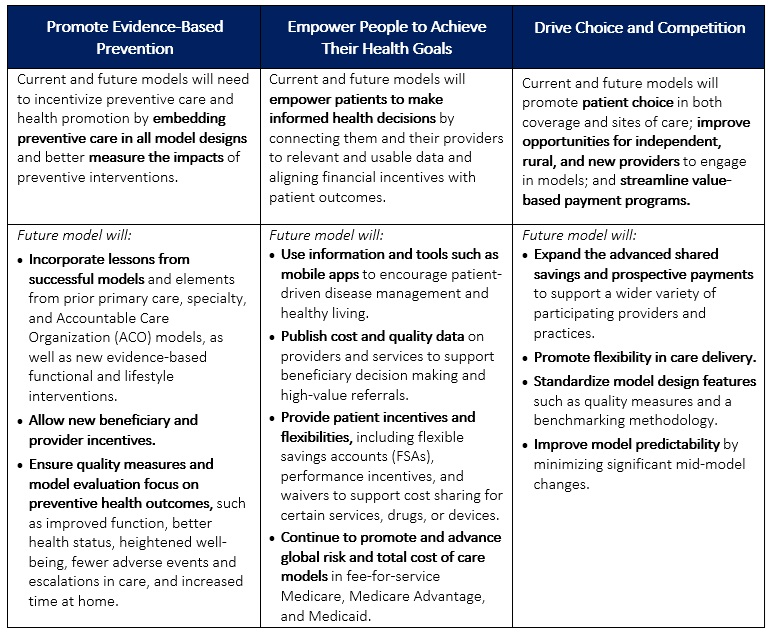
The strategy has three interrelated, foundational pillars:
- Promoting evidence-based prevention
- Empowering people to achieve their health goals
- Driving choice and competition.
Table 1 provides more detail on each pillar.
In addition to the new agenda, CMS released a request for information (RFI) seeking industry input on strategies that can better leverage data and technology to empower consumers. The focus of the RFI aligns with the Innovation Center’s strategic pillars to use tools, information, and processes that better connect people to their health data and allow them to make informed health decisions alongside their providers.
Table 1. CMMI’s Interrelated Strategic Pillars
Takeaways and Considerations
Critical to CMS’s approach is the belief that empowering individuals to make their health decisions—through incentives, better data access, and more flexible options—can lead to better health outcomes and lower overall costs. This shift reflects an evolution in healthcare policy that places greater emphasis on personal accountability and private sector collaboration—a key theme that is emerging across the administration’s policy initiatives.
Consumer Engagement. One of the most notable aspects of the new Innovation Center strategy is the promotion of consumer engagement; it places more focus on direct consumer engagement through education and incentives compared with earlier initiatives. This is one area in which the Innovation Center plans to collaborate with the private sector to develop consumer-facing tools (e.g., mobile apps, nudges toward healthy behaviors, etc.).
The focus on consumer engagement also presents opportunities for organizations to enhance their customer experience. By understanding the needs and preferences of their patients, organizations can tailor their services and care models to better meet those demands. This personalized approach not only improves patient satisfaction, but also drives continuity of care, ultimately contributing to long-term improvements in health.
Data and Technology. The new strategy also emphasizes the importance of data, indicating intentions to better equip organizations that participate in the model with data that can inform decisions and optimize their processes. CMS officials are examining policies and collaborations that will empower private sector organizations, including model participants, researchers, and technology vendors, to develop innovative data-driven solutions to drive efficiencies and improved health.
To that end, the May 16, 2025, Request for Information (RFI) from CMS and the Assistant Secretary for Technology Policy/Office of the National Coordinator for Health (ASTP/ONC), Health Technology Ecosystem (CMS-0042-NC), focuses on Medicare beneficiaries’ use of technology to improve health outcomes. The RFI, which HMA experts analyze here [insert bookmark or link to the other In Focus article] underscores the administration’s intentions of taking “bold steps to modernize the nation’s digital health ecosystem.”
Medicare Advantage. The Innovation Center’s new strategy indicates that stakeholders should expect more models that address Medicare Advantage (MA). The agency stated that “features of a model could include testing changes to payment for MA plans, such as testing the impact of inferred risk scores, regional benchmarks, or changes to quality measures that better align with promoting health.” Additionally, the strategy references a forthcoming specialty-focused longitudinal care model within MA and Medicaid, signaling intentions to drive multi-payer alignment.
Saving Federal Tax Dollars. Another major aspect of the strategy is “protecting federal taxpayers.” This goal reflects a continued emphasis on total cost of care accountability and indicates a more aggressive shift to downside risk. The Innovation Center says it will “require all models to have downside financial risk and require providers to assume some of the financial risk..” Additional provisions of protecting tax dollars include reducing role of state governments in rate setting, simplifying model benchmark methodology, and ensuring “proper and nondiscriminatory provision of funds for health care services.”
What to Watch
For healthcare organizations, the Innovation Center’s agenda signals a need to prioritize consumer-centric models. Hospitals, providers, and insurers should anticipate the following:
- Increased focus on preventive care initiatives to align with new model designs
- More robust data-sharing and technology requirements, meaning investments in patient-focused digital tools will become essential
- New opportunities in MA, given potential payment model innovations affecting plan structures and risk-adjusted reimbursement
Healthcare stakeholders should monitor possible developments related to the strategy.
- While details on specific strategies have yet to emerge, the Innovation Center indicated it plans to provide more information on new models, as well as changes to existing models, in the coming months.
- The Innovation Center has not provided a goal akin to the previous administration’s effort to have 100 percent of Medicare beneficiaries in accountable care relationships by 2030. It is still unknown whether these goals are forthcoming or if this will remain vague.
- Stakeholders are still awaiting clarity on changes to existing models, including key models set to conclude at the end of 2026 (i.e., ACO REACH and Kidney Care Choices).
- Strategy language indicates that the agency may develop payment innovation in prescription drugs, medical devices, and technology.
Connect With Us
The Health Management Associates Annual Conference, Adapting for Success in a Changing Healthcare Landscape, October 14-16, 2025, in New Orleans, LA, will feature discussions on how the new strategy is reshaping the healthcare system and care delivery for patients, particularly the opportunities to revisit provider contracts with MA plans and to integrate technology to advance the prevention of chronic conditions and achieve population health goals.
For more information about the opportunities and considerations the Innovation Center agenda presents for your organization, contact HMA’s featured experts below.

Transforming Crisis Care Intervention: The Role of 988
This week, our third In Focus section highlights the national 988 Suicide and Crisis Lifeline, the three-digit number for individuals in need of behavioral health crisis support. The 988 Lifeline is composed of 200-plus contact centers across the country, which connect people to trained counselors to deescalate crises, provide behavioral health resources, or connect individuals to an in-person responder. Supported by federal legislation to help create a nationwide, standardized, easy to remember 3-digit number, the program is still in its early stages, having been established three years ago this coming July.
In this article, Health Management Associates (HMA) experts provide important context about the 988 Lifeline and future policy direction and suggests actions state leaders can take to enhance use of this critical resource.
988 Lifeline: A Product of Coordinated Collaboration
The story of how the 988 Lifeline was created is an example of long-term advocacy and innovation that demonstrates how a solution needs to combine the state and local decisionmakers with federal policy and support. People experiencing a mental health crisis, thoughts of suicide, or concerns about substance misuse should receive the appropriate local response to seek support or care.
Prior to the 988 Lifeline, individuals experiencing a behavioral health crisis may have contacted 911 and, therefore, not always received the most appropriate response for their unique needs. In some situations, 911 responders—typically law enforcement, emergency medical services, or hospital emergency departments—are ill-equipped to direct people experiencing a behavioral health crisis. Trained behavioral health professionals responding to an individual experiencing a crisis is the appropriate intervention at most points of access. Increased diversion from 911 calls to 988 when an individual is experiencing a behavioral health crisis is an expected long-term outcome.
The federal government’s role is to continue to support the work to enhance the 988 Lifeline, but there’s so much more that needs to happen to increase education and awareness in states, localities, and Tribal nations. They still need support in building out their systems.
State Initiatives Strengthening the 988 Lifeline
Since the launch of the 988 Lifeline in July 2022, 50 percent of the states have approved some type of appropriation or some type of legislation to further cement 988 in their local communities. Some states have established trust funds or implemented 988 cell phone fees similar to what 911 does to provide financial support. Other states have established committees to study and support 988 implementation, building out the various components of a true coordinated crisis system of care.
HMA experts have identified strategic and operational recommendations to support this ongoing work, including:
- Be intentional about having the right people at the table where decisions are made, including voices with lived experience and people who are part of the policy-making process. Establishing this formal, standardized 988 system enables local communities to better allocate resources in crisis situations. In most cases, the contact with the 988 Lifeline is the best intervention to ensure people get the support or resources needed to resolve or deescalate the crisis.
- When designing a crisis system in a community, think about prevention and what happens when the crisis is over. Crisis systems established on a poor behavioral health foundation will fail. Stakeholders and decisionmakers should continue building out their systems by remembering that the entire continuum of care—from crisis to ongoing support—is needed.
- Identify the data that are needed to tell the story about the value of the 988 Lifeline and crisis care systems. Anecdotes are essential and should be paired with data, especially when ongoing funding is needed.
Where Is the 988 Lifeline Headed?
It is likely to take decades to generate greater awareness about the 988 Lifeline, to have interoperability between 911/988, to ensure every person in the country has access to the service no matter their zip code, and to see a fully transformed behavioral health crisis system will take decades to accomplish. The collaboration between federal, state, territories, Tribal nations, and local communities is pivotal to reaching these goals.
While we are at the beginning phases of this work, much has been done that should be celebrated. The 988 Lifeline has transformed how we as a nation talk about behavioral health and suicide prevention. Still, we as a collective have work ahead to achieve the vision of transforming the behavioral health crisis care system.
Connect with Us
Health Management Associates (HMA) is hosting a live, interactive event on Thursday, May 29, 2025. [The Ask the Experts: Behavioral Health Town Hall https://www.healthmanagement.com/insights/webinars/ask-hma-experts-behavioral-health-town-hall/ ] will explore the latest developments in behavioral health—from policy shifts and funding trends to real-world solutions for service delivery, workforce challenges, and system design. HMA and Leavitt Partners, an HMA Company, experts will be on hand to answer participant questions and share insights about 988 and other topics:
- Policy and funding updates at the federal level
- Innovative approaches to crisis response, 988 implementation, and substance use services
- Revenue cycle improvements and evolving payment models
- Strategies to strengthen the workforce, integrate care, and leverage digital mental health tools
For more information about 988 systems and effective practices emerging in crisis care, contact Monica Johnson, Managing Director for Behavioral Health. Prior to joining HMA, Ms. Johnson, Managing Director for Behavioral Health, was the director of the 988 & Behavioral Health Crisis Coordinating Office at the Substance Abuse and Mental Health Services Administration—the federal agency that leads public health efforts to advance the behavioral health of the nation.

May 21, 2025
CMS Seeks Input on the Future of Digital Health: What the Health Technology Ecosystem RFI Means for Stakeholders

Building State Capacities for Medicaid Work and Community Engagement Requirements
Medicaid covers nearly 80 million people nationally, with an estimated 20 million covered through the Medicaid expansion. As state legislatures pass work requirement laws, governors consider executive actions, and Congress contemplates a nationwide mandate, vetting key implementation issues can significantly impact the direction of related policies.
It is difficult to generate accurate projections given the lack of specificity in the current legislation and state implementation variables. According to Congressional Budget Office (CBO) estimates, approximately 5 million people with coverage because of the Medicaid expansion would lose their coverage as a result of not meeting community engagement requirements. The legislation passed by the House on May 22nd establishes a deadline of December 31, 2026 for implementation, but individual states could move earlier. Even before implementation, states must test operations, enable systems, and establish connections to beneficiaries to reduce potential implementation missteps, inappropriate disenrollments, and litigation risks.
If the goal of Medicaid work requirement policies is to stimulate connections between health benefits and employment/workforce, building state and federal capacities to support these approaches is critical to effectuating that change. This blog focuses on introducing operational dynamics that need to be discussed, tested, and built.
Legislative and Other Context
In the language that House advanced, all states would be obliged to implement work and community engagement requirements for adults without dependents for at least 80 hours per month.[1] Employment, work programs, education, or community service (or a combination of those activities) would satisfy the requirement. There were also provisions which enabled states to implement more frequent eligibility checks and compliance requirements as well as co-pays for certain services. Though the federal authorization has received a great deal of attention, at least 14 states have moved forward (see Table 1) in advance of the current federal debate by passing laws and submitting work requirement demonstration requests to the Centers for Medicare & Medicaid Services (CMS).
Table 1. A Review of 2025 States’ Approaches to Work Requirements in Medicaid
| Status | State | Population Criteria | Requirements | Exemptions/ Notes | Public Comment |
| Work Requirement Request Submitted | Arizona | Ages 19−55 | 80 hours/month | Multiple exemptions; 5-year lifetime limit | Closed |
| Work Requirement Request Submitted | Arkansas | Ages 19−64; covered by a qualified health plan (QHP) | Data matching to assess whether on track/not on track | No exemptions | Closed |
| Work Requirement Amendment Request Submitted | Georgia | Ages 19−64; 0-100% FPL | 80 hours/month | Already has approval but is requesting reporting be changed from monthly to annually and adding more qualifying activities | Federal comment period open through June 1, 2025 |
| Work Requirement Request Submitted | Ohio | Ages 19−54; expansion adults | Unspecified hours | Limited list of exemptions | Closed |
| Legislation Passed | Idaho | Ages 19−64 | 20 hours/week required | Limited list of exemptions | — |
| Legislation Passed | Indiana | Ages 19−64; expansion adults | 20 hours/week required | Limited list of exemptions | — |
| Legislation Passed | Montana | Ages 19−55 | 80 hours/month required | Multiple exemptions | — |
| Ballot Initiative Passed | South Dakota | Expansion adults | — | 2024 ballot initiative asking voters for approval for state to impose work requirements for expansion adults passed | — |
| Legislation Pending | North Carolina | — | — | Pursue requirements that are CMS approvable | — |
| Work Requirement Request Draft | Iowa | Ages 19−64; expansion adults | 100 hours/month required | Limited list of exemptions Separate bill would end expansion if work requirements are withdrawn/ prohibited (80 hr./mo.) | Closed |
| Work Requirement Request Draft | Kentucky | Ages 19−60; no dependents; enrolled more than 12 months | Connected to employment resources | Multiple exemptions | State comment period open through June 12, 2025 |
| Work Requirement Request Draft | South Carolina | Ages 19−64; 67%−100% FPL | Specified activities (work specific is 80 hours/month) | Limiting participation to 11,400 individuals based upon available state funding | State comment period open through May 31, 2025 |
| Work Requirement Request Draft | Utah | Expansion adults ages 19−59 | Register for work, complete an employment training assessment and assigned job training, and apply to jobs with at least 48 employers within 3 months of enrollment | Several exemptions, largely aligned with federal SNAP exemptions | State comment period open through May 22, 2025 |
| Anticipated Waiver Request | Alabama | Non-expansion population | — | Potential to resubmit previous work requirement demonstration request | — |
Key Questions Regarding State Policy Options
Considerable research and findings put policymakers in a better position to be prepared to act on a new law since previous attempts and implementing similar policies exposed fundamental problems. Some previous findings include the high cost of administration relative to potential savings, the importance of systems that support foundational items like logging an enrollee’s compliance activities and exemptions, as well as developing an efficient appeals process. The Medicaid and CHIP Payment and Access Commission, General Accounting Office, National Institutes for Health, and multiple researchers have published assessments regarding previous experiences that could improve policymaking.
Below we discuss critical issues and considerations including:
- Exemptions, particularly medical frailty definitions and assessments
- Developing and streamlining systems and process to promote continued coverage for eligible individuals
- Clinical and utilization data that promotes eligibility assessment
- Managed Care engagement in Work Requirements/Community Engagement initiatives
- Measuring impact and adapting policies where needed
1. Which populations are exempt from work requirements?
The requirements in the current legislation would apply only to individuals between the ages of 19 and 64 without dependents, and the following groups are exempted: women who are pregnant or entitled to postpartum medical assistance, members of Tribes, individuals who are medically frail (i.e., people who are blind, disabled, with chronic substance use disorder, serious or complex medical conditions, or others as approved by the Secretary of the U.S. Department of Health and Human Services), parents or caregivers to a dependent child or individuals with a disability, veterans, people who are participating in a drug or alcoholic treatment and rehabilitation program, or individuals who are incarcerated or have been released from incarceration in the past 90 days. Additionally, individuals who already meet work requirements through other programs, such as Temporary Assistance for Needy Families (TANF) or the Supplemental Nutrition Assistance Program (SNAP), would be exempt. However, according to the House-passed version, the eligibility verification and work requirements for SNAP have been made more stringent and program costs are being shifted to states, which affects cross-functional eligibility. Lastly, the legislation includes temporary hardship waivers for natural disasters and areas with an unemployment rate greater than 8 percent or 150 percent of the national average.
The federal government and/or states will identify individuals classified as “medically frail” and make them exempt them from the mandates. This includes those with chronic, serious, or complex medical conditions. Various methods may be employed to identify these individuals, such as analyzing historical medical and pharmacy data to categorize complex conditions, using proprietary algorithms to stratify individuals with multiple comorbidities, and enabling physicians to evaluate enrollees without relying on a claims history.
2. Which systems best align to build from and support coverage?
The Medicaid unwinding from the COVID Public Health Emergency taught lessons about the complexities of Medicaid systems (e.g., assessing cases to ensure eligible children retain coverage if a parent is removed), patient engagement, and reliable methods of member outreach (e.g., email, text, and member portals rather than paper communication). Call abandonment rates, call center wait times, and application processing times surfaced as practical measures of performance (or lack thereof) during the Medicaid unwinding. Multiple informal sources point to poor mailing address or “return to sender” as being anywhere between 15 and 50 percent, bringing tangibility to an implementation baseline. TANF and SNAP programs have work requirement provisions. While those programs are regulated and administered by multiple federal and state agencies, the platforms that support those provisions and the potential for integration are critical vehicles to explore.
State Workforce Commissions and Departments of Labor are clear partners, as they manage integrated eligibility systems and data-sharing agreements across programs like SNAP and TANF, which also serve many Medicaid participants. These and other partnerships will need to be explored to address engagement challenges for many populations, including individuals facing housing instability, which disrupts communication, engagement, and compliance tracking.[2] It is essential that states develop targeted outreach and education strategies to support awareness of participation requirements and ways for individuals to meaningfully engage.
3. Do we have a sense of the healthcare needs/chronic conditions among the Medicaid enrollees that will be affected by work requirements?
Many individuals with chronic diseases may be exempt from the requirements, but not all of them. To that end, insights regarding pharmacy claims may be a useful lens through which we can ascertain an understanding of the potential impact on utilization trends. Notably, the Medicaid expansion population still has significant healthcare utilization rates for services related to behavioral health and for chronic health conditions like hypertension and diabetes. In fact, a recent Health Management Associates (HMA), analysis of CMS data indicated that the top pharmaceuticals spending classes for the Medicaid expansion population were hypoglycemics ($7.6 billion), antivirals ($5.5 billion), and anti-inflammatories ($3.3 billion). The drugs are used to treat autoimmune conditions, including rheumatoid arthritis and psoriatic arthritis. Knowing the health status and chronic conditions of the populations affected and which conditions qualify for exemption are variables as implementation issues like the definition of medically frail are addressed.
4. What does this mean for managed care organizations?
Approximately 80 percent of Medicaid expansion beneficiaries are enrolled in comprehensive managed care organizations (MCOs). States will need to review the scope of existing vendor contracts as well as determine the need for new services, roles, third-party reporting, oversight, and potential exemptions for emergencies. Work requirements can disrupt MCO risk pool stability and care coordination because of administrative burdens and disruptive, less predictable enrollment cycles. That said, MCOs not only have a financial incentive to drive down inappropriate disenrollments, but are also uniquely positioned to support state responsibilities, including maintenance of up-to-date contact information. The delineation of roles and clarification of contracts and responsibilities among states, MCOs, TPAs, and other specialty organizations supporting work requirements will be a critical early-stage framing point for a functional infrastructure.
Many states have sought to support more seamlessness among insurers, with a goal of having the same insurers provide coverage to people as they transition through Medicaid, Marketplace, and employer-sponsored insurance (ESI) as their employment status changes over time. States like Nevada, Rhode Island, and New Mexico require Medicaid MCOs to participate in the Marketplace. Additionally, states like North Carolina, Utah, and West Virginia not only require MCO participation in the Marketplace, but also enable MCOs to co-market Medicaid and Marketplace products for individuals who lose their Medicaid eligibility.
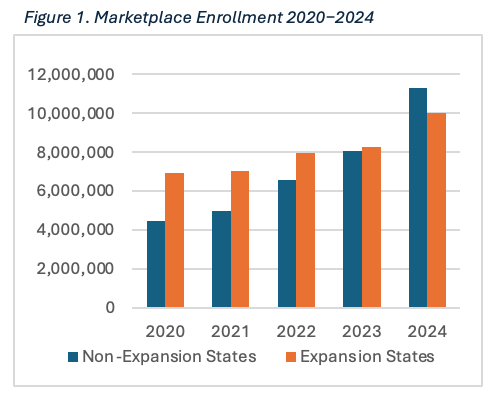
As Figure 1 indicates, Marketplace enrollment in non-expansion states has received considerable traction in recent years and has outpaced expansion states with respect to member growth in the past five years. Marketplaces have undeniably carved out large roles in the health coverage infrastructure in non-expansion states—a point that was less clear just a few years ago. Though, multiple factors affect those Marketplace growth rates, including congressional decisions regarding the continuation and funding of the enhanced premium tax credit program. In the current legislation, these credits expire, which the CBO estimates will lead to an additional coverage loss of nearly 5 million by 2034.
5. Can states measure and be nimble with policies as the impacts are determined?
Federal and state regulations that identify contextualized and dynamic metrics that provide actionable information to federal and state policy makers will support effective oversight and monitoring. States starting with listening sessions in the near term can help identify goals and metrics. The focus of such efforts could include actively monitoring potential changes and cost shifts for the uninsured population to non-public payers and providers.
The Medicaid unwinding also demonstrated that the story was far less of a red/blue story than a series of complex tasks that required many administrative resources, provider and community partnerships, and enrollee outreach to create a path that would limit unnecessary disruptions and expenses. CMS guidance for goals and evaluations as well as state inputs will need to emerge prior to implementation so policymakers can be well-equipped to be nimble and dynamic with policy changes as well as understanding the short-term and longitudinal effects of this fundamental shift.
[1] U.S. Congress. House. One Big Beautiful Bill Act. H.R.1. 119th Cong., 1st sess. Introduced May 20, 2025.
[2] Soni A, Blackburn J. Health Characteristics of Adults Unable to Complete Medicaid Renewal During the Unwinding Period. JAMA Health Forum. 2025;6(3):e250092. doi:10.1001/jamahealthforum.2025.0092

Supporting Medicaid Dental Benefit Administrators: Oral health and dental care are vital for the health of communities
HMA Spotlight
Supporting Medicaid Dental Benefit Administrators: Oral health and dental care are vital for the health of communities
Whether performing under risk-based prepaid ambulatory health plan (PAHP) contracts or non-risk (administrative service organizations), Medicaid dental managed care organizations (MCOs) and dental benefit administrators (DBAs) face the same challenges as Medicaid MCOs, and state Medicaid agencies, including but not limited to:
– Getting into and staying in compliance with state regulatory and contract requirements
– Understanding and responding to new federal and state rules and regulations
– Growing market share including success in state procurements, in MCO solicitations for DBAs, and attracting and retaining enrollees
– Improving utilization to meet quality measure targets, medical loss ratios, and margin expectations including increased utilization of preventive oral health care, and decreased utilization of unnecessary care such as avoidable emergency room care for dental diagnoses
– Excelling in benefit administration operations including member services and engagement, provider network development and provider services, claim/encounter administration, reporting, and other functional areas
– Managing financial risk including developing or validating capitation rates and developing value-based payment arrangements
The importance of oral health and dental care
Oral health is integral to the overall health and quality of an individual’s life, and lack of access to oral health care negatively impacts entire populations.
Tooth decay affects 90% of adults 20 to 64 years of age and costs the U.S. about $45.9B in lost productivity in 2015. This frequently results in visits to hospital emergency rooms where care is often palliative but does not treat the root cause of problems1
Gum disease affects almost 50% of adults 45 to 64 years of age and is a risk factor for nearly 60 other adverse health conditions, including Alzheimer’s disease, diabetes, and heart disease2
More than half of working-age adults living in poverty have untreated caries (52%), whereas only 1 out of 5 adults with incomes of twice the federal poverty guideline or higher have untreated caries (20%)3
Tooth decay is preventable but impacts nearly 46% of U.S. children. Left untreated, tooth decay can cause chronic pain, impaired development, disfiguration, and social isolation. In severe cases, bacteria from a tooth infection can even travel to the brain and cause death. Caries disproportionately affect children who experience poverty, belong to certain racial and ethnic groups, or are affected by other social factors4
OUR EXPERTISE
At HMA, our consultants have led MCOs, state Medicaid agencies, and include senior officials from Medicare, directors of large nonprofit and social services organizations, top-level advisors, C-level executives at hospitals, health systems and health plans, and senior-level physicians. We know that oral health, access to dental care, and oral health literacy play a vital role in the health of communities supported by Medicaid MCOs. HMA can support the work that DBAs do and the challenges they face in the changing Medicaid environment.
How HMA can help
HMA has decades of experience working with Medicaid MCOs, DBAs, state Medicaid agency dental policy makers, and oral health providers. HMA can:
Provide actionable insights into new federal and state regulations and guidance to help clients understand potential impacts and opportunities for their business. We assist clients to determine what must be done, what can be done, and develop recommendations for what should be done, and to implement those activities. DBAs are frequently performing as PAHPs and are subject to many of the federal rules related to interoperability, prior authorization, access, and eligibility that apply to Medicaid MCOs. HMA provides our Medicaid provider and payer clients with analyses about those rules, which could also benefit DBAs.
Perform validation and compliance support to help clients identify and address any compliance gaps and support clients in validating their own compliance with any state or MCO imposed Corrective Action Plans. We also support clients to grow and strengthen their own capabilities and infrastructure to perform these functions.
Support client growth with end-to-end procurement assistance, including market conditioning and strategy, writing, mock scoring, orals preparation, implementation, and operations stabilization assistance; and with market analysis.
Support delivery system, reimbursement, and provider network design by conducting research and analysis on oral health delivery system approaches, provider reimbursement structures, coverage, and access trends.
Identify, assess, and help implement best practices in oral health care programs related to special populations, including children’s access to oral health care and dental access in rural communities.
Support quality improvement and utilization management initiatives that increase appropriate and desired utilization and curb inappropriate utilization. This can include help achieving Healthcare Effectiveness Data and Information Set (HEDIS) measure goals and developing oral health literacy programs, achieving accreditation, developing and implementing Performance Improvement Plans (PIPs), and conducting data analysis to understand utilization and evaluate the impact of program changes on utilization.
Provide actuarial services in support of benefit and program design, capitation rate development, and capitation rate validation.
Design and evaluate value-based payment models that tie provider payments to quality and value.
Project spotlight
Minnesota Medicaid Dental Program Study
The 2021 Minnesota Legislature directed the Department of Human Services (DHS) to conduct a review of Medicaid dental program delivery systems in states that have enacted and implemented a “carve out” dental delivery system. This legislation also directed DHS to conduct an analysis of dental provider hesitancy to participate in the Medical Assistance (MA) program as an enrolled provider. DHS contracted with HMA to conduct the analyses mandated in the legislation. HMA reviewed the Medicaid dental program delivery systems in states that have implemented a carve-out dental delivery system, including comparing state program designs, program costs and rates where available, and quality metrics for children one through 20 years of age with at least one preventive dental service within a year. HMA also surveyed dental providers to better understand hesitancy to participate in Medicaid and opinions on policy approaches to improve provider participation.
The final report, available at https://www.lrl.mn.gov/docs/2022/mandated/220701.pdf, described the analysis of state dental carve-out experiences and the dental provider survey results.
Contact our experts:

Sarah Arvey
Associate Principal

Rebecca Kellenberg
Principal

Beth Kidder
Regional Director

Stephen Palmer
Principal

Caroline (Carrie) Rosenzweig
Principal
[1] Oral Health in America – April 2022 Bulletin, National Institute of Dental and Craniofacial Research, accessed 4/1/2025, https://www.nidcr.nih.gov/research/oralhealthinamerica/section-3a-summary#:~:text=In%20adulthood%2C%20the%20relationship%20between,to%20achieving%20better%20oral%20health
[2] Oral Health in America – April 2022 Bulletin, National Institute of Dental and Craniofacial Research, accessed 4/1/2025, https://www.nidcr.nih.gov/research/oralhealthinamerica/section-3a-summary#:~:text=In%20adulthood%2C%20the%20relationship%20between,to%20achieving%20better%20oral%20health
[3] National Institutes of Health. Oral Health in America: Advances and Challenges. Bethesda, MD: US Department of Health and Human Services, National Institutes of Health, National Institute of Dental and Craniofacial Research, 2021, https://www.nidcr.nih.gov/sites/default/files/2021-12/Oral-Health-in-America-Advances-and-Challenges.pdf#page=343
[4] Big Hopes for Little Teeth, National Institute of Dental and Craniofacial Research, accessed 4/1/2025, https://www.nidcr.nih.gov/news-events/nidcr-news/2024/big-hopes-little-teeth#:~:text=Left%20untreated%2C%20tooth%20decay%20can,the%20brain%20and%20cause%20death